Abstract
Purpose
Lower transverse abdominal incisions are typically used by obstetricians/gynecologists and colorectal surgeons. The suture technique and choice of material when closing the abdomen is an essential factor to decrease the risk of incisional hernia. We conducted a nationwide survey among obstetricians/gynecologists and colorectal surgeons investigating the surgical handling of the fascia, rectus muscle, subcutis, peritoneum, and skin, in lower transverse incisions.
Methods
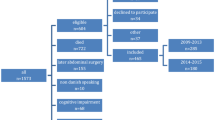
All departments of obstetrics/gynecology and departments of surgery performing colorectal surgery in Denmark were invited to participate. An online questionnaire was sent to consultant obstetricians/gynecologists and colorectal surgeons. The survey consisted of demographic information together with questions on surgical details. The study was reported according to STROBE guidelines.
Results
A total of 252 (64.5%) consultants provided a complete response to the survey. We found that 98.0% of the colorectal surgeons and 65.8% of the obstetricians/gynecologists used monofilament suture when closing the fascia. The majority of the colorectal surgeons used continuous suture and small bites technique. This was only the case for half of the obstetricians/gynecologists. Approximately two thirds of the colorectal surgeons and one third of the OB/GYN used the suture length to wound length ratio > 4:1. Furthermore, we found significant differences between the groups in the handling of subcutis, peritoneum, and skin.
Conclusion
We found significant variation in abdominal wall closure techniques in lower transverse incisions. Disagreement between the current guidelines within the specialties together with insufficient evidence on the closure of lower transverse incisions emphasizes the need for education as well as further studies.

Similar content being viewed by others
References
Alkatout I, Mettler L (2017) Hysterectomy a comprehensive surgical approach. J Turk Ger Gynecol Assoc 18:221–223
National Institute for Health and Care Excellence (2011) Caesarean section-Clinical guideline. https://www.nice.org.uk/guidance/cg132/resources/caesarean-section-pdf-35109507009733. Accessed 22 Apr 2020
Berghella V (2019) Cesarean delivery: Surgical technique—UpToDate. https://www.uptodate.com/contents/cesarean-delivery-surgical-technique. Accessed 22 Apr 2020
Kisielinski K, Conze J, Murken AH, Lenzen NN, Klinge U, Schumpelick V (2004) The Pfannenstiel or so called "bikini cut": still effective more than 100 years after first description. Hernia 8:177–181
Muysoms FE, Antoniou SA, Bury K, Campanelli G, Conze J, Cuccurullo D et al (2015) European Hernia Society guidelines on the closure of abdominal wall incisions. Hernia 19:1–24
Williams Z, Williams S, Easley HA, Seita HM, Hope WW (2017) An evaluation of abdominal wall closure in general surgical and gynecological residents. Hernia 21:873–877
Dahlke JD, Mendez-Figueroa H, Rouse DJ, Berghella V, Baxter JK, Chauhan SP (2013) Evidence-based surgery for cesarean delivery: an updated systematic review. Am J Obstet Gynecol 209:294–306
Anderson ER, Gates S (2004) Techniques and materials for closure of the abdominal wall in caesarean section. Cochrane Database Syst Rev CD004663
de Graaf IM, Oude Rengerink K, Wiersma IC, Donker ME, Mol BW, Pajkrt E (2012) Techniques for wound closure at caesarean section: a randomized clinical trial. Eur J Obstet Gynecol Reprod Biol 165:47–52
Husslein H, Gutschi M, Leipold H, Herbst C, Franz M, Worda C (2014) Suture closure versus non-closure of subcutaneous fat and cosmetic outcome after cesarean section: a randomized controlled trial. PLoS ONE 9:e114730
Chelmow D, Rodriguez EJ, Sabatini MM (2004) Suture closure of subcutaneous fat and wound disruption after cesarean delivery: a meta-analysis. Obstet Gynecol 103:974–980
