Abstract
Objectives
This systematic review and network meta-analysis aimed to answer to the following questions: (a) In patients undergoing alveolar ridge preservation after tooth extraction, which grafting material best attenuates horizontal and vertical ridge resorption, as compared to spontaneous healing?, and (b) which material(s) promotes bone formation in the extraction socket?
Materials and methods
The MEDLINE, SCOPUS, CENTRAL, and EMBASE databases were screened in duplicate for RCTs up to March 2021. Two independent authors extracted the data and assessed the risk of bias of the included studies. Primary outcomes were ridge horizontal and vertical dimension changes and new bone formation into the socket. Both pairwise and network meta-analysis (NMA) were undertaken to obtain estimates for primary outcomes and compare different grafting materials.
Results
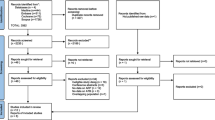
Eighty-eight RCTs were included, with a total of 2805 patients and 3073 sockets. Overall, a total of 1740 sockets underwent alveolar ridge preservation with different materials (1432 were covered by a membrane). Pairwise meta-analysis showed that, as compared to spontaneous healing, all materials statistically significantly reduced horizontal and vertical shrinkage. According to the multidimensional scale ranking of the NMA, xenografts (XG) and allografts (AG), alone or combined with bioactive agents (Bio + AG), were the most predictable materials for horizontal and vertical ridge dimension preservation, while platelet concentrates performed best in the percentage of new bone formation.
Conclusions
Alveolar ridge preservation is effective in reducing both horizontal and vertical shrinkage, as compared to untreated sockets. NMA confirmed the consistency of XG for ridge dimension preservation, but several other materials and combinations like AG, Bio + AG, and AG + alloplasts, produced even better results than XG in clinical comparisons. Further evidence is needed to confirm the value of such alternatives to XG for alveolar ridge preservation. Bio + AG performed better than the other materials in preserving ridge dimension and platelet concentrates in new bone formation. However, alloplasts, xenografts, and AG + AP performed consistently good in majority of the clinical comparisons.
Clinical relevance
XG and Bio + AG demonstrated significantly better performance in minimizing post-extraction horizontal and vertical ridge dimension changes as compared with other grafting materials or with spontaneous healing, even if they presented the worst histological outcomes. Allografts and other materials or combinations (AG + AP) presented similar performances while spontaneous healing ranked last.








Similar content being viewed by others
References
Kassebaum NJ, Smith AGC, Bernabe E, Fleming TD, Reynolds AE, Vos T, Murray CJL, Marcenes W, Collaborators GBDOH (2017) Global, regional, and national prevalence, incidence, and disability-adjusted life years for oral conditions for 195 countries, 1990-2015: a systematic analysis for the global burden of diseases, injuries, and risk factors. J Dent Res 96(4):380–387. https://doi.org/10.1177/0022034517693566
Giannobile WV, Lang NP (2016) Are dental implants a Panacea or should we better strive to save teeth? J Dent Res 95(1):5–6. https://doi.org/10.1177/0022034515618942
Avila-Ortiz G, Chambrone L, Vignoletti F (2019) Effect of alveolar ridge preservation interventions following tooth extraction: a systematic review and meta-analysis. J Clin Periodontol 46(Suppl 21):195–223. https://doi.org/10.1111/jcpe.13057
Avila-Ortiz G, Elangovan S, Kramer KW, Blanchette D, Dawson DV (2014) Effect of alveolar ridge preservation after tooth extraction: a systematic review and meta-analysis. J Dent Res 93(10):950–958. https://doi.org/10.1177/0022034514541127
Cardaropoli G, Araujo M, Hayacibara R, Sukekava F, Lindhe J (2005) Healing of extraction sockets and surgically produced - augmented and non-augmented - defects in the alveolar ridge. An experimental study in the dog. J Clin Periodontol 32(5):435–440. https://doi.org/10.1111/j.1600-051X.2005.00692.x
Cardaropoli G, Araujo M, Lindhe J (2003) Dynamics of bone tissue formation in tooth extraction sites. An experimental study in dogs. J Clin Periodontol 30(9):809–818. https://doi.org/10.1034/j.1600-051x.2003.00366.x
Tan WL, Wong TL, Wong MC, Lang NP (2012) A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res 23(Suppl 5):1–21. https://doi.org/10.1111/j.1600-0501.2011.02375.x
Van der Weijden F, Dell’Acqua F, Slot DE (2009) Alveolar bone dimensional changes of post-extraction sockets in humans: a systematic review. J Clin Periodontol 36(12):1048–1058. https://doi.org/10.1111/j.1600-051X.2009.01482.x
Araujo MG, Lindhe J (2005) Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol 32(2):212–218. https://doi.org/10.1111/j.1600-051X.2005.00642.x
Huynh-Ba G, Pjetursson BE, Sanz M, Cecchinato D, Ferrus J, Lindhe J, Lang NP (2010) Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement. Clin Oral Implants Res 21(1):37–42. https://doi.org/10.1111/j.1600-0501.2009.01870.x
