Abstract
Purpose
There is a growing body of diagnostic performance studies for emergency radiology-related artificial intelligence/machine learning (AI/ML) tools; however, little is known about user preferences, concerns, experiences, expectations, and the degree of penetration of AI tools in emergency radiology. Our aim is to conduct a survey of the current trends, perceptions, and expectations regarding AI among American Society of Emergency Radiology (ASER) members.
Methods
An anonymous and voluntary online survey questionnaire was e-mailed to all ASER members, followed by two reminder e-mails. A descriptive analysis of the data was conducted, and results summarized.
Results
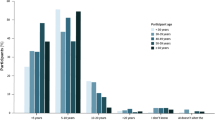
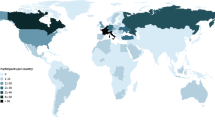
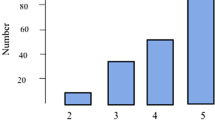
A total of 113 members responded (response rate 12%). The majority were attending radiologists (90%) with greater than 10 years’ experience (80%) and from an academic practice (65%). Most (55%) reported use of commercial AI CAD tools in their practice. Workflow prioritization based on pathology detection, injury or disease severity grading and classification, quantitative visualization, and auto-population of structured reports were identified as high-value tasks. Respondents overwhelmingly indicated a need for explainable and verifiable tools (87%) and the need for transparency in the development process (80%). Most respondents did not feel that AI would reduce the need for emergency radiologists in the next two decades (72%) or diminish interest in fellowship programs (58%). Negative perceptions pertained to potential for automation bias (23%), over-diagnosis (16%), poor generalizability (15%), negative impact on training (11%), and impediments to workflow (10%).
Conclusion
ASER member respondents are in general optimistic about the impact of AI in the practice of emergency radiology and its impact on the popularity of emergency radiology as a subspecialty. The majority expect to see transparent and explainable AI models with the radiologist as the decision-maker.
Similar content being viewed by others
References
Fujita H (2020) AI-based computer-aided diagnosis (AI-CAD): the latest review to read first. Radiol Phys Technol 13(1):6–19
Zhou SK, Greenspan H, Davatzikos C, Duncan JS, Van Ginneken B, Madabhushi A, Prince JL, Rueckert D, Summers RM (2021) A review of deep learning in medical imaging: imaging traits, technology trends, case studies with progress highlights, and future promises. Proc IEEE 109(5):820–838
West E, Mutasa S, Zhu Z, Ha R (2019) Global trend in artificial intelligence–based publications in radiology from 2000 to 2018. Am J Roentgenol 213(6):1204–1206
Ebrahimian S, Kalra MK, Agarwal S, Bizzo BC, Elkholy M, Wald C, Allen B, Dreyer KJ (2022) FDA-regulated AI algorithms: trends, strengths, and gaps of validation studies. Acad Radiol 29(4):559–566
Banaste N, Caurier B, Bratan F, Bergerot J-F, Thomson V, Millet I (2018) Whole-body CT in patients with multiple traumas: factors leading to missed injury. Radiology 289(2):374–383
Hanna TN, Zygmont ME, Peterson R, Theriot D, Shekhani H, Johnson J-O, Krupinski EA (2018) The effects of fatigue from overnight shifts on radiology search patterns and diagnostic performance. J Am Coll Radiol 15(12):1709–1716
Bruno MA (2020) Radiology errors across the diurnal cycle. Radiology 297(2):380–381. https://doi.org/10.1148/radiol.2020202902
Glover M IV, Almeida RR, Schaefer PW, Lev MH, Mehan WA Jr (2017) Quantifying the impact of noninterpretive tasks on radiology report turn-around times. J Am Coll Radiol 14(11):1498–1503
Chong ST, Robinson JD, Davis MA, Bruno MA, Roberge EA, Reddy S, Pyatt RS Jr, Friedberg EB (2019) Emergency radiology: current challenges and preparing for continued growth. J Am Coll Radiol 16(10):1447–1455
Hanna TN, Shekhani H, Lamoureux C, Mar H, Nicola R, Sliker C, Johnson J-O (2017) Emergency radiology practice patterns: shifts, schedules, and job satisfaction. J Am Coll Radiol 14(3):345–352
Kalyanpur A, Weinberg J, Neklesa V, Brink JA, Forman HP (2003) Emergency radiology coverage: technical and clinical feasibility of an international teleradiology model. Emerg Radiol 10(3):115–118
