Abstract
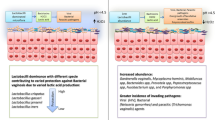
The vaginal composition of African women is more often lactobacillus-deficient compared to that of women from other areas around the world. Lactobacillus-deficient microflora is a known risk factor for serious health problems, such as preterm birth, cervix cancer, and entrapment of human immunodeficiency virus (HIV) and other sexually transmitted infections (STIs). The aim of this study was to assess the effect of local vaginal antibiotic or antiseptic treatment on abnormal vaginal flora (AVF), aerobic vaginitis (AV), and bacterial vaginosis (BV) among women in rural, semi-urban, and urban areas in Uganda, as compared to placebo. In a double-blind, placebo-controlled, randomized trial, 300 women presenting for outpatient routine, follow-up, or medical care at Mulago Hospital in Kampala, Uganda, were enrolled to receive 6 days of treatment with vaginal rifaximin (RFX), dequalinium chloride (DQC), or placebo if they had an increased vaginal pH of >4.5 as determined by self-testing. At initial visit and at control visit after 4 weeks, a smear was taken for blinded wet mount microscopy to determine AVF, BV, AV, and Candida severity scores. As compared to placebo, both RFX or DQC treatments dramatically diminished BV prevalence and severity from the initial to follow-up visit: the BV score declined from 2.5 to 1.6 (p < 0.0001) and from 2.5 to 1.9 (p < 0.0001), respectively. Similarly, strong improvements in the AV score were seen in both treatment regimens: moderate and severe AV declined from AV scores of 6.3 to 3.6 (p = 0.003) and from 6.6 to 4.1 (p < 0.004), respectively. Also, women with AVF (deceased or absent lactobacilli) showed similar improvements when compared with placebo. Women with normal flora and Candida at the initial visit showed less Candida after 4 weeks in the group treated with DQC (p = 0.014). Even after a short duration of intravaginal treatment with local non-absorbable antiseptics or antibiotics produced significant, lasting improvements in the vaginal microbiome composition of women with disturbed vaginal microflora. As African women have high prevalences of BV, AV, and AVF, this approach could improve their odds to prevent health-compromising complications. Further studies assessing direct health outcomes are needed to substantiate this.


Similar content being viewed by others
References
Donders GG, Caeyers T, Tydhof P, Riphagen I, van den Bosch T, Bellen G (2007) Comparison of two types of dipsticks to measure vaginal pH in clinical practice. Eur J Obstet Gynecol Reprod Biol 134(2):220–224
Donders GG, Guaschino S, Peters K, Tacchi R, Lauro V; VARIANT 1 Study Group (2013) A multicenter, double-blind, randomized, placebo-controlled study of rifaximin for the treatment of bacterial vaginosis. Int J Gynaecol Obstet 120:131–136
Cruciani F, Brigidi P, Calanni F, Lauro V, Tacchi R, Donders G et al (2012) Efficacy of rifaximin vaginal tablets in treatment of bacterial vaginosis: a molecular characterization of the vaginal microbiota. Antimicrob Agents Chemother 56(8):4062–4070
Cruciani F, Wasinger V, Turroni S, Calanni F, Donders G, Brigidi P et al (2013) Proteome profiles of vaginal fluids from women affected by bacterial vaginosis and healthy controls: outcomes of rifaximin treatment. J Antimicrob Chemother 68(11):2648–2659
Laghi L, Picone G, Cruciani F, Brigidi P, Calanni F, Donders G et al (2014) Rifaximin modulates the vaginal microbiome and metabolome in women affected by bacterial vaginosis. Antimicrob Agents Chemother 58(6):3411–3420
Weissenbacher ER, Donders G, Unzeitig V, Martinez de Tejada B, Gerber S, Halaška M et al (2012) A comparison of dequalinium chloride vaginal tablets (Fluomizin®) and clindamycin vaginal cream in the treatment of bacterial vaginosis: a single-blind, randomized clinical trial of efficacy and safety. Gynecol Obstet Invest 73(1):8–15
Donders GG, Andabati G, Donders F, Michiels T, Eggermont N, Bellen G et al (2012) Acceptance of self-testing for increased vaginal Ph in different subsets of Ugandan women. Int J STD AIDS 23(1):30–35
Donders GG, Marconi C, Bellen G, Donders F, Michiels T (2014) Effect of short training on vaginal fluid microscopy (wet mount) learning. J Low Genit Tract Dis 19(2):165–169
Donders GG, Vereecken A, Bosmans E, Dekeersmaecker A, Salembier G, Spitz B (2002) Definition of a type of abnormal vaginal flora that is distinct from bacterial vaginosis: aerobic vaginitis. BJOG 109(1):34–43
Donders GG (2007) Definition and classification of abnormal vaginal flora. Best Pract Res Clin Obstet Gynaecol 21(3):355–373
Jespers V, Crucitti T, van de Wijgert J, Vaneechoutte M, Delany-Moretlwe S, Mwaura M et al (2016) A DNA tool for early detection of vaginal dysbiosis in African women. Res Microbiol 167(2):133–141
