Abstract
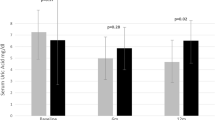
Uric acid has been recognised as a potential marker of endothelial dysfunction and kidney disease but there are scarce data about its importance in systemic lupus erythematosus (SLE) nephritis. This study aimed to evaluate serum uric acid (UA) levels in lupus nephritis (LN), by comparing SLE patients with normal renal function, with and without nephritis. Forty-six female SLE patients were consecutively selected and divided in two groups according to renal activity at the evaluation: presence of a recently diagnosed lupus nephritis (LN+, n = 18) and absence of lupus nephritis (LN−, n = 28). Age-matched healthy women were selected (CONTROL, n = 28). Patients with gout, creatinine clearance lower than 80 ml/min and use of drugs that interfere in UA were excluded. Laboratory and clinical data were analysed by appropriate tests. A multivariate analysis was performed, and a receiver operating characteristic (ROC) curve was plotted, and the area under the curve was calculated to assess the diagnostic strength of UA in LN. The mean age was similar among LN+, LN− and CONTROL groups (32.44 ± 6.09 vs. 30.68 ± 5.36 vs. 30.86 ± 5.00 years, p = 0.52). UA was significantly higher in LN+ compared to LN− (5.54 ± 1.67 vs. 3.65 ± 1.090 mg/dL, p < 0.001) and CONTROL (5.54 ± 1.67 vs. 3.92 ± 0.95 mg/dL p < 0.001). Multivariate analysis confirmed that high UA was an independent variable related to LN (p < 0.001). The cut-off value for UA using the ROC curve was 4.47 mg/dL (AUC 0.86, p = 0.00004, CI 95% 0.75–0.96). Lupus nephritis was associated with higher UA. Hyperuricemia as a predictor of renal damage in SLE needs to be evaluated in further studies.


Similar content being viewed by others
References
Bomback AS, Appel GB (2010) Updates on the treatment of lupus nephritis. J Am Soc Nephrol 21(12):2028–2035. https://doi.org/10.1681/ASN.2010050472
Houssiau FA (2004) Management of lupus nephritis: an update. J Am Soc Nephrol 15(10):2694–2704. https://doi.org/10.1097/01.ASN.0000140218.77174.0A
Ugolini-Lopes MR, Seguro LPC, Castro MXF, Daffre D, Lopes AC, Borba EF, Bonfá E (2017) Early proteinuria response: a valid real-life situation predictor of long-term lupus renal outcome in an ethnically diverse group with severe biopsy-proven nephritis? Lupus Sci Med 4:e000213. https://doi.org/10.1136/lupus-2017-000213
Yang Z, Liang Y, Xi W, Zhu Y, Li C, Zhong R (2011) Association of serum uric acid with lupus nephritis in systemic lupus erythematosus. Rheumatol Int 31(6):743–748. https://doi.org/10.1007/s00296-010-1373-x
Kang DH, Nakagawa T (2005) Uric acid and chronic renal disease: possible implication of hyperuricemia on progression of renal disease. Semin Nephrol 25(1):43–49. https://doi.org/10.1016/j.semnephrol.2004.10.001
Kang DH, Kanellis J (2005) Uric acid as a mediator of endothelial dysfunction, inflammation and vascular disease. Semin Nephrol 25:39–42
Sánchez-Lozada LG, Tapia E, Santamaría J, Avila-Casado C, Soto V, Nepomuceno T, Rodríguez-Iturbe B, Johnson RJ, Herrera-Acosta J (2005) Mild hyperuricemia induces vasoconstriction and maintains glomerular hypertension in normal and remnant kidney rats. Kidney Int 67(1):237–247. https://doi.org/10.1111/j.1523-1755.2005.00074.x
Johnson RJ, Kang DH, Feig D, Kivlighn S, Kanellis J, Watanabe S, Tuttle KR, Rodriguez-Iturbe B, Herrera-Acosta J, Mazzali M (2003) Is there a pathogenetic role for uric acid in hypertension and cardiovascular and renal disease? Hypertension 41(6):1183–1190. https://doi.org/10.1161/01.HYP.0000069700.62727.C5
Ficociello LH, Rosolowsky ET, Niewczas MA, Maselli NJ, Weinberg JM, Aschengrau A, Eckfeldt JH, Stanton RC, Galecki AT, Doria A, Warram JH, Krolewski AS (2010) High-normal serum uric acid increases risk of early progressive renal function loss in type 1 diabetes: results of a 6-year follow-up. Diabetes Care 33(6):1337–1343. https://doi.org/10.2337/dc10-0227
Frocht A, Leek JC, Robbins DL (1987) Gout and hyperuricemia in systemic lupus erythematosus. Br J Rheumatol 26(4):303–306. https://doi.org/10.1093/rheumatology/26.4.303
Reátegui-Sokolova C, Ugarte-Gil MF, Gamboa-Cárdenas RV, Zevallos F, Cucho-Venegas JM, Alfaro-Lozano JL, Medina M, Rodriguez-Bellido Z, Pastor-Asurza CA, Alarcón GS, Perich-Campos RA (2017) Serum uric acid levels contribute to new renal damage in systemic lupus erythematosus patients. Clin Rheumatol 36(4):845–852. https://doi.org/10.1007/s10067-017-3538-4
