Abstract
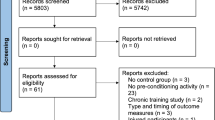
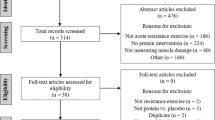
Photobiomodulation therapy (PBMT) was introduced as an ergogenic aid for sport performance in healthy individuals is still controversial. The main aim of this study is to assess the potential enhancements in muscle endurance and recovery from muscle strength and injuries mediated by PBMT among individuals exhibiting diverse activity levels. Randomized controlled trials (RCT) of PBMT interventions for healthy people (both trained and untrained individuals) exercising were searched (up to January 16, 2024) in four electronic databases: Web of Science, PubMed, Scopus and Embase. Primary outcome measures included muscle endurance, muscle strength and creatine kinase (CK) levels; secondary outcome measure included Lactate dehydrogenase (LDH) levels. Subgroup analyses based on physical activity levels were conducted for each outcome measure. Thirty-four RCTs were included based on the article inclusion and exclusion criteria. Statistical results showed that PBMT significantly improved muscle endurance (standardized mean difference [SMD] = 0.31, 95%CI 0.11, 0.51, p < 0.01), indicating a moderate effect size. It also facilitated the recovery of muscle strength (SMD = 0.24, 95%CI 0.10, 0.39, p < 0.01) and CK (mean difference [MD] = -77.56, 95%CI -112.67, -42.44, p < 0.01), indicating moderate and large effect sizes, respectively. Furthermore, pre-application of PBMT significantly improved muscle endurance, recovery of muscle strength and injuries in physically inactive individuals and athletes (p < 0.05), while there was no significant benefit for physically active individuals. Pre-application of PBMT improves muscle endurance and promotes recovery from muscle strength and injury (includes CK and LDH) in athletes and sedentary populations, indicating moderate to large effect sizes, but is ineffective in physically active populations. This may be due to the fact that physically active people engage in more resistance training, which leads to a decrease in the proportion of red muscle fibres, thus affecting photobiomodulation.





Similar content being viewed by others
Abbreviations
- CK:
-
Creatine kinase
- CP:
-
Carbonylated protein
- EIMD:
-
Exercise-induced muscle damage
- IPAQ:
-
International Physical Activity Questionnaire
- LEDT:
-
Light emitting diode therapy
- LDH:
-
Lactate dehydrogenase
- LLLT:
-
Low-level laser therapy
- MIVC:
-
Maximum isometric voluntary contraction
- MVC:
-
Maximum voluntary contraction
- PBMT:
-
Photobiomodulation therapy
- ROS:
-
Reactive oxygen species
- SOD:
-
Superoxide dismutase
- TBARS:
-
Thiobarbituric acid reactive substances
- VAS:
-
Visual Analogue Scale
- M:
-
Mean
- MD:
-
Mean difference
- SEM:
-
Standard error of mean
- SMD:
-
Standardized mean difference
References
Howatson G, van Someren KA (2008) The prevention and treatment of exercise-induced muscle damage. Sports Med 38:483–503. https://doi.org/10.2165/00007256-200838060-00004
Fritsch CG, Dornelles MP, Severo-Silveira L et al (2016) Effects of low-level laser therapy applied before or after plyometric exercise on muscle damage markers: randomized, double-blind, placebo-controlled trial. Lasers Med Sci 31:1935–1942. https://doi.org/10.1007/s10103-016-2072-y
Warren GL, Lowe DA, Armstrong RB (1999) Measurement tools used in the study of eccentric contraction-induced injury. Sports Med 27:43–59. https://doi.org/10.2165/00007256-199927010-00004
