Abstract
Background and objectives
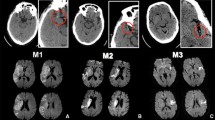
ASPECTs is a widely used marker to identify early stroke signs on non-enhanced computed tomography (NECT), yet it presents interindividual variability and it may be hard to use for non-experts. We introduce an algorithm capable of automatically estimating the NECT volumetric extension of early acute ischemic changes in the 3D space. We compared the power of this marker with ASPECTs evaluated by experienced practitioner in predicting the clinical outcome.
Methods
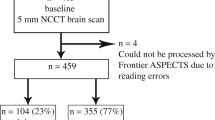
We analyzed and processed neuroimaging data of 153 patients admitted with acute ischemic stroke. All patients underwent a NECT at admission and on follow-up. The developed algorithm identifies the early ischemic hypodense region based on an automatic comparison of the gray level in the images of the two hemispheres, assumed to be an approximate mirror image of each other in healthy patients.
Results
In the two standard axial slices used to estimate the ASPECTs, the regions identified by the algorithm overlap significantly with those identified by experienced practitioners. However, in many patients, the regions identified automatically extend significantly to other slices. In these cases, the volume marker provides supplementary and independent information. Indeed, the clinical outcome of patients with volume marker = 0 can be distinguished with higher statistical confidence than the outcome of patients with ASPECTs = 10.
Conclusion
The volumetric extension and the location of acute ischemic region in the 3D-space, automatically identified by our algorithm, provide data that are mostly in agreement with the ASPECTs value estimated by expert practitioners, and in some cases complementary and independent.



Similar content being viewed by others
References
Sacco RL, Kasner SE, Broderick JP et al (2013) An updated definition of stroke for the 21st century: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 44(7):2064–2089. https://doi.org/10.1161/STR.0b013e318296aeca
Truelsen T, Piechowski-Jóźwiak B, Bonita R et al (2006) Stroke incidence and prevalence in Europe: a review of available data. Eur J Neurol 13(6):581–598. https://doi.org/10.1111/j.1468-1331.2006.01138.x
Jauch EC, Saver JL, Adams HP Jr et al (2013) Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 44(3):870–947. https://doi.org/10.1161/STR.0b013e318284056a
Martins SC, Freitas GR, Pontes-Neto OM et al (2012) Guidelines for acute ischemic stroke treatment: part II: stroke treatment. ArqNeuropsiquiatr 70(11):885–893. https://doi.org/10.1590/S0004-282X2012001100012
Powers WJ, Rabinstein AA, Ackerson T et al (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke. Stroke 50:e344–e418
Campbell BC V, Ma H, Ringleb PA, et al (2019) Extending thrombolysis to 4.5–9 h and wake-up stroke using perfusion imaging: a systematic review and meta-analysis of individual patient data. Lancet (London, England). https://doi.org/10.1016/S0140-6736(19)31053-0
Furlanis G, Ajcevic M, Buoite Stella A et al (2020) Wake-up stroke: thrombolysis reduces ischemic lesion volume and neurological deficit. J Neurol 267:666–673. https://doi.org/10.1007/s00415-019-09603-7
Berkhemer OA, Fransen PS, Beumer D et al (2015) A randomized trial of intraarterial treatment for acute ischemic stroke. N Engl J Med 372(1):11–20. https://doi.org/10.1056/NEJMoa1411587
Goyal M, Demchuk AM, Menon BK et al (2015) Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med 372(11):1019–1030. https://doi.org/10.1056/NEJMoa1414905
Campbell BC, Mitchell PJ, Kleinig TJ et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372(11):1009–1018. https://doi.org/10.1056/NEJMoa1414792
