Abstract
Aim
The aim of this article is to systematically review the effect of subcrestal implant placement compared with equicrestal position on hard and soft tissues around dental implants with platform switch.
Material and methods
A manual and electronic search (National Library of Medicine and Cochrane Central Register of Controlled Trials) was performed for animal and human studies published up to December 2016. Primary outcome variable was marginal bone level (MBL) and secondary outcomes were crestal bone level (CBL), soft tissue dimensions (barrier epithelium, connective tissue, and peri-implant mucosa), and changes in the position of soft tissue margin. For primary and secondary outcomes, data reporting mean values and standard deviations of each study were extracted and weighted mean differences (WMDs) and 95% confidence intervals (CIs) were calculated.
Results
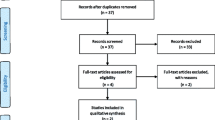
A total of 14 publications were included (7 human studies and 7 animal investigations). The results from the meta-analyses have shown that subcrestal implants, when compared with implants placed in an equicrestal position, exhibited less MBL changes (human studies: WMD = − 0.18 mm; 95% CI = − 1.31 to 0.95; P = 0.75; animal studies: WMD = − 0.45 mm; 95% CI = − 0.66 to − 0.24; P < 0.001). Furthermore, the CBL was located at a more coronal position in subcrestal implants with respect to the implant shoulder (WMD = − 1.09 mm; 95% CI = − 1.43 to − 0.75; P < 0.001). The dimensions of the peri-implant mucosa seem to be affected by the positioning of the microgap and were greater at implants placed in a subcrestal position than those inserted equicrestally (WMD = 0.60 mm; 95% CI = 0.26 to 0.95; P < 0.001). While the length of the barrier epithelium was significantly greater in implants placed in a subcrestal position (WMD = 0.39 mm; 95% CI = 0.19 to 0.58; P < 0.001), no statistical significant differences were observed between equicrestal and subcrestal implant positioning for the connective tissue length (WMD = 0.17 mm; 95% CI = − 0.03 to 0.36; P = 0.10).
Conclusion
This systematic review suggests that PS implants placed in a subcrestal position have less MBL changes when compared with implants placed equicrestally. Furthermore, the location of the microgap seems to have an influence on the dimensions of peri-implant soft tissues.
Clinical relevance
When compared with PS placed in an equicrestal position, subcrestal implant positioning demonstrated less peri-implant bone remodeling.




Similar content being viewed by others
References
Leonhardt A, Grondahl K, Bergstrom C, Lekholm U (2002) Long-term follow-up of osseointegrated titanium implants using clinical, radiographic and microbiological parameters. Clin Oral Implants Res 13(2):127–132. https://doi.org/10.1034/j.1600-0501.2002.130202.x
Rasmusson L, Roos J, Bystedt H (2005) A 10-year follow-up study of titanium dioxide-blasted implants. Clin Implant Dent Relat Res 7(1):36–42. https://doi.org/10.1111/j.1708-8208.2005.tb00045.x
Pjetursson BE, Thoma D, Jung R, Zwahlen M, Zembic A (2012) A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after a mean observation period of at least 5 years. Clin Oral Implants Res 23(Suppl 6):22–38. https://doi.org/10.1111/j.1600-0501.2012.02546.x
Palaska I, Tsaousoglou P, Vouros I, Konstantinidis A, Menexes G (2016) Influence of placement depth and abutment connection pattern on bone remodeling around 1-stage implants: a prospective randomized controlled clinical trial. Clin Oral Implants Res 27(2):e47–e56. https://doi.org/10.1111/clr.12527
Adell R, Lekholm U, Rockler B, Branemark PI (1981) A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 10(6):387–416. https://doi.org/10.1016/S0300-9785(81)80077-4
Albrektsson T, Zarb G, Worthington P, Eriksson AR (1986) The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants 1(1):11–25
Laurell L, Lundgren D (2011) Marginal bone level changes at dental implants after 5 years in function: a meta-analysis. Clin Implant Dent Relat Res 13(1):19–28. https://doi.org/10.1111/j.1708-8208.2009.00182.x