Schropp L, Wenzel A, Kostopoulos L, Karring T (2003) Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent 23(4):313–323
Sculean A, Stavropoulos A, Bosshardt DD (2019) Self-regenerative capacity of intra-oral bone defects. J Clin Periodontol 46(Suppl 21):70–81. https://doi.org/10.1111/jcpe.13075
Baumer D, Zuhr O, Rebele S, Hurzeler M (2017) Socket shield technique for immediate implant placement - clinical, radiographic and volumetric data after 5 years. Clin Oral Implants Res 28(11):1450–1458. https://doi.org/10.1111/clr.13012
Hurzeler MB, Zuhr O, Schupbach P, Rebele SF, Emmanouilidis N, Fickl S (2010) The socket-shield technique: a proof-of-principle report. J Clin Periodontol 37(9):855–862. https://doi.org/10.1111/j.1600-051X.2010.01595.x
Salama M, Ishikawa T, Salama H, Funato A, Garber D (2007) Advantages of the root submergence technique for pontic site development in esthetic implant therapy. Int J Periodontics Restorative Dent 27(6):521–527
Salama H, Salama M (1993) The role of orthodontic extrusive remodeling in the enhancement of soft and hard tissue profiles prior to implant placement: a systematic approach to the management of extraction site defects. Int J Periodontics Restorative Dent 13(4):312–333
Amato F, Mirabella AD, Macca U, Tarnow DP (2012) Implant site development by orthodontic forced extraction: a preliminary study. Int J Oral Maxillofac Implants 27(2):411–420
Joo JY, Son S, Lee JY (2016) Implant site development for enhancing esthetics of soft and hard tissue and simplification of implant surgery using a forced eruption. Int J Periodontics Restorative Dent 36(4):583–589. https://doi.org/10.11607/prd.2291
Tan-Chu JH, Tuminelli FJ, Kurtz KS, Tarnow DP (2014) Analysis of buccolingual dimensional changes of the extraction socket using the “ice cream cone” flapless grafting technique. Int J Periodontics Restorative Dent 34(3):399–403. https://doi.org/10.11607/prd.1605
Atieh MA, Alsabeeha NH, Payne AG, Ali S, Faggion CMJ, Esposito M (2021) Interventions for replacing missing teeth: alveolar ridge preservation techniques for dental implant site development. Cochrane Database Syst Rev 4:CD010176. https://doi.org/10.1002/14651858.CD010176.pub3
Balli G, Ioannou A, Powell CA, Angelov N, Romanos GE, Soldatos N (2018) Ridge preservation procedures after tooth extractions: a systematic review. Int J Dent 2018:8546568. https://doi.org/10.1155/2018/8546568
Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L, Cardaropoli G (2012) Socket preservation using bovine bone mineral and collagen membrane: a randomized controlled clinical trial with histologic analysis. Int J Periodontics Restorative Dent 32(4):421–430
Mardas N, Trullenque-Eriksson A, MacBeth N, Petrie A, Donos N (2015) Does ridge preservation following tooth extraction improve implant treatment outcomes: a systematic review: group 4: therapeutic concepts & methods. Clin Oral Implants Res 26(Suppl 11):180–201. https://doi.org/10.1111/clr.12639
Nart J, Barallat L, Jimenez D, Mestres J, Gomez A, Carrasco MA, Violant D, Ruiz-Magaz V (2017) Radiographic and histological evaluation of deproteinized bovine bone mineral vs. deproteinized bovine bone mineral with 10% collagen in ridge preservation. A randomized controlled clinical trial. Clin Oral Implants Res 28(7):840–848. https://doi.org/10.1111/clr.12889
Araujo MG, Liljenberg B, Lindhe J (2010) Dynamics of Bio-Oss Collagen incorporation in fresh extraction wounds: an experimental study in the dog. Clin Oral Implants Res 21(1):55–64. https://doi.org/10.1111/j.1600-0501.2009.01854.x
Willenbacher M, Al-Nawas B, Berres M, Kammerer PW, Schiegnitz E (2016) The effects of alveolar ridge preservation: a meta-analysis. Clin Implant Dent Relat Res 18(6):1248–1268. https://doi.org/10.1111/cid.12364
Canellas J, Medeiros PJD, Figueredo C, Fischer RG, Ritto FG (2019) Which is the best choice after tooth extraction, immediate implant placement or delayed placement with alveolar ridge preservation? A systematic review and meta-analysis. J Craniomaxillofac Surg 47(11):1793–1802. https://doi.org/10.1016/j.jcms.2019.08.004
Iocca O, Farcomeni A, Pardinas Lopez S, Talib HS (2017) Alveolar ridge preservation after tooth extraction: a Bayesian network meta-analysis of grafting materials efficacy on prevention of bone height and width reduction. J Clin Periodontol 44(1):104–114. https://doi.org/10.1111/jcpe.12633
Stone PW (2002) Popping the (PICO) question in research and evidence-based practice. Appl Nurs Res 15(3):197–198. https://doi.org/10.1053/apnr.2002.34181
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188. https://doi.org/10.1016/0197-2456(86)90046-2
Chaimani A, Higgins JP, Mavridis D, Spyridonos P, Salanti G (2013) Graphical tools for network meta-analysis in STATA. PLoS One 8(10):e76654. https://doi.org/10.1371/journal.pone.0076654
Pang KM, Um IW, Kim YK, Woo JM, Kim SM, Lee JH (2017) Autogenous demineralized dentin matrix from extracted tooth for the augmentation of alveolar bone defect: a prospective randomized clinical trial in comparison with anorganic bovine bone. Clin Oral Implants Res 28(7):809–815. https://doi.org/10.1111/clr.12885