Feig DI, Kang DH, Johnson RJ (2008) Uric acid and cardiovascular risk. N Engl J Med 359(17):1811–1821. https://doi.org/10.1056/NEJMra0800885
Hochberg MC (1997) Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum 40(9):1725. https://doi.org/10.1002/art.1780400928
Neogi T, Jansen TL, Dalbeth N, Fransen J, Schumacher HR, Berendsen D et al (2015) 2015 gout classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheumatol 67(10):2557–2568. https://doi.org/10.1002/art.39254
Bombardier C, Gladman DD, Urowitz MB, Caron D, Chang CH (1992) Derivation of the SLEDAI. A disease activity index for lupus patients. The committee on prognosis studies in SLE. Arthritis Rheum 35(6):630–640. https://doi.org/10.1002/art.1780350606
Kosugi T, Nakayama T, Heinig M, Zhang L, Yuzawa Y, Sanchez-Lozada LG, Roncal C, Johnson RJ, Nakagawa T (2009) Effect of lowering uric acid on renal disease in the type 2 diabetic db/db mice. Am J Physiol Renal Physiol 297(2):F481–F488. https://doi.org/10.1152/ajprenal.00092.2009
Ohno I, Hosoya T, Gomi H, Ichida K, Okabe H, Hikita M (2001) Serum uric acid and renal prognosis in patients with IgA nephropathy. Nephron 87(4):333–339. https://doi.org/10.1159/000045939
Myllymäki J, Honkanen T, Syrjänen J, Helin H, Rantala I, Pasternack A, Mustonen J (2005) Uric acid correlates with the severity of histopathological parameters in IgA nephropathy. Nephrol Dial Transplant 20:89–95
Khosla UM, Zharikov S, Finch JL, Nakagawa T, Roncal C, Mu W, Krotova K, Blok ER, Prabhakar S, Johnson RJ (2005) Hyperucicemia induces endothelial dysfunction. Kidney Int 67(5):1739–1742. https://doi.org/10.1111/j.1523-1755.2005.00273.x
Hovind P, Rossing P, Tarnow L, Johnson RJ, Parving HH (2009) Serum uric acid as a predictor for development of diabetic nephropathy in type 1 diabetes—an inception cohort study. Diabetes 58(7):1668–1671. https://doi.org/10.2337/db09-0014
Ejaz AA, Mu W, Kang DH, Roncal C, Sautin YY, Henderson G, Tabah-Fisch I, Keller B, Beaver TM, Nakagawa T, Johnson RJ (2007) Could uric acid have a role in acute renal failure? Clin J Am Soc Nephrol 2:16–21. https://doi.org/10.2215/CJN.00350106
Corry DB, Eslami P, Yamamoto K, Nyby MD, Makino H, Tuck ML (2008) Uric acid stimulate vascular smooth muscles cell proliferation and oxidative stress via the vascular renin-angiotensin system. J Hipertens 26(2):269–275. https://doi.org/10.1097/HJH.0b013e3282f240bf
Kang DH, Nakagawa T, Feng L, Watanabe S, Hen L, Mazzali M, Truong L, Harris R, Johnson RJ (2002) A role for uric acid in the progression of renal disease. J Am Soc Nephrol 13:2888–2897
Kohagura K, Kochi M, Miyagi T, Kinjyo T, Maehara Y, Nagahama K, Sakima A, Iseki K, Ohya Y (2013) An association between uric acid levels and renal arteriolopathy in chronic kidney disease: a biopsy-based study. Hypertens Res 36(1):43–49. https://doi.org/10.1038/hr.2012.135
Martinon F, Pétrilli V, Mayor A, Tardivel A, Tschopp J (2006) Gout-associated uric acid crystals activate the NALP3 inflammasome. Nature 440:237–241
Ruggiero C, Cherubini A, Ble A, Bos AJ, Maggio M, Dixit VD, Lauretani F, Bandinelli S, Senin U, Ferrucci L (2006) Uric acid and inflammatory markers. Eur Heart J 27(10):1174–1181. https://doi.org/10.1093/eurheartj/ehi879
Giclas PC, Ginsberg MH, Cooper NR (1979) Immunoglobulin G independent activation of the classical complement pathway by monosodium urate crystals. J Clin Invest 63(4):759–764. https://doi.org/10.1172/JCI109360
Shi Y, Evans JE, Rock KL (2003) Molecular identification of a danger signal that alerts the immune system to dying cells. Nature 425(6957):516–521. https://doi.org/10.1038/nature01991
Ziyadeh FN, Wolf G (2008) Pathogenesis of the podocytopathy and proteinuria in diabetic glomerulopathy. Curr Diabetes Rev 4(1):39–45. https://doi.org/10.2174/157339908783502370
Zhuang Y, Yu Y, Huang Y, Zhong X (2014) Study on hyperuricemia in HBV-associated glomerulonephritis. Am J Clin Pathol 141:72–77. https://doi.org/10.1309/AJCP2H0FOVIRWMSU
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
None.
Rights and permissions
About this article
Cite this article
Calich, A.L., Borba, E.F., Ugolini-Lopes, M.R. et al. Serum uric acid levels are associated with lupus nephritis in patients with normal renal function. Clin Rheumatol 37, 1223–1228 (2018). https://doi.org/10.1007/s10067-018-3991-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-018-3991-8