Abstract
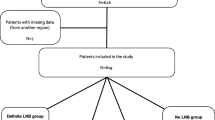
We aimed to describe the clinical characteristics, management, and residual symptoms (RS) in patients with definite and possible Lyme neuroborreliosis (LNB). We conducted a retrospective French multicenter cohort study (2010–2020). Cases of LNB were defined as clinical manifestations attributed to LNB and a positive Borrelia-specific intrathecal antibody index (AI) (“possible” LNB) and with pleocytosis (“definite” LNB). Risk factors of RS were determined using a logistic regression model. We included 138 adult patients with a positive AI. Mean age was 59.5 years (± 14.7). The median duration of symptoms before diagnosis was 1.0 [0.5–4.0] months. The most frequent manifestation was radicular pain (n = 79, 57%). Complete cerebrospinal fluid (CSF) leukocyte analysis was available in 131 patients, of whom 72 (55%) had pleocytosis. Patients with definite LNB had a shorter duration of symptoms (median 1.0 [0.5–2.6] vs. 3.0 [0.6–7.0] months, p < 0.01) and more radicular pain (74% vs 44%, p < 0.01) than patients with possible LNB. At the last visit (median duration of follow-up: 70 [30–175] days), 74/124 patients (59.7%) reported RS, mostly radicular pain (n = 31, 25%). In multivariate analysis, definite LNB (OR = 0.21 [0.05–0.931], p = 0.039) and duration of symptoms less than 3 months (OR = 0.04 [0.01–0.37], p = 0.005) were protective factors against RS at last follow-up. Our study highlights the challenges of LNB management, especially for patients with a positive AI without pleocytosis, questioning whether LB is still ongoing or not. Early diagnosis and treatment are important to improve outcomes and to lower potential RS.


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available but are available from the corresponding author on reasonable request.
Code availability
SPSS 22.0 (IBM, Armonk, NY, USA).
References
Stanek G, Fingerle V, Hunfeld K-P, Jaulhac B, Kaiser R, Krause A et al (2011) Lyme borreliosis: clinical case definitions for diagnosis and management in Europe. Clin Microbiol Infect 1(17):69–79. https://doi.org/10.1111/j.1469-0691.2010.03175.x
Borréliose de Lyme : données épidémiologiques 2020 [Internet]. [cited 2021 9]; https://www.santepubliquefrance.fr/les-actualites/2021/borreliose-de-lyme-donnees-epidemiologiques-2020. Accessed 18 June 2022
Septfons A, Goronflot T, Jaulhac B, Roussel V, De Martino S, Guerreiro S et al (2019) Epidemiology of Lyme borreliosis through two surveillance systems: the national Sentinelles GP network and the national hospital discharge database, France, 2005 to 2016. Euro Surveill 24:1800134. https://doi.org/10.2807/1560-7917.ES.2019.24.11.1800134
Hansen K, Lebech AM (1992) The clinical and epidemiological profile of Lyme neuroborreliosis in Denmark 1985–1990. A prospective study of 187 patients with Borrelia burgdorferi specific intrathecal antibody production. Brain 115(Pt 2):399–423. https://doi.org/10.1093/brain/115.2.399
Halperin JJ (2017) Neuroborreliosis. J Neurol 264:1292–1297. https://doi.org/10.1007/s00415-016-8346-2
Hammers-Berggren S, Hansen K, Lebech A-M, Karlsson M (1993) Borrelia burgdorferi-specific intrathecal antibody production in neuroborreliosis: a follow-up study. Neurology 1(43):169–169. https://doi.org/10.1212/WNL.43.1_Part_1.169
Kaiser R (1994) Variable CSF findings in early and late Lyme neuroborreliosis: a follow-up study in 47 patients. J Neurol 242:26–36. https://doi.org/10.1007/BF00920571
Rauer S, Kastenbauer S, Hofmann H, Fingerle V, Huppertz H-I, Hunfeld K-P et al (2020) Guidelines for diagnosis and treatment in neurology—Lyme neuroborreliosis. Ger Med Sci 18:Doc3. https://doi.org/10.3205/000279
Dersch R, Sommer H, Rauer S, Meerpohl JJ (2016) Prevalence and spectrum of residual symptoms in Lyme neuroborreliosis after pharmacological treatment: a systematic review. J Neurol 263:17–24. https://doi.org/10.1007/s00415-015-7923-0
Charlson M, Szatrowski TP, Peterson J, Gold J (1994) Validation of a combined comorbidity index. J Clin Epidemiol 47:1245–1251. https://doi.org/10.1016/0895-4356(94)90129-5
Reiber H, Lange P (1991) Quantification of virus-specific antibodies in cerebrospinal fluid and serum: sensitive and specific detection of antibody synthesis in brain. Clin Chem 37:1153–1160
Figoni J, Chirouze C, Hansmann Y, Lemogne C, Hentgen V, Saunier A et al (2019) Lyme borreliosis and other tick-borne diseases. Guidelines from the French Scientific Societies (I): prevention, epidemiology, diagnosis. Med Mal Infect 49:318–34. https://doi.org/10.1016/j.medmal.2019.04.381
Knudtzen FC, Andersen NS, Jensen TG, Skarphédinsson S (2017) Characteristics and clinical outcome of Lyme neuroborreliosis in a high endemic area, 1995–2014: a retrospective cohort study in Denmark. Clin Infect Dis 16(65):1489–1495. https://doi.org/10.1093/cid/cix568
Nordberg CL, Bodilsen J, Knudtzen FC, Storgaard M, Brandt C, Wiese L et al (2020) Lyme neuroborreliosis in adults: a nationwide prospective cohort study. Ticks Tick-borne Dis 11:101411. https://doi.org/10.1016/j.ttbdis.2020.101411