Coomes AM, Mealey BL, Huynh-Ba G, Barboza-Arguello C, Moore WS, Cochran DL (2014) Buccal bone formation after flapless extraction: a randomized, controlled clinical trial comparing recombinant human bone morphogenetic protein 2/absorbable collagen carrier and collagen sponge alone. J Periodontol 85(4):525–535. https://doi.org/10.1902/jop.2013.130207
Sisti A, Canullo L, Mottola MP, Covani U, Barone A, Botticelli D (2012) Clinical evaluation of a ridge augmentation procedure for the severely resorbed alveolar socket: multicenter randomized controlled trial, preliminary results. Clin Oral Implants Res 23(5):526–535. https://doi.org/10.1111/j.1600-0501.2011.02386.x
Ntounis A, Geurs N, Vassilopoulos P, Reddy M (2015) Clinical assessment of bone quality of human extraction sockets after conversion with growth factors. Int J Oral Maxillofac Implants 30(1):196–201. https://doi.org/10.11607/jomi.3518
Crespi R, Cappare P, Gherlone E (2011) Comparison of magnesium-enriched hydroxyapatite and porcine bone in human extraction socket healing: a histologic and histomorphometric evaluation. Int J Oral Maxillofac Implants 26(5):1057–1062
Hauser F, Gaydarov N, Badoud I, Vazquez L, Bernard JP, Ammann P (2013) Clinical and histological evaluation of postextraction platelet-rich fibrin socket filling: a prospective randomized controlled study. Implant Dent 22(3):295–303. https://doi.org/10.1097/ID.0b013e3182906eb3
Jo DW, Cho YD, Seol YJ, Lee YM, Lee HJ, Kim YK (2019) A randomized controlled clinical trial evaluating efficacy and adverse events of different types of recombinant human bone morphogenetic protein-2 delivery systems for alveolar ridge preservation. Clin Oral Implants Res 30(5):396–409. https://doi.org/10.1111/clr.13423
Cha JK, Song YW, Park SH, Jung RE, Jung UW, Thoma DS (2019) Alveolar ridge preservation in the posterior maxilla reduces vertical dimensional change: a randomized controlled clinical trial. Clin Oral Implants Res 30(6):515–523. https://doi.org/10.1111/clr.13436
Clementini M, Agostinelli A, Castelluzzo W, Cugnata F, Vignoletti F, De Sanctis M (2019) The effect of immediate implant placement on alveolar ridge preservation compared to spontaneous healing after tooth extraction: radiographic results of a randomized controlled clinical trial. J Clin Periodontol 46(7):776–786. https://doi.org/10.1111/jcpe.13125
Clark D, Rajendran Y, Paydar S, Ho S, Cox D, Ryder M, Dollard J, Kao RT (2018) Advanced platelet-rich fibrin and freeze-dried bone allograft for ridge preservation: a randomized controlled clinical trial. J Periodontol 89(4):379–387. https://doi.org/10.1002/JPER.17-0466
Iorio-Siciliano V, Ramaglia L, Blasi A, Bucci P, Nuzzolo P, Riccitiello F, Nicolo M (2020) Dimensional changes following alveolar ridge preservation in the posterior area using bovine-derived xenografts and collagen membrane compared to spontaneous healing: a 6-month randomized controlled clinical trial. Clin Oral Investig 24(2):1013–1023. https://doi.org/10.1007/s00784-019-02979-w
Jung RE, Ioannidis A, Hammerle CHF (2000) Thoma DS (2018) Alveolar ridge preservation in the esthetic zone. Periodontol 77(1):165–175. https://doi.org/10.1111/prd.12209
Kollati P, Koneru S, Dwarakanath CD, Gottumukkala S (2019) Effectiveness of naturally derived bovine hydroxyapatite (Cerabone) combined with platelet-rich fibrin matrix in socket preservation: a randomized controlled clinical trial. J Indian Soc Periodontol 23(2):145–151. https://doi.org/10.4103/jisp.jisp_400_18
Machtei EE, Mayer Y, Horwitz J, Zigdon-Giladi H (2019) Prospective randomized controlled clinical trial to compare hard tissue changes following socket preservation using alloplasts, xenografts vs no grafting: clinical and histological findings. Clin Implant Dent Relat Res 21(1):14–20. https://doi.org/10.1111/cid.12707
Nunes FAS, Pignaton TB, Novaes AB Jr, Taba M Jr, Messora MR, Palioto DB, Spin-Neto R, de Souza SLS (2018) Evaluation of a bone substitute covered with a collagen membrane for ridge preservation after tooth extraction. Clinical and tomographic randomized controlled study in humans. Clin Oral Implants Res 29(4):424–433. https://doi.org/10.1111/clr.13140
Santana R, Gyurko R, Kanasi E, Xu WP, Dibart S (2019) Synthetic polymeric barrier membrane associated with blood coagulum, human allograft, or bovine bone substitute for ridge preservation: a randomized, controlled, clinical and histological trial. Int J Oral Maxillofac Surg 48(5):675–683. https://doi.org/10.1016/j.ijom.2018.02.012
Sun DJ, Lim HC, Lee DW (2019) Alveolar ridge preservation using an open membrane approach for sockets with bone deficiency: a randomized controlled clinical trial. Clin Implant Dent Relat Res 21(1):175–182. https://doi.org/10.1111/cid.12668
Lim HC, Shin HS, Cho IW, Koo KT, Park JC (2019) Ridge preservation in molar extraction sites with an open-healing approach: a randomized controlled clinical trial. J Clin Periodontol 46(11):1144–1154. https://doi.org/10.1111/jcpe.13184
