Abstract
Objectives
To explore the efficacy of Hyaluronic acid as an adjunctive in treatment of gingival recessions (GR).
Materials and methods
A systematic literature search was performed in several electronic databases, including Medline/ PubMed, Embase, CENTRAL and LILACS. Recession improvement was evaluated through multiple outcome variables. The Cochrane Risk of Bias tool and the ROBINS-I tool were used to assess the quality of the included trials. Weighted Mean Differences (WMDs) and 95% confidence intervals (CIs) between test and control sites were estimated through meta-analysis using a random-effect model for the amount of Relative Root Coverage (RRC).
Results
A total of 3 randomised studies were deemed as eligible for inclusion. Their data were also used for pooling the effect estimates. Overall analysis of RRC (3 studies) presented a WMD of 7.49% (p = 0.42; 95% CIs -10.88, 25.86) in favour of adjunctive use of hyaluronic acid during Coronally Advanced Flap (CAF) technique, although statistical significance was not reached. Statistical heterogeneity was found to be high (I2 = 80%).
Conclusions
Within their limitations, the present data indicate that the local application of Hyaluronic acid does not lead to additional clinical benefits when used as an adjunctive to the treatment of GR with CAF. However, due to the high heterogeneity among the studies, additional well-designed RCTs are needed to provide further evidence on this clinical indication for the use of Hyaluronic acid.
Clinical relevance
In the frame of the current review, the adjunctive use of Hyaluronic acid does not additionally improve the clinical outcomes obtained during treatment of GR with CAF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Gingival recession (GR) may become a major source of concern for both the practitioner and the patient; defined as an apical shift of the gingival margin with respect to the cemento-enamel junction, it leads to exposure of a root surface’s portion [1, 2]. This situation can be either localized or generalized and in conjunction to one or more tooth surfaces [3] and it has been related to several triggering factors such as traumatic toothbrushing, periodontal disease and orthodontic tooth movement [4,5,6].
As recession develops, several problems may also arise including compromised aesthetics, root caries and dental hypersensitivity [7], forcing patients to seek treatment.
Epidemiological studies have revealed that gingival recessions affect the majority of the adult population and in fact its prevalence, extent and severity seem to increase with age [8], thus making the management of recessions a serious concern for every clinician.
Several surgical techniques have been already proposed in order to address this clinical problem, by achieving complete root coverage, including coronally advanced flaps (CAF), laterally repositioned flaps and tunnel techniques [9, 10]. The existing evidence supports the concurrent use of CAF with sub-epithelial connective tissue grafts (SCTG) as the “golden standard” procedure for achieving optimal results [11]. Additionally, several biomaterials have been examined as possible adjunctive of root coverage procedures in order to avoid patient morbidity, such as enamel matrix derivative, collagen matrices and acellular dermal matrices [12,13,14].
Hyaluronic acid (HA), an anionic, non-sulfated glycosaminoglycan and a major component of the extracellular matrix in most tissues, is being used in various regenerative medical and tissue engineering approaches [15]. Recently, it has been studied as a possible adjacent treatment in periodontal [16] and implant surgery [17].
Several studies have shown HA’s positive effect on wound healing and tissue regeneration, by its properties of stimulating cell adhesion, migration and proliferation, mediation of cell signalling [18], clot formation, inducing angiogenesis, limiting bacterial contamination and stabilizing granulation tissue [19,20,21,22].
To the best of our knowledge, there is currently a lack of studies systematically evaluating all possible study designs that assess the possible benefits from the use of HA in root coverage procedures in order to provide the clinicians with up to date clinical evidence [23].
Therefore, the aim of the current systematic review was to explore the efficacy of hyaluronic acid as an adjunctive in treatment of gingival recessions.
Materials and methods
Registration of the study protocol
The study protocol was submitted to the PROSPERO international prospective register of systematic reviews hosted by the National Institute for Health Research (NIHR), University of York, UK, Center for Reviews and Dissemination and was allocated the identification number CRD42022321748.
Reporting format
The latest (2021) Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) were adopted throughout the process of the present systematic review [24].
Focused question and PICOS schema—Population (P), Intervention (I), Comparison (C), Outcomes (O) and study design
Focused question
In the surgical treatment of patients with gingival recessions, how efficacious is the adjunctive use of HA in comparison to standard treatment without supplementary use of HA, in terms of GR reduction?
