Abstract
Aim
To systematically review the literature to compare the efficacy of air polishing to hand or ultrasonic instrumentation to reduce periodontal inflammation during treatment of residual pockets or supportive periodontal care.
Methods
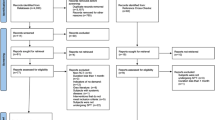
Electronic searches were performed in five different databases, and two databases were used to capture the “grey literature partially.” Clinical trials that compared the use of an air-polishing device to either conventional scaling and root planing (hand and/or ultrasonic instrumentation) or no treatment during periodontal therapy were included without restriction of year and publication status. The Joanna Briggs Institute instrument for clinical trials was used to appraise the studies critically. The results were submitted to qualitative descriptive analysis. The systematic review protocol was registered in PROSPERO (CRD420220156176).
Results
Electronic searches found 1100 hits published between 2008 and 2019. Thirteen studies were included in the review, out of which four had a follow-up longer than 180 days. Results indicated no differences between the efficacy of air polishing and hand or ultrasonic instruments to reduce periodontal inflammation.
Conclusions
Our findings suggest that there is no difference in the efficacy of air polishing and hand or ultrasonic instrumentation to control biofilm and reduce periodontal inflammation. However, these findings must be carefully interpreted owing to methodological issues, including a short follow-up, and a potential conflict of interest related to industry funding.
Clinical relevance
Air polishing for biofilm control may be used as an alternative to hand and ultrasonic instrumentation to reduce periodontal inflammation during treatment of residual pockets or supportive periodontal care.

Similar content being viewed by others
References
Nascimento GG, Leite FRM, Scheutz F, López R (2017) Periodontitis: from Infection to Inflammation. Curr Oral Health Rep 4(4):301–308
Belibasakis GN, Mylonakis E (2015) Oral infections: clinical and biological perspectives. Virulence 6(3):173–176. https://doi.org/10.1080/21505594.2015.1025191
Haffajee AD, Cugini MA, Dibart S, Smith C, Kent RL Jr, Socransky SS (1997) The effect of SRP on the clinical and microbiological parameters of periodontal diseases. J Clin Periodontol 24(5):324–334. https://doi.org/10.1111/j.1600-051x.1997.tb00765.x
Petersilka G, Faggion CM Jr, Stratmann U, Gerss J, Ehmke B, Haeberlein I, Flemmig TF (2008) Effect of glycine powder air-polishing on the gingiva. J Clin Periodontol 35(4):324–332. https://doi.org/10.1111/j.1600-051X.2007.01195.x
Park EJ, Kwon EY, Kim HJ, Lee JY, Choi J, Joo JY (2018) Clinical and microbiological effects of the supplementary use of an erythritol powder air-polishing device in non-surgical periodontal therapy: a randomized clinical trial. J Periodontal Implant Sci 48(5):295–304. https://doi.org/10.5051/jpis.2018.48.5.295
Möene R, Decaillet F, Andersen E, Mombelli A (2010) Subgingival plaque removal using a new air-polishing device. J Periodontol 81(1):79–88. https://doi.org/10.1902/jop.2009.090394
Flemmig TF, Hetzel M, Topoll H, Gerss J, Haeberlein I, Petersilka G (2007) Subgingival debridement efficacy of glycine powder air polishing. J Periodontol 78(6):1002–1010. https://doi.org/10.1902/jop.2007.060420
Zhang J, Liu J, Li J, Chen B, Li H, Yan F (2019) The clinical efficacy of subgingival debridement by ultrasonic instrumentation compared with subgingival air polishing during periodontal maintenance: a systematic review. J Evid Based Dent Pract 19(4):101314. https://doi.org/10.1016/j.jebdp.2019.02.001
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700. https://doi.org/10.1136/bmj.b2700
Balshem H, Helfand M, Schunemann HJ, Oxman AD, Kunz R, Brozek J, Vist GE, Falck-Ytter Y, Meerpohl J, Norris S, Guyatt GH (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64(4):401–406. https://doi.org/10.1016/j.jclinepi.2010.07.015
Tufanaru CMZ, Aromataris E, Campbell J, Hopp L (2017) Chapter 3: Systematic reviews of effectiveness. In: Aromataris E, Munn Z (eds) Joanna Briggs Institute Reviewer's Manual. Joanna Briggs Institute, Australia
Kruse AB, Akakpo DL, Maamar R, Woelber JP, Al-Ahmad A, Vach K, Ratka-Krueger P (2019) Trehalose powder for subgingival air-polishing during periodontal maintenance therapy: A randomized controlled trial. J Periodontol 90(3):263–270. https://doi.org/10.1002/JPER.17-0403