Girish Kumar N, Chaudhary R, Kumar I, Arora SS, Kumar N, Singh H (2018) To assess the efficacy of socket plug technique using platelet rich fibrin with or without the use of bone substitute in alveolar ridge preservation: a prospective randomised controlled study. Oral Maxillofac Surg 22(2):135–142. https://doi.org/10.1007/s10006-018-0680-3
Aimetti M, Romano F, Griga FB, Godio L (2009) Clinical and histologic healing of human extraction sockets filled with calcium sulfate. Int J Oral Maxillofac Implants 24(5):902–909
Alzahrani AA, Murriky A, Shafik S (2017) Influence of platelet rich fibrin on post-extraction socket healing: a clinical and radiographic study. Saudi Dent J 29(4):149–155. https://doi.org/10.1016/j.sdentj.2017.07.003
Andrade Munhoz E, Bodanezi A, Ferreira Junior O, Mauro Granjeiro J (2011) Bone crestal height and bone density after third-molar extraction and grafting: a long-term follow-up study. Clin Oral Investig 15(1):123–126. https://doi.org/10.1007/s00784-010-0412-z
Araujo MG, da Silva JCC, de Mendonca AF, Lindhe J (2015) Ridge alterations following grafting of fresh extraction sockets in man. A randomized clinical trial. Clin Oral Implants Res 26(4):407–412. https://doi.org/10.1111/clr.12366
Avila-Ortiz G, Rodriguez JC, Rudek I, Benavides E, Rios H, Wang HL (2014) Effectiveness of three different alveolar ridge preservation techniques: a pilot randomized controlled trial. Int J Periodontics Restorative Dent 34(4):509–521. https://doi.org/10.11607/prd.1838
Barone A, Aldini NN, Fini M, Giardino R, Calvo Guirado JL, Covani U (2008) Xenograft versus extraction alone for ridge preservation after tooth removal: a clinical and histomorphometric study. J Periodontol 79(8):1370–1377. https://doi.org/10.1902/jop.2008.070628
Barone A, Ricci M, Tonelli P, Santini S, Covani U (2013) Tissue changes of extraction sockets in humans: a comparison of spontaneous healing vs. ridge preservation with secondary soft tissue healing. Clin Oral Implants Res 24(11):1231–1237. https://doi.org/10.1111/j.1600-0501.2012.02535.x
Barone A, Toti P, Quaranta A, Alfonsi F, Cucchi A, Negri B, Di Felice R, Marchionni S, Calvo-Guirado JL, Covani U, Nannmark U (2017) Clinical and histological changes after ridge preservation with two xenografts: preliminary results from a multicentre randomized controlled clinical trial. J Clin Periodontol 44(2):204–214. https://doi.org/10.1111/jcpe.12655
Brownfield LA, Weltman RL (2012) Ridge preservation with or without an osteoinductive allograft: a clinical, radiographic, micro-computed tomography, and histologic study evaluating dimensional changes and new bone formation of the alveolar ridge. J Periodontol 83(5):581–589. https://doi.org/10.1902/jop.2011.110365
Camargo PM, Lekovic V, Weinlaender M, Klokkevold PR, Kenney EB, Dimitrijevic B, Nedic M, Jancovic S, Orsini M (2000) Influence of bioactive glass on changes in alveolar process dimensions after exodontia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90(5):581–586. https://doi.org/10.1067/moe.2000.110035
Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L (2014) Relationship between the buccal bone plate thickness and the healing of postextraction sockets with/without ridge preservation. Int J Periodontics Restorative Dent 34(2):211–217. https://doi.org/10.11607/prd.1885
Cavdar FH, Keceli HG, Hatipoglu H, Demiralp B, Caglayan F (2017) Evaluation of extraction site dimensions and density using computed tomography treated with different graft materials: a preliminary study. Implant Dent 26(2):270–274. https://doi.org/10.1097/ID.0000000000000567
Crespi R, Cappare P, Gherlone E (2009) Magnesium-enriched hydroxyapatite compared to calcium sulfate in the healing of human extraction sockets: radiographic and histomorphometric evaluation at 3 months. J Periodontol 80(2):210–218. https://doi.org/10.1902/jop.2009.080400
Das S, Jhingran R, Bains VK, Madan R, Srivastava R, Rizvi I (2016) Socket preservation by beta-tri-calcium phosphate with collagen compared to platelet-rich fibrin: a clinico-radiographic study. Eur J Dent 10(2):264–276. https://doi.org/10.4103/1305-7456.178298
Feng L, Zhang L, Cui Y, Song TX, Qiu ZY, Wang XM, Tan BS (2016) Clinical evaluations of mineralized collagen in the extraction sites preservation. Regen Biomater 3(1):41–48. https://doi.org/10.1093/rb/rbv027
Fernandes PG, Muglia VA, Reino DM, Maia LP, de Moraes Grisi MF, de Souza SL, Taba M Jr, Palioto DB, de Almeida AG, Novaes AB Jr (2016) Socket preservation therapy with acellular dermal matrix and mineralized bone allograft after tooth extraction in humans: a clinical and histomorphometric study. Int J Periodontics Restorative Dent 36(2):e16–e25. https://doi.org/10.11607/prd.2307
Fernandes PG, Novaes AB Jr, de Queiroz AC, de Souza SL, Taba M Jr, Palioto DB, Grisi MF (2011) Ridge preservation with acellular dermal matrix and anorganic bone matrix cell-binding peptide P-15 after tooth extraction in humans. J Periodontol 82(1):72–79. https://doi.org/10.1902/jop.2010.100241