Eligibility criteria
Studies meeting the following in inclusion criteria were included:
-
Population: Patients with any type of gingival recessions in mandibular or maxillary teeth
-
Intervention: Root coverage procedure with the adjunctive use of HA
-
Comparison: Root coverage procedures without adjunctive use of HA
-
Outcomes: GR reduction/ Complete Root Coverage (CRC)/ Relative Root Coverage (RRC)/ Recession Depth (RD)/ Recession Reduction (RR)/ Recession Width (RW) as primary outcome variables and gain in Clinical attachment level (CAL) / Periodontal pocket depth (residual or closure) (PPD)/ gain in Keratinized Tissue Width (KTW)/ Patient morbidity/ Change in bleeding on probing (BoP)/ Plaque Index (PI)/ Patient-related outcome measures (PROMs) such as pain, satisfaction, discomfort/ Quality of Life indicators and economic factors/ Root coverage Esthetic Score (RES), as secondary variables.
-
Study design: Any study design was considered eligible for inclusion in this review, including randomized clinical trials (RCTs), non-randomized studies, prospective and retrospective studies. Case reports and case series were excluded. Follow up: All observation periods were accepted.
Exclusion criteria
-
i.
Studies with insufficient information about the study design/ Pre-clinical studies/ Abstracts/ Letters to editors
-
ii.
Studies that included individuals with systemic diseases.
Search strategy
Detailed search strategies were developed and appropriately revised for each database, considering the differences in controlled vocabulary and syntax rules by the last author (DK). No language or publication date restrictions were applied.
Electronic search
We searched the following electronic databases to find reports of relevant published studies up to 01.06.2023:
-
The Cochrane Central Register of Controlled Trials (CENTRAL);
-
MEDLINE (PubMed and via OVID);
-
Ovid EMBASE
-
LILACS
The full search strategy of Medline/ Pubmed is shown in Appendix 1.
Unpublished literature search
In order to further identify potential articles for inclusion, grey literature and possible ongoing trials were researched in the register of clinical studies hosted by the US National Institutes of Health (www.clinicaltrials.gov), the multidisciplinary European database (www.opengrey.eu), the National Research Register, and Pro-Quest Dissertation Abstracts and Thesis databases (https://about.proquest.com).
Manual search
Researchers engaging with the field were contacted in pursuit of additional relevant literature. All identified eligible studies ’reference lists were screened and manual searching of other published systematic reviews was conducted in order to obtain additional studies.
Study selection
All study selection steps were performed independently and in duplicate by two authors of the review (EK, EO), who were aware of study author identity, institution and study outcomes. Study selection comprised title-, abstract- and full-text-reading phases. After exclusion of non-eligible studies, discrepancies concerning the eligible studies were resolved by discussion with the third author of the review (AS). A record of all decisions on study identification was kept.
Data collection
Three authors were involved in data extraction. Data were initially extracted independently and in duplicate by the first two authors (EK, AB). Disagreements were resolved by discussion with the last author (DK). Data relating to the following study characteristics were collected: Author/ title/ year of study, study design, study aim, exclusion criteria, number/age/gender of patients, types of intervention across groups, follow-up period, outcome assessed, method of outcome assessment, measure of outcome, results and conclusion.
If stated, the sources of funding, trial registration, and publishing of the trial's protocol was recorded. This information was used to facilitate the assessment of heterogeneity and the external validity of the included studies.
Quality assessment
The methodological quality assessment of the included studies implemented the Revised Cochrane risk-of-bias tool (Rob 2) for the randomized trials [25] and the ROBINS-I tool for the non-randomised studies [26]. The studies were assessed individually and in duplicate by two reviewers (AR, AS) and their findings were compared. The last author (DK) was consulted to resolve any concerns on the quality assessment process.
Data analysis
Meta-analyses were conducted for studies reporting on similar interventions, comparisons and the same outcome measures in homogeneous populations. For continuous variables, mean differences and standard deviations were used to summarize the data gathered from each study. Regarding meta-analysis for continuous data, weighted mean differences (WMDs) and 95% Cls were calculated.
Heterogeneity
Examination of the study characteristics, the similarity between types of participants, the interventions, and the outcomes as specified in the inclusion criteria for considering studies for this review was performed in order to assess clinical and methodological heterogeneity. Statistical heterogeneity was reported by means of a Chi2 test and I2 statistic.
