Abstract
Background
Migrainous aura (MA) represents the third most common stroke mimic (SM). Advanced neuroimaging is pivotal in the assessment of patients with focal neurological acute symptoms. We investigated brain perfusion alterations in MA-SM patients using a novel CT perfusion (CTP)-based quantitative approach in order to improve differential diagnosis between MA and acute stroke.
Methods
We processed and analysed the clinical and neuroimaging CTP data, acquired within 4.5 h from symptom onset, of patients with acute focal neurological symptoms receiving a final diagnosis of MA. The differences between ROI, compatible with MA symptoms, and contralateral side were automatically estimated in terms of asymmetry index (AI%) by the newly developed tool for mean transit time (MTT), CBF, and cerebral blood volume (CBV) CTP parameters. The AI% ≥ 10% was considered significant.
Results
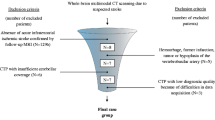
Out of 923 admitted patients, 14 patients with MA were included. In 13 out of 14 cases, a significant pattern of hypoperfusion was observed by quantitative analysis in at least one of the CTP maps. In 7 patients, all three CTP maps were significantly altered. In particular, MTT-AI% increased in 11 (79%) cases, while CBF-AI% and CBV-AI% decreased in 12 (86%) and in 9 (64%) patients, respectively. All CBV values were above ischemic stroke core threshold and all MTT-AI were below ischemic penumbra threshold.
Conclusions
Our data suggest that a novel CTP-quantitative approach may detect during MA a moderate hypoperfusion pattern in the cerebral regions compatible with aura symptoms. The use of this novel tool could support differential diagnosis between MA and acute stroke.

Similar content being viewed by others
Abbreviations
- CBF:
-
Cerebral blood flow
- CBV:
-
Cerebral blood volume
- CT:
-
Computed tomography
- CTP:
-
Computed tomography perfusion
- CTA:
-
Computed tomography angiography
- DWI:
-
Diffusion-weighted imaging
- ED:
-
Emergency Department
- MA:
-
Migrainous aura
- MTT:
-
Mean transit time
- MRI:
-
Magnetic resonance imaging
- NECT:
-
Non-enhanced CT
- NIHSS:
-
National Institutes of Health Stroke Scale
- ROI:
-
Region of interest
- SM:
-
Stroke mimic
- SU:
-
Stroke unit
- TTP:
-
Time to peak
References
Kirchmann M (2006) Migraine with aura: new understanding from clinical epidemiologic studies. Curr Opin Neurol. 19(3):286–293
Merino JG, Luby M, Benson RT, Davis LA, Hsia AW, Latour LL, Lynch JK, Warach S (2013) Predictors of acute stroke mimics in 8187 patients referred to a stroke service. J Stroke Cerebrovasc Dis. 22(8):e397–e403
Mehta S, Vora N, Edgell RC, Allam H, Alawi A, Koehne J, Kumar A, Feen E, Cruz-Flores S, Alshekhlee A (2014) Stroke mimics under the drip-and-ship paradigm. J Stroke Cerebrovasc Dis. 23(5):844–849
Terrin A, Toldo G, Ermani M, Mainardi F, Maggioni F (2018) When migraine mimics stroke: a systematic review. Cephalalgia. 38(14):2068–2078
Ferrante E, Prone V, Longoni M, Agostoni EC (2017) Stroke-like attack: first episode of sporadic hemiplegic migraine. Neurol Sci. 38(Suppl 1):189–191
Wintermark M, Luby M, Bornstein NM, Demchuk A, Fiehler J, Kudo K, Lees KR, Liebeskind DS, Michel P, Nogueira RG, Parsons MW, Sasaki M, Wardlaw JM, Wu O, Zhang W, Zhu G, Warach SJ (2015) International survey of acute stroke imaging used to make revascularization treatment decisions. Int J Stroke. 10(5):759–762
Caruso P, Naccarato M, Furlanis G, Ajčević M, Stragapede L, Ridolfi M, Polverino P, Ukmar M, Manganotti P (2018) Wake-up stroke and CT perfusion: effectiveness and safety of reperfusion therapy. Neurol Sci. 39(10):1705–1712
Furlanis G, Ajčević M, Stragapede L, Lugnan C, Ridolfi M, Caruso P, Naccarato M, Ukmar M, Manganotti P (2018) Ischemic volume and neurological deficit: correlation of computed tomography perfusion with the national institutes of health stroke scale score in acute ischemic stroke. J Stroke Cerebrovasc Dis. 27(8):2200–2207