Festa VM, Addabbo F, Laino L, Femiano F, Rullo R (2013) Porcine-derived xenograft combined with a soft cortical membrane versus extraction alone for implant site development: a clinical study in humans. Clin Implant Dent Relat Res 15(5):707–713. https://doi.org/10.1111/j.1708-8208.2011.00398.x
Fickl S, Fischer K, Petersen N, Happe A, Schlee M, Schlagenhauf U, Kebschull M (2017) Dimensional evaluation of different ridge preservation techniques: a randomized clinical study. Int J Periodontics Restorative Dent 37(3):403–410. https://doi.org/10.11607/prd.2629
Fiorellini JP, Howell TH, Cochran D, Malmquist J, Lilly LC, Spagnoli D, Toljanic J, Jones A, Nevins M (2005) Randomized study evaluating recombinant human bone morphogenetic protein-2 for extraction socket augmentation. J Periodontol 76(4):605–613. https://doi.org/10.1902/jop.2005.76.4.605
Gholami GA, Najafi B, Mashhadiabbas F, Goetz W, Najafi S (2012) Clinical, histologic and histomorphometric evaluation of socket preservation using a synthetic nanocrystalline hydroxyapatite in comparison with a bovine xenograft: a randomized clinical trial. Clin Oral Implants Res 23(10):1198–1204. https://doi.org/10.1111/j.1600-0501.2011.02288.x
Goh BT, Teh LY, Tan DB, Zhang Z, Teoh SH (2015) Novel 3D polycaprolactone scaffold for ridge preservation--a pilot randomised controlled clinical trial. Clin Oral Implants Res 26 (3):271-277. doi:https://doi.org/10.1111/clr.12486
Guarnieri R, Stefanelli L, De Angelis F, Mencio F, Pompa G, Di Carlo S (2017) Extraction socket preservation using porcine-derived collagen membrane alone or associated with porcine-derived bone. Clinical results of randomized controlled study. J Oral Maxillofac Res 8(3):e5. https://doi.org/10.5037/jomr.2017.8305
Hoda N, Saifi AM, Giraddi GB (2016) Clinical use of the resorbable bioscaffold poly lactic co-glycolic acid (PLGA) in post-extraction socket for maintaining the alveolar height: a prospective study. J Oral Biol Craniofac Res 6(3):173–178. https://doi.org/10.1016/j.jobcr.2016.03.001
Iasella JM, Greenwell H, Miller RL, Hill M, Drisko C, Bohra AA, Scheetz JP (2003) Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol 74(7):990–999. https://doi.org/10.1902/jop.2003.74.7.990
Iorio-Siciliano V, Blasi A, Nicolo M, Iorio-Siciliano A, Riccitiello F, Ramaglia L (2017) Clinical outcomes of socket preservation using bovine-derived xenograft collagen and collagen membrane post-tooth extraction: a 6-month randomized controlled clinical trial. Int J Periodontics Restorative Dent 37(5):e290–e296. https://doi.org/10.11607/prd.2474
Joshi CP, D’Lima CB, Samat UC, Karde PA, Patil AG, Dani NH (2017) Comparative alveolar ridge preservation using allogenous tooth graft versus free-dried bone allograft: a randomized, controlled, prospective, clinical pilot study. Contemp Clin Dent 8(2):211–217. https://doi.org/10.4103/ccd.ccd_147_17
Joshi CP, Dani NH, Khedkar SU (2016) Alveolar ridge preservation using autogenous tooth graft versus beta-tricalcium phosphate alloplast: A randomized, controlled, prospective, clinical pilot study. J Indian Soc Periodontol 20(4):429–434. https://doi.org/10.4103/0972-124X.188335
Jung RE, Philipp A, Annen BM, Signorelli L, Thoma DS, Hammerle CH, Attin T, Schmidlin P (2013) Radiographic evaluation of different techniques for ridge preservation after tooth extraction: a randomized controlled clinical trial. J Clin Periodontol 40(1):90–98. https://doi.org/10.1111/jcpe.12027
Kim YJ, Lee JY, Kim JE, Park JC, Shin SW, Cho KS (2014) Ridge preservation using demineralized bone matrix gel with recombinant human bone morphogenetic protein-2 after tooth extraction: a randomized controlled clinical trial. J Oral Maxillofac Surg 72(7):1281–1290. https://doi.org/10.1016/j.joms.2014.01.022
Kotsakis GA, Salama M, Chrepa V, Hinrichs JE, Gaillard P (2014) A randomized, blinded, controlled clinical study of particulate anorganic bovine bone mineral and calcium phosphosilicate putty bone substitutes for socket preservation. Int J Oral Maxillofac Implants 29(1):141–151. https://doi.org/10.11607/jomi.3230
Kutkut A, Andreana S, Kim HL, Monaco E Jr (2012) Extraction socket preservation graft before implant placement with calcium sulfate hemihydrate and platelet-rich plasma: a clinical and histomorphometric study in humans. J Periodontol 83(4):401–409. https://doi.org/10.1902/jop.2011.110237
Madan R, Mohan R, Bains VK, Gupta V, Singh GP, Madan M (2014) Analysis of socket preservation using polylactide and polyglycolide (PLA-PGA) sponge: a clinical, radiographic, and histologic study. Int J Periodontics Restorative Dent 34(2):e36–e42. https://doi.org/10.11607/prd.1375
Mardas N, Chadha V, Donos N (2010) Alveolar ridge preservation with guided bone regeneration and a synthetic bone substitute or a bovine-derived xenograft: a randomized, controlled clinical trial. Clin Oral Implants Res 21(7):688–698. https://doi.org/10.1111/j.1600-0501.2010.01918.x
Mayer Y, Zigdon-Giladi H, Machtei EE (2016) Ridge preservation using composite alloplastic materials: a randomized control clinical and histological study in humans. Clin Implant Dent Relat Res 18(6):1163–1170. https://doi.org/10.1111/cid.12415