van de Wijgert J, Altini L, Jones H, de Kock A, Young T, Williamson A et al (2006) Two methods of self-sampling compared to clinician sampling to detect reproductive tract infections in Gugulethu, South Africa. Sex Transm Dis 33(8):516–523
Jespers V, van de Wijgert J, Cools P, Verhelst R, Verstraelen H, Delany-Moretlwe S et al (2015) The significance of Lactobacillus crispatus and L. vaginalis for vaginal health and the negative effect of recent sex: a cross-sectional descriptive study across groups of African women. BMC Infect Dis 15:115
Pellett Madan R, Masson L, Tugetman J, Werner L, Grobler A, Mlisana K et al (2015) Innate antibacterial activity in female genital tract secretions is associated with increased risk of HIV acquisition. AIDS Res Hum Retroviruses 31:1153−1159
Cohen CR, Lingappa JR, Baeten JM, Ngayo MO, Spiegel CA, Hong T et al (2012) Bacterial vaginosis associated with increased risk of female-to-male HIV-1 transmission: a prospective cohort analysis among African couples. PLoS Med 9(6):e1001251
Balkus JE, Richardson BA, Rabe LK, Taha TE, Mgodi N, Kasaro MP et al (2014) Bacterial vaginosis and the risk of trichomonas vaginalis acquisition among HIV-1-negative women. Sex Transm Dis 41(2):123–128
Chohan V, Baeten JM, Benki S, Graham SM, Lavreys L, Mandaliya K et al (2009) A prospective study of risk factors for herpes simplex virus type 2 acquisition among high-risk HIV-1 seronegative women in Kenya. Sex Transm Infect 85(7):489–492
Mastromarino P, Di Pietro M, Schiavoni G, Nardis C, Gentile M, Sessa R (2014) Effects of vaginal lactobacilli in chlamydia trachomatis infection. Int J Med Microbiol 304(5–6):654–661
Marconi C, Donders GG, Martin LF, Ramos BR, Duarte MT, Parada CM et al (2011) Chlamydial infection in a high risk population: association with vaginal flora patterns. Arch Gynecol Obstet 285(4):1013–1018
Foxman B, Wen A, Srinivasan U, Goldberg D, Marrs CF, Owen J et al (2014) Mycoplasma, bacterial vaginosis-associated bacteria BVAB3, race, and risk of preterm birth in a high-risk cohort. Am J Obstet Gynecol 210(3):226.e1–226.e7
Choi SJ, Park SD, Jang IH, Uh Y, Lee A (2012) The prevalence of vaginal microorganisms in pregnant women with preterm labor and preterm birth. Ann Lab Med 32(3):194–200
Donders GG, Van Calsteren K, Bellen G, Reybrouck R, Van den Bosch T, Riphagen I et al (2009) Predictive value for preterm birth of abnormal vaginal flora, bacterial vaginosis and aerobic vaginitis during the first trimester of pregnancy. BJOG 116(10):1315–1324
Gao W, Weng J, Gao Y, Chen X (2013) Comparison of the vaginal microbiota diversity of women with and without human papillomavirus infection: a cross-sectional study. BMC Infect Dis 13:271
Vieira-Baptista P, Lima-Silva J, Pinto C, Saldanha C, Beires J, Martinez-De-Oliveira J et al (2016) Bacterial vaginosis, aerobic vaginitis, vaginal inflammation and major Pap smear abnormalities. Eur J Clin Microbiol Infect Dis 35:657–664
Guédou FA, Van Damme L, Mirembe F, Solomon S, Becker M, Deese J et al (2012) Intermediate vaginal flora is associated with HIV prevalence as strongly as bacterial vaginosis in a cross-sectional study of participants screened for a randomised controlled trial. Sex Transm Infect 88(7):545–551
Donders G, Bellen G, Rezeberga D (2011) Aerobic vaginitis in pregnancy. BJOG 118(10):1163–1170
Donders GG, Zodzika J, Rezeberga D (2014) Treatment of bacterial vaginosis: what we have and what we miss. Expert Opin Pharmacother 15(5):645–657
Acknowledgments
The authors sincerely thank the collaborating nurses and midwives at Mulago University Hospital, Kampala, for their ever-lasting efforts to motivate and help the patients with the questionnaires and practical organization of the study visits.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No official grant was obtained for this study. Femicare, a non-profit organization based in Tienen, Belgium, provided the lab support and covered the travel and accommodation fees of the co-investigators. Both study products and their corresponding placebos were kindly donated by Alfa Wasserman and Medinova, respectively.
Conflict of interest
None of the authors has any competing interests to disclose. Prof. G. Donders was a scientific consultant for both Alfa Wasserman, Bologna, Italy, and Medinova, Zürich, Switzerland.
Ethical approval
Protocol revised and approved by Kampala University Hospital Ethical Committee.
Informed consent
Every patient received information and signed written informed consent in full accordance with Good Clinical Practice (GCP), all applicable subject privacy requirements, and the guiding principles of the Declaration of Helsinki.
Rights and permissions
About this article
Cite this article
Donders, G., Bellen, G., Donders, F. et al. Improvement of abnormal vaginal flora in Ugandan women by self-testing and short use of intravaginal antimicrobials. Eur J Clin Microbiol Infect Dis 36, 731–738 (2017). https://doi.org/10.1007/s10096-016-2856-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-016-2856-9