Abstract
Objectives
This meta-analysis aimed to elucidate the effects of various acid etching patterns on the sensitivity of teeth and their clinical effectiveness following composite resin repair.
Materials and methods
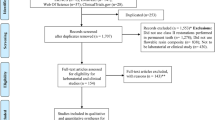
PubMed, Cochrane Library, Web of Science, and Embase databases were searched for relevant studies on the postoperative sensitivity (POS) of composite resin restorations after using different bonding systems. The retrieval was from the inception of the databases to August 13, 2022, with no filter of written language. Literature screening was conducted by two independent researchers. The Cochrane risk-of-bias assessment tool was adopted for quality evaluation, and Stata 15.0 for analysis.
Results
Twenty-five randomized controlled trials were included in the present study. Following resin composite restoration, 1309 restorations were bonded by self-etching (SE) adhesives, whereas 1271 restorations were bonded by total-etching (TE) adhesives. The meta-analyses showed that there is no evidence to prove the SE and TE will affect POS at present when measured using the modified United States Public Health Service (USPHS) criteria [RR = 1.00 (95% CI: 0.96, 1.04)], the World Dental Federation (FDI) [RR = 1.06 (95% CI: 0.98, 1.15)], or the visual analog scale (VAS) [SMD = 0.02 (95% CI: −0.15, 0.20)] scales. At a certain follow-up time, TE adhesives provide better outcomes in terms of color match, marginal staining, and marginal adaptation. In other words, TE adhesives have better esthetic results.
Conclusions
The type of bonding technique (ER and SE) does not affect the risk and degree of POS in class I/II and class V restorations. Further research is required to verify whether these findings apply to different forms of composite resin restorations.
Clinical relevance
Besides the fact that TE barely increase postoperative sensitivity, it also yields superior cosmetic results.







Similar content being viewed by others
References
Perdigão J, Araujo E, Ramos RQ, Gomes G, Pizzolotto L (2021) Adhesive dentistry: current concepts and clinical considerations. J Esthet Restor Dent 33:51–68. https://doi.org/10.1111/jerd.12692
Rosa WL, Piva E, Silva AF (2015) Bond strength of universal adhesives: a systematic review and meta-analysis. J Dent 43:765–776. https://doi.org/10.1016/j.jdent.2015.04.003
Yin H, Kwon S, Chung SH, Kim RJY (2022) Performance of universal adhesives in composite resin repair. Biomed Res Int 2022:7663490. https://doi.org/10.1155/2022/7663490
Bedran-Russo A, Leme-Kraus AA, Vidal CMP, Teixeira EC (2017) An overview of dental adhesive systems and the dynamic tooth–adhesive interface. Dent Clin North Am 61:713–731. https://doi.org/10.1016/j.cden.2017.06.001
Cuevas-Suárez CE, da Rosa WLO, Lund RG, da Silva AF, Piva E (2019) Bonding performance of universal adhesives: an updated systematic review and meta-analysis. J Adhes Dent 21:7–26. https://doi.org/10.3290/j.jad.a41975
Schroeder M, Correa IC, Bauer J, Loguercio AD, Reis A (2017) Influence of adhesive strategy on clinical parameters in cervical restorations: a systematic review and meta-analysis. J Dent 62:36–53. https://doi.org/10.1016/j.jdent.2017.05.006
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
Higgins JPTSJ, Page MJ, Elbers RG, Sterne JAC (2022) Chapter 8: assessing risk of bias in a randomized trial. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (eds) Cochrane handbook for systematic reviews of interventions version 6.3 (updated February 2022), Cochrane
