Abstract
Background and purpose
Elective inguinal hernia repair is a ubiquitous procedure that carries risks; chronic pain and impacts on quality of life (QoL) must be considered when advising patients around repair. The length of time from surgery date and impacts on quality of life are often limited to only a few years of follow-up and despite hernia repair being quite common, long-term outcomes are not often reported.
Methods
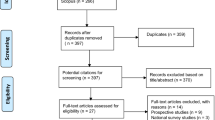
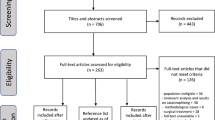
A cohort of patients who had received Lichtenstein inguinal hernia repair over the previous 10 years were contacted and surveyed using the Brief Pain Inventory Short Form (BPI) to assess chronic pain and its effects on their QoL. Patient and operative factors were correlated with pain through linear regression and t-test analysis provided statistical significance for mean comparisons (P < 0.05).
Results
The rate of chronic pain was 17.2% with recurrence of 3.1% at an average post-operative interval of 5.84 years. Of the various metrics compared between groups, age was one of the only significant predictors of chronic pain with younger patients reporting higher pain. Further time from surgery also translated to significantly less pain with a difference of 1.3 years. BPI respondents identified pain that interfered to varying degrees in different aspects of life but had relatively low average magnitudes (range: 1.82/10–2.91/10).
Conclusions
These long-term considerations of post-surgical impact should be considered alongside potential benefits when advising patients about surgery and may help moderate post-operative expectations to optimize the outcome of common inguinal hernia repairs.

Similar content being viewed by others
References
Dabbas N, Adams K, Pearson K, Royle G (2011) Frequency of abdominal wall hernias: is classical teaching out of date? JRSM Short Rep 2(1):1–6
Barkun J, Neville A, Fitzgerald GWN, Litwin D, McKenzie M (2008) Canadian association of general surgeons and American college of surgeons evidence-based reviews in surgery. 26. Watchful waiting versus repair of inguinal hernia in minimally symptomatic men. Canadian journal of surgery. Can Med Assoc 51:406–409
Fitzgibbons RJ, Giobbie-Hurder A, Gibbs JO, Dunlop DD, Reda DJ, McCarthy M, et al. Watchful waiting vs repair of inguinal hernia in minimally symptomatic men: A randomized clinical trial. J Am Med Assoc [Internet]. 2006 Jan 18 [cited 2020 Apr 22];295(3):285–92. Available from: http://www.ncbi.nlm.nih.gov/pubmed/16418463
Fitzgibbons RJ, Jonasson O, Gibbs J, Dunlop DD, Henderson W, Reda D, et al. The development of a clinical trial to determine if watchful waiting is an acceptable alternative to routine herniorrhaphy for patients with minimal or no hernia symptoms. J Am Coll Surg [Internet]. 2003 May 1 [cited 2020 Apr 23];196(5):737–42. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12742207
Gong W, Li J. Operation versus watchful waiting in asymptomatic or minimally symptomatic inguinal hernias: The meta-analysis results of randomized controlled trials. Int J Surg [Internet]. 2018 Apr 1 [cited 2020 Apr 23];52:120–5. Available from: http://www.ncbi.nlm.nih.gov/pubmed/29471159
Jenkins JT, O’Dwyer PJ. Inguinal hernias [Internet]. Vol. 336, BMJ. 2008 [cited 2020 Apr 22]. p. 269–72. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18244999
Phillips LaPinska M, Blatnik J. Surgical Principles in Inguinal Hernia Repair - A Comprehensive Guide to Anatomy and Operative Techniques. 1st ed. LaPinska MP, Blatnik JA, editors. Springer, Cham; 2018. 15–24
Bay-Nielsen M, Perkins FM, Kehlet H. Pain and functional impairment 1 year after inguinal herniorrhaphy: A nationwide questionnaire study. Vol. 233, Annals of Surgery. Lippincott, Williams, and Wilkins; 2001. p. 1–7
Schug SA, Lavand’Homme P, Barke A, Korwisi B, Rief W, Treede RD. The IASP classification of chronic pain for ICD-11: Chronic postsurgical or posttraumatic pain. Pain [Internet]. 2019 Jan 1 [cited 2022 Apr 16];160(1):45–52. Available from: https://journals.lww.com/pain/Fulltext/2019/01000/The_IASP_classification_of_chronic_pain_for.6.aspx
Wennergren JE, Plymale M, Davenport D, Levy S, Hazey J, Perry KA et al (2016) Quality-of-life scores in laparoscopic preperitoneal inguinal hernia repair. Surg Endosc 30(8):3467–3473
Huntington CR, Wormer BA, Cox TC, Blair LJ, Lincourt AE, Augenstein VA et al (2015) Local anesthesia in open inguinal hernia repair improves postoperative quality of life compared to general anesthesia: a prospective, international study. Am Surg 81(7):704–709
