Abstract
Mirror therapy is a commonly used rehabilitation intervention in post stroke upper limb rehabilitation. Despite many potential technological developments, mirror therapy is routinely delivered through the use of a static mirror or mirror box. This review aims to synthesise evidence on the application of immersive virtual reality mirror therapy (IVRMT) in poststroke upper limb rehabilitation. A scoping review was performed on relevant English studies published between 2013 to 2023. Literature search was undertaken on APA PsycInfo, CINAHL, Cochrane Library, MEDLINE, PubMed and Web of Science between August 5 and 17, 2023. Additional studies were included from Google Scholar and reference lists of identified articles. A total of 224 records were identified, of which 8 full-text articles were selected for review. All included studies were published between 2019 and 2023, and from high- and upper-middle-income nations. All the studies were experimental (n = 8). The total sample size in the studies was 259, most of whom were stroke patients with upper limb weakness (n = 184). This review identified three major themes and two sub-themes based on the contents of the studies conducted on the application of IVRMT: IVRMT’s technical application, feasibility and impact on clinical outcomes (motor recovery and adverse events). IVRMT was concluded to be a safe and feasible approach to post-stroke upper limb rehabilitation, offering enhanced engagement and motor recovery. However, more methodologically robust studies should be conducted to advance this area of practice, and to include a uniform IVRMT intervention protocol, dose, and use of outcome measure.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In recent years, mirror box therapy has played an important part in the interventions offered by the healthcare provider in upper limb rehabilitation after stroke. Mirror therapy involves the use of a mirror that reflects the image of the unaffected upper limb in a way that the affected upper limb is visually replaced by its mirror image [1]. The mirror is positioned along the patient’s midsagittal plane and enables simple exercises and functional tasks with the unaffected upper limb to be performed while looking at the mirror. In this way, a visual illusion of the unaffected upper limb is created in place of the affected limb [2]. This visual illusion is believed to rewire neural connections in the brain [3] following repeated performance and exposures, and consequently can improve motor functioning of upper limbs in patients with stroke. Evidence from a Cochrane review also showed that mirror therapy had a significant positive effect on motor function and motor impairment and was found effective in improving pain and enhancing activities of daily living. However, it has been found that stroke patients’ adherence to mirror therapy across the treatment continuum has been observed to decline over time [4, 5]. It is postulated that users may tire of the simple movement protocols that have typically been used in mirror therapy intervention. Thus, the emergence of technologies such as immersive virtual reality may offer a more engaging environment for intervention delivery and is thus gaining attention as a promising technological innovation for post-stroke upper limb rehabilitation [6]. Furthermore, a recent study demonstrated the capability of immersive virtual reality-based interventions to stimulate neurons in a damaged brain areas and enhance functional recovery of upper limbs after stroke [7], eliciting multisensory stimulation [8] and its gamified nature has been effective in engaging stroke patients in upper limb rehabilitative process [9]. In a mechanism similar to that thought to be achieved through ‘traditional’ mirror therapy, Chang et al. recently confirmed that immersive virtual reality mirror therapy has the potential to enhance neuroplasticity in the motor cortex, that is, through neural reorganization and adaptation following injury which manifests in motor recovery in poststroke patients [10].
Therefore, the integration of mirror therapy principles with immersive virtual reality technology might present a synergetic and promising approach for upper limb rehabilitation delivery in poststroke survivors. This implies that using the concepts of mirror therapy in immersive VR technology could be a more effective and promising method for supporting stroke survivors regain movement and function in their arms and hands. The immersive and realistic nature of VR could potentially enhance the effects of mirror therapy, leading to better outcomes in rehabilitation. However, the landscape of existing evidence on this matter has not yet been collated. Therefore, the aim of this scoping review was to explore and synthesise the available evidence on the application of IVRMT for poststroke upper limb rehabilitation.
Methods
A scoping review was performed to explore the nature, extent and characteristics of studies [11, 12] conducted on the application of IVRMT for upper limb rehabilitation following stroke (Supplementary file 1). To do this, the following five steps were adopted [12];
-
Step 1. Identifying the research question
The guiding review question was formulated according to the PICO (Population, Intervention, Comparison, Outcome) framework [13] and stated as “What is the available evidence on the application of immersive virtual reality mirror box therapy for upper limb rehabilitation following stroke?”.