Neiva RF, Tsao YP, Eber R, Shotwell J, Billy E, Wang HL (2008) Effects of a putty-form hydroxyapatite matrix combined with the synthetic cell-binding peptide P-15 on alveolar ridge preservation. J Periodontol 79(2):291–299. https://doi.org/10.1902/jop.2008.070038
Pang C, Ding Y, Zhou H, Qin R, Hou R, Zhang G, Hu K (2014) Alveolar ridge preservation with deproteinized bovine bone graft and collagen membrane and delayed implants. J Craniofac Surg 25(5):1698–1702. https://doi.org/10.1097/SCS.0000000000000887
Poulias E, Greenwell H, Hill M, Morton D, Vidal R, Shumway B, Peterson TL (2013) Ridge preservation comparing socket allograft alone to socket allograft plus facial overlay xenograft: a clinical and histologic study in humans. J Periodontol 84(11):1567–1575. https://doi.org/10.1902/jop.2013.120585
Sadeghi R, Babaei M, Miremadi SA, Abbas FM (2016) A randomized controlled evaluation of alveolar ridge preservation following tooth extraction using deproteinized bovine bone mineral and demineralized freeze-dried bone allograft. Dent Res J (Isfahan) 13(2):151–159. https://doi.org/10.4103/1735-3327.178202
Scheyer ET, Heard R, Janakievski J, Mandelaris G, Nevins ML, Pickering SR, Richardson CR, Pope B, Toback G, Velasquez D, Nagursky H (2016) A randomized, controlled, multicentre clinical trial of post-extraction alveolar ridge preservation. J Clin Periodontol 43(12):1188–1199. https://doi.org/10.1111/jcpe.12623
Schnutenhaus S, Doering I, Dreyhaupt J, Rudolph H, Luthardt RG (2018) Alveolar ridge preservation with a collagen material: a randomized controlled trial. J Periodontal Implant Sci 48(4):236–250. https://doi.org/10.5051/jpis.2018.48.4.236
Serrano Mendez CA, Lang NP, Caneva M, Ramirez Lemus G, Mora Solano G, Botticelli D (2017) Comparison of allografts and xenografts used for alveolar ridge preservation. A clinical and histomorphometric RCT in humans. Clin Implant Dent Relat Res 19(4):608–615. https://doi.org/10.1111/cid.12490
Shim JY, Lee Y, Lim JH, Jin MU, Lee JM, Suh JY, Kim YG (2018) Comparative evaluation of recombinant human bone morphogenetic protein-2/hydroxyapatite and bovine bone for new bone formation in alveolar ridge preservation. Implant Dent 27(6):623–629. https://doi.org/10.1097/ID.0000000000000814
Spinato S, Galindo-Moreno P, Zaffe D, Bernardello F, Soardi CM (2014) Is socket healing conditioned by buccal plate thickness? A clinical and histologic study 4 months after mineralized human bone allografting. Clin Oral Implants Res 25(2):e120–e126. https://doi.org/10.1111/clr.12073
Suttapreyasri S, Leepong N (2013) Influence of platelet-rich fibrin on alveolar ridge preservation. J Craniofac Surg 24(4):1088–1094. https://doi.org/10.1097/SCS.0b013e31828b6dc3
Temmerman A, Vandessel J, Castro A, Jacobs R, Teughels W, Pinto N, Quirynen M (2016) The use of leucocyte and platelet-rich fibrin in socket management and ridge preservation: a split-mouth, randomized, controlled clinical trial. J Clin Periodontol 43(11):990–999. https://doi.org/10.1111/jcpe.12612
Thakkar DJ, Deshpande NC, Dave DH, Narayankar SD (2016) A comparative evaluation of extraction socket preservation with demineralized freeze-dried bone allograft alone and along with platelet-rich fibrin: A clinical and radiographic study. Contemp Clin Dent 7(3):371–376. https://doi.org/10.4103/0976-237X.188567
Toloue SM, Chesnoiu-Matei I, Blanchard SB (2012) A clinical and histomorphometric study of calcium sulfate compared with freeze-dried bone allograft for alveolar ridge preservation. J Periodontol 83(7):847–855. https://doi.org/10.1902/jop.2011.110470
Tomasi C, Donati M, Cecchinato D, Szathvary I, Corra E, Lindhe J (2018) Effect of socket grafting with deproteinized bone mineral: An RCT on dimensional alterations after 6 months. Clin Oral Implants Res 29(5):435–442. https://doi.org/10.1111/clr.13141
Vance GS, Greenwell H, Miller RL, Hill M, Johnston H, Scheetz JP (2004) Comparison of an allograft in an experimental putty carrier and a bovine-derived xenograft used in ridge preservation: a clinical and histologic study in humans. Int J Oral Maxillofac Implants 19(4):491–497
Ahmed N, Gopalakrishna V, Shetty A, Nagraj V, Imran M, Kumar P (2019) Efficacy of PRF vs PRF + biodegradable collagen plug in post-extraction preservation of socket. J Contemp Dent Pract 20(11):1323–1328
Azangookhiavi H, Ghodsi S, Jalil F, Dadpour Y (2020) Comparison of the efficacy of platelet-rich fibrin and bone allograft for alveolar ridge preservation after tooth extraction: a clinical trial. Front Dent 17(1):1–6. https://doi.org/10.18502/fid.v17i1.3961
Ben Amara H, Kim JJ, Kim HY, Lee J, Song HY, Koo KT (2021) Is ridge preservation effective in the extraction sockets of periodontally compromised teeth? A randomized controlled trial. J Clin Periodontol 48(3):464–477. https://doi.org/10.1111/jcpe.13412