Ogrinc K, Lusa L, Lotrič-Furlan S, Bogovič P, Stupica D, Cerar T et al (2016) Course and outcome of early European Lyme neuroborreliosis (Bannwarth syndrome): clinical and laboratory findings. Clin Infect Dis 1(63):346–353. https://doi.org/10.1093/cid/ciw299
Schwenkenbecher P, Pul R, Wurster U, Conzen J, Pars K, Hartmann H et al (2017) Common and uncommon neurological manifestations of neuroborreliosis leading to hospitalization. BMC Infect Dis 17:90. https://doi.org/10.1186/s12879-016-2112-z (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5251276/)
Ogrinc K, Kastrin A, Lotrič-Furlan S, Bogovič P, Rojko T, Maraspin V et al (2021) Colocalization of radicular pain and erythema migrans in patients with Bannwarth syndrome suggests a direct spread of borrelia into the central nervous system. Clin Infect Dis 4:ciab867. https://doi.org/10.1093/cid/ciab867
Koedel U, Fingerle V, Pfister H-W (2015) Lyme neuroborreliosis—epidemiology, diagnosis and management. Nat Rev Neurol 11:446–456. https://doi.org/10.1038/nrneurol.2015.121
Ursinus J, Vrijmoeth HD, Harms MG, Tulen AD, Knoop H, Gauw SA et al (2021) Prevalence of persistent symptoms after treatment for Lyme borreliosis: a prospective observational cohort study. Lancet Reg Health Eur 6:100142. https://doi.org/10.1016/j.lanepe.2021.100142
Eikeland R, Mygland Å, Herlofson K, Ljøstad U (2013) Risk factors for a non-favorable outcome after treated European neuroborreliosis. Acta Neurol Scand 127:154–160. https://doi.org/10.1111/j.1600-0404.2012.01690.x
Ljøstad U, Mygland Å (2010) Remaining complaints 1 year after treatment for acute Lyme neuroborreliosis; frequency, pattern and risk factors. Eur J Neurol 17:118–123. https://doi.org/10.1111/j.1468-1331.2009.02756.x
Cepok S, Zhou D, Vogel F, Rosche B, Grummel V, Sommer N et al (2003) The immune response at onset and during recovery from Borrelia burgdorferi meningoradiculitis. Arch Neurol 60:849–855. https://doi.org/10.1001/archneur.60.6.849
Mygland A, Ljøstad U, Fingerle V, Rupprecht T, Schmutzhard E, Steiner I et al (2010) EFNS guidelines on the diagnosis and management of European Lyme neuroborreliosis. Eur J Neurol 17(8–16):e1-4. https://doi.org/10.1111/j.1468-1331.2009.02862.x
Krüger H, Pulz M, Martin R, Sticht-Groh V (1990) Long-term persistence of specific T- and B-lymphocyte responses to Borrelia burgdorferi following untreated neuroborreliosis. Infection 18:263–267. https://doi.org/10.1007/BF01646998
Jaulhac B, Saunier A, Caumes E, Bouiller K, Gehanno JF, Rabaud C et al (2019) Lyme borreliosis and other tick-borne diseases. Guidelines from the French scientific societies (II). Biological diagnosis, treatment, persistent symptoms after documented or suspected Lyme borreliosis. Med Mal Infect 49:335–46. https://doi.org/10.1016/j.medmal.2019.05.001
Ljøstad U, Skogvoll E, Eikeland R, Midgard R, Skarpaas T, Berg A et al (2008) Oral doxycycline versus intravenous ceftriaxone for European Lyme neuroborreliosis: a multicentre, non-inferiority, double-blind, randomised trial. Lancet Neurol 7:690–695. https://doi.org/10.1016/S1474-4422(08)70119-4
Solheim AM, Lorentzen ÅR, Dahlberg AO, Flemmen HØ, Brune S, Forselv KJN et al (2022) Six versus 2 weeks treatment with doxycycline in European Lyme neuroborreliosis: a multicentre, non-inferiority, double-blinded, randomised and placebo-controlled trial. J Neurol Neurosurg Psychiatry 27(93):1222–1228. https://doi.org/10.1136/jnnp-2022-329724
Résultats du contrôle du marché des réactifs de sérologie de la borréliose de lyme—ANSM [Internet]. [cited 2022 20]; https://ansm.sante.fr/page/resultats-du-controle-du-marche-des-reactifs-de-serologie-de-la-borreliose-de-lyme. Accessed 18 June 2022
Author information
Authors and Affiliations
Contributions
PN: investigation, writing—original draft preparation; AR: conceptualization, investigation, writing – original draft preparation, resources; SZ: investigation, resources, writing—reviewing and editing; TK: resources, writing—reviewing and editing; EB: resources, writing—reviewing and editing; MM: resources, writing—reviewing and editing; LP: resources, writing—reviewing and editing; EC: resources, writing—reviewing and editing; CC: conceptualization, resources, writing—reviewing and editing; KB: conceptualization, resources, supervision, formal analysis, writing—reviewing and editing.
Corresponding authors
Ethics declarations
Ethics approval
This is an observational study. The University of Besancon Research Ethics Committee has confirmed that no ethical approval is required.
Consent to participate
Informed consent was collected from all patients in conformity with the French national ethical guidelines.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pauline Naudion and Alice Raffetin participated equally in this work as first co-authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Naudion, P., Raffetin, A., Zayet, S. et al. Positive intrathecal anti-Borrelia antibody synthesis: what are the implications for clinical practice? Clinical features and outcomes of 138 patients in a French multicenter cohort study. Eur J Clin Microbiol Infect Dis 42, 441–452 (2023). https://doi.org/10.1007/s10096-023-04574-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-023-04574-0