Assessment of reporting bias
Reporting bias arises when the nature or direction of the findings affects the reporting of research findings [27]. Potential reporting biases including publication bias, multiple (duplicate reports) publications and language bias were reduced by conducting an accurate and at the same time a sensitive search of multiple sources with no language restriction. Also, a search for ongoing trials was performed.
Subgroup analyses / Sensitivity analysis
As no sufficient data existed, subgroup analyses based on study characteristics or sensitivity analysis based on the risk of bias were not conducted.
Unit of analysis issues
We anticipated that some of the included studies presented data from repeated observations on participants, which could lead to unit-of-analysis errors. In such cases, we followed the advice provided in section 9.3.4 of the Cochrane Handbook for Systematic Reviews of Interventions [27].
Results
Description of studies
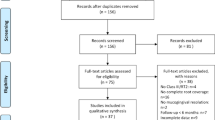
The initial electronic search yielded 74 records. After title and abstract screening, 8 studies were further examined for eligibility in their full-text forms. In addition, 1 more study was identified through hand searching and was included in the study. After full-text reading, 6 studies were excluded, resulting in a total of 3 studies eligible for inclusion [28,29,30]. All 3 studies were RCTs (Tables 1 and 2). Two case series studies were excluded, although reporting relevant data, due to their design [31, 32]. The study selection process is presented in Fig. 1.
Quality assessment
Randomized clinical trials
The RCT of Pilloni et al. was rated at an overall low risk, due to the low risk of bias that was applied to each domain based on the Cochrane risk of bias Robins 2 tool [28]. The RCTs conducted by Kumar et al. [29] and Rajan et al. [30] were judged to be at an overall high risk of bias, as the method of patient selection and allocation concealment were not described. Detailed assessment of the RCTs is provided in Table 3.
Comparison of Complete Root Coverage (CRC)
The incidence of CRC was assessed in one study, where it was evaluated as the number of teeth with complete coverage of the recession defect after the root coverage procedure. The findings of Pilloni et al. in a RCT comparing the effect of application of HA in conjunction with coronally advanced flap (CAF) (test group, n = 15) to CAF alone (control group, n = 15) on single Miller class I/recession type 1 (RT1) gingival recessions, yielded that the application of HA provided increased probability of CRC. CRC was achieved in 80% of the test group and 33.3% of the control group (p < 0.05) [28].
Comparison of Relative Root Coverage (RRC)
The percentage of RRC, considering the reduction in recession depths at different time intervals, was assessed in all studies. The RCT of Pilloni et al. [28] found statistically greater improvement in RRC (p < 0.005) in the test group, which was treated with CAF and cross-linked HA application before flap suture (93.8 ± 13.08%), compared to the control group, which was treated with CAF only (73.1 ± 20.8%). RRC percentage was also higher in the test group in the 3-month clinical evaluation [test group: 58.43 (± 8.80)], control group: [48.07 (± 13.35)] (p = 0.005), in the RCT of Rajan et al. [30]. The test group was treated with CAF and HA, while, in the control group, a SCTG was harvested and CAF technique was performed. Likewise, a split-mouth RCT reported that higher RRC was obtained with CAF and HA application before flap advancement (68.33 ± 28.81 mm) than with CAF alone (61.67 ± 30.22 mm) in a 6-month follow-up examination [29].
Periodontal Probing Depth (PPD)
PPD was recorded in all the included studies. Even though Rajan et al. recorded lower probing depths in the control group during the 3- and 9- month examination, no other study revealed statistically significant differences regarding this parameter between groups at any of the time points [28,29,30]. It has been to be noted, though, that baseline PPD scores were significantly different between groups in this study.
Recession Depth (RD) and Recession Reduction (RR)
The depth of the recession defect, measured from the cemento-enamel junction to the gingival margin, was recorded in 3 RCTs. In the RCT of Pilloni et al., depth decreased more (p < 0.05) in the test group (CAF and HA application before flap suture) than in the control group (CAF alone), however, the median depth decreased significantly for both groups from baseline to 18 months after intervention [28]. According to the study of Rajan et al., more improvement in depth was observed in the test group (CAF + HA) in 1 month after intervention. No other differences were revealed between groups during the rest observation period [30]. Kumar et al. in their split-mouth RCT reported that the differences in recession depth values between groups were not statistically significant [29].
RR was evaluated as a separate clinical parameter in the study of Pilloni et al., where more reduction was attained in the test group (CAF and HA application before flap suture) (2.7 ± 1 mm) than in the control group (CAF alone) (1,9 ± 1 mm) from baseline to the 18-month evaluation [28].
