Abstract
Purpose
To evaluate whether Alberta Stroke Program Early CT Score (ASPECTS) could provide incremental value to collateral score, and their integration could be an effective surrogate of CTP in predicting target mismatch.
Material and methods
One hundred and fifty-nine stroke patients (onset time 6–16 h or with unknown onset time) with MCA and/or ICA occlusion underwent non-contrast computed tomography (NCCT) and CT perfusion (CTP) scan for initial assessment. Simulated single-phase CT angiography (sCTA, peak arterial phase) and multiphase CTA (mCTA) were reconstructed from CTP. ASPECTS was assessed on NCCT and sCTA. Collateral score was evaluated on mCTA. Target mismatch was defined as infarct core volume < 70 mL, the mismatch ratio ≥ 1.8, and the absolute mismatch volume ≥ 15 mL. Pearson correlation analysis, Mann–Whitney U test, chi-square test, and receiver operating characteristic curve analyses were performed.
Results
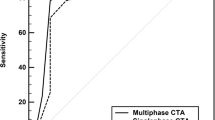
Median CTA source image (CTA-SI) ASPECTS was significantly lower than NCCT ASPECTS (p = 0.001). NCCT ASPECTS, CTA-SI ASPECTS, and mCTA collateral score correlated significantly with infarct core volume and mismatch ratio (all p < 0.05). Mismatch group showed significantly higher NCCT ASPECTS, CTA-SI ASPECTS, and mCTA collateral score than non-mismatch group (all p < 0.001). NCCT ASPECTS and CTA-SI ASPECTS showed comparable predicting performance with mCTA collateral score (p > 0.05). Adding CTA-SI ASPECTS to mCTA collateral score improved the performance of mCTA in predicting target mismatch (area under curve, 0.905 vs. 0.804, p = 0.003).
Conclusion
ASPECTS can provide incremental information to collateral score in predicting target mismatch. If CTP scan fails, clinical decision based on ASPECTS and collateral score might be reasonable.


Similar content being viewed by others
References
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL, on behalf of the American Heart Association Stroke Council (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 50(12):e344–e418
Ma H, Campbell BCV, Parsons MW, Churilov L, Levi CR, Hsu C, Kleinig TJ, Wijeratne T, Curtze S, Dewey HM, Miteff F, Tsai CH, Lee JT, Phan TG, Mahant N, Sun MC, Krause M, Sturm J, Grimley R, Chen CH, Hu CJ, Wong AA, Field D, Sun Y, Barber PA, Sabet A, Jannes J, Jeng JS, Clissold B, Markus R, Lin CH, Lien LM, Bladin CF, Christensen S, Yassi N, Sharma G, Bivard A, Desmond PM, Yan B, Mitchell PJ, Thijs V, Carey L, Meretoja A, Davis SM, Donnan GA, EXTEND Investigators (2019) Thrombolysis guided by perfusion imaging up to 9 hours after onset of stroke. N Engl J Med 380(19):1795–1803
Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, McTaggart RA, Torbey MT, Kim-Tenser M, Leslie-Mazwi T, Sarraj A, Kasner SE, Ansari SA, Yeatts SD, Hamilton S, Mlynash M, Heit JJ, Zaharchuk G, Kim S, Carrozzella J, Palesch YY, Demchuk AM, Bammer R, Lavori PW, Broderick JP, Lansberg MG, DEFUSE 3 Investigators (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378(8):708–718
Kauw F, Heit JJ, Martin BW, van Ommen F, Kappelle LJ, Velthuis BK, de Jong HWAM, Dankbaar JW, Wintermark M (2020) Computed tomography perfusion data for acute ischemic stroke evaluation using rapid software: pitfalls of automated postprocessing. J Comput Assist Tomogr 44(1):75–77
Caruso P, Naccarato M, Furlanis G, Ajčević M, Stragapede L, Ridolfi M, Polverino P, Ukmar M, Manganotti P (2018) Wake-up stroke and CT perfusion: effectiveness and safety of reperfusion therapy. Neurol Sci 39(10):1705–1712
Frölich AM, Psychogios MN, Klotz E, Schramm R, Knauth M, Schramm P (2012) Angiographic reconstructions from whole-brain perfusion CT for the detection of large vessel occlusion in acute stroke. Stroke 43(1):97–102
Berkhemer OA, Jansen IG, Beumer D, Fransen PS, van den Berg LA, Yoo AJ, Lingsma HF, Sprengers ME, Jenniskens SF, Lycklama À, Nijeholt GJ, van Walderveen MA, van den Berg R, Bot JC, Beenen LF, Boers AM, Slump CH, Roos YB, van Oostenbrugge RJ, Dippel DW, van der Lugt A, van Zwam WH, Marquering HA, Majoie CB, MR CLEAN Investigators (2016) Collateral status on baseline computed tomographic angiography and intra-arterial treatment effect in patients with proximal anterior circulation stroke. Stroke 47(3):768–76
Tan IY, Demchuk AM, Hopyan J, Zhang L, Gladstone D, Wong K, Martin M, Symons SP, Fox AJ, Aviv RI (2009) CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am J Neuroradiol 30(3):525–531
Vagal A, Menon BK, Foster LD, Livorine A, Yeatts SD, Qazi E, d’Esterre C, Shi J, Demchuk AM, Hill MD, Liebeskind DS, Tomsick T, Goyal M (2016) Association between CT angiogram collaterals and CT perfusion in the interventional management of stroke III trial. Stroke 47(2):535–538
