Abstract
Objectives
This study aimed to evaluate the soft tissue prediction accuracy of patients undergoing orthognathic surgery to correct skeletal class III malocclusion using maxillofacial regional aesthetic units.
Materials and methods
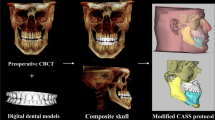
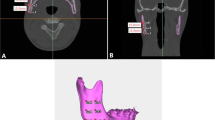
Pre- and postoperative cone-beam computed tomography (CBCT) and 3D facial scans were taken for 58 patients who had undergone orthognathic surgery. The preoperative 3D facial scan was integrated with the preoperative CBCT using ProPlan CMF software. The software simulated the surgery and generated postoperative soft tissue prediction. The simulated 3D facial scan was then compared with the actual 3D facial scan obtained at least 6 months after the surgery by the maxillofacial regional aesthetic units and the facial soft tissue landmark points.
Results
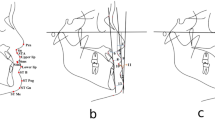
The anatomical regions of the upper lip, lower lip, chin, right external buccal and left external buccal prediction were above 2.0 mm. As for the soft tissue landmarks, at chl, chr, ls, stm and li, the position of predicted scan was higher than that of the actual postoperative scan.
Conclusions
The accuracy of 3D soft tissue predictions using ProPlan CMF software in Skeletal III patients was clinically satisfactory according to maxillofacial regional aesthetic units combined with facial soft tissue landmark points. However, the accuracy of prediction still needed improvement in some areas.
Clinical relevance
The accuracy of soft tissue prediction can be analyzed more clearly through maxillofacial regional aesthetic units so that clinicians have a deeper understanding of the use of the software to predict soft tissue change after orthognathic surgery.





Similar content being viewed by others
References
Lee KJC, Tan SL, Low HYA et al (2021) Accuracy of 3-dimensional soft tissue prediction for orthognathic surgery in a Chinese population. J Stomatol Oral Maxillofac Surg. https://doi.org/10.1016/j.jormas.2021.08.001
Gossett CB, Preston CB, Dunford R, Lampasso J et al (2005) Prediction accuracy of computer-assisted surgical visual treatment objectives as compared with conventional visual treatment objectives. J Oral Maxillofac Surg 63(5):609–17. https://doi.org/10.1016/j.joms.2005.01.004
Eckhardt CE, Cunningham SJ (2004) How predictable is orthognathic surgery? Eur J Orthod 26(3):303–9. https://doi.org/10.1093/ejo/26.3.303
San Miguel Moragas J, Van Cauteren W, Mommaerts MY (2014) A systematic review on soft-to-hard tissue ratios in orthognathic surgery part I: maxillary repositioning osteotomy. J Craniomaxillofac Surg 42(7):1341–51. https://doi.org/10.1016/j.jcms.2014.03.024
Dvortsin DP, Sandham A, Pruim GJ, Dijkstra PU et al (2008) A comparison of the reproducibility of manual tracing and on-screen digitization for cephalometric profile variables. Eur J Orthod 30(6):586–91. https://doi.org/10.1093/ejo/cjn041
Xia JJ, Shevchenko L, Gateno J, Teichgraeber JF et al (2011) Outcome study of computer-aided surgical simulation in the treatment of patients with craniomaxillofacial deformities. J Oral Maxillofac Surg 69(7):2014–24. https://doi.org/10.1016/j.joms.2011.02.018
Mazzoni S, Bianchi A, Schiariti G et al (2015) Computer-aided design and computer-aided manufacturing cutting guides and customized titanium plates are useful in upper maxilla waferless repositioning. J Oral Maxillofac Surg 73(4):701–7. https://doi.org/10.1016/j.joms.2014.10.028
Aboul-Hosn Centenero S, Hernández-Alfaro F (2012) 3D planning in orthognathic surgery: CAD/CAM surgical splints and prediction of the soft and hard tissues results - our experience in 16 cases. J Craniomaxillofac Surg 40(2):162–8. https://doi.org/10.1016/j.jcms.2011.03.014
Bruce V (2012) Applied research in face processing. Applied Research in Face Processing Oxford Handbooks. https://doi.org/10.1093/oxfordhb/9780199559053.013.0008
Knoops PGM, Borghi A, Breakey RWF et al (2019) Three-dimensional soft tissue prediction in orthognathic surgery: a clinical comparison of Dolphin, ProPlan CMF, and probabilistic finite element modelling. Int J Oral Maxillofac Surg 48:511–518. https://doi.org/10.1016/j.ijom.2018.10.008
Gonzalez-Ulloa M (1956) Restoration of the face covering by means of selected skin in regional aesthetic units. Br J Plast Surg 9(3):212–21. https://doi.org/10.1016/s0007-1226(56)80036-2
Fattahi TT (2003) An overview of facial aesthetic units. J Oral Maxillofac Surg 61:1207–1211. https://doi.org/10.1016/s0278-2391(03)00684-0
Kaipatur NR, Flores-Mir C (2009) Accuracy of computer programs in predicting orthognathic surgery soft tissue response. J Oral Maxillofac Surg 67(4):751–9. https://doi.org/10.1016/j.joms.2008.11.006
Kim BR, Oh KM, Cevidanes LHS, Park J-E et al (2013) Analysis of 3D soft tissue changes after 1- and 2-jaw orthognathic surgery in mandibular prognathism patients. J Oral Maxillofac Surg 71(1):151–61. https://doi.org/10.1016/j.joms.2012.02.005
Hwang HS, Yuan D, Jeong K-H, Uhm G-S et al (2012) Three-dimensional soft tissue analysis for the evaluation of facial asymmetry in normal occlusion individuals. Korean J Orthod 42(2):56–63. https://doi.org/10.4041/kjod.2012.42.2.56
