Abstract
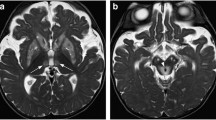
Vestibular migraine (VM) has been increasingly recognized as a frequent cause of episodic vertigo, affecting up to 1 % of the general population, with female preponderance. Recently, both the Bárány Society and the Migraine Classification Subcommittee of the International Headache Society have proposed original diagnostic criteria for VM, which have been included in the recent edition of the ICHD-3 beta version. VM diagnosis implies that vestibular symptoms are present during a migraine attack, with or without headache, in the absence of objectively demonstrated interictal vestibulopathy. Nevertheless, despite a growing body of literature, there is still an ongoing debate regarding whether VM origin is principally central or peripheral. However, during the past few years, the extensive application of advanced MRI techniques has contributed to significantly improve the understanding VM pathophysiology. Functional and structural abnormalities have been detected in brain areas involved in multisensory vestibular control and central vestibular processing in patients with VM. In this brief review, we will focus on these recent neuroimaging findings.
Similar content being viewed by others
References
Headache Classification Committee of the International Headache Society (IHS) (2013) The International Classification of Headache Disorders, 3rd edn (beta version). Cephalalgia 33(9):629–808
Headache Classification Subcommittee of the International Headache Society (2004) The International Classification of Headache Disorders, 2nd edn. Cephalalgia 24(Suppl 1):1–160
Lempert T (2013) Vestibular migraine. Semin Neurol 33(3):212–218. doi:10.1055/s-0033-1354596
Furman JM, Marcus DA, Balaban CD (2013) Vestibular migraine: clinical aspects and pathophysiology. Lancet Neurol 12(7):706–715
Neuhauser HK, von Brevern M, Radtke A, Lezius F, Feldmann M, Ziese T, Lempert T (2005) Epidemiology of vestibular vertigo: a neurotological survey of the general population. Neurology 65(6):898–904
Neuhauser HK, Lempert T (2009) Vertigo: epidemiologic aspects. Semin Neurol 29(5):473–481
Balaban CD (2011) Migraine, vertigo and migrainous vertigo: links between vestibular and pain mechanisms. J Vestib Res 21(6):315–321. doi:10.3233/VES-2011-0428 (Review)
von Brevern M, Zeise D, Neuhauser H, Clarke AH, Lempert T (2005) Acute migrainous vertigo: clinical and oculographic findings. Brain 128(Pt 2):365–374 (Epub 2004 Dec 15)
Taylor RL, Zagami AS, Gibson WP, Black DA, Watson SR, Halmagyi MG, Welgampola MS (2012) Vestibular evoked myogenic potentials to sound and vibration: characteristics in vestibular migraine that enable separation from Meniere’s disease. Cephalalgia 32(3):213–225. doi:10.1177/0333102411434166
Radtke A, von Brevern M, Neuhauser H, Hottenrott T, Lempert T (2012) Vestibular migraine: long-term follow-up of clinical symptoms and vestibulo-cochlear findings. Neurology 79(15):1607–1614. doi:10.1212/WNL.0b013e31826e264f
Shin JH, Kim YK, Kim HJ, Kim JS (2014) Altered brain metabolism in vestibular migraine: comparison of interictal and ictal findings. Cephalalgia 34(1):58–67. doi:10.1177/0333102413498940
Jeong SH, Oh SY, Kim HJ, Koo JW, Kim JS (2010) Vestibular dysfunction in migraine: effects of associated vertigo and motion sickness. J Neurol 257(6):905–912. doi:10.1007/s00415-009-5435-5
Cutrer FM, Sorensen AG, Weisskoff RM, Ostergaard L, Sanchez del Rio M, Lee EJ, Rosen BR, Moskowitz MA (1998) Perfusion-weighted imaging defects during spontaneous migrainous aura. Ann Neurol 43(1):25–31
Dieterich M, Brandt T (2008) Functional brain imaging of peripheral and central vestibular disorders. Brain 131(Pt 10):2538–2552. doi:10.1093/brain/awn042
Russo A, Marcelli V, Esposito F, Corvino V, Marcuccio L, Giannone A, Conforti R, Marciano E, Tedeschi G, Tessitore A (2014) Abnormal thalamic function in patients with vestibular migraine. Neurology 82(23):2120–2126
Borsook D, Burstein R (2012) The enigma of the dorsolateral pons as a migraine generator. Cephalalgia 32(11):803–812. doi:10.1177/0333102412453952
Espinosa-Sanchez Juan M, Lopez-Escamez JA (2015) New insights into pathophysiology of vestibular migraine Front. Neurol. doi:10.3389/fneur.2015.00012
King S, Wang J, Priesol AJ, Lewis RF (2014) Central integration of canal and otolith signals is abnormal in vestibular migraine. Front Neurol 5:233. doi:10.3389/fneur.2014.00233
Tedeschi G, Russo A, Tessitore A (2013) Relevance of functional neuroimaging studies for understanding migraine mechanisms. Expert Rev Neurother 13(3):275–285. doi:10.1586/ern.13.20
Granziera C, DaSilva AF, Snyder J, Tuch DS, Hadjikhani N (2006) Anatomical alterations of the visual motion processing network in migraine with and without aura. PLoS Med 3(10):e402
Rocca MA, Pagani E, Colombo B, Tortorella P, Falini A, Comi G, Filippi M (2008) Selective diffusion changes of the visual pathways in patients with migraine: a 3-T tractography study. Cephalalgia 28(10):1061–1068. doi:10.1111/j.1468-2982.2008.01655.x
Rocca MA, Ceccarelli A, Falini A, Tortorella P, Colombo B, Pagani E, Comi G, Scotti G, Filippi M (2006) Diffusion tensor magnetic resonance imaging at 3.0 tesla shows subtle cerebral grey matter abnormalities in patients with migraine. J Neurol Neurosurg Psychiatry 77(5):686–689
Hougaard A, Amin FM, Ashina M (2014) Migraine and structural abnormalities in the brain. Curr Opin Neurol 27(3):309–314. doi:10.1097/WCO.0000000000000086
Obermann M, Wurthmann S, Steinberg BS, Theysohn N, Diener HC, Naegel S (2014) Central vestibular system modulation in vestibular migraine. Cephalalgia 34(13):1053–1061
Conflict of interest
The authors certify that there is no actual or potential conflict of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tedeschi, G., Russo, A., Conte, F. et al. Vestibular migraine pathophysiology: insights from structural and functional neuroimaging. Neurol Sci 36 (Suppl 1), 37–40 (2015). https://doi.org/10.1007/s10072-015-2161-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-015-2161-x