Allen DG, Lamb GD, Westerblad H (2008) Skeletal muscle fatigue: Cellular mechanisms. Physiol Rev 88:287–332. https://doi.org/10.1152/physrev.00015.2007
Enoka RM, Duchateau J (2016) Translating fatigue to human performance. Med Sci Sports Exerc 48:2228–2238. https://doi.org/10.1249/MSS.0000000000000929
Dupuy O, Douzi W, Theurot D et al (2018) An evidence-based Approach for choosing post-exercise recovery techniques to reduce markers of muscle damage, soreness, fatigue, and inflammation: a systematic review with Meta-analysis. Front Physiol 9:403. https://doi.org/10.3389/fphys.2018.00403
Fatouros IG, Jamurtas AZ (2016) Insights into the molecular etiology of exercise-induced inflammation: opportunities for optimizing performance. J Inflamm Res 9:175–186. https://doi.org/10.2147/JIR.S114635
Baroni BM, Leal Junior ECP, De Marchi T et al (2010) Low level laser therapy before eccentric exercise reduces muscle damage markers in humans. Eur J Appl Physiol 110:789–796. https://doi.org/10.1007/s00421-010-1562-z
Silver MD (2001) Use of ergogenic aids by athletes. J Am Acad Orthop Surg 9:61–70. https://doi.org/10.5435/00124635-200101000-00007
Vanin AA, Verhagen E, Barboza SD et al (2018) Photobiomodulation therapy for the improvement of muscular performance and reduction of muscular fatigue associated with exercise in healthy people: a systematic review and meta-analysis. Lasers Med Sci 33:181–214. https://doi.org/10.1007/s10103-017-2368-6
Chow RT, Johnson MI, Lopes-Martins RAB, Bjordal JM (2009) Efficacy of low-level laser therapy in the management of neck pain: a systematic review and meta-analysis of randomised placebo or active-treatment controlled trials. Lancet 374:1897–1908. https://doi.org/10.1016/S0140-6736(09)61522-1
Agrawal T, Gupta GK, Rai V et al (2014) Pre-conditioning with low-level laser (light) therapy: light before the storm. https://doi.org/10.2203/dose-response.14-032.Agrawal. Dose-Response 12:dose-response.1
Castro KMR, De Paiva Carvalho RL, Junior GMR et al (2020) Can photobiomodulation therapy (PBMT) control blood glucose levels and alter muscle glycogen synthesis? J Photochem Photobiol B 207:111877. https://doi.org/10.1016/j.jphotobiol.2020.111877
Antonialli FC, De Marchi T, Tomazoni SS et al (2014) Phototherapy in skeletal muscle performance and recovery after exercise: effect of combination of super-pulsed laser and light-emitting diodes. Lasers Med Sci 29:1967–1976. https://doi.org/10.1007/s10103-014-1611-7
Follmer B, Dellagrana RA, Rossato M et al (2018) Photobiomodulation therapy is beneficial in reducing muscle fatigue in Brazilian jiu-jitsu athletes and physically active men. Sport Sci Health 14:685–691. https://doi.org/10.1007/s11332-018-0495-5
Leal-Junior ECP, Vanin AA, Miranda EF et al (2015) Effect of phototherapy (low-level laser therapy and light-emitting diode therapy) on exercise performance and markers of exercise recovery: a systematic review with meta-analysis. Lasers Med Sci 30:925–939. https://doi.org/10.1007/s10103-013-1465-4
Abreu JS, de Dos Santos S, Fonsati GV L, et al (2020) Time-Response of Photobiomodulation Therapy by Light-Emitting diodes on muscle torque and Fatigue Resistance in Young men: Randomized, Double-Blind, crossover and placebo-controlled study. Photobiomodul Photomed Laser Surg 38:750–757. https://doi.org/10.1089/photob.2020.4813
Azuma RHE, Merlo JK, Jacinto JL et al (2021) Photobiomodulation Therapy at 808 nm does not improve biceps Brachii performance to exhaustion and Delayed-Onset Muscle Soreness in Young Adult women: a Randomized, controlled, crossover trial. Front Physiol 12:664582. https://doi.org/10.3389/fphys.2021.664582
