Abstract
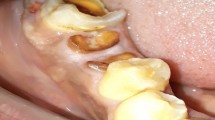
Bone remodeling results in loss of alveolar bone height and thickness. Photobiomodulation (PBM) based on photochemical stimulation by low-intensity lasers emerges as an adjunctive therapy for alveolar socket preservation. Our study aimed to evaluate the effects of PBM therapy on alveolar bone repair. Twenty healthy patients in need of bilateral extraction of lower molars were enrolled in this split-mouth randomized and blind clinical trial. The extraction sites were randomly selected to receive either the PBM therapy with a CW GaAIAs diode laser (808 nm; 0.028 mm2; 0.1 W; 3.6 W/cm2; 89 J/cm2; 2.5 J/point) or no treatment (Control). Bone biopsies were harvested 45 days after the dental extraction and evaluated using micro-computerized tomography (μCT), morphometric, and histological analysis. Data were compared using the paired t test, and the level of significance was set at 5%. Bone surface (p = 0.029), bone surface/total volume (p = 0.028), trabecular number (p = 0.025), and connectivity density (p = 0.029) were higher at the PBM group compared with Control. The histological observations confirmed the μCT findings. PBM samples exhibited higher number of organized and connected bone trabeculae along with higher density of blood vessels than Control. Control samples displayed a dense and highly cellular connective tissue at the central area accompanied by the presence of immature bone trabeculae at the periphery. Our results indicated that the PBM therapy improved the newly bone trabeculae formation and their connectivity which increased bone surface, indicating the positive effect of the laser on alveolar human socket repair.





Similar content being viewed by others
References
Park JB, Ahn SJ, Kang YG, Kim EC, Heo JS, Kang KL (2015) Effects of increased low-level diode laser irradiation time on extraction socket healing in rats. Lasers Med Sci 30:719–726. https://doi.org/10.1007/s10103-013-1402-6
Cardaropoli G, Araújo MG, Lindhe J (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol 30:809–818
Cohen N, Cohen-Lévy J (2014) Healing processes following tooth extraction in orthodontic cases. J Dentofacial Anom Orthod 17:304. https://doi.org/10.1051/odfen/2014006
Pietrokovski J, Massler M (1967) Alveolar ridge resorption following tooth extraction. J Prosthet Dent 17:21–27
Schropp L, Wenzel A, Kostopoulos L, Karring T (2003) Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 23:313–323
Hammerle CH, Araujo MG, Simion M (2012) Evidence-based knowledge on the biology and treatment of extraction sockets. Clin Oral Implants Res 23(Suppl 5):80–82. https://doi.org/10.1111/j.1600-0501.2011.02370.x
Klokkevold PR, Han TJ (2007) How do smoking, diabetes, and periodontitis affect outcomes of implant treatment? Int J Oral Maxillofac Implants 22(Suppl):173–202
Atieh MA, Alsabeeha NH, Payne AG, Duncan W, Faggion CM, Esposito M (2015) Interventions for replacing missing teeth: alveolar ridge preservation techniques for dental implant site development. Cochrane Database Syst Rev 28:CD010176. https://doi.org/10.1002/14651858.CD010176.pub2
Vignoletti F, Matesanz P, Rodrigo D, Figuero E, Martin C, Sanz M (2012) Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clin Oral Implants Res 5:22–38. https://doi.org/10.1111/j.1600-0501.2011.02331.x
Fee L (2017) Socket preservation. Br Dent J 21:579–582. https://doi.org/10.1038/sj.bdj.2017.355
Troiano G, Zhurakivska K, Lo Muzio L, Laino L, Cicciù M, Russo L (2017) Combination of bone graft and resorbable membrane for alveolar ridge preservation: a systematic review, meta-analysis and trial sequential analysis. J Periodontol 12:1–17. https://doi.org/10.1902/jop.2017.170241
Baumer D, Zuhr O, Rebele S, Hurzeler M (2017) Socket shield technique for immediate implant placement - clinical, radiographic and volumetric data after 5 years. Clin Oral Implants Res 28:1450–1458. https://doi.org/10.1111/clr.13012