Cadenas-Vacas G, Martinez-Rodriguez N, Barona-Dorado C, Sanchez-Labrador L, Cortes-Breton Brinkmann J, Meniz-Garcia C, Martinez-Gonzalez JM (2021) Calcium phosphate modified with silicon vs. bovine hydroxyapatite for alveolar ridge preservation: densitometric evaluation, morphological changes and histomorphometric study. Materials (Basel) 14 (4). doi:https://doi.org/10.3390/ma14040940
Saito H, Couso-Queiruga E, Shiau HJ, Stuhr S, Prasad H, Allareddy TV, Reynolds MA, Avila-Ortiz G (2021) Evaluation of poly lactic-co-glycolic acid-coated beta-tricalcium phosphate for alveolar ridge preservation: A multicenter randomized controlled trial. J Periodontol 92(4):524–535. https://doi.org/10.1002/JPER.20-0360
Stumbras A, Galindo-Moreno P, Januzis G, Juodzbalys G (2021) Three-dimensional analysis of dimensional changes after alveolar ridge preservation with bone substitutes or plasma rich in growth factors: Randomized and controlled clinical trial. Clin Implant Dent Relat Res 23(1):96–106. https://doi.org/10.1111/cid.12950
Collins JR, Jimenez E, Martinez C, Polanco RT, Hirata R, Mousa R, Coelho PG, Bonfante EA, Tovar N (2014) Clinical and histological evaluation of socket grafting using different types of bone substitute in adult patients. Implant Dent 23(4):489–495. https://doi.org/10.1097/ID.0000000000000106
Hassan M, Prakasam S, Bain C, Ghoneima A, Liu SS (2017) A randomized split-mouth clinical trial on effectiveness of amnion-chorion membranes in alveolar ridge preservation: a clinical, radiologic, and morphometric study. Int J Oral Maxillofac Implants 32(6):1389–1398. https://doi.org/10.11607/jomi.5875
Uzeda MJ, de Brito Resende RF, Sartoretto SC, Alves A, Granjeiro JM, Calasans-Maia MD (2017) Randomized clinical trial for the biological evaluation of two nanostructured biphasic calcium phosphate biomaterials as a bone substitute. Clin Implant Dent Relat Res 19(5):802–811. https://doi.org/10.1111/cid.12516
Milani S, Dal Pozzo L, Rasperini G, Sforza C, Dellavia C (2016) Deproteinized bovine bone remodeling pattern in alveolar socket: a clinical immunohistological evaluation. Clin Oral Implants Res 27(3):295–302. https://doi.org/10.1111/clr.12535
Anitua E, Murias-Freijo A, Alkhraisat MH, Orive G (2015) Clinical, radiographical, and histological outcomes of plasma rich in growth factors in extraction socket: a randomized controlled clinical trial. Clin Oral Investig 19(3):589–600. https://doi.org/10.1007/s00784-014-1278-2
Heberer S, Al-Chawaf B, Jablonski C, Nelson JJ, Lage H, Nelson K (2011) Healing of ungrafted and grafted extraction sockets after 12 weeks: a prospective clinical study. Int J Oral Maxillofac Implants 26(2):385–392
Froum S, Cho SC, Rosenberg E, Rohrer M, Tarnow D (2002) Histological comparison of healing extraction sockets implanted with bioactive glass or demineralized freeze-dried bone allograft: a pilot study. J Periodontol 73(1):94–102. https://doi.org/10.1902/jop.2002.73.1.94
Keil C, Gollmer B, Zeidler-Rentzsch I, Gredes T, Heinemann F (2021) Histological evaluation of extraction sites grafted with Bio-Oss Collagen - randomized controlled trial. Ann Anat 151722. doi:https://doi.org/10.1016/j.aanat.2021.151722
Stumbras A, Januzis G, Gervickas A, Kubilius R, Juodzbalys G (2020) Randomized and controlled clinical trial of bone healing after alveolar ridge preservation using xenografts and allografts versus plasma rich in growth factors. J Oral Implantol 46(5):515–525. https://doi.org/10.1563/aaid-joi-D-19-00179
Crespi R, Cappare P, Romanos GE, Mariani E, Benasciutti E, Gherlone E (2011) Corticocancellous porcine bone in the healing of human extraction sockets: combining histomorphometry with osteoblast gene expression profiles in vivo. Int J Oral Maxillofac Implants 26(4):866–872
Novaes AB Jr, Garani Fernandes P, Adelino Suaid F, de Moraes Grisi MF, Scombatti de Souza SS, Taba M Jr, Bazan Palioto D, Muglia VA (2012) Ridge preservation with acellular dermal matrix and anorganic bone matrix cell-binding peptide P-15 after tooth extraction in humans. A histologic and morphometric study. J Osseointegration 2(4):23–30
Alkan EA, Tuter G, Parlar A, Yucel A, Kurtis B (2016) Evaluation of peri-implant crevicular fluid prostaglandin E2 levels in augmented extraction sockets by different biomaterials. Acta Odontol Scand 74(7):532–538. https://doi.org/10.1080/00016357.2016.1214979
Sanz M, Lindhe J, Alcaraz J, Sanz-Sanchez I, Cecchinato D (2017) The effect of placing a bone replacement graft in the gap at immediately placed implants: a randomized clinical trial. Clin Oral Implants Res 28(8):902–910. https://doi.org/10.1111/clr.12896
Natto ZS, Parashis A, Steffensen B, Ganguly R, Finkelman MD, Jeong YN (2017) Efficacy of collagen matrix seal and collagen sponge on ridge preservation in combination with bone allograft: A randomized controlled clinical trial. J Clin Periodontol 44(6):649–659. https://doi.org/10.1111/jcpe.12722
Gomes-Ferreira PH, Okamoto R, Ferreira S, De Oliveira D, Momesso GA, Faverani LP (2016) Scientific evidence on the use of recombinant human bone morphogenetic protein-2 (rhBMP-2) in oral and maxillofacial surgery. Oral Maxillofac Surg 20(3):223–232. https://doi.org/10.1007/s10006-016-0563-4