-
Step 2. Identifying relevant studies
Once the authors established the review question, the review proceeded to identify relevant studies. The source of literature were online databases, related-article reference lists and Google scholar. A systematic literature search, limited to English-language articles published from 2013 to 2023, undertaken on APA PsycInfo, CINAHL, Cochrane Library, MEDLINE, PubMed and Web of Science between August 5 and 17, 2023. Furthermore, relevant studies were included from Google Scholar and related-article reference lists. The PICO framework was used as guidance in building literature searching strategies [13]. Accordingly, the following key concepts were used to formulate the literature search strategies; a) Immersive virtual reality OR virtual reality OR VR b) mirror therapy OR mirror visual feedback OR mirror box therapy OR mirror neurons c) upper limb OR upper extremity OR hand OR arm d) recovery OR rehabilitation e) stroke OR cerebrovascular accident OR CVA. Detail searching strategies and results can be seen in Supplementary file 2.
-
Step 3. Study selection
Two authors undertook the process of article screening and selection, using Mendeley software. All identified references were exported to Mendeley, duplicates removed, followed by title and abstract screening guided by the review aim and question. Full-text articles were evaluated for inclusion as per the following eligibility criteria:
-
Inclusion
The PICO framework was used to refine the inclusion criteria [13].
-
Population -studies conducted on adult stroke populations with upper limb weakness.
-
Intervention-studies that applied immersive virtual reality mirror for upper limb rehabilitation post stroke.
-
Comparison- all studies with or without a comparator were eligible for inclusion.
-
Outcome- all studies needed to report on at least one outcome of clinical applicability relevant to use of the system.
-
-
Exclusion
-
Conference, abstract, registry, commentary and other opinion pieces were excluded.
-
-
Final inclusion of an article was decided upon through consensus of two authors (GG, APA) having thoroughly considered each study. Arbitration by the third author (NA) was not required as full consensus was achieved.
-
Step 4. Charting
Two authors (GG, APA) determined the specific information to be extracted from each included study and created a data extraction table to do so. Data that aligned with the review question was extracted and tabulated. This included details such as authors, publication year, country, methods, key findings, and other information pertinent to the broader review question. All authors reviewed and ensured the charting process was consistent.
-
Step 5. Collating, summarising, and reporting
This scoping review adapted a thematic analysis. Thematic analysis is a flexible approach that can be adapted to studies with a variety of questions and data types [14]. The analysis and synthesis of data was executed with NVIVO software. Initially, the selected articles were imported to NVIVO software, read to fully understood their content, and recurring concepts, ideas and meanings coded. These codes were then grouped as themes. Clear and meaningful names were given to the themes, which were organized as findings and reported coherently.
Results
Article selection process
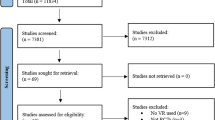
As presented in Fig. 1, the search for articles generated a total of 224 records, of which 213 were retrieved through online database searching and the remaining 11 were handpicked records from Google scholar and related-article reference lists. From the database-generated records, 128 were removed for duplication, resulting in 85 records for further screening. Of these, 69 were excluded after title and abstract screening, and 16 full-text articles were retrieved and evaluated for inclusion in the review. In addition, out of 11 handpicked records, 3 full-text articles were retrieved and evaluated against the criteria for inclusion. Overall, 11 articles were excluded because of the following reasons: studies with non-immersive VR MT intervention (n = 5), reports with no study population of interest (n = 3), studies with non-clinically applicable outcome (n = 1) and conference paper (n = 1). Eight articles [7, 15,16,17,18,19,20,21] were identified as being eligible for inclusion.