Cabreira LMB, Merlo JK, Jacinto JL et al (2022) Photobiomodulation therapy with light-emitting diode does not improve lower-body muscle performance and delayed-onset muscle soreness in resistance-trained women: a randomized, controlled, crossover trial. Sci Sports 37:635. e1-635.e9
Wang D, Wang X (2019) Efficacy of laser therapy for exercise-induced fatigue: a meta-analysis. Med (Baltim) 98:e17201. https://doi.org/10.1097/MD.0000000000017201
De Marchi T, Leal Junior ECP, Bortoli C et al (2012) Low-level laser therapy (LLLT) in human progressive-intensity running: effects on exercise performance, skeletal muscle status, and oxidative stress. Lasers Med Sci 27:231–236. https://doi.org/10.1007/s10103-011-0955-5
de Almeida P, Lopes-Martins RAB, De Marchi T et al (2012) Red (660 nm) and infrared (830 nm) low-level laser therapy in skeletal muscle fatigue in humans: what is better? Lasers Med Sci 27:453–458. https://doi.org/10.1007/s10103-011-0957-3
Orssatto LBR, Rossato M, Vargas M et al (2020) Photobiomodulation Therapy effects on Resistance Training volume and discomfort in Well-trained adults: a Randomized, Double-Blind, placebo-controlled trial. Photobiomodul Photomed Laser Surg 38:720–726. https://doi.org/10.1089/photob.2019.4777
Nussbaumer-Streit B, Klerings I, Dobrescu AI et al (2020) Excluding non-english publications from evidence-syntheses did not change conclusions: a meta-epidemiological study. J Clin Epidemiol 118:42–54. https://doi.org/10.1016/j.jclinepi.2019.10.011
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Seifert E (2014) OriginPro 9.1: Scientific Data Analysis and Graphing Software—Software Review. J Chem Inf Model 54:1552–1552. https://doi.org/10.1021/ci500161d
Higgins JPT, Thomas J, Chandler J et al (2022) Cochrane Handbook for Systematic Reviews of Interventions version 6.3 (updated February 2022). In: Cochrane. https://training.cochrane.org/handbook
Keating SE, Johnson NA, Mielke GI, Coombes JS (2017) A systematic review and meta-analysis of interval training versus moderate-intensity continuous training on body adiposity. Obes Rev 18:943–964. https://doi.org/10.1111/obr.12536
Schünemann HJ, Best D, Vist G, Oxman AD (2003) Letters, numbers, symbols and words: how to communicate grades of evidence and recommendations. CMAJ 169:677–680
Leal Junior ECP, Lopes-Martins RAB, Baroni BM et al (2009) Comparison between single-diode low-level laser therapy (LLLT) and LED multi-diode (cluster) therapy (LEDT) applications before high-intensity exercise. Photomed Laser Surg 27:617–623. https://doi.org/10.1089/pho.2008.2350
Ferreira Marinho B, Vidal Andreato L, Follmer B, Franchini E (2016) Comparison of body composition and physical fitness in elite and non-elite Brazilian jiu-jitsu athletes. Sci Sports 31:129–134. https://doi.org/10.1016/j.scispo.2015.12.001
Clarkson PM, Hubal MJ (2002) Exercise-Induced muscle damage in humans. Am J Phys Med Rehabil 81:S52–S69. https://doi.org/10.1097/00002060-200211001-00007
Hayworth CR, Rojas JC, Padilla E et al (2010) In vivo low-level light therapy increases cytochrome oxidase in skeletal muscle. Photochem Photobiol 86:673–680. https://doi.org/10.1111/j.1751-1097.2010.00732.x
MacDougall JD, Sale DG, Moroz JR et al (1979) Mitochondrial volume density in human skeletal muscle following heavy resistance training. Med Sci Sports 11:164–166
