Abstract
Objectives
To determine if periodontitis patients benefit from treatment with Lactobacillus brevis and Lactobacillus plantarum strains, applied into periodontal pockets as gel and thereafter taken as lozenges, as an adjunct to scaling and root planing (SRP).
Materials and methods
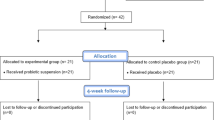
In a double-blind, randomized, placebo-controlled trial, 40 patients received scaling and root planing (SRP) in two sessions within 7 days. Patients then received either probiotic gel and lozenges (n = 20) or placebo (n = 20). The primary outcome variable was the number of diseased sites (DS: PD > 4 mm + BOP) at the 3-month re-evaluation. The effects of gender, age, probiotic therapy, presence of Porphyromonas gingivalis or Aggregatibacter actinomycetemcomitans, smoking, tooth being a molar and interdental location were evaluated using a multivariate multilevel logistic regression model.
Results
The number of DS after 3 months was similar in the test (Me = 8, IQR = 5–11) and control (Me = 5, IQR = 1–10) groups. Both groups showed substantial but equivalent improvements in periodontal parameters. The logistic regression showed higher odds for the healing of gingival bleeding (OR = 2.12, p = 0.048) and lower odds for the healing of DS (OR = 0.51; p < 0.001) in the probiotic group.
Conclusions
Patients with periodontitis benefit from adjunctive use of probiotics containing L. brevis and L. plantarum in terms of reduction of gingival bleeding. However, adjunctive probiotics increase the number of persisting diseased sites with PD > 4 mm and BOP.
Clinical relevance
The adjunctive use of probiotics containing L. brevis and L. plantarum strains in treating chronic periodontitis results in a higher number of residual diseased sites when compared with SRP + placebo; its use is therefore unfounded.


Similar content being viewed by others
References
Haffajee AD, Teles R, Socransky S (2006) The effect of periodontal therapy on the composition of the subgingival microbiota. Periodontology 2000 42:219–258
Goodson J, Haffajee A, Socransky S, Kent R, Teles R, Hasturk H, Bogren A, Van Dyke T, Wennstrom J, Lindhe J (2012) Control of periodontal infections: a randomized controlled trial I. The primary outcome attachment gain and pocket depth reduction at treated sites. J Clin Periodontol 39(6):526–536
Teughels W, Durukan A, Ozcelik O, Pauwels M, Quirynen M, Haytac MC (2013) Clinical and microbiological effects of Lactobacillus reuteri probiotics in the treatment of chronic periodontitis: a randomized placebo-controlled study. J Clin Periodontol 40(11):1025–1035
Teughels W, Newman M, Coucke W, Haffajee AD, Van der Mei HC, Kinder Haake S, Schepers E, Cassisman JJ, Van Eldere J, van Steenberghe D, Quirynen M (2007) Guiding periodontal pocket recolonization: a proof of concept. J Dent Res 86(11):1078–1082
Geier M, Butler R, Howarth G (2007) Inflammatory bowel disease: current insights into pathogenesis and new therapeutic options; probiotics, prebiotics and synbiotics. Int J Food Microbiol 115(1):1–11
Bermúdez-Brito M, Plaza-Díaz J, Muñoz-Quezada S, Gómez-Llorente C, Gil A (2012) Probiotic mechanisms of action. Ann Nutr Metab 61(2):160–174
Bhuvaneswarri J, Ramya V, Manisundar P (2013) Probiotics and its implications in periodontal therapy: a review. IOSR JDMS 2(5):11–15
Bosch M, Nart J, Audivert S, Bonachera M, Alemany A, Fuentes M, Cune J (2012) Isolation and characterization of probiotic strains for improving oral health. Arch Oral Biol 57(5):539–549
Fang F, Xu J, Li Q, Xia X, Du G (2018) Characterization of a Lactobacillus brevis strain with potential oral probiotic properties. BMC Microbiol 18(1):221–230
Koll-Klais P, Mandar R, Leibur E, Marcotte H, Hammarstrom L, Mikelsaar M (2005) Oral lactobacilli in chronic periodontitis and periodontal health: species composition and antimicrobial activity. Oral Microbiol Immunol 20(6):354–361
Della Riccia DN, Bizzini F, Perilli MG, Polimeni A, Trinchieri V, Amicosante G, Cifone MG (2007) Anti-inflammatory effects of Lactobacillus brevis (CD2) on periodontal disease. Oral Dis 13(4):376–385