Flow diagram of selection of studies following the guidelines of the PRISMA statement 2020 [22]
Characteristics of studies
The studies in this review were conducted in high- and upper-middle-income nations such as Germany (n = 2; 22,27), Taiwan (n = 2; 24,26), China (n = 1;14), Brazil (n = 1; 21), Poland (n = 1; 23) and USA (n = 1; 25). All the studies were published between 2019 and 2023, of which five were published in the past year 2022/23 [15,16,17,18, 21]. All studies were experimental (n = 8). Of these, three studies [7, 17, 20] had two comparison groups, two studies [15, 18] had three comparison groups, and the remaining three [16, 19, 21] had no comparison group. The total sample size in the studies was 259, ranging from 10 [19] to 54 participants [18], with the majority of subjects being stroke patients with upper limb weakness (n = 184). Most of the study participants were recruited from clinical settings, in particular, rehabilitation departments and centers (Table 1).
This review identified three major themes and two sub-themes based on the contents of the studies conducted on the application of IVRMT: IVRMT’s technical application, feasibility and impact on clinical outcomes (motor recovery and adverse events).
Technical application of IVRMT
The procedure of using IVRMT was similar across all the included studies. Seven studies developed an IVRMT system [7, 15,16,17,18,19,20] while one [21] relied on existing system. In all studies, IVRMT was implemented using smartphone or computer-compatible software or Apps that displayed a reversed image of the unaffected upper limb. The movement of the unaffected limb was captured by a Leap Motion Controller (LMC) and mirroring capability within the IVRMT software/App enabled duplication of these movements from the unaffected upper limb, leading to the creation of coordinated movements on the affected upper limb at the center of the VR goggles viewpoint. The IVRMT experienced by the participant is of both upper limbs represented within the VR goggles, and thus patients are immersed in the mirror illusion of bilateral activity and active use of the affected limb. The intervention delivered through the IVRMT primarily comprised training sessions incorporating exercises [16,17,18,19,20], functional activities [7, 15, 19, 21] and gamified virtual tasks [15, 21] (see Table 2). Gamified training sessions were dominant across the intervention protocols and were noted to be motivating and engaging for participants. However, the clinical intervention protocol and dose varied among all studies (Table 2) which thus inhibits any direct comparisons being made.
Feasibility
Two studies exploring the feasibility of IVRMT for poststroke upper limb recovery [21], using the System Usability Scale (SUS) reported variations in usability. Jacques et al. [15] found that both mirror therapy and VR-based mirror therapy were both rated as having low levels of perceived useability. Whilst mirror therapy was viewed as being more easily adaptable and causing less overall discomfort, the comfort levels of the headset goggles was a key factor in useability of IVRMT for post stroke rehabilitation use and that IVRMT was viewed as requiring a greater effort with a less positive overall experience for older adults. Conversely, Weber et al. [19] concluded that IVRMT was well tolerated and safe, with high compliance and an above average SUS score.
One study [16] explored feasibility through use of the Acceptance of Technology and Motivation Questionnaire and the meCUE 2.0 user experience questionnaire. Results reported positive ratings towards IVRMT on both outcome measures with an overall adherence to the intervention of 100% and both participants and therapists reporting high ratings for usefulness and useability.
Two studies [17, 21] used standardized outcome assessments to assess impact upon quality of life through the use of IVRMT using the SF-36 [17] and the EQ-5D-5L scale [21]. Both studies reported statistically significant improvements in quality-of-life measurements following intervention.
Impact on clinical outcomes
Motor recovery
Seven studies [7, 16,17,18,19,20,21] assessed the motor function recovery of stroke patients after IVMRT use. Six studies used the Fugl-Meyer motor assessment for upper extremity (FMA-UE) to evaluate upper limb motor function recovery of stroke patients after IVMRT interventions [7, 16,17,18,19,20]. One study [21] used the Functional Independence Measure (FIM) to measure the patients’ level of independence in performing various activities such as self-care. In six studies [7, 16,17,18, 20, 21] patients showed improvements to the recovery of their upper extremities following use of the IVRMT, of which, five studies [7, 16,17,18, 20] demonstrated statistically significant changes of FMA-UE scores pre- to post- tests, and the remaining study demonstrating a significant increase in baseline FIM score over a period of 6 weeks [21]. However, one study [19] demonstrated no such significant changes to the FMA-UE or to Action Research Arm Test (ARAT) scores.