Larkin-Kaiser KA, Christou E, Tillman M et al (2015) Near-infrared light therapy to attenuate strength loss after strenuous resistance exercise. J Athl Train 50:45–50. https://doi.org/10.4085/1062-6050-49.3.82
Rossato M, Dellagrana RA, Sakugawa RL et al (2018) Time Response of Photobiomodulation Therapy on muscular fatigue in humans. J Strength Cond Res 32:3285–3293. https://doi.org/10.1519/JSC.0000000000002339
Jacobs RA, Lundby C (2013) Mitochondria express enhanced quality as well as quantity in association with aerobic fitness across recreationally active individuals up to elite athletes. J Appl Physiol 114:344–350. https://doi.org/10.1152/japplphysiol.01081.2012
de Carvalho AR, Caovilla AR, Ficagna A et al (2021) Using a single dose of photobiomodulation (laser + LED) to improve performance of lower limbs in functional test: randomized clinical trial. J Bodyw Mov Ther 28:255–263. https://doi.org/10.1016/j.jbmt.2021.06.024
Brancaccio P, Maffulli N, Limongelli FM (2007) Creatine kinase monitoring in sport medicine. Br Med Bull 81–82:209–230. https://doi.org/10.1093/bmb/ldm014
Ebbeling CB, Clarkson PM (1989) Exercise-induced muscle damage and adaptation. Sports Med 7:207–234. https://doi.org/10.2165/00007256-198907040-00001
Yoshikawa S, Shimada A (2015) Reaction mechanism of cytochrome c oxidase. Chem Rev 115:1936–1989. https://doi.org/10.1021/cr500266a
Molina Correa JC, Padoin S, Varoni PR et al (2022) Ergogenic effects of Photobiomodulation on performance in the 30-Second Wingate Test: a Randomized, Double-Blind, Placebo-Controlled, crossover study. J Strength Cond Res 36:1901–1908. https://doi.org/10.1519/JSC.0000000000003734
Karu TI, Pyatibrat LV, Afanasyeva NI (2005) Cellular effects of low power laser therapy can be mediated by nitric oxide. Lasers Surg Med 36:307–314. https://doi.org/10.1002/lsm.20148
Maegawa Y, Itoh T, Hosokawa T et al (2000) Effects of near-infrared low-level laser irradiation on microcirculation. Lasers Surg Med 27:427–437. https://doi.org/10.1002/1096-9101(2000)27:5<427::AID-LSM1004>3.0.CO;2-A
Schaffer M, Bonel H, Sroka R et al (2000) Effects of 780 nm diode laser irradiation on blood microcirculation: preliminary findings on time-dependent T1-weighted contrast-enhanced magnetic resonance imaging (MRI). J Photochem Photobiol B 54:55–60. https://doi.org/10.1016/s1011-1344(99)00155-4
Newton MJ, Morgan GT, Sacco P et al (2008) Comparison of responses to strenuous eccentric exercise of the elbow flexors between resistance-trained and untrained men. J Strength Cond Res 22:597–607. https://doi.org/10.1519/JSC.0b013e3181660003
Leal-Junior ECP, Lopes-Martins RÁB, Bjordal JM (2019) Clinical and scientific recommendations for the use of photobiomodulation therapy in exercise performance enhancement and post-exercise recovery: current evidence and future directions. Braz J Phys Ther 23:71–75. https://doi.org/10.1016/j.bjpt.2018.12.002
Markus I, Constantini K, Hoffman JR et al (2021) Exercise-induced muscle damage: mechanism, assessment and nutritional factors to accelerate recovery. Eur J Appl Physiol 121:969–992. https://doi.org/10.1007/s00421-020-04566-4
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, BM., Qiu, DY., Ni, PS. et al. Can pre-exercise photobiomodulation improve muscle endurance and promote recovery from muscle strength and injuries in people with different activity levels? A meta-analysis of randomized controlled trials. Lasers Med Sci 39, 132 (2024). https://doi.org/10.1007/s10103-024-04079-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10103-024-04079-y