Clinical Attachment Level (CAL)
Measurements of CAL were obtained in three studies at baseline and follow-up examinations and were calculated as the sum of PPD and RD at the midfacial site of the tooth. Pilloni et al. demonstrated a greater improvement in CAL (p < 0.05) in the group treated with CAF and HA application (3 ± 1 mm) than in the control group (2 ± 1 mm) [28]. Similarly, in the study of Rajan et al., CAL measurements improved more for the test group (CAF + HA), when compared to those of the control group (SCTG + CAF) [3 months: higher level in test group [2.55 (± 1.10)] than in control group [3.05 (± 0.83)] (p < 0.05) and 9 months: higher level in test group [1.90 (± 1.07)] than in control group [1.10 (± 0.91)] (p < 0.005) [30]. In the contrary, Kumar et al. found no significant differences in CAL between the test (CAF and HA) and control group (CAF alone) at follow-up examinations [29].
Keratinized Tissue Width (KTW)
KTW was investigated in two studies and was calculated as the distance between the gingival margin and the mucogingival junction at the midfacial point of each tooth. In the RCT conducted by Pilloni et al., no differences were found concerning the KTW between baseline and follow-ups or between test (CAF and HA) and control (CAF alone) group [28]. The differences between the test (CAF + HA) and control group (SCTG + CAF) were also non-significant in the study of Rajan et al. [30].
Post-operative patient morbidity
Patient morbidity was evaluated by Pilloni et al. through Visual Analogue Scale questionnaires at 7 days after intervention. With respect to pain intensity, there were no differences between the test (CAF and HA) and control group (CAF alone), while swelling and discomfort were rated as lower in the test group (p = 0.010 and p = 0.029, respectively) [28].
Quantitative synthesis of included studies
A meta-analysis was only feasible for RRC. Despite the methodological heterogeneity, mainly in terms of follow-up, we have decided to report the meta-analysis and highlight its limitations. Data from 3 studies were used for meta-analysis [28,29,30]. Overall analysis of RRC presented a WMD of 7.49% (p = 0.42; 95% CIs -10.88, 25.86) in favor of adjunctive use of hyaluronic acid, although statistical significance was not reached. Statistical heterogeneity was found to be high (I2 = 80%) (Fig. 2).
Discussion
The aim of the present study was to assess the level of evidence on the use of HA in the treatment of gingival recessions. Based on the best available evidence (i.e. three RCTs) no conclusions could be drawn with respect to the adjunctive clinical efficacy of HA.
It is well documented that to provide the best outcomes in terms of mean and complete root coverage, as well as to increase keratinized tissue, SCTG is the most effective therapeutic approach for Miller Class I and II single-tooth recessions, as concluded in the consensus report of the 2015 AAP Regeneration Workshop. Nevertheless, following the harvesting procedure, some post-operative sequelae such as patient’s discomfort have been reported [33]. Consequently, the use of alternative biomaterials, such as acellular dermal matrix graft [34] or enamel matrix derivative [35] have been proposed to serve as alternatives to autogenous tissue and have been described as less painful, whereas use of palatal tissue as a donor site has been related to increased complications [33]. More specifically, research concerning gingival recession treatment always focused on exploring convenient alternatives to reduce patient morbidity and maximize the intervention predictability [36,37,38,39].
A critical factor determining the outcome of root coverage procedures, apart from excellent surgical technique, is the undisturbed wound healing process. Recently, the application of HA on the surgical area has been proposed based on its characteristics which promote the early wound healing phases; during the inflammatory phase of wound healing, HA has been shown to enhance inflammatory cell migration, proinflammatory cytokine production and stabilization of granulation matrix. Thereby, HA exerts its effects through two main routes, firstly via HA receptors such as CD44 that are present on cell membranes of nearly all human cells and by providing a wound-microenvironment that enables optimal healing [40, 41]. Subsequently, in the granulation phase, HA promotes the extracellular matrix cell proliferation and migration, and facilitates angiogenesis. Lastly, HA aids in epithelium formation [42]. Thus, it is expected that the addition of HA to root coverage procedures will have a positive effect in terms of CRC and RRC increase.
The ideal goal of every mucogingival surgical intervention is to obtain the CRC [43, 44]. HA application combined with a CAF, CRC was detected in a higher percentage of cases compared to CAF alone [28]. On the other hand, other studies which applied HA in combination with a SCTG and a tunnel technique, reported a CRC in 50 and 20% of single and multiple recessions [31, 32]. A plausible explanation for this difference is the fact that treating multiple recessions is often a more demanding surgical procedure with increased risk of complications during the healing process [45].