One study suggested that IVRMT had a comparatively better effect on motor functioning of upper extremities over traditional mirror therapy [20]. Conversely, in another study, the comparative group-by-time difference of motor function between conventional occupational therapy, mirror therapy (MT), and VR-based MT was statistically insignificant (the FMA-UE total score) [18]. However, over the intervention period, significant within-group differences were recorded in both MT and VR-based MT groups, as evidenced by the total FMA-UE scores, but remained below the minimal detectable change [18].
Mekbib et al. [7] studied the mechanism of motor cortex and parietal cortex activity using mirrored VR activity. As a result, significant neural functional connectivity and functional improvements were noted. The researchers concluded that limb mirroring exercise in an immersive virtual environment was associated with cortical reorganisation, which significantly linked with motor functioning improvements.
Adverse events
Cybersickness is a commonly reported concern regarding the use of virtual reality in all settings [23]. Adverse events associated with the use of the immersive virtual reality by stroke patients with upper limb weakness was explored in five of the papers [16,17,18,19,20] (Table 2). The approach and tools adapted in the assessment of adverse outcomes varied across studies. Standardised outcome assessment was only undertaken in two studies using the Simulator Sickness Questionnaire [16, 19]; with adverse event monitoring questionnaires and protocols being used in four studies [15, 16, 18, 20] to assess more general susceptibility to symptoms such as finger tingling/numbness, heat sensation, fingertips sensation, dizziness, nausea, visual disturbance, unusual pain or feeling of tiredness.
Whilst all studies concluded that IVRMT was a well-tolerated and safe intervention for stroke patients with upper limb weakness, 3 studies did record some report of symptoms aligned with cybersickness [15, 16, 19]. Whilst these were small scale studies using mainly non-standardised outcomes, it remains an important aspect to explore further particularly given the likely overlay of post-stroke fatigue, sensory, perceptual and cognitive symptoms that this patient population present with. Interestingly, one study noted the report of amelioration in pain and sensory impressions after the use of IVRMT [17].
Discussion
The aim of this scoping review was to explore and synthesise existing evidence on the application of immersive virtual reality mirror therapy for poststroke upper limb rehabilitation. Accordingly, eight studies were found that assessed the application of immersive virtual reality mirror therapy for upper limb rehabilitation in people with stroke. Amongst these, the earliest published research paper to use an avatar based immersional VR system was conducted by Weber et al. in 2019 [19] which was a small-scale study that concluded that the IVRMT was safe, and well-tolerated. All subsequent studies identified through this review adapted a variety of technology and software to develop an iteration of immersive virtual reality mirror therapy (Tables 1 and 2). Like the variation in technology, the dose, type and duration of the interventions were similarly varied across the studies as seen in Table 2. The duration of intervention ranged from two [7, 16] to nine [18, 20] weeks, and the basis of intervention founded on virtual games [15, 21], exercises [16,17,18,19,20] or functional tasks [7, 15, 19, 21]. Whilst this heterogeneity provides a broad lens through which to view the potential development and application of IVRMT, it highlights the need for the implementation of a more consistent technology, intervention and dose protocol to enable direct comparison across studies to be made.
In addition, immersive virtual reality mirror therapy was reported as a safe, tolerated, and feasible intervention for stroke patients with upper limb weakness [16,17,18,19,20]. However, adverse events such as cybersickness were not rigorously investigated and thus attention needs to be given to this aspect, particularly given the likely overlay of health issues related to a post stroke presentation that could be exacerbated by the use of an immersional VR-based system [23].
Nevertheless, six of the selected studies [7, 16,17,18, 20, 21] confirmed progressive upper limb recovery among stroke patients following immersive virtual reality mirror therapy. Of these, two studies [18, 20] presented the comparative effectiveness of IVRMT on motor recovery of upper extremities over conventional mirror therapy. However, while one of these studies concluded that IVRMT was statistically superior to conventional mirror therapy, the second did not find a significant difference between them. Furthermore, only one study has investigated and confirmed that IVRMT was less comfortable than conventional mirror therapy [15]. Of course, this discomfort might be due to the headset and motion sickness often associated with immersive virtual reality. Hence, further comparative studies are needed to conclude whether IVRMT is more effective for regaining motor recovery of upper extremities than conventional mirror therapy in upper limb rehabilitation after stroke. Moreover, it is evident that the effectiveness of rehabilitation programme relies upon the degree of patient engagement with prescribed interventions. In this application, engagement may have been enhanced through the multisensory experiences and illusive engagement of users provided by virtual reality-based mirror therapy [24].