Kim K-L, Cheol N, Cho B-H (2013) The effect of clinical performance on the survival estimates of direct restorations. Restor Dent Endod 38:11–20. https://doi.org/10.5395/rde.2013.38.1.11
Hickel R, Peschke A, Tyas M, Mjör I, Bayne S, Peters M, Hiller K-A, Randall R, Vanherle G, Heintze SD (2010) FDI World Dental Federation - clinical criteria for the evaluation of direct and indirect restorations. Update and clinical examples. Clin Oral Investig 14(4):349–366. https://doi.org/10.1007/s00784-010-0432-8
Atalay C, Ozgunaltay G, Yazici AR (2020) Thirty-six-month clinical evaluation of different adhesive strategies of a universal adhesive. Clin Oral Investig 24:1569–1578. https://doi.org/10.1007/s00784-019-03052-2
Bekes K, Boeckler L, Gernhardt CR, Schaller HG (2007) Clinical performance of a self-etching and a total-etch adhesive system - 2-year results. J Oral Rehabil 34:855–861. https://doi.org/10.1111/j.1365-2842.2007.01745.x
Chermont AB, Carneiro KK, Lobato MF, Machado SMM (2010) Clinical evaluation of postoperative sensitivity using self-etching adhesives containing glutaraldehyde. Braz Oral Res 24:349–354. https://doi.org/10.1590/s1806-83242010000300015
Costa C, Albuquerque N, Mendonça JS, Loguercio AD, Saboia V, Santiago SL (2020) Catechin-based dentin pretreatment and the clinical performance of a universal adhesive: a two-year randomized clinical trial. Oper Dent 45:473–483. https://doi.org/10.2341/19-088-C
Cruz J, Silva AL, Eira R, Coito C, Lopes M, Cavalheiro A (2021) 24-Month clinical performance of a universal adhesive on non-carious cervical lesions: self-etch and etch-and-rinse techniques. J Adhes Dent 23:379–387. https://doi.org/10.3290/j.jad.b2000173
Daudt E, Lopes GC, Vieira LC (2013) Does operatory field isolation influence the performance of direct adhesive restorations? J Adhes Dent 15:27–32. https://doi.org/10.3290/j.jad.a28194
Dutra-Correa M, Saraceni CH, Ciaramicoli MT, Kiyan VH, Queiroz CS (2013) Effect of chlorhexidine on the 18-month clinical performance of two adhesives. J Adhes Dent 15:287–292. https://doi.org/10.3290/j.jad.a29533
Hass V, Matos TP, Parreiras SO, Szesz AL, de Souza JJ, Gutiérrez MF, Reis A, Loguercio AD (2022) An 18-month clinical evaluation of prolonged polymerization of a universal adhesive in non-carious cervical lesions: a double-blind randomized clinical trial. Dent Mater 38:68–78. https://doi.org/10.1016/j.dental.2021.10.012
Lawson NC, Robles A, Fu CC, Lin CP, Sawlani K, Burgess JO (2015) Two-year clinical trial of a universal adhesive in total-etch and self-etch mode in non-carious cervical lesions. J Dent 43:1229–1234. https://doi.org/10.1016/j.jdent.2015.07.009
Loguercio AD, Luque-Martinez IV, Fuentes S, Reis A, Muñoz MA (2018) Effect of dentin roughness on the adhesive performance in non-carious cervical lesions: a double-blind randomized clinical trial. J Dent 69:60–69. https://doi.org/10.1016/j.jdent.2017.09.011
Mushtaq U, Mushtaq F, Thakur D, Rathee K, Poonia N, Khullar S (2021) Comparative evaluation of postoperative sensitivity following restoration of class I lesions with different restorative materials: an in vivo study. J Contemp Dent Pract 22:650–654
Oz FD, Ergin E, Canatan S (2019) Twenty-four-month clinical performance of different universal adhesives in etch-and-rinse, selective etching and self-etch application modes in NCCL - a randomized controlled clinical trial. J Appl Oral Sci 27:e20180358. https://doi.org/10.1590/1678-7757-2018-0358
Perdigão J, Dutra-Corrêa M, Anauate-Netto C, Castilhos N, Carmo AR, Lewgoy HR, Amore R, Cordeiro HJ (2009) Two-year clinical evaluation of self-etching adhesives in posterior restorations. J Adhes Dent 11:149–159