Kalyanpur A (2020) Teleradiology and artificial intelligence–birds of the same feather. Acad Radiol 27(1):123–126
Agrawal A (2022) Emergency teleradiology-past, present, and is there a future? Front Radiol 2:866643
Soun J, Chow D, Nagamine M, Takhtawala R, Filippi C, Yu W, Chang P (2021) Artificial intelligence and acute stroke imaging. Am J Neuroradiol 42(1):2–11
Soffer S, Klang E, Shimon O, Barash Y, Cahan N, Greenspana H, Konen E (2021) Deep learning for pulmonary embolism detection on computed tomography pulmonary angiogram: a systematic review and meta-analysis. Sci Rep 11(1):1–8
Davis MA, Rao B, Cedeno PA, Saha A, Zohrabian VM (2022) Machine learning and improved quality metrics in acute intracranial hemorrhage by noncontrastcomputed tomography. Curr Probl Diagn Radiol 51(4):556–561. https://doi.org/10.1067/j.cpradiol.2020.10.007
Gipson J, Tang V, Seah J, Kavnoudias H, Zia A, Lee R, Mitra B, Clements W (2022) Diagnostic accuracy of a commercially available deep-learning algorithm in supine chest radiographs following trauma. Br J Radiol 95:20210979
Guermazi A, Tannoury C, Kompel AJ, Murakami AM, Ducarouge A, Gillibert A, Li X, Tournier A, Lahoud Y, Jarraya M (2022) Improving radiographic fracture recognition performance and efficiency using artificial intelligence. Radiology 302(3):627–636
Seah JC, Tang CH, Buchlak QD, Holt XG, Wardman JB, Aimoldin A, Esmaili N, Ahmad H, Pham H, Lambert JF (2021) Effect of a comprehensive deep-learning model on the accuracy of chest X-ray interpretation by radiologists: a retrospective, multireader multicase study. Lancet Digit Health 3(8):e496–e506
Kau T, Ziurlys M, Taschwer M, Kloss-Brandstätter A, Grabner G, Deutschmann H (2022) FDA-approved deep learning software application versus radiologists with different levels of expertise: detection of intracranial hemorrhage in a retrospective single-center study. Neuroradiology 64(5):981–990
Duron L, Ducarouge A, Gillibert A, Lainé J, Allouche C, Cherel N, Zhang Z, Nitche N, Lacave E, Pourchot A (2021) Assessment of an AI aid in detection of adult appendicular skeletal fractures by emergency physicians and radiologists: a multicenter cross-sectional diagnostic study. Radiology 300(1):120–129
Wismüller A, Stockmaster L (2020) A prospective randomized clinical trial for measuring radiology study reporting time on Artificial Intelligence-based detection of intracranial hemorrhage in emergent care head CT. In: Proc. SPIE 11317, Medical Imaging 2020: Biomedical Applications in Molecular, Structural, and Functional Imaging, p 113170M. https://doi.org/10.1117/12.2552400
Huisman M, Ranschaert E, Parker W, Mastrodicasa D, Koci M, Pinto de Santos D, Coppola F, Morozov S, Zins M, Bohyn C (2021) An international survey on AI in radiology in 1,041 radiologists and radiology residents part 1: fear of replacement, knowledge, and attitude. Eur Radiol 31(9):7058–7066
Huisman M, Ranschaert E, Parker W, Mastrodicasa D, Koci M, Pinto de Santos D, Coppola F, Morozov S, Zins M, Bohyn C (2021) An international survey on AI in radiology in 1041 radiologists and radiology residents part 2: expectations, hurdles to implementation, and education. Eur Radiol 31(11):8797–8806
van Hoek J, Huber A, Leichtle A, Härmä K, Hilt D, von Tengg-Kobligk H, Heverhagen J, Poellinger A (2019) A survey on the future of radiology among radiologists, medical students and surgeons: students and surgeons tend to be more skeptical about artificial intelligence and radiologists may fear that other disciplines take over. Eur J Radiol 121:108742
Jalal S, Parker W, Ferguson D, Nicolaou S (2021) Exploring the role of artificial intelligence in an emergency and trauma radiology department. Can Assoc Radiol J 72(1):167–174
Moulik SK, Kotter N, Fishman EK (2020) Applications of artificial intelligence in the emergency department. Emerg Radiol 27:355–358. https://doi.org/10.1007/s10140-020-01794-1
Jacques T, Fournier L, Zins M, Adamsbaum C, Chaumoitre K, Feydy A, Millet I, Montaudon M, Beregi J-P, Bartoli J-M (2021) Proposals for the use of artificial intelligence in emergency radiology. Diagn Interv Imaging 102(2):63–68
