Abstract
Purpose
Performing two anterior or two posterior inguinal hernia repairs in the same groin contradict guidelines. Nevertheless, there can be indications for using the same approach at reoperation, and information on complications other than the risk of a third repair and chronic pain is lacking in the literature. The aim was to assess intraoperative events and postoperative complications after two Lichtenstein repairs or laparoscopic inguinal hernia repairs in the same groin.
Methods
This nationwide cohort study included patients that had received two Lichtenstein repairs (Lichtenstein–Lichtenstein) or two laparoscopic (Laparoscopy–Laparoscopy) inguinal hernia repairs in the same groin. Patients were identified in the Danish Hernia Database and outcomes were identified in medical records during a period of 6 years. Outcomes were intraoperative events that deviated from a standard repair and 1-year postoperative complications classified according to the Clavien–Dindo classification. Outcomes were reported separately for the two cohorts.
Results
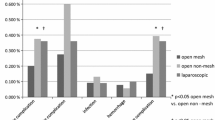
Among the included 102 Lichtenstein reoperations, 27% of the repairs had intraoperative events, with drain placement being most common (10%). Half of the reoperations resulted in complications where infection (15%) and hematoma (12%) were most frequent. Among the 58 laparoscopic reoperations, 16% had an intraoperative event where bleeding requiring clips was most common (10%). Half of the reoperations resulted in a complication with surgery in general anesthesia in the same groin area being the most frequent complication (9%).
Conclusions
Intraoperative events and 1-year postoperative complications were high for both Lichtenstein–Lichtenstein and Laparoscopy–Laparoscopy, and the results therefore support guidelines that recommend another approach at reoperation.

Similar content being viewed by others
References
HerniaSurge group (2018) International guidelines for groin hernia management. Hernia 22:1–165. https://doi.org/10.1007/s10029-017-1668-x
Simons MP, Aufenacker T, Bay-Nielsen M et al (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13:343–403. https://doi.org/10.1007/s10029-009-0529-7
Miserez M, Peeters E, Aufenacker T, Bouillot JL, Campanelli G, Conze J, Fortelny R, Heikkinen T, Jorgensen LN, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Simons MP (2014) Update with level 1 studies of the European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 18:151–163. https://doi.org/10.1007/s10029-014-1236-6
Rosenberg J, Bisgaard T, Kehlet H, Wara P, Asmussen T, Juul P, Strand L, Andersen FH, Bay-Nielsen M (2011) Danish Hernia database recommendations for the management of inguinal and femoral hernia in adults. Dan Med Bull 58:C4243
Bisgaard T, Bay-Nielsen M, Kehlet H (2008) Re-recurrence after operation for recurrent inguinal hernia A nationwide 8-year follow-up study on the role of type of repair. Ann Surg 247:707–711. https://doi.org/10.1097/SLA.0b013e31816b18e3
Öberg S, Andresen K, Rosenberg J (2016) Surgical approach for recurrent inguinal hernias: a nationwide cohort study. Hernia 20:777–782. https://doi.org/10.1007/s10029-016-1531-5
Öberg S, Andresen K, Baker JJ, Angenete E, Rosenberg J (2019) Chronic pain after reoperation of an inguinal hernia with Lichtenstein or laparoscopic repair following a primary Lichtenstein repair: a nationwide questionnaire study. Am J Surg. https://doi.org/10.1016/j.amjsurg.2019.04.015. (In press)
Öberg S, Andresen K, Nilsson H, Angenete E, Rosenberg J (2019) Chronic pain after two laparoendoscopic inguinal hernia repairs compared with laparoendoscopic repair followed by the Lichtenstein repair: an international questionnaire study. Surg Endosc. https://doi.org/10.1007/s00464-019-06853-4 (In press)
Vandenbroucke JP, von Elm E, Altman DG, Gotzsche PC, Mulrow CD, Pocock SJ, Poole C, Schlesselman JJ, Egger M (2014) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. Int J Surg 12:1500–1524. https://doi.org/10.1016/j.ijsu.2014.07.014
Friis-Andersen H, Bisgaard T (2016) The Danish inguinal Hernia database. Clin Epidemiol 8:521–524
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196. https://doi.org/10.1097/SLA.0b013e3181b13ca2
Gupta A, Kaur K, Sharma S, Goyal S, Arora S, Murthy RS (2010) Clinical aspects of acute post-operative pain management & its assessment. J Adv Pharm Technol Res 1:97–108
Uzuner O, Goldstein I, Luo Y, Kohane I (2008) Identifying patient smoking status from medical discharge records. J Am Med Inform Assoc 15:14–24
Danish Health Authority (2014) Alcohol [Internet]. https://www.sst.dk/en/health-and-lifestyle/alcohol. Accessed 13 Feb 2019.