Saver JL, Goyal M, Bonafe A et al (2015) Solitaire with the intention for thrombectomy as primary endovascular treatment for acute ischemic stroke (SWIFT PRIME) trial: protocol for a randomized, controlled, multicenter study comparing the Solitaire revascularization device with IV tPA with IV tPA alone in acute ischemic stroke. Int J Stroke 10(3):439–448. https://doi.org/10.1111/ijs.12459
Fink JN, Selim MH, Kumar S et al (2002) Is the association of National Institutes of Health Stroke Scale scores and acute magnetic resonance imaging stroke volume equal for patients with right- and left-hemisphere ischemic stroke? Stroke 33:954–958
Adams HP Jr, Davis PH, Leira EC et al (1999) Neurology 53(1):126–131
Furlanis G, Ajcevic M, Stragapede L et al (2018) Ischemic volume and neurological deficit: correlation of computed tomography perfusion with the national institutes of health stroke scale score in acute ischemic stroke. J Stroke Cerebrovasc Dis 27(8):2200–2207
Frankel MR, Morgenstern LB, Kwiatkowski T et al (2000) Predicting prognosis after stroke: a placebo group analysis from the National Institute of Neurological Disorders and Stroke rt-PA Stroke Trial. Neurology 55(7):952–959
Kidwell CS, Chalela JA, Saver JL, Starkman S et al (2004) Comparison of MRI and CT for detection of acute intracerebral hemorrhage. JAMA 292(15):1823–1830
Chalela JA, Kidwell CS, Nentwich LM et al (2007) Magnetic resonance imaging and computed tomography in emergency assessment of patients with suspected acute stroke: a prospective comparison. Lancet 369(9558):293–298
Bouchez L, Sztajzel R, Vargas MI et al (2017) CT imaging selection in acute stroke. Eur J Radiol 96:153–161. https://doi.org/10.1016/j.ejrad.2016.10.026
Coles JP (2007) Imaging after brain injury. Br J Anaesth 99:49–60
Pexman JH, Barber PA, Hill MD, Sevick RJ et al (2001) Use of the Alberta Stroke Program Early CT Score (ASPECTS) for assessing CT scans in patients with acute stroke. AJNR Am J Neuroradiol 22(8):1534–1542
Baek JH, Kim K, Lee YB et al (2015) Predicting stroke outcome using clinical- versus imaging-based scoring system. J Stroke Cerebrovasc Dis 24(3):642–648. https://doi.org/10.1016/j.jstrokecerebrovasdis.2014.10.009
Ajčević M, Furlanis G, Buoite Stella A et al (2020) A CT perfusion based model predicts outcome in wake-up stroke patients treated with recombinant tissue plasminogen activator. Physiol Meas 41:075011. https://doi.org/10.1088/1361-6579/ab9c70
Hill MD, Rowley HA, Adler F et al (2016) PROACT-II investigators, selection of acute ischemic stroke patients for intra-arterial thrombolysis with pro-urokinase by using ASPECTS. Stroke 34(8):1925–1931
Coutts SB, Demchuk AM, Barber PA et al (2004) Interobserver variation of ASPECTS in real time. Stroke 35(5):e103–e105
Chilamkurthy S, Ghosh R, Tanamala S et al (2018) Deep learning algorithms for detection of critical findings in head CT scans: a retrospective study. Lancet 392(10162):2388–2396. https://doi.org/10.1016/S0140-6736(18)31645-3
Lee EJ, Kim YH, Kim N, Kang DW (2017) Deep into the brain: artificial intelligence in stroke imaging. J Stroke 19:277–285
Herweh C, Ringleb PA, Rauch G et al (2016) Performance of e-ASPECTS software in comparison to that of stroke physicians on assessing CT scans of acute ischemic stroke patients. Int J Stroke 11(4):438–445. https://doi.org/10.1177/1747493016632244
Pfaff J, Herweh C, Schieber S et al (2017) e-ASPECTS correlates with and is predictive of outcome after mechanical thrombectomy. AJNR Am J Neuroradiol 38(8):1594–1599. https://doi.org/10.3174/ajnr.A5236
Nagel S, Wang X, Carcel C et al (2018) Clinical utility of electronic alberta stroke program early computed tomography score software in the ENCHANTED trial database. Stroke 49(6):1407–1411. https://doi.org/10.1161/STROKEAHA.117.019863
Nagel S, Sinha D, Day D et al (2017) e-ASPECTS software is non-inferior to neuroradiologists in applying the ASPECT score to computed tomography scans of acute ischemic stroke patients. Int J Stroke 12(6):615–622. https://doi.org/10.1177/1747493016681020