When focusing on the RRC, 2 out of the 3 RCTs reported better results in the test compared to the control group, supporting the assumption that HA may facilitate a more favorable wound healing process and, thus, more satisfactory clinical results (Fig. 2). Considering the study of Rajan et al. [30], that was included in this meta-analysis, it has to be noted that the patient oral hygiene motivation may decrease significantly after 6 months post-op; in that frame, late success may not always be achievable.
When focusing on the KTW, no differences were detected in the studies of Pilloni et al. [28] and Rajan et al. [30]. With respect to the periodontal parameters (i.e. CAL and PD), in the RCTs of Pilloni et al. and Rajan et al., more improvement was observed in the test groups [28, 30]. The explanation of this difference may again lie on the basis of the HA biological properties on wound healing modulation [16, 42, 46]. On the other hand, Kumar et al. reported no differences in CAL between the groups (CAF and HA before flap advancement, CAF alone) at the 24-week follow-up, even though the CAL gain was significant for both groups [30]. In contrast to some studies which reported positive results in terms of PPD reduction following non-surgical periodontal treatment and local application of HA [47, 48], the present studies did not detect statistically significant changes at any follow-ups.
One of the aspects that has to be taken into consideration when performing mucogingival procedures, is patient morbidity and mainly pain perception [49]: in the study by Pilloni and co-workers [28], the application of HA resulted in statistically significant, although minor, improvements in swelling and discomfort, as compared to the control group. These outcomes may again be explained by the angiogenic properties of HA, its role as a hydrating active ingredient and its contribution in the regulation of inflammation, through enhancing the lymphocyte, inflammatory, and connective tissue cell motility [20, 42, 46, 50,51,52].
Nevertheless, it has to be pointed out that despite the biologically plausible effects of HA with respect to wound healing and regeneration, the clinical evidence for the adjunctive application of HA to recession coverage surgery is still very limited. A recent systematic review, including 3 studies, also reached the same conclusion [53].
Limitations
Limitations of this review were foremost the shortage of studies eligible for inclusion, as well as the included studies’ design. The meta-analysis included RCTs with various follow up periods: 6 months for the study of Kumar et al. [29], 9 months for the study of Rajan et al. [30] and 18 months for the study of Pilloni et al. [28]. Despite this fact, the review team has accepted 6 month follow up as adequate to retrieve clinically significant results.
Conclusions
Given the limited available evidence, as well as the paucity of high-quality evidence, valid inferences concerning possible effect of HA on root coverage procedure could not be drawn. Therefore, further research is required to improve the quality of evidence concerning this topic.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Cortellini P, Bissada NF (2018) Mucogingival conditions in the natural dentition: narrative review, case definitions, and diagnostic considerations. J Clin Periodontol 45:S190–S198. https://doi.org/10.1111/jcpe.12948
Pini Prato G (1999) Mucogingival deformities. Ann Periodontol 4(1):98–101. https://doi.org/10.1902/annals.1999.4.1.98
Kassab MM, Cohen RE (2003) The etiology and prevalence of gingival recession. JADA 134(2):220–225. https://doi.org/10.14219/jada.archive.2003.0137
Joss-Vassalli I, Grebenstein C, Topouzelis N, Sculean A, Katsaros C (2010) Orthodontic therapy and gingival recession: a systematic review. Orthod Craniofac Res 13(3):127–141. https://doi.org/10.1111/j.1601-6343.2010.01491.x
Löe H, Anerud A, Boysen H (1992) The natural history of periodontal disease in man: prevalence, severity, and extent of gingival recession. J Periodontol 63(6):489–495. https://doi.org/10.1902/jop.1992.63.6.489