Tonnesen H, Rosenberg J, Nielsen HJ, Rasmussen V, Hauge C, Pedersen IK, Kehlet H (1999) Effect of preoperative abstinence on poor postoperative outcome in alcohol misusers: randomised controlled trial. BMJ 318:1311–1316
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Scheuermann U, Niebisch S, Lyros O, Jansen-Winkeln B, Gockel I (2017) Transabdominal Preperitoneal (TAPP) versus Lichtenstein operation for primary inguinal hernia repair—a systematic review and meta-analysis of randomized controlled trials. BMC Surg 17:55. https://doi.org/10.1186/s12893-017-0253-7
Köckerling F, Bittner R, Kuthe A, Stechemesser B, Lorenz R, Koch A, Reinpold W, Niebuhr H, Hukauf M, Schug Pass C (2017) Laparo-endoscopic versus open recurrent inguinal hernia repair: should we follow the guidelines? Surg Endosc 31:3168–3185. https://doi.org/10.1007/s00464-016-5342-7
Emile SH, Elfeki H (2018) Desarda's technique versus Lichtenstein technique for the treatment of primary inguinal hernia: a systematic review and meta-analysis of randomized controlled trials. Hernia 22:385–395. https://doi.org/10.1007/s10029-017-1666-z
Li J, Ji Z, Cheng T (2012) Comparison of open preperitoneal and Lichtenstein repair for inguinal hernia repair: a meta-analysis of randomized controlled trials. Am J Surg 204:769–778. https://doi.org/10.1016/j.amjsurg.2012.02.010
Choi YY, Kim Z, Hur KY (2010) The safety and effectiveness of laparoscopic total extraperitoneal (TEP) repair for recurrent inguinal hernia after open hernioplasty. J Laparoendosc Adv Surg Tech A 20:537–539. https://doi.org/10.1089/lap.2010.0029
Köckerling F, Bittner R, Jacob DA, Seidelmann L, Keller T, Adolf D, Kraft B, Kuthe A (2015) TEP versus TAPP: comparison of the perioperative outcome in 17,587 patients with a primary unilateral inguinal hernia. Surg Endosc 29:3750–3760. https://doi.org/10.1007/s00464-015-4150-9
Nolsøe A, Andresen K, Rosenberg J (2016) Repair of recurrent hernia is often performed at a different clinic. Hernia 20:783–787. https://doi.org/10.1007/s10029-016-1539-x
Funding
This study received no financial support from extramural sources.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Öberg reports no potential conflicts of interest. Jessen reports no potential conflicts of interest. Andresen reports no potential conflicts of interest. Rothman reports no potential conflicts of interest. Rosenberg reports personal fees from Bard and Merck, outside the submitted work.
Ethical approval
For this type of study, ethical approval was not required
Statement of human and animal rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Öberg, S., Jessen, M.L., Andresen, K. et al. High complication rates during and after repeated Lichtenstein or laparoscopic inguinal hernia repairs in the same groin: a cohort study based on medical records. Hernia 24, 801–810 (2020). https://doi.org/10.1007/s10029-019-02083-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-019-02083-8