Kelly MP, Vaughn OL, Anderson PA (2016) Systematic review and meta-analysis of recombinant human bone morphogenetic protein-2 in localized alveolar ridge and maxillary sinus augmentation. J Oral Maxillofac Surg 74(5):928–939. https://doi.org/10.1016/j.joms.2015.11.027
Schliephake H (2015) Clinical efficacy of growth factors to enhance tissue repair in oral and maxillofacial reconstruction: a systematic review. Clin Implant Dent Relat Res 17(2):247–273. https://doi.org/10.1111/cid.12114
Corbella S, Taschieri S, Francetti L, Weinstein R, Del Fabbro M (2017) Histomorphometric results after postextraction socket healing with different biomaterials: a systematic review of the literature and meta-analysis. Int J Oral Maxillofac Implants 32(5):1001–1017. https://doi.org/10.11607/jomi.5263
Dias S (2018) Network meta-analysis for decision making. Wiley, Hoboken
Phillippo DM, Dias S, Ades AE, Didelez V, Welton NJ (2018) Sensitivity of treatment recommendations to bias in network meta-analysis. J R Stat Soc Ser A Stat Soc 181(3):843–867. https://doi.org/10.1111/rssa.12341
Salanti G, Del Giovane C, Chaimani A, Caldwell DM, Higgins JP (2014) Evaluating the quality of evidence from a network meta-analysis. PLoS One 9(7):e99682. https://doi.org/10.1371/journal.pone.0099682
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
Not applicable
Informed consent
Not applicable
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The manuscript represents the proceedings of a consensus conference of the Italian Society of Osseointegration (IAO, https://www.iao-online.com).
Supplementary information
Supplemental Fig. 1.
Risk of Bias table (JPG 563 kb)
Supplemental Fig. 2
A-B-C. Spontaneous healing vs xenografts dimensional data 2a horizontal 2b vertical 2c histological data. (JPEG 4675 kb)
Supplemental Fig. 2
D. Subgroup analysis for SH Vs XG. The forest plot displays the study labels, the number of studies within each group ( K), the plot of effect sizes and their CIs ( plot), the values of effect sizes (Hedge’s g) and their CIs, and the p-values (p-value) of the corresponding significance tests. The test investigates whether the overall effect sizes corresponding to two groups are different or not. (PDF 970 kb)
Supplemental Fig. 3
A-B Spontaneous healing vs allografts dimensional data 3a horizontal 3b vertical 3c histological data. (JPEG 3072 kb)
Supplemental Fig. 3
D Subgroup analysis for SH Vs AG. The forest plot displays the study labels, the number of studies within each group ( K), the plot of effect sizes and their CIs ( plot), the values of effect sizes and their CIs (esci), and the p-values (pvalue) of the corresponding significance tests. The test investigates whether the overall effect sizes corresponding to two groups are the same. (PDF 904 kb)
Supplemental Fig. 4
A-B Spontaneous healing vs alloplasts dimensional data 4a horizontal 4b vertical 4c histological data (JPEG 3484 kb)
Supplemental Fig. 5
A-B Spontaneous healing vs platelet concentrates dimensional data 5a horizontal 5b vertical 5c histological data (JPEG 2009 kb)
Supplemental Fig. 6
A Network Geometry Plot for horizontal outcome in preserving alveolar socket for 3–4 months’ follow-up. Supplemental Fig. 6B. Predictive Interval and Confidence Interval Plot in preserving alveolar socket for 3–4 months’ follow-up. Supplemental Fig. 6C. Multidimensional Scale Ranking for 3–4 months’ follow-up for horizontal dimension. (JPEG 2363 kb)
Supplemental Fig. 7
A Network Geometry Plot for Horizontal Outcome in preserving alveolar socket for ≥ 6 months’ follow-up. Supplemental Fig. 7B. Predictive Interval and Confidence Interval Plot in preserving alveolar socket for ≥ 6 months’ follow-up for Horizontal Dimension. Supplemental Fig. 7C. Multidimensional Scale Ranking for ≥6 months’ follow-up for horizontal dimension. (JPEG 2228 kb)
Supplemental Fig. 8
A Network Geometry Plot for vertical dimension outcome in preserving alveolar socket for 3–4 months’ follow-up. Supplemental Fig. 8B. Predictive Interval and Confidence Interval Plot in preserving alveolar socket for ≥ 3–4 months’ follow-up for vertical dimension outcome. Supplemental Fig. 8C. Multidimensional Scale Ranking for 3–4 months’ follow-up for vertical dimension. (JPEG 2489 kb)
Supplemental Fig. 9
A Network Geometry Plot for vertical dimension outcome in preserving alveolar socket for ≥6 months’ follow-up. Supplemental Fig. 9B. Predictive Interval and Confidence Interval Plot in preserving alveolar socket for ≥ 6 months’ follow-up for vertical dimension. Supplemental Fig. 9C. Multidimensional Scale Ranking for 6 months’ follow-up for vertical dimension. (JPEG 2069 kb)
ESM 1
(DOCX 137 kb)
Rights and permissions
About this article
Cite this article
Canullo, L., Del Fabbro, M., Khijmatgar, S. et al. Dimensional and histomorphometric evaluation of biomaterials used for alveolar ridge preservation: a systematic review and network meta-analysis. Clin Oral Invest 26, 141–158 (2022). https://doi.org/10.1007/s00784-021-04248-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04248-1