Abstract
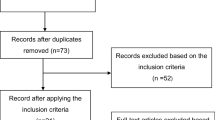
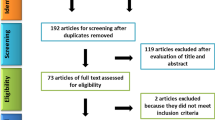
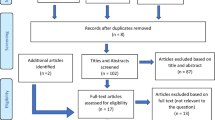
This systematic review assessed if photobiomodulation of human dental pulp tissue improved cell viability, proliferation, and/or differentiation compared with a placebo. This systematic review was conducted in line with PRISMA. PICO question was established; inclusion and exclusion criteria were established before a search had begun. A literature search was conducted through PubMed, Scopus, and Cochrane. Studies were included if published within the last 20 years in English language, or where translation was available; laser parameters were mentioned; human dental pulp tissue was studied in vitro. Studies were excluded if non-human dental pulp tissue was studied and where the study was an in vivo study. Out of the total 121 studies found, 109 were excluded. Of the twelve included studies, three full-text articles were not available despite attempts made to contact the respective authors, leaving nine studies. Four of the included studies reported the use of stem cells derived from human deciduous teeth (SHEDs), and five used those from human permanent teeth (DPSCs). Most included studies utilized InGaAlP laser with wavelengths 660 nm, and one study with 610 nm. Other types of lasers included LED InGaN, and GaAlAs. Out of all included studies, two had a moderate risk of bias, and the rest had a low risk of bias. All studies confirmed positive effects on proliferation. One study also found improved osteogenic differentiation of the stem cells derived from stem cells of deciduous teeth. After assessing SHEDs and DPSCs separately, it is found that photobiomodulation improved cell proliferation in both subgroups. Due to heterogeneity in design protocols and laser parameters, it was not possible to compare the studies together. However, this study indicated that cell viability and proliferation did improve with photobiomodulation.

Similar content being viewed by others
References
Neel EAA, Chrzanowski W, Salih VM, Kim HW, Knowles JC (2014) Tissue engineering in dentistry. J Dent 42(8):915–928 [cited 2019 Sep 11]
Diniz IMA, Carreira ACO, Sipert CR et al (2018) Photobiomodulation of mesenchymal stem cells encapsulated in an injectable rhBMP4-loaded hydrogel directs hard tissue bioengineering. J Cell Physiol 233(6):4907–4918
Kunimatsu R, Nakajima K, Awada T, Tsuka Y, Abe T, Ando K et al (2018) Comparative characterization of stem cells from human exfoliated deciduous teeth, dental pulp, and bone marrow-derived mesenchymal stem cells. Biochem Biophys Res Commun 501(1):193–198 [cited 2019 Sep 11]
Marques MM, Miyagi de Cara SPH, Abe GL, Lima PLV, Moreira MS (2016) Photobiomodulation of dental derived mesenchymal stem cells: a systematic review. Photomed Laser Surg 34(11):1–9 [cited 2019 Sep 11]
Farhani AB (2016) Effect of low-level laser irradiation on proliferation of human dental mesenchymal stem cells: a systematic review. J Photochem Photobiol B 162:577–582 [cited 2019 Sep 11]
Staffoli S, Romeo U, Amorim RNS, Migliau G, Palaia G, Resende L et al (2017) The effects of low level laser irradiation on proliferation of human dental pulp: a narrative review. Clin Ter 168(5):320–326 [cited 2019 Sep 11]
Higgins J, Green S (2011) Cochrane Handbook for Systematic Reviews of Interventions. The Cochrane Collaboration. [cited 2019 Sep 11]; Available from: www.cochrane-handbook.org [accessed 3 February 2013]
IOM (Institute of Medicine) (2011) Finding what works in health care: Standards for systematic reviews. The National Academies Press, Washington, DC, p 318 [cited 2019 Oct 3]. Available at: http://www.nap.edu/openbook.php?record_id=13059
Viswanathan M, Ansari M, Berkman ND, Chang S, Hartling L, McPheeters LM et al (2013) Assessing risk of bias and confounding in observational studies of interventions or exposures: further development of the RTI item bank. Agency for Healthcare Research and Quality (AHRQ) 13 [cited 2019 Sep 11]. Available at: http://www.effectivehealthcare.ahrq.gov/ehc/products/414/1612/RTI-item-bank-bias-precision-130805.pdf
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) The PRISMA Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med 6(7):e1000097 [cited 2019 Sep 11]