Lakhani P, Prater AB, Hutson RK, Andriole KP, Dreyer KJ, Morey J, Prevedello LM, Clark TJ, Geis JR, Itri JN (2018) Machine learning in radiology: applications beyond image interpretation. J Am Coll Radiol 15(2):350–359
Noguerol TM, Paulano-Godino F, Martín-Valdivia MT, Menias CO, Luna A (2019) Strengths, weaknesses, opportunities, and threats analysis of artificial intelligence and machine learning applications in radiology. J Am Coll Radiol 16(9):1239–1247
Goldberg JE, Rosenkrantz AB (2019) Artificial intelligence and radiology: a social media perspective. Curr Probl Diagn Radiol 48(4):308–311
Langlotz CP, Allen B, Erickson BJ, Kalpathy-Cramer J, Bigelow K, Cook TS, Flanders AE, Lungren MP, Mendelson DS, Rudie JD (2019) A roadmap for foundational research on artificial intelligence in medical imaging: from the 2018 NIH/RSNA/ACR/The Academy Workshop. Radiology 291(3):781
Allen B Jr, Seltzer SE, Langlotz CP, Dreyer KP, Summers RM, Petrick N, Marinac-Dabic D, Cruz M, Alkasab TK, Hanisch RJ (2019) A road map for translational research on artificial intelligence in medical imaging: from the 2018 National Institutes of Health/RSNA/ACR/The Academy Workshop. J Am Coll Radiol 16(9):1179–1189
Park SH, Han K (2018) Methodologic guide for evaluating clinical performance and effect of artificial intelligence technology for medical diagnosis and prediction. Radiology 286(3):800–809
Chen H, Gomez C, Huang C-M, Unberath M (2022) Explainable medical imaging AI needs human-centered design: guidelines and evidence from a systematic review. npj Digit Med 5(1):1–15
Bluemke DA, Moy L, Bredella MA, Ertl-Wagner BB, Fowler KJ, Goh VJ, Halpern EF, Hess CP, Schiebler ML, Weiss CR (2020) assessing radiology research on artificial intelligence: a brief guide for authors, reviewers, and readers-from the radiology editorialboard. Radiology 294(3):487–489. https://doi.org/10.1148/radiol.2019192515
Jones RM, Sharma A, Hotchkiss R, Sperling JW, Hamburger J, Ledig C, O’Toole R, Gardner M, Venkatesh S, Roberts MM (2020) Assessment of a deep-learning system for fracture detection in musculoskeletal radiographs. NPJ Digit Med 3(1):1–6
Dupuis M, Delbos L, Veil R, Adamsbaum C (2022) External validation of a commercially available deep learning algorithm for fracture detection in children. Diagn Interv Imaging 103(3):151–159
Chilamkurthy S, Ghosh R, Tanamala S, Biviji M, Campeau NG, Venugopal VK, Mahajan V, Rao P, Warier P (2018) Deep learning algorithms for detection of critical findings in head CT scans: a retrospective study. Lancet 392(10162):2388–2396
Ginat DT (2020) Analysis of head CT scans flagged by deep learning software for acute intracranial hemorrhage. Neuroradiology 62(3):335–340
Voter A, Larson M, Garrett J, Yu J-P (2021) Diagnostic accuracy and failure mode analysis of a deep learning algorithm for the detection of cervical spine fractures. Am J Neuroradiol 42(8):1550–1556
Voter AF, Meram E, Garrett JW, John-Paul JY (2021) Diagnostic accuracy and failure mode analysis of a deep learning algorithm for the detection of intracranial hemorrhage. J Am Coll Radiol 18(8):1143–1152
Arrieta AB, Díaz-Rodríguez N, Del Ser J, Bennetot A, Tabik S, Barbado A, Garcia S, Gil-Lopez S, Molina D, Benjamins R (2020) Explainable artificial intelligence (XAI): concepts, taxonomies, opportunities and challenges toward responsible AI. Inf Fusion 58:82–115
Lavin A, Gilligan-Lee CM, Visnjic A, Ganju S, Newman D, Ganguly S, Lange D, Baydin AG, Sharma A, Gibson A (2022) Technology readiness levels for machine learning systems. Nat Commun 13(1):1–19
Lee S, Summers RM (2021) Clinical artificial intelligence applications in radiology: chest and abdomen. Radiol Clin 59(6):987–1002
Dreizin D, Zhou Y, Fu S, Wang Y, Li G, Champ K, Siegel E, Wang Z, Chen T, Yuille AL (2020) A Multiscale Deep Learning Method for Quantitative Visualization of Traumatic Hemoperitoneum at CT: Assessment of Feasibility and Comparison with Subjective Categorical Estimation. Radiol Artif Intell 2(6):e190220
