Abstract
Regional cerebral oximetry using near-infrared spectroscopy devices is commonly used for detecting cerebral ischemia during cardiopulmonary bypass, and aim to avoid poor cerebral perfusion which may result in perioperative neurological impairment. Today, several devices that can detect cerebral ischemia are commercially available. Although these devices operate on the same measurement principles, their algorithms for detecting and calculating cerebral ischemia are different and no criteria for directly comparing values measured by such different devices exist. From January 2017 to August 2017, 80 adult cardiovascular surgery patients were enrolled in the prospective study. In each patient, preoperative regional cerebral oxygen saturation values were measured by two different devices and their correlations with various preoperative factors were evaluated. Regional cerebral oxygen saturation levels were significantly higher for values of FORE-SIGHT ELITE (CAS Medical Systems, Branford, CT, USA) (F value) than those of the INVOS 5100C (Medtronic, Minneapolis, MN, USA) (I value). Scalp–cortex distance, hemoglobin concentration, and the presence or absence of hemodialysis showed significant correlations with ratios of measured values specific to each device (F/I). An appropriate device should be selected according to preoperative patient characteristics, and factors influencing regional cerebral oxygen saturation values should be considered to ensure the correct interpretation of measured values. This research was conducted with the approval of the ethics committee of our university (approval number: B16–96).



Similar content being viewed by others
Change history
17 July 2018
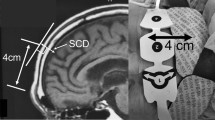
In the original publication, the length unit of the SCD in Table 1 and Fig. 2 has been incorrectly published as cm. The correct length unit is mm.
References
Tsai HI, Chung PC, Lee CW, Yu HP. Cerebral perfusion monitoring in acute care surgery: current and perspective use. Expert Rev Med Devices. 2016;13:865–75.
Denault A, Deschamps A, Murkin JM. A proposed algorithm for the intraoperative use of cerebral near-infrared spectroscopy. Semin Cardiothorac Vasc Anesth. 2007;11:274–81.
Colak Z, Borojevic M, Bogovic A, Ivancan V, Biocina B, Majeric-Kogler V. Influence of intraoperative cerebral oximetry monitoring on neurocognitive function after coronary artery bypass surgery: a randomized, prospective study. Eur J Cardiothorac Surg. 2015;47:447–54.
Gottlieb EA, Fraser CD Jr, Andropoulos DB, Diaz LK. Bilateral monitoring of cerebral oxygen saturation results in recognition of aortic cannula malposition during pediatric congenital heart surgery. Paediatr Anaesth. 2006;16:787–9.
Chan SK, Underwood MJ, Ho AM, So JM, Ho AK, Wan IY, Wong RH. Cannula malposition during antegrade cerebral perfusion for aortic surgery: role of cerebral oximetry. Can J Anaesth. 2014;61:736–40.
Kobayashi K, Kitamura T, Kohira S, Torii S, Horai T, Hirata M, Mishima T, Sughimoto K, Ohkubo H, Irisawa Y, Matsushiro T, Hayashi H, Miyata Y, Tsuchida Y, Ohtomo N, Miyaji K. Factors associated with a low initial cerebral oxygen saturation value in patients undergoing cardiac surgery. J Artif Organs. 2017;20:110–6.
Gregory AJ, Hatem MA, Yee K, Grocott HP. Optimal placement of cerebral oximeter monitors to avoid the frontal sinus as determined by computed tomography. J Cardiothorac Vasc Anesth. 2016;30:127–33.
Food, Administration D, Center for Drug Evaluation and Research (CDER). Guidance for industry: bioavailability and bioequivalence studies for orally administered drug products—general considerations. Washington, DC: FDA; 2003.
Arrowsmith JE, Grocott HP, Reves JG, Newman MF. Central nervous system complications of cardiac surgery. Br J Anaesth. 2000;84:378–93.
Jöbsis FF. Noninvasive, infrared monitoring of cerebral and myocardial oxygen sufficiency and circulatory parameters. Science. 1977;198:1264–7.
Scheeren TW, Schober P, Schwarte LA. Monitoring tissue oxygenation by near infrared spectroscopy (NIRS): background and current applications. J Clin Monit Comput. 2012;26:279–87.