Baysal A, Sahan AO, Ozturk MA et al (2016) Reproducibility and reliability of three-dimensional soft tissue landmark identification using three-dimensional stereophotogrammetry. Angle Orthod 86:1004–1009. https://doi.org/10.2319/120715-833.1
Plooij JM, Swennen GR, Rangel FA et al (2009) Evaluation of reproducibility and reliability of 3D soft tissue analysis using 3D stereophotogrammetry. Int J Oral Maxillofac Surg 38:267–273. https://doi.org/10.1016/j.ijom.2008.12.009
Badiali G, Roncari A, Bianchi A et al (2015) Navigation in orthognathic surgery: 3D accuracy. Facial Plast Surg 31(5):463–73. https://doi.org/10.1055/s-0035-1564716
Baan F, Liebregts J, Xi T et al (2016) A new 3D tool for assessing the accuracy of bimaxillary surgery: the OrthoGnathicAnalyser. PLoS One 11(2):e0149625. https://doi.org/10.1371/journal.pone.0149625
Khambay B, Ullah R (2015) Current methods of assessing the accuracy of three-dimensional soft tissue facial predictions: technical and clinical considerations. Int J Oral Maxillofac Surg 44:132–138. https://doi.org/10.1016/j.ijom.2014.04.007
Mundluru T, Almukhtar A, Ju X et al (2017) The accuracy of three-dimensional prediction of soft tissue changes following the surgical correction of facial asymmetry: an innovative concept. Int J Oral Maxillofac Surg 46:1517–1524. https://doi.org/10.1016/j.ijom.2017.04.017
Holzinger D, Juergens P, Shahim K et al (2018) Accuracy of soft tissue prediction in surgery-first treatment concept in orthognathic surgery: a prospective study. J Craniomaxillofac Surg 46:1455–1460. https://doi.org/10.1016/j.jcms.2018.05.055
Liebregts JH, Timmermans M, De Koning MJ et al (2015) Three-dimensional facial simulation in bilateral sagittal split osteotomy: a validation study of 100 patients. J Oral Maxillofac Surg 73:961–970. https://doi.org/10.1016/j.joms.2014.11.006
Liebregts J, Xi T, Timmermans M et al (2015) Accuracy of three-dimensional soft tissue simulation in bimaxillary osteotomies. J Craniomaxillofac Surg 43:329–335. https://doi.org/10.1016/j.jcms.2014.12.012
Shafi MI, Ayoub A, Ju X et al (2013) The accuracy of three-dimensional prediction planning for the surgical correction of facial deformities using Maxilim. Int J Oral Maxillofac Surg 42:801–806. https://doi.org/10.1016/j.ijom.2013.01.015
Ullah R, Turner PJ, Khambay BS (2015) Accuracy of three-dimensional soft tissue predictions in orthognathic surgery after Le Fort I advancement osteotomies. Br J Oral Maxillofac Surg 53:153–157. https://doi.org/10.1016/j.bjoms.2014.11.001
González-Ulloa M (1987) Regional aesthetic units of the face. Plast Reconstr Surg 26(1S):S4–S9. https://doi.org/10.1097/00006534-198703000-00044
Thompson S, Menick FJ (1994) Aesthetic facial reconstruction: blending human perception and the facial subunit theory. Plast Surg Nurs 14(4):211–216. https://doi.org/10.1097/00006527-199401440-00004 (224)
Mohlhenrich SC, Heussen N, Kamal M et al (2015) Influence of setback and advancement osseous genioplasty on facial outcome: a computer-simulated study. J Craniomaxillofac Surg 43:2017–2025. https://doi.org/10.1016/j.jcms.2015.10.017
Ying X, Tian K, Zhang K et al (2021) Accuracy of virtual surgical planning in segmental osteotomy in combination with bimaxillary orthognathic surgery with surgery first approach. BMC Oral Health 21:529. https://doi.org/10.1186/s12903-021-01892-7
Olivetti EC, Nicotera S, Marcolin F et al (2019) 3D soft-tissue prediction methodologies for orthognathic surgery—a literature review. Appl Sci 9. https://doi.org/10.3390/app9214550
Kim D, Ho DC, Mai H et al (2017) A clinically validated prediction method for facial soft-tissue changes following double-jaw surgery. Med Phys 44:4252–4261. https://doi.org/10.1002/mp.12391
Kim D, Kuang T, Rodrigues YL et al (2019) A new approach of predicting facial changes following orthognathic surgery using realistic lip sliding effect. Med Image Comput Comput Assist Interv 11768:336–344. https://doi.org/10.1007/978-3-030-32254-0_38
Lim YK, Chu EH, Lee DY et al (2010) Three-dimensional evaluation of soft tissue change gradients after mandibular setback surgery in skeletal Class III malocclusion. Angle Orthod 80:896–903. https://doi.org/10.2319/021210-90.1
Acknowledgements
The authors offer many thanks to Dr Yang Li and Dr Wei He for permitting access to some of the patients and their records included in this study.
Funding
This study was supported by National Key Research and Development Program of China (2019YFF0302401) and the Beijing Municipal Science & Technology Commission (Z181100001718130, No. 2016–1-4103).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Lei Hou. The first draft of the manuscript was written by Lei Hou, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All the procedure was approved by the Ethics Committee of Peking University School and Hospital of Stomatology (protocol no. PKUSSIRB-202059180) and was conducted in accordance with the relevant guidelines and regulations.
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hou, L., He, Y., Yi, B. et al. Evaluation of soft tissue prediction accuracy for orthognathic surgery with skeletal class III malocclusion using maxillofacial regional aesthetic units. Clin Oral Invest 27, 173–182 (2023). https://doi.org/10.1007/s00784-022-04705-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-022-04705-5