Annunziata M, Guida L, Nastri L, Piccirillo A, Sommese L, Napoli C (2018) The role of autologous platelet concentrates in alveolar socket preservation: a systematic review. Transf Med Hemother 45:195–203. https://doi.org/10.1159/000488061
Ozawa Y, Shimizu N, Kariya G, Abiko Y (1998) Low-energy laser irradiation stimulates bone nodule formation at early stages of cell culture in rat calvarial cells. Bone 22:347–354
Petri AD, Teixeira LN, Crippa GE, Beloti MM, de Oliveira PT, Rosa AL (2010) Effects of low-level laser therapy on human osteoblastic cells grown on titanium. Braz Dent J 21:491–498
Fujihara NA, Hiraki NRN, Marques MM (2006) Irradiation at 780 nm increases proliferation rate of osteoblasts independently of dexamethasone presence. Lasers Surg Med 38:332–336. https://doi.org/10.1002/lsm.20298
Kawasaki K, Shimizu N (2000) Effects of low-energy laser irradiation on bone remodeling during experimental tooth movement in rats. Lasers Surg Med 26:282–291
Shirazi M, Akhoundi MSA, Javadi E, Kamali A, Motahhari P, Rashidpour M, Chiniforush N (2015) The effects of diode laser (660 nm) on the rate of tooth movements: an animal study. Lasers Med Sci 30:713–718. https://doi.org/10.1007/s10103-013-1407-1
Kesler G, Romanos G, Koren R (2006) Use of Er:YAG laser to improve osseointegration of titanium alloy implants--a comparison of bone healing. Int J Oral Maxillofac Implants 21:375–379
Jonasson TH, Zancan R, de Oliveira-Azevedo L, Fonseca AC, Silva MCD, Giovanini AF, Zielak JC, Araujo MR (2017) Effects of low-level laser therapy and platelet concentrate on bone repair: histological, histomorphometric, immunohistochemical, and radiographic study. J Craniomaxillofac Surg 45:1846–1853. https://doi.org/10.1016/j.jcms.2017.08.008
Angeletti P, Pereira MD, Gomes HC, Hino CT, Ferreira LM (2010) Effect of low-level laser therapy (GaAlAs) on bone regeneration in midpalatal anterior suture after surgically assisted rapid maxillary expansion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:e38–e46. https://doi.org/10.1016/j.tripleo.2009.10.043
Avila-Ortiz G, Elangovan S, Kramer KW, Blanchette D, Dawson DV (2014) Effect of alveolar ridge preservation after tooth extraction: a systematic review and meta-analysis. J Dent Res 93:950–958. https://doi.org/10.1177/0022034514541127
Romão MMA, Marques MM, Cortes ARG, Horliana ACRT, Moreira MS, Lascala CA (2015) Micro-computed tomography and histomorphometric analysis of human alveolar bone repair induced by laser phototherapy: a pilot study. Int J Oral Maxillofac Surg 44:1521–1528. https://doi.org/10.1016/j.ijom.2015.08.989
Kučcerová H, Dostálová T, Himmlová L, Bártová J, Mazánek J (2000) Low-level laser therapy after molar extraction. J Clin Laser Med Surg 18:309–315
Noba C, Mello-Moura ACV, Gimenez T, Tedesco TK, Moura-Netto C (2018) Laser for bone healing after oral surgery: systematic review. Lasers Med Sci 33:667–674. https://doi.org/10.1007/s10103-017-2400-x
Mozzati M, Martinasso G, Cocero N, Pol R, Maggiora M, Muzio G, Canuto RA (2011) Influence of superpulsed laser therapy on healing processes following tooth extraction. Photomed Laser Surg 29:565–571. https://doi.org/10.1089/pho.2010.2921
Korany NS, Mehanni SS, Hakam HM, El-Maghraby EM (2012) Evaluation of socket healing in irradiated rats after diode laser exposure (histological and morphometric studies). Arch Oral Biol 57:884–891. https://doi.org/10.1016/j.archoralbio.2012.01.009
Kulkarni S, Meer M, George R (2019) Efficacy of photobiomodulation on accelerating bone healing after tooth extraction: a systematic review. Lasers Med Sci 34:685–692. https://doi.org/10.1007/s10103-018-2641-3
Pinheiro AL, Gerbi ME (2006) Photoengineering of bone repair processes. Photomed Laser Surg 24:169–178