Goebel J, Stenzel E, Guberina N et al (2018) Automated ASPECT rating: comparison between the Frontier ASPECT Score software and the Brainomix software. Neuroradiology 60(12):1267–1272. https://doi.org/10.1007/s00234-018-2098-x
Hacke W, Kaste M, Fieschi C et al (1998) Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian Acute Stroke Study Investigators. Lancet 352(9136):1245–51
Adams HP Jr, Bendixen BH, Kappelle LJ et al (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41
Rorden C, Bonilha L, Fridriksson J et al (2012) Age-specific CT and MRI templates for spatial normalization. Neuroimage 61(4):957–965. https://doi.org/10.1016/j.neuroimage.2012.03.020
Ashburner J, Friston KJ (1999) Nonlinear spatial normalization using basis functions. Hum Brain Mapp 7(4):254–266
Tzourio-Mazoyer N, Landeau B, Papathanassiou D et al (2002) Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage 15(1):273–289
Caruso P, Ridolfi M, Lugnan C, Ajčević M, Furlanis G, Bellavita G, Mucelli RAP, Zdjelar A, Ukmar M, Naccarato M, Stella AB, Manganotti P (2021) Multimodal CT pc-ASPECTS in infratentorial stroke: diagnostic and prognostic value. Neurol Sci 42(10):4231–4240. https://doi.org/10.1007/s10072-021-05072-x
Bouslama M, Ravindran K, Harston G, Rodrigues GM, Pisani L, Haussen DC, Frankel MR, Nogueira RG (2021) Noncontrast computed tomography e-Stroke infarct volume is similar to RAPID computed tomography perfusion in estimating postreperfusion infarct volumes. Stroke 52(2):634–641. https://doi.org/10.1161/STROKEAHA.120.031651
Kobeissi H, Ghozy S, Adusumilli G, Bilgin C, Tolba H, Amoukhteh M, Kadirvel R, Brinjikji W, Heit JJ, Rabinstein AA, Kallmes DF (2023) CT perfusion vs noncontrast CT for late window stroke thrombectomy: a systematic review and meta-analysis. Neurology 100(22):e2304–e2311. https://doi.org/10.1212/WNL.0000000000207262
Tian H, Parsons MW, Levi CR et al (2019) Influence of occlusion site and baseline ischemic core on outcome in patients with ischemic stroke. Neurology 92:e2626–e2643. https://doi.org/10.1212/WNL.0000000000007553
Ajčević M, Furlanis G, Naccarato M et al (2021) Hyper-acute EEG alterations predict functional and morphological outcomes in thrombolysis-treated ischemic stroke: a wireless EEG study. Med Biol EngComput 59(1):121–129. https://doi.org/10.1007/s11517-020-02280-z
Bentley P, Ganesalingam J, Carlton Jones AL et al (2014) Prediction of stroke thrombolysis outcome using CT brain machine learning. Neuroimage Clin 30(4):635–640. https://doi.org/10.1016/j.nicl.2014.02.003
Chawla M, Sharma S, Sivaswamy J et al (2009) A method for automatic detection and classification of stroke from brain CT images. Conf Proc IEEE Eng Med Biol Soc 2009:3581–3584. https://doi.org/10.1109/IEMBS.2009.5335289
Shieh Y, Chang CH, Shieh M et al (2014) Computer-aided diagnosis of hyperacute stroke with thrombolysis decision support using a contralateral comparative method of CT image analysis. J Digit Imaging 27(3):392–406
Acknowledgements
The authors wish to thank Michele Allegra for data processing support.
Author information
Authors and Affiliations
Contributions
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Corresponding author
Ethics declarations
Ethical approval and informed consent
We conducted our study according to the principles of the Declaration of Helsinki. All participants released their informed consent to participate in the study after all procedures had been fully explained. Approval for the study had been obtained from the local ethics committee.
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bernardi, M.S., Rodriguez, A., Caruso, P. et al. Improving acute stroke assessment in non-enhanced computed tomography: automated tool for early ischemic lesion volume detection. Neurol Sci (2024). https://doi.org/10.1007/s10072-024-07339-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10072-024-07339-5