Khocht A, Simon G, Person P, Denepitiya JL (1993) Gingival recession in relation to history of hard toothbrush use. J Periodontol 64(9):900–905. https://doi.org/10.1902/jop.1993.64.9.900
Roccuzzo M, Bunino M, Needleman I, Sanz M (2002) Periodontal plastic surgery for treatment of localized gingival recessions: a systematic review. J Clin Periodontol 29(Suppl 3):178–194. https://doi.org/10.1034/j.1600-051x.29.s3.11.x
Susin C, Haas AN, Oppermann RV, Haugejorden O, Albandar JM (2004) Gingival recession: epidemiology and risk indicators in a representative urban Brazilian population. J Periodontol 75(10):1377–1386. https://doi.org/10.1902/jop.2004.75.10.1377
Buti J, Baccini M, Nieri M, La Marca M, Pini-Prato GP (2013) Bayesian network meta-analysis of root coverage procedures: ranking efficacy and identification of best treatment. J Clin Periodontol 40(4):372–386. https://doi.org/10.1111/jcpe.12028
Hofmänner P, Alessandri R, Laugisch O, Aroca S, Salvi GE, Stavropoulos A, Sculean A (2012) Predictability of surgical techniques used for coverage of multiple adjacent gingival recessions–a systematic review. Quintessence Int 43(7):545–554
Chambrone L, Chambrone D, Pustiglioni FE, Chambrone LA, Lima LA (2008) Can subepithelial connective tissue grafts be considered the gold standard procedure in the treatment of Miller Class I and II recession-type defects? J Dent 36(9):659–671. https://doi.org/10.1016/j.jdent.2008.05.007
Del Pizzo M, Zucchelli G, Modica F, Villa R, Debernardi C (2005) Coronally advanced flap with or without enamel matrix derivative for root coverage: a 2-year study. J Clin Periodontol 32(11):1181–1187. https://doi.org/10.1111/j.1600-051X.2005.00831.x
Aroca S, Molnár B, Windisch P, Gera I, Salvi GE, Nikolidakis D, Sculean A (2013) Treatment of multiple adjacent Miller class I and II gingival recessions with a Modified Coronally Advanced Tunnel (MCAT) technique and a collagen matrix or palatal connective tissue graft: a randomized, controlled clinical trial. J Clin Periodontol 40(7):713–720. https://doi.org/10.1111/jcpe.12112
Woodyard JG, Greenwell H, Hill M, Drisko C, Iasella JM, Scheetz J (2004) The clinical effect of acellular dermal matrix on gingival thickness and root coverage compared to coronally positioned flap alone. J Periodontol 75(1):44–56. https://doi.org/10.1902/jop.2004.75.1.44
Neuman MG, Nanau RM, Oruña-Sanchez L, Coto G (2015) Hyaluronic acid and wound healing. J Pharm Pharm Sci 18(1):53–60. https://doi.org/10.18433/j3k89d
Casale M, Moffa A, Vella P, Sabatino L, Capuano F, Salvinelli B, Lopez MA, Carinci F, Salvinelli F (2016) Hyaluronic acid: perspectives in dentistry. A systematic review. Int J Immunopathol Pharmacol 29(4):572–582. https://doi.org/10.1177/0394632016652906
Castro-Calderón A, Roccuzzo A, Ferrillo M, Gada S, González-Serrano J, Fonseca M, Molinero-Mourelle P (2022) Hyaluronic acid injection to restore the lost interproximal papilla: a systematic review. Acta Odontol Scand 80(4):295–307. https://doi.org/10.1080/00016357.2021.2007282
Bartold PM, Wiebkin OW, Thonard JC (1981) Glycosaminoglycans of human gingival epithelium and connective tissue. Connect Tissue Res 9(2):99–106. https://doi.org/10.3109/03008208109160247
Scully MF, Kakkar VV, Goodwin CA, O’Regan M (1995) Inhibition of fibrinolytic activity by hyaluronan and its alcohol ester derivatives. Thromb Res 8(3):255–258. https://doi.org/10.1016/0049-3848(95)90876-h
West DC, Hampson IN, Arnold F, Kumar S (1985) Angiogenesis induced by degradation products of hyaluronic acid. Science (New York, N.Y.) 228(4705):1324–1326. https://doi.org/10.1126/science.2408340
Pirnazar P, Wolinsky L, Nachnani S, Haake S, Pilloni A, Bernard GW (1999) Bacteriostatic effects of hyaluronic acid. J Periodontol 70(4):370–374. https://doi.org/10.1902/jop.1999.70.4.370
de Brito BB, Mendes Brazão MA, de Campos ML, Casati MZ, Sallum EA, Sallum AW (2012) Association of hyaluronic acid with a collagen scaffold may improve bone healing in critical-size bone defects. Clin Oral Implants Res 23(8):938–942. https://doi.org/10.1111/j.1600-0501.2011.02234.x