Perdigão J (1939) Geraldeli S and Hodges JS (2003) Total-etch versus self-etch adhesive: effect on postoperative sensitivity. J Am Dent Assoc 134:1621–1629. https://doi.org/10.14219/jada.archive.2003.0109
Peumans M, Vandormael S, Heeren A, De Munck J, Van Meerbeek B (2021) Six-year clinical performance of a 2-step self-etch adhesive in noncarious cervical lesions. J Adhes Dent 23:201–215. https://doi.org/10.3290/j.jad.b1367831
Peumans M, Wouters L, De Munck J, Van Meerbeek B, Van Landuyt K (2018) Nine-year clinical performance of a HEMA-free one-step self-etch adhesive in noncarious cervical lesions. J Adhes Dent 20:195–203. https://doi.org/10.3290/j.jad.a40630
Barceleiro MO, Lopes LS, Tardem C, Calazans FS, Matos TP, Reis A, Calixto AL, Loguercio AD (2022) Thirty-six-month follow-up of cervical composite restorations placed with an MDP-free universal adhesive system using different adhesive protocols: a randomized clinical trial. Clin Oral Investig 26:4337–4350. https://doi.org/10.1007/s00784-022-04397-x
de Albuquerque EG, Warol F, Tardem C, Calazans FS, Poubel LA, Matos TP, Souza JJ, Reis A, Barceleiro MO, Loguercio AD (2022) Universal simplified adhesive applied under different bonding technique’s: 36-month randomized multicentre clinical trial. J Dent 122:104120. https://doi.org/10.1016/j.jdent.2022.104120
Yazici AR, Uslu Tekce A, Kutuk ZB (2022) Comparative evaluation of different adhesive strategies of a universal adhesive in class II bulk-fill restorations: a 48-month randomized controlled trial. J Dent 117:103921. https://doi.org/10.1016/j.jdent.2021.103921
Sancakli HS, Yildiz E, Bayrak I, Ozel S (2019) Effect of different adhesive strategies on the post-operative sensitivity of class I composite restorations. Eur J Dent 8:15–22. https://doi.org/10.4103/1305-7456.126234
Swift EJ, Ritter AV, Heymann HO, Sturdevant JR, Wilder AD (2008) 36-Month clinical evaluation of two adhesives and microhybrid resin composites in class I restorations. Am J Dent 21:148–152
de Oliveira ILM, Hanzen TA, de Paula AM, Perdigão J, Montes M, Loguercio AD, Monteiro GQM (2022) Postoperative sensitivity in posterior resin composite restorations with prior application of a glutaraldehyde-based desensitizing solution: a randomized clinical trial. J Dent 117:103918. https://doi.org/10.1016/j.jdent.2021.103918
Soares AD, Ramos JC, Alves LC, Pereira JL, Caramelo F, Costa AL (2022) Evaluation of the efficacy of a 2-step etch-and-rinse, 2-step self-etch and 1-step self-etch adhesive systems, in class II primary molars restorations. An one year prospective, randomized clinical trial. Eur Arch Paediatr Dent 23(5):845–854. https://doi.org/10.1007/s40368-022-00748-0
Türkün SL (2003) Clinical evaluation of a self-etching and a one-bottle adhesive system at two years. J Dent 31:527–534. https://doi.org/10.1016/S0300-5712(03)00107-6
Merle CL, Fortenbacher M, Schneider H, Schmalz G, Challakh N, Park KJ, Häfer M, Ziebolz D, Haak R (2022) Clinical and OCT assessment of application modes of a universal adhesive in a 12-month RCT. J Dent 119:104068. https://doi.org/10.1016/j.jdent.2022.104068
Rathore M, Singh A, Pant VA (2012) The dental amalgam toxicity fear: a myth or actuality. Toxicol Int 19:81–88. https://doi.org/10.4103/0971-6580.97191
al-Shraideh M, al-Wahadni A, Khasawneh S, al-Shraideh MJ (2002) The mercury burden in waste water released from dental clinics. SADJ 57:213–215