Limitations of the review
This review was restricted to articles published in the English language between 2013 and 2023 and accessed through the specified databases. Therefore, research papers published in other databases, outside this period and/or in other languages will have been omitted.
Conclusion
This review found only eight studies published since 2019 that investigated the application of immersive virtual reality mirror therapy for poststroke upper limb rehabilitation. These studies focused on the application of immersive virtual reality-based mirror therapy and considered some key outcome measures such as feasibility, motor functioning and adverse events. Overall, immersive virtual reality mirror therapy was found to offer a safe and feasible approach to post-stroke upper limb rehabilitation, with enhanced participant engagement and improved motor recovery outcomes. However, the current scoping review has highlighted inconsistencies across studies in terms of intervention protocol type and dose, as well a lack of standardized measurement of cybersickness as a potential outcome. Furthermore, methodologically robust studies need to be conducted using a standardized protocol with a core outcome measure set to enable definitive conclusions to be drawn as to the patient benefits of immersive virtual mirror therapy for poststroke upper limb rehabilitation.
Data availability
All materials used to support the conclusions are submitted along with the manuscript.
References
Zhuang J-Y, Ding L, Shu B-B, Chen D, Jia J (2021) Associated mirror therapy enhances motor recovery of the upper extremity and daily function after stroke: A randomized control study. Hua X-Y, editor. Neural Plast [Internet]. Sep 29;2021:1–9. Available from: https://www.hindawi.com/journals/np/2021/7266263/
Dohle C, Altschuler E, Ramachandran VS (2020) Chapter 20 - mirror therapy. In: Sathian K, Ramachandran VSBT-MP (eds) Academic Press, pp 449–461. https://doi.org/10.1016/B978-0-12-812492-5.00020-6
Ramachandran VS (2005) Plasticity and functional recovery in neurology. Clin Med J R Coll Phys London 5(4):368–373
Rothgangel A, Braun S, Smeets R, Beurskens A (2019) Feasibility of a traditional and teletreatment approach to mirror therapy in patients with phantom limb pain: a process evaluation performed alongside a randomized controlled trial. Clin Rehabil 33(10):1649–1660
Rothgangel A, Braun S, Winkens B, Beurskens A, Smeets R (2018) Traditional and augmented reality mirror therapy for patients with chronic phantom limb pain (PACT study): results of a three-group, multicentre single-blind randomized controlled trial. Clin Rehabil 32(12):1591–1608
Demeco, A. Zola L, Frizziero A, Martini C, Palumbo A, Foresti R, Costantino C (2023) Immersive virtual reality in post-stroke rehabilitation: a systematic review. Sensors (Basel, Switzerland) 23(3). https://doi.org/10.3390/s23031712
Mekbib DB, Zhao Z, Wang J, Xu B, Zhang L, Cheng R et al (2020) Proactive motor functional recovery following immersive virtual reality-based limb mirroring therapy in patients with subacute stroke. Neurotherapeutics 17(4):1919–1930
Giroux M, Barra J, Zrelli IE, Barraud PA, Cian C, Guerraz M (2018) The respective contributions of visual and proprioceptive afferents to the mirror illusion in virtual reality. PLoS ONE 13(8):1–14
Gueye T, Dedkova M, Rogalewicz V, Grunerova-Lippertova M, Angerova Y (2021) Early post-stroke rehabilitation for upper limb motor function using virtual reality and exoskeleton: equally efficient in older patients. Neurol Neurochir Pol [Internet] 55(1):91–6. Available from: https://journals.viamedica.pl/neurologia_neurochirurgia_polska/article/view/70645
Chang WK, Lim H, Park SH, Lim C, Paik N-J, Kim W-S et al (2023) Effect of immersive virtual mirror visual feedback on Mu suppression and coherence in motor and parietal cortex in stroke. Sci Rep [Internet] 13(1):12514. Available from: https://login.napier.idm.oclc.org/login?url=https://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=37532803&site=ehost-live