Jalil O, Rowlands C, Ruddle A, Hassn A, Morcous P. Medium-Term Recurrence and Quality of Life Assessment Using the Hernia-Specific Carolinas Comfort Scale Following Laparoscopic Inguinal Hernia Repair. J Laparoendosc Adv Surg Tech A [Internet]. 2015 Jun 1 [cited 2021 Dec 20];25(6):477–80. Available from: https://pubmed.ncbi.nlm.nih.gov/25946471/
Bande D, Moltó L, Pereira JA, Montes A. Chronic pain after groin hernia repair: Pain characteristics and impact on quality of life. BMC Surg [Internet]. 2020 Jul 1 [cited 2021 Dec 19];20(1):1–11. Available from: https://doaj.org/article/a1118004de974d24b5cce41c63b59ebb
Amid PK, Lichtenstein IL. Long-term result and current status of the Lichtenstein open tension-free hernioplasty. Hernia 1998 22 [Internet]. 1998 Jun [cited 2022 May 1];2(2):89–94. Available from: https://link.springer.com/article/https://doi.org/10.1007/BF01207492
Cleeland C. User guide The Brief Pain Inventory. Pain Res Gr [Internet]. 1991 [cited 2021 Sep 2];143–7. Available from: www.mdanderson.org
Erdfelder E, Faul F, Buchner A, Lang AG (2009) Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Methods 41(4):1149–1160
Sevinç B, Damburaci N, Güner M, Karahan Ö (2019) Comparison of early and long term outcomes of open lichtenstein repair and totally extraperitoneal herniorrhaphy for primary inguinal hernias. Turkish J Med Sci 49(1):38–41
Sanders DL, Nienhuijs S, Ziprin P, Miserez M, Gingell-Littlejohn M, Smeds S. Randomized clinical trial comparing self-gripping mesh with suture fixation of lightweight polypropylene mesh in open inguinal hernia repair. 2014 [cited 2020 May 15]; Available from: www.bjs.co.uk
Eker HH, Langeveld HR, Klitsie PJ, Van’t Riet M, Stassen LPS, Weidema WF et al (2012) Randomized clinical trial of total extraperitoneal inguinal hernioplasty vs lichtenstein repair: a long-term follow-up study. Arch Surg 147(3):256–260
Eklund A, Montgomery A, Bergkvist L, Rudberg C (2010) Chronic pain 5 years after randomized comparison of laparoscopic and Lichtenstein inguinal hernia repair. Br J Surg 97(4):600–608
Bakker WJ, van Hessen C V., Verleisdonk EJMM, Clevers GJ, Davids PHP, Schouten N, et al. Is young age a risk factor for chronic postoperative inguinal pain after endoscopic totally extraperitoneal (TEP) repair? Hernia [Internet]. 2019 Dec 1 [cited 2022 Sep 3];23(6):1053–9. Available from: https://link.springer.com/article/https://doi.org/10.1007/s10029-019-01882-3
Weber A, Valencia S, Garteiz D, Burguess A. Epidemology of Hernias in the Female. Abdom Wall Hernias [Internet]. 2001 [cited 2021 Dec 12];613–9. Available from: https://link.springer.com/chapter/https://doi.org/10.1007/978-1-4419-8574-3_90
Reinpold W (2020) Risk factors of chronic pain after inguinal hernia repair: a systematic review. Innovative surgical sciences. De Gruyter 2:61–68
Dansie EJ, Turk DC (2013) Assessment of patients with chronic pain. Br J Anaesth 111(1):19–25
Heikkinen T, Bringman S, Ohtonen P, Kunelius P, Haukipuro K, Hulkko A (2004) Five-year outcome of laparoscopic and Lichtenstein hernioplasties. Surg Endosc Other Interv Tech 18(3):518–522
Chung L, Ch MBB, O’dwyer PJ. Clinical Science Pain and its effects on physical activity and quality of life before operation in patients undergoing elective inguinal and ventral hernia repair. [cited 2021 Dec 19]; Available from: http://dx.doi.org/https://doi.org/10.1016/j.amjsurg.2014.02.011
Acknowledgements
The authors are grateful to the participants who elected to be part of this study and to the UBC Faculty of Medicine for educational resource and support. There was no external funding source associated with this study.
Funding
This project was funded by the clinical lead. The authors state there are no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest to declare.
Human and Animal Rights
There was no use of animals within this study by any of the authors.
Informed Consent
A signed informed consent form was collected from each of the participants included in this study.
Data Availability
De-identified data remain in the authors' possession and request for access may be made.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Moreton, M.L., Truter, A. Evaluation of inguinal hernia repair using post-operative pain and quality of life metrics. Hernia 27, 71–76 (2023). https://doi.org/10.1007/s10029-022-02701-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-022-02701-y