Strober B, Veitz-Keenan A, Barna JA, Matthews AG, Vena D, Craig RG, Curro FA, Thompson VP (2013) Effectiveness of a resin-modified glass ionomer liner in reducing hypersensitivity in posterior restorations: a study from the practitioners engaged in applied research and learning network. J Am Dent Assoc 144:886–897. https://doi.org/10.14219/jada.archive.2013.0206
Briso AL, Mestrener SR, Delício G, Sundfeld RH, Bedran-Russo AK, de Alexandre RS, Ambrosano GM (2007) Clinical assessment of postoperative sensitivity in posterior composite restorations. Oper Dent 32:421–426. https://doi.org/10.2341/06-141
Wilson NH, Wilson MA, offtell DG and Smith GA (1991) Performance of occlusin in butt-joint and bevel-edged preparations: five-year results. 4. Dent Mater 7 92-98. https://doi.org/10.1016/0109-5641(91)90052-z
Ibarra G, Johnson GH, Geurtsen W, Vargas MA (2007) Microleakage of porcelain veneer restorations bonded to enamel and dentin with a new self-adhesive resin-based dental cement. Dent Mater 23:218–225. https://doi.org/10.1016/j.dental.2006.01.013
Unemori M, Matsuya Y, Hyakutake H, Matsuya S, Goto Y, Akamine A (2007) Long-term follow-up of composite resin restorations with self-etching adhesives. J Dent 35:535–540. https://doi.org/10.1016/j.jdent.2007.02.005
Nash RW, Lowe RA, Leinfelder K (2001) Using packable composites for direct posterior placement. J Am Dent Assoc 132:1099–1104. https://doi.org/10.14219/jada.archive.2001.0334
Availability of data and materials
The original contributions presented in the study are included in the article/supplementary material; further inquiries can be directed to the corresponding author.
Funding
This work was supported by the Project of NINGBO Leading Medical & Health Discipline, Project Number: 2022-F20.
Author information
Authors and Affiliations
Contributions
Conceptualization: Keda Fang; methodology: Kenan Chen; formal analysis and investigation: Mengqi Shi; writing original draft preparation: Mengqi Shi, Liang Wang; writing review and editing: Keda Fang, Kenan Chen; funding acquisition: Keda Fang; resources: Kenan Chen, Liang Wang; supervision: Keda Fang; and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(DOCX 18 kb)

Supplementary Figure 1
Forest plots of the performed meta-analysis, meta-analysis for using the USPHS criteria to measure surface texture of self-etching vs. total-etching systems in (a) Class I/II and (b) Class V composite resin restorations. Study, pooled effect estimates for different outcomes, 95% confidence intervals (95% CI) and relative weight (%) from random- and fixed-effect meta-analysis are presented. Heterogeneity was assessed by I2-statistic and p value. SMD, standardized; RR, relative risk (PNG 70 kb)

Supplementary Figure 1b
(PNG 94 kb)

Supplementary Figure 2
Forest plots of the performed meta-analysis, meta-analysis for using the USPHS criteria to measure marginal integrity of self-etching vs. total-etching systems in Class I/II composite resin restorations. Study, pooled effect estimates for different outcomes, 95% confidence intervals (95% CI) and relative weight (%) from random- and fixed-effect meta-analysis are presented. Heterogeneity was assessed by I2-statistic and p value. SMD, standardized; RR, relative risk (PNG 117 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fang, K., Chen, K., Shi, M. et al. Effect of different adhesive systems on dental defects and sensitivity to teeth in composite resin restoration: a systematic review and meta-analysis. Clin Oral Invest 27, 2495–2511 (2023). https://doi.org/10.1007/s00784-023-05007-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-023-05007-0