Mayanagi G, Kimura M, Nakaya S, Hirata H, Sakamoto M, Benno Y, Shimauchi H (2009) Probiotic effects of orally administered Lactobacillus salivarius WB21-containing tablets on periodontopathic bacteria: a controlled, randomized clinical trial. J Clin Periodontol 36(6):506–513
Shimauchi H, Mayanagi G, Nakaya S, Minamibuchi M, Ito Y, Yamaki K, Hirata H (2008) Improvement of periodontal condition by probiotics with Lactobacillus salivarius WB21: placebo-controlled study. J Clin Periodontol 35(10):897–905
Vicario M, Santos A, Violant D, Nart J, Giner L (2013) Clinical changes in periodontal subjects with the probiotic Lactobacillus reuteri Prodentis: a preliminary randomized clinical trial. Acta Odontol Scand 71(3–4):813–819
Lee J, Kim S, Ko S, Ouwehand A, Ma D (2015) Modulation of the host response by probiotic Lactobacillus Brevis CD2 in experimental gingivitis. Oral Dis 21(6):705–712
Krasse P, Carlsson B, Dahl C, Paulsson A, Nilsson A, Sinkiewicz G (2006) Decreased gum bleeding and reduced gingivitis by the probiotic Lactobacillus reuteri. Swed Dent J 30(2):55–60
Martin-Cabezas R, Davideau J, Tenenbaum H, Huck O (2016) Clinical efficacy of probiotics as an adjunctive therapy to non-surgical periodontal treatment of chronic periodontitis: a systematic review and meta-analysis. J Clin Periodontol 43(6):520–530
Matsubara VH, Bandara HMHN, Ishikawa KH, Mayer PA, Samaranayake LP (2016) The role of probiotic bacteria in managing periodontal disease: a systematic review. Expert Rev Anti-Infect Ther 14(7):643–655
Ikram S, Hassan N, Raffat MA, Mirza S, Akram Z (2018) Systematic review and meta- analysis of double- blind, placebo- controlled, randomized clinical trials using probiotics in chronic periodontitis. J Investig Clin Dent 9(3):e12338
Tekce M, Ince G, Gursoy HSDI, Cakar G, Kadir T, Clinical YS (2015) Clinical and microbiological effects of probiotic lozenges in the treatment of chronic periodontitis: a 1-year follow-up study. J Clin Periodontol 42(4):363–372
Stamatova I, Meurman JH (2009) Probiotics and periodontal disease. Periodontology 2000 51(1):141–151
Montero E, Iniesta M, Rodrigo M, Marín MJ, Figuero E, Herrera D, Sanz M (2017) Clinical and microbiological effects of the adjunctive use of probiotics in the treatment of gingivitis: a randomized controlled clinical trial. J Clin Periodontol 44(7):708–716
Laleman I, Eftal Y, Ozcelik O, Haytac C, Pauwels M, Herrero ER, Slomka V, Quirynen M, Alkaya B, Teughels W (2015) The effect of a streptococci containing probiotic in periodontal therapy: a randomized controlled trial. J Clin Periodontol 42(11):1032–1041
Vivekananda MR, Vandana KL, Bhat KG (2010) Effect of the probiotic Lactobacilli reuteri (Prodentis) in the management of periodontal disease: a preliminary randomized clinical trial. J Oral Microbiol 2:5344
Sajedinejad N, Paknejad M, Houshmand B, Sharafi H, Jelodar R, Zahiri HS, Noghabi KA (2017) Lactobacillus salivarius NK02: a potent probiotic for clinical application in mouthwash. Probiotics & Antimicro Prot 10(3):485–495
Morales A, Carvajal P, Silva N, Hernandez M, Godoy C (2016) Clinical effects of Lactobacillus rhamnosus in non-surgical treatment of chronic periodontitis: a randomized placebo-controlled trial with 1-year follow-up. J Periodontol 87(8):944–952
Pelekos G, Ho SN, Acharya A, Keung Leung W, McGrath C (2019) A double-blind, paralleled-arm, placebo-controlled, randomized clinical trial of the effectiveness of probiotics as an adjunct in periodontal care. J Clin Periodontol 46(12):1217–1227
Invernici MM, Salvador SL, Silva PHF, Soares MSM, Casarin R, Palioto DB, Souza SLS, Taba M Jr, Novaes AB Jr, Furlaneto FAC, Messora MR (2018) Effects of Bifidobacterium probiotic on the treatment of chronic periodontitis: a randomized clinical trial. J Clin Periodontol 45(10):1198–1210
Tomasi C, Leyland AH, Wennström JL (2007) Factors influencing the outcome of non-surgical periodontal treatment : a multilevel approach. J Clin Periodontol 34(8):682–690