Strada L, Streifler JY, Del Sette B, Puntoni M, Castaldi A, Bianchini D et al (2017) Is CT perfusion helpful in the treatment allocation of patients with acute ischemic stroke? An expert-opinion analysis. Neurol Sci. 38(10):1771–1777
Kim T, Koo J, Kim SH, Song IU, Chung SW, Lee KS (2018) Blood-brain barrier permeability assessed by perfusion computed tomography predicts hemorrhagic transformation in acute reperfusion therapy. Neurol Sci. 39(9):1579–1584
Austein F, Huhndorf M, Meyne J, Laufs H, Jansen O, Lindner T (2018) Advanced CT for diagnosis of seizure-related stroke mimics. Eur Radiol. 28(5):1791–1800
Manganotti P, Furlanis G, Ajčević M, Polverino P, Caruso P, Ridolfi M, Pozzi-Mucelli RA, Cova MA, Naccarato M (2019) CT perfusion and EEG patterns in patients with acute isolated aphasia in seizure-related stroke mimics. Seizure. 71:110–115
Ridolfi M, Granato A, Polverino P, Furlanis G, Ukmar M, Zorzenon I, Manganotti P (2018) Migrainous aura as stroke-mimic: the role of perfusion-computed tomography. Clin Neurol Neurosurg. 166:131–135
Angermaier A, Langner S, Kirsch M, Khaw AV (2014) Prolonged aphasia and perfusion computed tomography abnormalities in migraine with aura. Int J Case Rep Images 3:221–224
Miller C, Goldberg MF (2012) Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine. Emerg Radiol. 19(6):565–569
Shah L, Rana S, Valeriano J, Scott TF (2013) Reversible CT perfusion abnormalities in patient with migraine variant: a two phase process. Clin Neurol Neurosurg. 115(6):830–832
Campbell BC, Weir L, Desmond PM, Tu HT, Hand PJ, Yan B et al (2013) CT perfusion improves diagnostic accuracy and confidence in acute ischaemic stroke. J Neurol Neurosurg Psychiatry. 84(6):613–618
Nieuwkamp DJ, van der Schaaf IC, Biessels GJ (2010) Migraine aura presenting as dysphasia with global cognitive dysfunction and abnormalities on perfusion CT. Cephalalgia 30(8):1007–1009
Hansen JM, Schytz HW, Larsen VA, Iversen HK, Ashina M (2011) Hemiplegic migraine aura begins with cerebral hypoperfusion: imaging in the acute phase. Headache. 51(8):1289–1296
Rath CL, He J, Nordling MM, Wienecke T (2017) Acute intravenous calcium antagonist for suspected hemiplegic migraine-a case story. Case Rep Neurol. 9(1):98–105
Headache Classification Committee of the International Headache Society (IHS) (2013) The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 33:629–808
Kellner-Weldon F, El-Koussy M, Jung S, Jossen M, Klinger-Gratz PP, Wiest R (2018) Cerebellar hypoperfusion in migraine attack: incidence and significance. AJNR Am J Neuroradiol. 39(3):435–440
Wintermark M, Flanders AE, Velthuis B, Meuli R, van Leeuwen M, Goldsher D, Pineda C, Serena J, Schaaf I, Waaijer A, Anderson J, Nesbit G, Gabriely I, Medina V, Quiles A, Pohlman S, Quist M, Schnyder P, Bogousslavsky J, Dillon WP, Pedraza S (2006) Perfusion-CT assessment of infarct core and penumbra: receiver operating characteristic curve analysis in 130 patients suspected of acute hemispheric stroke. Stroke. 37(4):979–985
Khan NI, Chaku S, Goehl C, Endris L, Mueller-Luckey G, Siddiqui FM (2018) Novel algorithm to help identify stroke mimics. J Stroke Cerebrovasc Dis. 27(3):703–708
Goyal N, Tsivgoulis G, Male S, Metter EJ, Iftikhar S, Kerro A, Chang JJ, Frey JL, Triantafyllou S, Papadimitropoulos G, Abedi V, Alexandrov AW, Alexandrov AV, Zand R (2016) FABS: an intuitive tool for screening of stroke mimics in the emergency department. Stroke. 47(9):2216–2220
Lui YW, Tang ER, Allmendinger AM, Spektor V (2010) Evaluation of CT perfusion in the setting of cerebral ischemia: patterns and pitfalls. AJNR Am J Neuroradiol. 31(9):1552–1563
Shen J, Li X, Li Y, Wu B (2017) Comparative accuracy of CT perfusion in diagnosing acute ischemic stroke: a systematic review of 27 trials. PLoS One. 12(5):e0176622
Krishnan P, Murphy A, Aviv RI (2017) CT-based techniques for brain perfusion. Top Magn Reson Imaging. 26(3):113–119
Mangla R, Ekhom S, Jahromi B et al (2014) CT perfusion in acute stroke: know the mimics, potential pitfalls, artifacts, and technical errors. Emerg Radiol. 21(1):49–65