Montoro LA, Turrioni AP, Basso FG, de Souza Costa CA, Hebling J (2014) Infrared LED irradiation photobiomodulation of oxidative stress in human dental pulp cells. Int Endod J 47(8):747–755 [cited 2019 Sep 11]
Eduardo Fde P, Bueno DF, de Freitas PM, Marques MM, Passos-Bueno MR, Eduardo Cde P et al (2008) Stem cell proliferation under low intensity laser irradiation: a preliminary study. Lasers Surg Med 40(6):433–438 [cited 2019 Sep 11]
Zaccara IV, Ginani F, Mota-Filho HG, Henriques ACG, Barboza CAG (2015) Effect of low-level laser irradiation on proliferation and viability of human dental pulp stem cells. J Lasers Med Sci 30:2259–2264 [cited 2019 Sep 11]
Tabatabaei FS, Torshabi M, Nasab MM, Khosraviani K, Khojasteh A (2015) Effect of low-level diode laser on proliferation and osteogenic differentiation of dental pulp stem cells. Laser Phys 25 [cited 2019 Sep 11]
Moura-Netto C, Ferreira LS, Maranduba CM, Mello-Moura ACV, Marques MM (2016) Low-intensity laser phototherapy enhances the proliferation of dental pulp stem cells under nutritional deficiency. Braz Oral Res 30(1) [cited 2019 Sep 11]
Marques NCT, Neto NL, Prado MTO, Vitor LLR, Oliveira RC, Sakai VT et al (2017) Effects of PBM in different energy densities and irradiance on maintaining cell viability and proliferation of pulp fibroblasts from human primary teeth. J Lasers Med Sci 32(7):1621–1628 [cited 2019 Sep 11]
Kim HB, Baik KY, Choung PH, Chung JH (2017) Pulse frequency dependency of photobiomodulation on the bioenergetic functions of human dental pulp stem cells. Sci Rep 7(1):15927 [cited 2019 Sep 11]
Pinheiro CCG, de Pinho MC, Aranha AC, Fregnani E, Bueno DF, Low Power Laser Therapy (2018) A strategy to promote the osteogenic differentiation of deciduous dental pulp stem cells from cleft lip and palate patients. Tissue Eng A 24(7–8):569–575 [cited 2019 Sep 11]
Sivakumar TT, Muruppel AM, Joseph AP, Reshmi JA, Ramachandran R, Nair PD et al (2019) Photobiomodulatory effect delivered by low-level laser on dental pulp stem cell differentiation for osteogenic lineage. Laser Dent Sci 3:175 [cited 2019 Sep 11]
Ferreira MP, Ferrari RA, Gravalos ED, Martins MD, Bussadori SK, Gonzalez DA et al (2009) Effect of low-energy gallium-aluminum-arsenide and aluminium gallium indium phosphide laser irradiation on the viability of C2C12 myoblasts in a muscle injury model. Photomed Laser Surg 27(6):901–906 [cited 2019 Sep 11]
Heiskanen V, Hamblin MR (2018) Photobiomodulation: lasers vs. light emitting diodes. Photochem Photobiol Sci 17(8):1003–1017 [cited 2019 Sep 11]
Hashmi JT, Huang YY, Sharma SK, Kurup DB, De Taboada L, Carroll JD et al (2010) Effect of pulsing in low-level light therapy. Lasers Surg Med 42:450–466 [cited 2019 Sep 19]
Public health England (2017) Passage numbers explained. European Collection of Authenticated Cell Cultures. [cited 2019 Sep 12]. Available at: https://www.phe-culturecollections.org.uk/products/celllines/generalcell/detail.jsp?refId=92020424&collection=ecacc_gc
Gerschman JA, Ruben J, Gebart-Eaglemont J (1994) Low level laser therapy for dentinal tooth hypersensitivity. Aust Dent J 39:353–357 [cited 2019 Sep 11]
Pereira LO, Longo JP, Azevedo RB (2012) Laser irradiation did not increase the proliferation or the differentiation of stem cells from normal and inflamed dental pulp. Arch Oral Biol 57(8):1079–1085 [cited 2019 Sep 11]
Wang Y, Huang Y, Wang Y, Lyu P, Hamblin MR (2017) Red (660 nm) or near-infrared (810 nm) photobiomodulation stimulates, while blue (415 nm), green (540 nm) light inhibits proliferation in human adipose-derived stem cells. Sci Rep 7:7781 [cited 2020 May 5]
Zein R, Selting W, Hamblin MR (2018) Review of light parameters and photobiomodulation efficacy: dive into complexity. J Biomed Opt 23(12):120901 [cited 2020 May 5]
Sunil PM, Manikandan R, Muthumurugan M, Yoithapprabhunath TR, Sivakumar M (2015) Harvesting dental stem cells – overview. J Pharm Bioallied Sci 7(2):384–386 [cited 2019 Sep 11]
Milward MR, Hadis MA, Cooper PR, Gorecki P, Carroll JD, Palin W (2015) Biomodulatory effects of laser irradiation on dental pulp cells in vitro. Proc SPIE 9309:930908–930901 [cited 2019 Sep 11]
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kulkarni, S., Meer, M. & George, R. The effect of photobiomodulation on human dental pulp–derived stem cells: systematic review. Lasers Med Sci 35, 1889–1897 (2020). https://doi.org/10.1007/s10103-020-03071-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-020-03071-6