Eliezer M, Imber JC, Sculean A, Pandis N, Teich S (2019) Hyaluronic acid as adjunctive to non-surgical and surgical periodontal therapy: a systematic review and meta-analysis. Clin Oral Investig 23(9):3423–3435. https://doi.org/10.1007/s00784-019-03012-w
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng HY, Corbett MS, Eldridge SM, Emberson JR, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 28(366):l4898. https://doi.org/10.1136/bmj.l4898
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan AW, Churchill R, Deeks JJ, Hróbjartsson A, Kirkham J, Jüni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schünemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins JP, Thomas J (2019) Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev 10:ED000142
Pilloni A, Schmidlin PR, Sahrmann P, Sculean A, Rojas MA (2019) Effectiveness of adjunctive hyaluronic acid application in coronally advanced flap in Miller class I single gingival recession sites: a randomized controlled clinical trial. Clin Oral Investig 23(3):1133–1141. https://doi.org/10.1007/s00784-018-2537-4
Kumar R, Srinivas M, Pai J, Suragimath G, Prasad K, Polepalle T (2014) Efficacy of hyaluronic acid (hyaluronan) in root coverage procedures as an adjunct to coronally advanced flap in Millers Class I recession: a clinical study. J Indian Soc Periodontol 18(6):746–750. https://doi.org/10.4103/0972-124X.147411
Rajan P, Rao N, Nera M, Rahaman S (2015) Hyaluronon As an adjunct to coronally advanced flap for the treatment of gingival recession defects – a clinical study. Natl J Integr Res Med 6(2):94–100
Guldener K, Lanzrein C, Eliezer M, Katsaros C, Stähli A, Sculean A (2020) Treatment of single mandibular recessions with the modified coronally advanced tunnel or laterally closed tunnel, hyaluronic acid, and subepithelial connective tissue graft: a report of 12 cases. Quintessence Int 51(6):456–463. https://doi.org/10.3290/j.qi.a44492
Lanzrein C, Guldener K, Imber JC, Katsaros C, Stähli A, Sculean A (2020) Treatment of multiple adjacent recessions with the modified coronally advanced tunnel or laterally closed tunnel in conjunction with cross-linked hyaluronic acid and subepithelial connective tissue graft: a report of 15 cases. Quintessence Int 51(9):710–719. https://doi.org/10.3290/j.qi.a44808
Tatakis DN, Chambrone L, Allen EP, Langer B, McGuire MK, Richardson CR, Zabalegui I, Zadeh HH (2015) Periodontal soft tissue root coverage procedures: a consensus report from the AAP Regeneration Workshop. J Periodontol 86(2 Suppl):S52–S55. https://doi.org/10.1902/jop.2015.140376
Felipe ME, Andrade PF, Grisi MF, Souza SL, Taba M, Palioto DB, Novaes AB (2007) Comparison of two surgical procedures for use of the acellular dermal matrix graft in the treatment of gingival recessions: a randomized controlled clinical study. J Periodontol 78(7):1209–1217. https://doi.org/10.1902/jop.2007.060356
Stähli A, Imber JC, Raptis E, Salvi GE, Eick S, Sculean A (2020) Effect of enamel matrix derivative on wound healing following gingival recession coverage using the modified coronally advanced tunnel and subepithelial connective tissue graft: a randomised, controlled, clinical study. Clin Oral Investig 2:1043–1051. https://doi.org/10.1007/s00784-019-03008-6
Zucchelli G, Mounssif I, Mazzotti C, Montebugnoli L, Sangiorgi M, Mele M, Stefanini M (2014) Does the dimension of the graft influence patient morbidity and root coverage outcomes? A randomized controlled clinical trial. J Clin Periodontol 41(7):708–716. https://doi.org/10.1111/jcpe.12256
Stefanini M, Mounssif I, Barootchi S, Tavelli L, Wang HL, Zucchelli G (2020) An exploratory clinical study evaluating safety and performance of a volume-stable collagen matrix with coronally advanced flap for single gingival recession treatment. Clin Oral Investig 24(9):3181–3191. https://doi.org/10.1007/s00784-019-03192-5
Martin-Cabezas R, Deschamps-Lenhardt S, Huck O (2021) Optimization of connective tissue graft length by graft splitting: a case series. Clin Adv Periodontics 11(3):165–170. https://doi.org/10.1002/cap.10175