Salvi GE, Lang NP (2005) The effects of non-steroidal anti-inflammatory drugs (selective and non-selective) on the treatment of periodontal diseases. Curr Pharm Des 11(14):1757–1769
Saminsky M, Halperin-Sternfeld M, Machtei EE, Horwitz J (2015) Variables affecting tooth survival and changes in probing depth: a long-term follow-up of periodontitis patients. J Clin Periodontol 42(6):513–519
Loos B, Nylund K, Claffey N, Egelberg J (1989) Clinical effects of root debridement in molar and non-molar teeth. A 2-year follow-up. J Clin Periodontol 16(8):498–504
Boutaga K, Winkelhoff AJ, Vandenbroucke-Grauls CMJE, Savelkoul PHM (2005) Periodontal pathogens: a quantitative comparison of anaerobic culture and real-time PCR. FEMS Immunology & Medical Microbiology 45(2):191–199
Brennan CA, Garrett WS (2019) Fusobacterium nucleatum - symbiont, opportunist and oncobacterium. Nat Rev Microbiol 17(3):156–166
Haffajee AD, Patel M, Socransky S (2008) Microbiological changes associated with four different periodontal therapies for the treatment of chronic periodontitis. Oral Microbiol Immunol 23(2):148–157
Patyna M, Deschner J, Kasaj A (2018) PR398: comparison of probiotics combined with antimicrobial photodynamic therapy in periodontal treatment. J Clin Periodontol 45(S19)
Meimandi M, Talebi Ardakani MR, Nejad AE, Yousefnejad P, Tayeed MH (2017) The effect of photodynamic therapy in the treatment of chronic periodontitis: a review of literature. J Lasers Med Sci 8(Suppl 1):S7–S11
Suez J, Zmora N, Zilberman-Schapira G, Mor U, Dori-Bachash M, Bashiardes S et al (2018) Post-antibiotic gut mucosal microbiome reconstitution is impaired by probiotics and improved by autologous FMT. Cell 174(6):1406–1423.e16
Zmora N, Zilberman-Schapira G, Suez J, Mor U, Dori-Bachash M, Bashiardes S et al (2018) Personalized gut mucosal colonization resistance to empiric probiotics is associated with unique host and microbiome features. Cell 174(6):1388–1405.e21
Çaglar E, Cildir S, Ergeneli S, Sandalli N, Twetman S (2006) Salivary mutans streptococci and lactobacilli levels after ingestion of the probiotic bacterium lactobacilli reuteri ATCC 55739 by straws or tablets. Acta Odontol Scand 64:314–318
Horz H, Meinelt A, Houben B, Conrads G (2007) Distribution and persistence of probiotic Streptococcus salivarius K12 in the human oral cavity as determined by real-time quantitative polymerase chain reaction. Oral Microbiol Immunol 22:126–130
Teughels W, Loozen G, Quirynen M (2011) Do probiotics offer opportunities to manipulate the periodontal oral microbiota? J Clin Periodontol 38(Suppl. 11):159–177
Sanz M, Herrera D, Kebschull M, Chapple I, Jepsen S, Berglund T, Sculean A, Tonetti MS Treatment of Stage I-III Periodontitis – the EFP S3 level Clinical Practice Guidelines. J Clin Periodontol, accepted for publication
Funding
The study was supported by the Ministry of Science and Technology of the Republic of Slovenia, grant No. P3-0293. We thank to Mrs. Vanja Erčulj, PhD (RHO sigma, Ljubljana) for statistical analysis. Probiotic and placebo gel and lozenges were donated by CMS Dental, Copenhagen, Denmark. The authors have declared no conflicts of interest in connection with this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures involving human participants were in accordance with the ethical standards of the 1964 Helsinki declaration and the Code of Medical Ethics of the Medical Association of Slovenia. The study protocol was reviewed by the National Medical Ethic Committee (No. 0120-365/2018/5) of the Republic of Slovenia. It was also registered at Clinicaltrials.gov (NCT04137419).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pudgar, P., Povšič, K., Čuk, K. et al. Probiotic strains of Lactobacillus brevis and Lactobacillus plantarum as adjunct to non-surgical periodontal therapy: 3-month results of a randomized controlled clinical trial. Clin Oral Invest 25, 1411–1422 (2021). https://doi.org/10.1007/s00784-020-03449-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03449-4