Levac D, Colquhoun H, O’Brien KK (2010) Scoping studies: Advancing the methodology. Implement Sci 5(1):1–9
Arksey H, O’Malley L (2005) Scoping studies: Towards a methodological framework. Int J Soc Res Methodol Theory Pract 8(1):19–32
McKenzie JE, Brennan SE, Ryan RE, Thomson HJ, Johnston RV, Thomas J (2019) Defining the criteria for including studies and how they will be grouped for the synthesis. Cochrane handbook for systematic reviews of interventions 33–65
Braun V, Clarke V (2006) Using thematic analysis in psychology. Qual Res Psychol 3(2):77–101
Jaques ED, Figueiredo AI, Schiavo A, Loss BP, da Silveira GH, Sangalli VA et al (2023) Conventional mirror therapy versus immersive virtual reality mirror therapy: The perceived usability after stroke. Stroke Res Treat [Internet]. 2023 May 25;2023:1–8. Available from: https://login.napier.idm.oclc.org/login?url=https://search.ebscohost.com/login.aspx?direct=true&db=c8h&AN=163948627&site=ehost-live
Heinrich C, Morkisch N, Langlotz T, Regenbrecht H, Dohle C (2022) Feasibility and psychophysical effects of immersive virtual reality-based mirror therapy. J NeuroEngineering Rehabil [Internet] 19(1):1–20. Available from: https://login.napier.idm.oclc.org/login?url=https://search.ebscohost.com/login.aspx?direct=true&db=c8h&AN=159547976&site=ehost-live
Sip P, Kozłowska M, Czysz D, Daroszewski P, Lisiński P (2023) Perspectives of motor functional upper extremity recovery with the use of immersive virtual reality in stroke patients. Sensors (Basel) [Internet] 23(2). Available from: https://login.napier.idm.oclc.org/login?url=https://search.ebscohost.com/login.aspx?direct=true&db=cmedm&AN=36679511&site=ehost-live
Hsu H-Y, Kuo L-C, Lin Y-C, Su F-C, Yang T-H, Lin C-W (2022) Effects of a virtual reality-based mirror therapy program on improving sensorimotor function of hands in chronic stroke patients: a randomized controlled trial. Neurorehabil Neural Repair 36(6):335–345
Weber LM, Nilsen DM, Gillen G, Yoon J, Stein J (2019) Immersive virtual reality mirror therapy for upper limb recovery after stroke: a pilot study. Am J Phys Med Rehabil 98(9):783–788
Lin C-W, Kuo L-C, Lin Y-C, Su F-C, Lin Y-A, Hsu H-Y (2021) Development and testing of a virtual reality mirror therapy system for the sensorimotor performance of upper extremity: a pilot randomized controlled trial. IEEE Access 9:14725–14734
Chen C-H, Kreidler T, Ochsenfahrt A (2022) Rehago - a home-based training app using virtual reality to improve functional performance of stroke patients with mirror therapy and gamification concept: a pilot study. Stud Health Technol Inform 292:91–95
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2020) The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021:372
Yildirim C (2020) Don’t make me sick: investigating the incidence of cybersickness in commercial virtual reality headsets. Virtual Real [Internet] 24(2):231–9. Available from: https://doi.org/10.1007/s10055-019-00401-0
Perez-Marcos D, Bieler-Aeschlimann M, Serino A (2018) Virtual reality as a vehicle to empower motor-cognitive neurorehabilitation. Front Psychol [Internet] 9:2120. Available from: https://www.frontiersin.org/article/10.3389/fpsyg.2018.02120/full
Funding
The lead author is funded by a PhD studentship awarded by Edinburgh Napier University, Scotland. No other financial support has been provided for this research.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. The first draft of the manuscript was written by GG and AP, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical statement
Not applicable.
Informed consent
Not applicable.
Conflicts of interest
The authors report there are no competing interests to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Gebreheat, G., Antonopoulos, N. & Porter-Armstrong, A. Application of immersive virtual reality mirror therapy for upper limb rehabilitation after stroke: a scoping review. Neurol Sci (2024). https://doi.org/10.1007/s10072-024-07543-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10072-024-07543-3