Heringlake M, Garbers C, Käbler JH, Anderson I, Heinze H, Schön J, Berger KU, Dibbelt L, Sievers HH, Hanke T. Preoperative cerebral oxygen saturation and clinical outcomes in cardiac surgery. Anesthesiology. 2011;114:58–69.
Slater JP, Guarino T, Stack J, Vinod K, Bustami RT, Brown JM 3rd, Rodriguez AL, Magovern CJ, Zaubler T, Freundlich K, Parr GV. Cerebral oxygen desaturation predicts cognitive decline and longer hospital stay after cardiac surgery. Ann Thorac Surg. 2009;87:36–44.
Goldman S, Sutter F, Ferdinand F, Trace C. Optimizing intraoperative cerebral oxygen delivery using noninvasive cerebral oximetry decreases the incidence of stroke for cardiac surgical patients. Heart Surg Forum. 2004;7:E376–81.
Murkin JM, Adams SJ, Novick RJ, Quantz M, Bainbridge D, Iglesias I, Cleland A, Schaefer B, Irwin B, Fox S. Monitoring brain oxygen saturation during coronary bypass surgery: a randomized, prospective study. Anesth Analg. 2007;104:51–8.
Bickler PE, Feiner JR, Rollins MD. Factors affecting the performance of 5 cerebral oximeters during hypoxia in healthy volunteers. Anesth Analg. 2013;117:813–23.
Edmonds HL Jr, Ganzel BL, Austin EH 3rd. Cerebral oximetry for cardiac and vascular surgery. Semin Cardiothorac Vasc Anesth. 2004;8:147–66.
Yoshitani K, Kawaguchi M, Miura N, Okuno T, Kanoda T, Ohnishi Y, Kuro M. Effects of hemoglobin concentration, skull thickness, and the area of the cerebrospinal fluid layer on near-infrared spectroscopy measurements. Anesthesiology 2007;106:458–62.
Young AE, Germon TJ, Barnett NJ, Manara AR, Nelson RJ. Behaviour of near-infrared light in the adult human head: implications for clinical near-infrared spectroscopy. Br J Anaesth. 2000;84:38–42.
Okada E, Delpy DT. Near-infrared light propagation in an adult head model. II. effect of superficial tissue thickness on the sensitivity of the near-infrared spectroscopy signal. Appl Opt. 2003;42:2915–22.
Yoshitani K, Kawaguchi M, Okuno T, Kanoda T, Ohnishi Y, Kuro M, Nishizawa M. Measurements of optical pathlength using phase-resolved spectroscopy in patients undergoing cardiopulmonary bypass. Anesth Analg. 2007;104:341–6.
Jiang XL, Wen JQ, Zhang LJ, Zheng G, Li X, Zhang Z, Liu Y, Zheng LJ, Wu L, Chen HJ, Kong X, Luo S, Lu GM, Ji XM, Zhang ZJ. Cerebral blood flow changes in hemodialysis and peritoneal dialysis patients: an arterial-spin labeling MR imaging. Metab Brain Dis. 2016;31:929–36.
Oliveira MF, Zelt JT, Jones JH, Hirai DM, O’Donnell DE, Verges S, Neder JA. Does impaired O2 delivery during exercise accentuate central and peripheral fatigue in patients with coexistent COPD-CHF? Front Physiol. 2015. https://doi.org/10.3389/fphys.2014.00514.
Fischer GW, Silvay G. Cerebral oximetry in cardiac and major vascular surgery. HSR Proc Intensive Care Cardiovasc Anesth. 2010;2:249–56.
Fischer GW, Lin HM, Krol M, Galati MF, Di Luozzo G, Griepp RB, Reich DL. Noninvasive cerebral oxygenation may predict outcome in patients undergoing aortic arch surgery. J Thorac Cardiovasc Surg. 2011;141:815–21.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kobayashi, K., Kitamura, T., Kohira, S. et al. Cerebral oximetry for cardiac surgery: a preoperative comparison of device characteristics and pitfalls in interpretation. J Artif Organs 21, 412–418 (2018). https://doi.org/10.1007/s10047-018-1052-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10047-018-1052-3