McGuire MK, Tavelli L, Feinberg SE, Rasperini G, Zucchelli G, Wang HL, Giannobile WV (2020) Living cell-based regenerative medicine technologies for periodontal soft tissue augmentation. J Periodontol 91(2):155–164. https://doi.org/10.1002/JPER.19-0353
Aruffo A, Stamenkovic I, Melnick M, Underhill CB, Seed B (1990) CD44 is the principal cell surface receptor for hyaluronate. Cell 61(7):1303–1313. https://doi.org/10.1016/0092-8674(90)90694-a
Litwiniuk M, Krejner A, Speyrer MS, Gauto AR, Grzela T (2016) Hyaluronic acid in inflammation and tissue regeneration. Wounds 28(3):78–88
Moseley R, Waddington RJ, Embery G (2002) Hyaluronan and its potential role in periodontal healing. Dent Update 29(3):144–8. https://doi.org/10.12968/denu.2002.29.3.144
Bertl K, Spineli LM, Mohandis K, Stavropoulos A (2021) Root coverage stability: a systematic overview of controlled clinical trials with at least 5 years of follow-up. Clin Exp Dent Res 7(5):692–710. https://doi.org/10.1002/cre2.395
Chambrone L, Ortega MAS, Sukekava F, Rotundo R, Kalemaj Z, Buti J, Prato GPP (2019) Root coverage procedures for treating single and multiple recession-type defects: an updated Cochrane systematic review. J Periodontol 90(12):1399–1422. https://doi.org/10.1002/JPER.19-0079
Chambrone L, Lima LA, Pustiglioni FE, Chambrone LA (2009) Systematic review of periodontal plastic surgery in the treatment of multiple recession-type defects. J Can Dent Assoc 75(3):203a–203f
Ferguson EL, Roberts JL, Moseley R, Griffiths PC, Thomas DW (2011) Evaluation of the physical and biological properties of hyaluronan and hyaluronan fragments. Int J Pharm 420(1):84–92. https://doi.org/10.1016/j.ijpharm.2011.08.031
Johannsen A, Tellefsen M, Wikesjö U, Johannsen G (2009) Local delivery of hyaluronan as an adjunct to scaling and root planing in the treatment of chronic periodontitis. J Periodontol 80(9):1493–1497. https://doi.org/10.1902/jop.2009.090128
Eick S, Renatus A, Heinicke M, Pfister W, Stratul SI, Jentsch H (2013) Hyaluronic acid as an adjunct after scaling and root planing: a prospective randomized clinical trial. J Periodontol 84(7):941–949. https://doi.org/10.1902/jop.2012.120269
Zucchelli G, Tavelli L, McGuire MK, Rasperini G, Feinberg SE, Wang HL, Giannobile WV (2020) Autogenous soft tissue grafting for periodontal and peri-implant plastic surgical reconstruction. J Periodontol 91(1):9–16. https://doi.org/10.1002/JPER.19-0350
Singer AJ, Clark RA (1999) Cutaneous wound healing. N Engl J Med 341(10):738–746. https://doi.org/10.1056/NEJM199909023411006
Chen WY, Abatangelo G (1999) Functions of hyaluronan in wound repair. Wound Repair Regen 7(2):79–89. https://doi.org/10.1046/j.1524-475x.1999.00079.x
Weigel PH, Frost SJ, McGary CT, LeBoeuf RD (1988) The role of hyaluronic acid in inflammation and wound healing. Int J Tissue React 10(6):355–365
Mehta V, Kaçani G, Moaleem MMA et al (2022) Hyaluronic acid: a new approach for the treatment of gingival recession-a systematic review. Int J Environ Res Public Health 19(21):14330. https://doi.org/10.3390/ijerph192114330
Funding
Open access funding provided by University of Bern No funding was acquired at any review stage.
Author information
Authors and Affiliations
Contributions
D.K and A.S contributed to the study conception and design, and E.K, E.O. and A.R, to the material preparation and data collection. D.K performed the statistical analysis. A.R and A. St. critically revised the manuscript and supervised the review process. The first draft of the manuscript was written by A.B., A.R. and A. St. and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Due to the nature of the present study with no patients ’involvement, ethical committee approval was not sought.
Consent to participate
To perform the present study, informed consent was not required.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kalimeri, E., Roccuzzo, A., Stähli, A. et al. Adjunctive use of hyaluronic acid in the treatment of gingival recessions: a systematic review and meta-analysis. Clin Oral Invest 28, 329 (2024). https://doi.org/10.1007/s00784-024-05701-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00784-024-05701-7