Lu SS, Zhang X, Xu XQ, Cao YZ, Zhao LB, Liu QH, Wu FY, Liu S, Shi HB (2019) Comparison of CT angiography collaterals for predicting target perfusion profile and clinical outcome in patients with acute ischemic stroke. Eur Radiol 29(9):4922–4929
Barber PA, Demchuk AM, Zhang J, Buchan AM, for the ASPECTS Study Group (2000) Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. Lancet 355(9216):1670–1674
Finlayson O, John V, Yeung R, Dowlatshahi D, Howard P, Zhang L, Swartz R, Aviv RI (2013) Interobserver agreement of ASPECT score distribution for noncontrast CT, CT angiography, and CT perfusion in acute stroke. Stroke 44(1):234–236
Sallustio F, Motta C, Pizzuto S, Diomedi M, Rizzato B, Panella M, Alemseged F, Stefanini M, Fabiano S, Gandini R, Floris R, Stanzione P, Koch G (2017) CT Angiography ASPECTS predicts outcome much better than noncontrast CT in patients with stroke treated endovascularly. AJNR Am J Neuroradiol 38(8):1569–1573
Naylor J, Churilov L, Chen Z, Koome M, Rane N, Campbell BCV (2017) Reliability, reproducibility and prognostic accuracy of the alberta stroke program early CT score on CT perfusion and non-contrast CT in hyperacute stroke. Cerebrovasc Dis 44(3–4):195–202
Caruso P, Ridolfi M, Lugnan C, Ajčević M, Furlanis G, Bellavita G, Mucelli RAP, Zdjelar A, Ukmar M, Naccarato M, Stella AB, Manganotti P (2021) Multimodal CT pc-ASPECTS in infratentorial stroke: diagnostic and prognostic value. Neurol Sci. [Epub ahead of print]
Dehkharghani S, Bammer R, Straka M, Bowen M, Allen JW, Rangaraju S, Kang J, Gleason T, Brasher C, Nahab F (2016) Performance of CT ASPECTS and collateral score in risk stratification: can target perfusion profiles be predicted without perfusion imaging? AJNR Am J Neuroradiol 37(8):1399–1404
Campbell BC, Christensen S, Levi CR, Desmond PM, Donnan GA, Davis SM, Parsons MW (2011) Cerebral blood flow is the optimal CT perfusion parameter for assessing infarct core. Stroke 42(12):3435–3440
Olivot JM, Mlynash M, Thijs VN, Kemp S, Lansberg MG, Wechsler L, Bammer R, Marks MP, Albers GW (2009) Optimal Tmax threshold for predicting penumbral tissue in acute stroke. Stroke 40(2):469–475
Menon BK, d’Esterre CD, Qazi EM, Almekhlafi M, Hahn L, Demchuk AM, Goyal M (2015) Multiphase CT angiography: a new tool for the imaging triage of patients with acute ischemic stroke. Radiology 275(2):510–520
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44(3):837–845
Kim EY, Shin DH, Noh Y, Goh BH, Lee YB (2016) Comparison of imaging selection criteria for intra-arterial thrombectomy in acute ischemic stroke with advanced CT. Eur Radiol 26(9):2974–2981
de Margerie-Mellon C, Turc G, Tisserand M, Naggara O, Calvet D, Legrand L, Meder JF, Mas JL, Baron JC, Oppenheim C (2013) Can DWI-ASPECTS substitute for lesion volume in acute stroke? Stroke 44(12):3565–3567
DiBiasio EL, Jayaraman MV, Goyal M, Yaghi S, Tung E, Hidlay DT, Tung GA, Baird GL, McTaggart RA (2019) Dismantling the ability of CT and MRI to identify the target mismatch profile in patients with anterior circulation large vessel occlusion beyond six hours from symptom onset. Emerg Radiol 26(4):401–408
Kawiorski MM, Martínez-Sánchez P, García-Pastor A, Calleja P, Fuentes B, Sanz-Cuesta BE, Lourido D, Marín B, Díaz-Otero F, Vicente A, Sierra-Hidalgo F, Ruiz-Ares G, Díez-Tejedor E, Fandiño E, Alonso de Leciñana M (2016) Alberta Stroke Program Early CT Score applied to CT angiography source images is a strong predictor of futile recanalization in acute ischemic stroke. Neuroradiology 58(5):487–493
Sharma M, Fox AJ, Symons S, Jairath A, Aviv RI (2011) CT angiographic source images: flow- or volume-weighted? AJNR Am J Neuroradiol 32(2):359–364
Herweh C, Ringleb PA, Rauch G, Gerry S, Behrens L, Möhlenbruch M, Gottorf R, Richter D, Schieber S, Nagel S (2016) Performance of e-ASPECTS software in comparison to that of stroke physicians on assessing CT scans of acute ischemic stroke patients. Int J Stroke 11(4):438–445
Kawano H, Bivard A, Lin L, Spratt NJ, Miteff F, Parsons MW, Levi CR (2016) Relationship between collateral status, contrast transit, and contrast density in acute ischemic stroke. Stroke 47(3):742–749
Funding
This research is funded by the National Natural Science Foundation of China (81971613 to Hai-Bin Shi).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical approval
None.
Conflict of interest
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ma, G., Cao, YZ., Xu, XQ. et al. Incremental value of Alberta Stroke Program Early CT Score to collateral score for predicting target mismatch in stroke patients with extended time window or unknown onset time. Neurol Sci 43, 1097–1104 (2022). https://doi.org/10.1007/s10072-021-05387-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05387-9