Leao AAP (1944) Spreading depression of activity in the cerebral cortex. J Neurophysiol 7:359–390
Olesen J, Friberg L, Olsen TS, Iversen HK, Lassen NA, Andersen AR et al (1990) Timing and topography of cerebral blood flow, aura, and headache during migraine attacks. Ann Neurol. 28(6):791–798
Chiu AH, Phillips TJ, Phatouros CC, Singh TP, Hankey GJ, Blacker DJ, McAuliffe W (2016) CT perfusion in acute stroke calls: a pictorial review and differential diagnoses. J Med Imaging Radiat Oncol. 60(2):165–171
Viola S, Viola P, Buongarzone MP, Fiorelli L, Cipulli M, Litterio P (2018) Microvascular vasospasm of cerebral cortex in prolonged aura migraine. Neurol Sci. 39(Suppl 1):95–96
Arngrim N, Hougaard A, Ahmadi K, Vestergaard MB, Schytz HW, Amin FM, Larsson HBW, Olesen J, Hoffmann MB, Ashina M (2017) Heterogenous migraine aura symptoms correlate with visual cortex functional magnetic resonance imaging responses. Ann Neurol. 82(6):925–939
Barbanti P, Fofi L, Aurilia C, Egeo G (2019) Does the migraine attack start in the cortex and is the cortex critical in the migraine process? Neurol Sci. 40(Suppl 1):31–37
Dreier JP, Reiffurth C (2015) The stroke-migraine depolarization continuum. Neuron. 86(4):902–922
Floery D, Vosko MR, Fellner FA, Fellner C, Ginthoer C, Gruber F, Ransmayr G, Doerfler A, Uder M, Bradley WG (2012) Acute-onset migrainous aura mimicking acute stroke: MR perfusion imaging features. AJNR Am J Neuroradiol. 33(8):1546–1552
Mourand I, Menjot de Champfleur N, Carra-Dallière C, Le Bars E, Roubertie A, Bonafé A et al (2012) Perfusion-weighted MR imaging in persistent hemiplegic migraine. Neuroradiology. 54(3):255–260
Linn J, Freilinger T, Morhard D, Brückmann H, Straube A (2007) Aphasic migraineous aura with left parietal hypoperfusion: a case report. Cephalalgia. 27(7):850–853
Jacob A, Mahavish K, Bowden A, Smith ET, Enevoldson P, White RP (2006) Imaging abnormalities in sporadic hemiplegic migraine on conventional MRI, diffusion and perfusion MRI and MRS. Cephalalgia. 26(8):1004–1009
Oberndorfer S, Wöber C, Nasel C, Asenbaum S, Lahrmann H, Fueger B, Grisold W (2004) Familial hemiplegic migraine: follow-up findings of diffusion-weighted magnetic resonance imaging (MRI), perfusion-MRI and [99mTc] HMPAO-SPECT in a patient with prolonged hemiplegic aura. Cephalalgia. 24(7):533–539
Wolf ME, Okazaki S, Eisele P, Rossmanith C, Gregori J, Griebe M, Günther M, Gass A, Hennerici MG, Szabo K, Kern R (2018) Arterial spin labeling cerebral perfusion magnetic resonance imaging in migraine aura: an observational study. J Stroke Cerebrovasc Dis. 27(5):1262–1266
Kim S, Kang M, Choi S (2016) A case report of sporadic hemiplegic migraine associated cerebral hypoperfusion: comparison of arterial spin labeling and dynamic susceptibility contrast perfusion MR imaging. Eur J Pediatr. 175(2):295–298
Iizuka T, Tominaga N, Kaneko J, Sato M, Akutsu T, Hamada J, Sakai F, Nishiyama K (2015) Biphasic neurovascular changes in prolonged migraine aura in familial hemiplegic migraine type 2. J Neurol Neurosurg Psychiatry. 86(3):344–353
Acknowledgments
The authors thank Matteo di Franza for the editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study has been conducted according to the principles of the Declaration of Helsinki, and it was approved by the Local Ethics Committee CEUR (Comitato Etico Unico Regionale, FVG, Italy) with approval number 115/2018. Each patient provided a written and signed informed consent that allowed the analysis of his/her data for clinical and research purposes.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Granato, A., D’Acunto, L., Ajčević, M. et al. A novel computed tomography perfusion-based quantitative tool for evaluation of perfusional abnormalities in migrainous aura stroke mimic. Neurol Sci 41, 3321–3328 (2020). https://doi.org/10.1007/s10072-020-04476-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04476-5