Simon CJ, Munivenkatappa Lakshmaiah Venkatesh P, Chickanna R (2015) Efficacy of glycine powder air polishing in comparison with sodium bicarbonate air polishing and ultrasonic scaling - a double-blind clinico-histopathologic study. Int J Dent Hyg 13(3):177–183. https://doi.org/10.1111/idh.12133
Wennström JL, Dahlen G, Ramberg P (2011) Subgingival debridement of periodontal pockets by air polishing in comparison with ultrasonic instrumentation during maintenance therapy. J Clin Periodontol 38(9):820–827. https://doi.org/10.1111/j.1600-051X.2011.01751.x
Hägi TT, Hofmanner P, Salvi GE, Ramseier CA, Sculean A (2013) Clinical outcomes following subgingival application of a novel erythritol powder by means of air polishing in supportive periodontal therapy: a randomized. controlled clinical study. Quintessence Int 44(10):753–761. https://doi.org/10.3290/j.qi.a30606
Müller N, Moene R, Cancela JA, Mombelli A (2014) Subgingival air-polishing with erythritol during periodontal maintenance: randomized clinical trial of twelve months. J Clin Periodontol 41(9):883–889. https://doi.org/10.1111/jcpe.12289
Flemmig TF, Arushanov D, Daubert D, Rothen M, Mueller G, Leroux BG (2012) Randomized controlled trial assessing efficacy and safety of glycine powder air polishing in moderate-to-deep periodontal pockets. J Periodontol 83(4):444–452. https://doi.org/10.1902/jop.2011.110367
Kargas K, Tsalikis L, Sakellari D, Menexes G, Konstantinidis A (2015) Pilot study on the clinical and microbiological effect of subgingival glycine powder air polishing using a cannula-like jet. Int J Dent Hyg 13(3):161–169. https://doi.org/10.1111/idh.12104
Caygur A, Albaba MR, Berberoglu A, Yilmaz HG (2017) Efficacy of glycine powder air-polishing combined with scaling and root planing in the treatment of periodontitis and halitosis: A randomised clinical study. J Int Med Res 45(3):1168–1174. https://doi.org/10.1177/0300060517705540
Lu H, He L, Zhao Y, Meng H (2018) The effect of supragingival glycine air polishing on periodontitis during maintenance therapy: a randomized controlled trial. PeerJ 6:e4371. https://doi.org/10.7717/peerj.4371
Tsang YC, Corbet EF, Jin LJ (2018) Subgingival glycine powder air-polishing as an additional approach to nonsurgical periodontal therapy in subjects with untreated chronic periodontitis. J Periodontal Res 53(3):440–445. https://doi.org/10.1111/jre.12532
Phillips B, Ball C, Sackett D, D. B (2009) Oxford Centre for Evidence-based Medicine – Levels of Evidence. Oxford Centre for Evidence-based Medicine,
Axelsson P, Nystrom B, Lindhe J (2004) The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J Clin Periodontol 31(9):749–757. https://doi.org/10.1111/j.1600-051X.2004.00563.x
Dosumu EB, Arowojolu MO, Savage KO (2002) Alveolar bone regeneration pattern following surgical and non-surgical treatment in juvenile periodontitis. West Afr J Med. 21(4):272–275
Michalowicz BS, Hodges JS, DiAngelis AJ, Lupo VR, Novak MJ, Ferguson JE, Buchanan W, Bofill J, Papapanou PN, Mitchell DA, Matsoane S, Tschida PA (2006) Treatment of periodontal disease and the risk of preterm birth. N Engl J Med. 355(18):1885–1894
Macones GA, Parry S, Nelson DB, Strauss JF, Ludmir J, Cohen AW, Stamilio DM, Appleby D, Clothier B, Sammel MD, Jeffcoat M (2010) Treatment of localized periodontal disease in pregnancy does not reduce the occurrence of preterm birth: results from the Periodontal Infections and Prematurity Study (PIPS). Am J Obstet Gynecol. 202(2):147.e1–147.e8
Jaramillo A, Arce R, Contreras A, Herrera JA (2012) Effect of periodontal therapy on the subgingival microbiota in preeclamptic patients. Biomedica. 32(2):233–238
López NJ, Quintero A, Casanova PA, Martínez B (2014) Routine prophylaxes every 3 months improves chronic periodontitis status in type 2 diabetes. J Periodontol. 85(7):e232–e240
Funding
This study was also financed in part by CAPES (Coordination for the Improvement of Higher Education Personnel–Brazilian Ministry of Education)-Finance Code 001. We are also thankful for the support of CNPq (Council for Scientific and Technological Development–Brazilian Ministry of Science, Technology and Innovations)-Finance Code 307808/2018-1.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOC 64 kb)
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Nascimento, G.G., Leite, F.R.M., Pennisi, P.R.C. et al. Use of air polishing for supra- and subgingival biofilm removal for treatment of residual periodontal pockets and supportive periodontal care: a systematic review. Clin Oral Invest 25, 779–795 (2021). https://doi.org/10.1007/s00784-020-03762-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03762-y