AboElsaad NS, Soory M, Gadalla LM, Ragab LI, Dunne S, Zalata KR, Louca C (2009) Effect of soft laser and bioactive glass on bone regeneration in the treatment of infra-bony defects (a clinical study). Lasers Med Sci 24:387–395. https://doi.org/10.1007/s10103-008-0576-9
Pourreau-Schneider N, Soudry M, Remusat M, Franquin JC, Martin PM (1989) Modifications of growth dynamics and ultrastructure after helium-neon laser treatment of human gingival fibroblasts. Quintessence Int 20:887–893
Park JJ, Kang KL (2012) Effect of 980-nm GaAlAs diode laser irradiation on healing of extraction sockets in streptozotocin-induced diabetic rats: a pilot study. Lasers Med Sci 27:223–230. https://doi.org/10.1007/s10103-011-0944-8
Saito S, Shimizu N (1997) Stimulatory effects of low-power laser irradiation on bone regeneration in midpalatal suture during expansion in the rat. Am J Orthod Dentofac Orthop 111:525–532
Amler MH (1969) The time sequence of tissue regeneration in human extraction wounds. Oral Surg Oral Med Oral Pathol 27:309–318
Trombelli L, Farina R, Marzola A, Bozzi L, Liljenberg B, Lindhe J (2008) Modeling and remodeling of human extraction sockets. J Clin Periodontol 35:630–639. https://doi.org/10.1111/j.1600-051X.2008.01246.x
Yamagishi H, Shinohara C, Saito S, Sasaki H, Kanegae H, Shibasaki Y (1994) A basic study on the use of semiconductor laser of penetrative sensitivity on living tissue. J Jpn Soc Laser Dent 5:13–22
Abd-Elaal AZ, El-Mekawii HA, Saafan AM, El Gawad LA, El-Hawary YM, Abdelrazik MA (2015) Evaluation of the effect of low-level diode laser therapy applied during the bone consolidation period following mandibular distraction osteogenesis in the human. Int J Oral Maxillofac Surg 44:989–997. https://doi.org/10.1016/j.ijom.2015.04.010
Paschoal MA, Santos-Pinto L (2012) Therapeutic effects of low-level laser therapy after premolar extraction in adolescents: a randomized double-blind clinical trial. Photomed Laser Surg 30:559–564. https://doi.org/10.1089/pho.2012.3243
Bouxsein ML, Boyd SK, Christiansen BA, Guldberg RE, Jepsen KJ, Müller R (2010) Guidelines for assessment of bone microstructure in rodents using micro-computed tomography. J Bone Miner Res 25:1468–1486. https://doi.org/10.1002/jbmr.141
Scalize PH, de Sousa LG, Regalo SC, Semprini M, Pitol DL, da Silva GA, de Almeida CJ, Coppi AA, Laad AA, Prado KF, Siessere S (2015) Low-level laser therapy improves bone formation: stereology findings for osteoporosis in rat model. Lasers Med Sci 30:1599–1607. https://doi.org/10.1007/s10103-015-1773-y
Pires-Oliveira DA, Oliveira RF, Amadei SU, Pacheco-Soares C, Rocha RF (2010) Laser 904 nm action on bone repair in rats with osteoporosis. Osteoporos Int 21:2109–2114. https://doi.org/10.1007/s00198-010-1183-8
Acknowledgments
The authors would like to thank the Facultad de Odontología de la Universitad Central del Ecuador for financial support. Daniel Uliana and Adriana Almeida are acknowledged for technical assistance during the microtomography evaluations.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures were in accordance with the ethical standards and with the 1964 Helsinki declaration, and were approved by the Ethics Committee for Human Studies (CAAE: 68617217.8.00000.0075) of the School of Dentistry at the University of Sao Paulo.
Statement of informed consent
Oral and written informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised: In the published online paper, the given name and family name of the author Kleber Arturo Vallejo Rosero was interchanged. The correct presentation should be Kleber Arturo Rosero Vallejo.
Rights and permissions
About this article
Cite this article
Rosero, K.A.V., Sampaio, R.M.F., Deboni, M.C.Z. et al. Photobiomodulation as an adjunctive therapy for alveolar socket preservation: a preliminary study in humans. Lasers Med Sci 35, 1711–1720 (2020). https://doi.org/10.1007/s10103-020-02962-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-020-02962-y