Bamigboye AA, Hofmeyr GJ (2014) Closure versus non-closure of the peritoneum at caesarean section: short- and long-term outcomes. Cochrane Database Syst Rev CD000163
Gurusamy KS, Cassar Delia E, Davidson BR (2013) Peritoneal closure versus no peritoneal closure for patients undergoing non-obstetric abdominal operations. Cochrane Database Syst Rev CD010424
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370:1453–1457
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381
Joel-Cohen S (1977) Abdominal and vaginal hysterectomy. Heinemann, Portsmouth
Israelsson LA, Millbourn D (2013) Prevention of incisional hernias: how to close a midline incision. Surg Clin N Am 93:1027–1040
Israelsson LA (1999) Bias in clinical trials: the importance of suture technique. Eur J Surg 165:3–7
Israelsson LA, Millbourn D (2012) Closing midline abdominal incisions. Langenbecks Arch Surg 397:1201–1207
Sanders DL, Kingsnorth AN (2012) The modern management of incisional hernias. BMJ 344:e2843
Jairam AP, Timmermans L, Eker HH, Pierik R, van Klaveren D, Steyerberg EW et al (2017) Prevention of incisional hernia with prophylactic onlay and sublay mesh reinforcement versus primary suture only in midline laparotomies (PRIMA): 2-year follow-up of a multicentre, double-blind, randomised controlled trial. Lancet 390:567–576
van Ramshorst GH, Eker HH, Hop WC, Jeekel J, Lange JF (2012) Impact of incisional hernia on health-related quality of life and body image: a prospective cohort study. Am J Surg 204:144–150
Grimshaw J, Eccles M, Tetroe J (2014) Implementing clinical guidelines: current evidence and future implications. J Contin Educ Health Prof 24:S31–S37
Gurusamy KS, Toon CD, Davidson BR (2014) Subcutaneous closure versus no subcutaneous closure after non-caesarean surgical procedures. Cochrane Database Syst Rev CD010425
Aabakke A, Andrésdóttir G, Bjørn AB, Bødker B, Clausen TD, Gade AW et al (2016) Sectio (kejsersnit) til terminen—operationsteknik og praktisk håndtering. Dansk Selvskab for Obstetrik og Gynækologi. https://static1.squarespace.com/static/5467abcce4b056d72594db79/t/572b6012f850826350fa1b6d/1462460435938/160505++Sectio+guideline_final.pdf. Accessed 22 Apr 2020
Bloemen A, De Kleijn R, Van Steensel S, Aarts F, Schreinemacher MHF, Bouvy ND (2019) Laparotomy closure techniques: do surgeons follow the latest guidelines? Results of a questionnaire. Int J Surg 71:110–116
Livingston EH, Wislar JS (2012) Minimum response rates for survey research. Arch Surg 147:110
Aerny-Perreten N, Dominguez-Berjon MF, Esteban-Vasallo MD, Garcia-Riolobos C (2015) Participation and factors associated with late or non-response to an online survey in primary care. J Eval Clin Pract 21:688–693
Groves RM, Peytcheva E (2008) The impact of nonresponse rates on nonresponse bias: a meta-analysis. Public Opin Q 71:167–189
Edwards PJ, Roberts I, Clarke MJ, Diguiseppi C, Wentz R, Kwan I et al (2009) Methods to increase response to postal and electronic questionnaires. Cochrane Database Syst Rev MR000008
Funding
No external funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval
Ethical approval was sought but not deemed necessary by the Ethics Committee in Denmark.
Human and animal rights
There are no human and animal rights issues to declare.
Informed consent
Potential participants were sent an information e-mail with the link to the questionnaire and informed about the nature and purpose of the study. The purpose of the survey was explained in the information e-mail. Only those willing to, completed and returned the questionnaires.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Paulsen, C.B., Zetner, D. & Rosenberg, J. Variation in abdominal wall closure techniques in lower transverse incisions: a nationwide survey across specialties. Hernia 25, 345–352 (2021). https://doi.org/10.1007/s10029-020-02280-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-020-02280-w