Dreizin D, Zhou Y, Zhang Y, Tirada N, Yuille AL (2020) Performance of a deep learning algorithm for automated segmentation and quantification of traumatic pelvic hematomas on CT. J Digit Imaging 33(1):243–251
Chen H, Unberath M, Dreizin D (2023) Toward automated interpretable AAST grading for blunt splenic injury. Emerg Radiol 30:41–50. https://doi.org/10.1007/s10140-022-02099-1
Zhou Y, Dreizin D, Wang Y, Liu F, Shen W, Yuille AL (2021) External attention assisted multi-phase splenic vascular injury segmentation with limited data. IEEE Trans Med Imaging 41(6):1346–1357
Dreizin D, Zhou Y, Chen T, Li G, Yuille AL, McLenithan A, Morrison JJ (2020) Deep learning-based quantitative visualization and measurement of extraperitoneal hematoma volumes in patients with pelvic fractures: potential role in personalized forecasting and decision support. J Trauma Acute Care Surg 88(3):425
Dreizin D, Chen T, Liang Y, Zhou Y, Paes F, Wang Y, Yuille AL, Roth P, Champ K, Li G (2021) Added value of deep learning-based liver parenchymal CT volumetry for predicting major arterial injury after blunt hepatic trauma: a decision tree analysis. Abdom Radiol 46(6):2556–2566
Choi J, Mavrommati K, Li NY, Patil A, Chen K, Hindin DI, Forrester JD (2022) Scalable deep learning algorithm to compute percent pulmonary contusion among patients with rib fractures. J Trauma Acute Care Surg 93(4):461–466
Röhrich S, Hofmanninger J, Negrin L, Langs G, Prosch H (2021) Radiomics score predicts acute respiratory distress syndrome based on the initial CT scan after trauma. Eur Radiol 31(8):5443–5453
Wang F, Kaushal R, Khullar D (2020) Should health care demand interpretable artificial intelligence or accept “Black Box” Medicine? Ann Intern Med 172(1):59–60. https://doi.org/10.7326/M19-2548
Adamson AS, Welch HG (2019) Machine learning and the cancer-diagnosis problem-no gold standard. N Engl J Med 381(24):2285–2287
Banerjee M, Chiew D, Patel KT, Johns I, Chappell D, Linton N, Cole GD, Francis DP, Szram J, Ross J (2021) The impact of artificial intelligence on clinical education: perceptions of postgraduate trainee doctors in London (UK) and recommendations for trainers. BMC Med Educ 21(1):1–10
Seyyed-Kalantari L, Zhang H, McDermott M, Chen IY, Ghassemi M (2021) Underdiagnosis bias of artificial intelligence algorithms applied to chest radiographs in under-served patient populations. Nat Med 27(12):2176–2182
He J, Baxter SL, Xu J, Xu J, Zhou X, Zhang K (2019) The practical implementation of artificial intelligence technologies in medicine. Nat Med 25(1):30–36
Daye D, Wiggins WF, Lungren MP, Alkasab T, Kottler N, Allen B, Roth CJ, Bizzo BC, Durniak K, Brink JA (2022) Implementation of clinical artificial intelligence in radiology: who decides and how? Radiology 305(3):555–563
Lin M (2022) What’s needed to bridge the gap between US FDA Clearance and real-world use of AI algorithms. Acad Radiol 29(4):567–568
Bin Dahmash A, Alabdulkareem M, Alfutais A, Kamel AM, Alkholaiwi F, Alshehri S, Al Zahrani Y, Almoaiqel M (2020) Artificial intelligence in radiology: does it impact medical students preference for radiology as their future career? BJR| Open 2:20200037
Ellahham S, Ellahham N, Simsekler MCE (2020) Application of artificial intelligence in the health care safety context: opportunities and challenges. Am J Med Qual 35(4):341–348
Challen R, Denny J, Pitt M, Gompels L, Edwards T, Tsaneva-Atanasova K (2019) Artificial intelligence, bias and clinical safety. BMJ Qual Saf 28(3):231–237
Lee CS, Nagy PG, Weaver SJ, Newman-Toker DE (2013) Cognitive and system factors contributing to diagnostic errors in radiology. Am J Roentgenol 201(3):611–617
Patlas MN, Katz DS, Scaglione M (2019) Errors in emergency and trauma radiology: Springer
Funding
David Dreizin funding source: NIH K08 EB027141-01A1 (PI: David Dreizin, MD)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Agrawal, A., Khatri, G.D., Khurana, B. et al. A survey of ASER members on artificial intelligence in emergency radiology: trends, perceptions, and expectations. Emerg Radiol 30, 267–277 (2023). https://doi.org/10.1007/s10140-023-02121-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-023-02121-0