Hermann JS, Buser D, Schenk RK, Schoolfield JD, Cochran DL (2001) Biologic width around one- and two-piece titanium implants. Clin Oral Implants Res 12(6):559–571. https://doi.org/10.1034/j.1600-0501.2001.120603.x
Linkevicius T, Apse P, Grybauskas S, Puisys A (2009) The influence of soft tissue thickness on crestal bone changes around implants: a 1-year prospective controlled clinical trial. Int J Oral Maxillofac Implants 24(4):712–719
Blanco J, Nunez V, Aracil L, Munoz F, Ramos I (2008) Ridge alterations following immediate implant placement in the dog: flap versus flapless surgery. J Clin Periodontol 35(7):640–648. https://doi.org/10.1111/j.1600-051X.2008.01237.x
Tarnow DP, Cho SC, Wallace SS (2000) The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol 71(4):546–549. https://doi.org/10.1902/jop.2000.71.4.546
Rodriguez-Ciurana X, Vela-Nebot X, Segala-Torres M, Calvo-Guirado JL, Cambra J, Mendez-Blanco V, Tarnow DP (2009) The effect of interimplant distance on the height of the interimplant bone crest when using platform-switched implants. Int J Periodontics Restorative Dent 29:141–151
Ericsson I, Persson LG, Berglundh T, Marinello CP, Lindhe J, Klinge B (1995) Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol 22(3):255–261
Hermann JS, Buser D, Schenk RK, Cochran DL (2000) Crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged and submerged implants in the canine mandible. J Periodontol 71(9):1412–1424. https://doi.org/10.1902/jop.2000.71.9.1412
Strietzel FP, Neumann K, Hertel M (2015) Impact of platform switching on marginal peri-implant bone-level changes. A systematic review and meta-analysis. Clin Oral Implants Res 26(3):342–358. https://doi.org/10.1111/clr.12339
Hammerle CH, Bragger U, Burgin W, Lang NP (1996) The effect of subcrestal placement of the polished surface of ITI implants on marginal soft and hard tissues. Clin Oral Implants Res 7(2):111–119. https://doi.org/10.1034/j.1600-0501.1996.070204.x
Duyck J, Vandamme K, Geris L, Van Oosterwyck H, De Cooman M, Vandersloten J, Puers R, Naert I (2006) The influence of micro-motion on the tissue differentiation around immediately loaded cylindrical turned titanium implants. Arch Oral Biol 51(1):1–9. https://doi.org/10.1016/j.archoralbio.2005.04.003
Abrahamsson I, Berglundh T, Lindhe J (1997) The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 24(8):568–572. https://doi.org/10.1111/j.1600-051X.1997.tb00230.x
Clementini M, Rossetti PH, Penarrocha D, Micarelli C, Bonachela WC, Canullo L (2014) Systemic risk factors for peri-implant bone loss: a systematic review and meta-analysis. Int J Oral Maxillofac Surg 43(3):323–334. https://doi.org/10.1016/j.ijom.2013.11.012
Zitzmann NU, Berglundh T (2008) Definition and prevalence of peri-implant diseases. J Clin Periodontol 35(8 Suppl):286–291. https://doi.org/10.1111/j.1600-051X.2008.01274.x
Hermann JS, Cochran DL, Nummikoski PV, Buser D (1997) Crestal bone changes around titanium implants. A radiographic evaluation of unloaded nonsubmerged and submerged implants in the canine mandible. J Periodontol 68(11):1117–1130. https://doi.org/10.1902/jop.1997.68.11.1117
Hermann JS, Jones AA, Bakaeen LG, Buser D, Schoolfield JD, Cochran DL (2011) Influence of a machined collar on crestal bone changes around titanium implants: a histometric study in the canine mandible. J Periodontol 82(9):1329–1338. https://doi.org/10.1902/jop.2011.090728
Broggini N, McManus LM, Hermann JS, Medina R, Schenk RK, Buser D, Cochran DL (2006) Peri-implant inflammation defined by the implant-abutment interface. J Dent Res 85(5):473–478. https://doi.org/10.1177/154405910608500515
Jung RE, Jones AA, Higginbottom FL, Wilson TG, Schoolfield J, Buser D, Hammerle CH, Cochran DL (2008) The influence of non-matching implant and abutment diameters on radiographic crestal bone levels in dogs. J Periodontol 79(2):260–270. https://doi.org/10.1902/jop.2008.070132
Cochran DL, Bosshardt DD, Grize L, Higginbottom FL, Jones AA, Jung RE, Wieland M, Dard M (2009) Bone response to loaded implants with non-matching implant-abutment diameters in the canine mandible. J Periodontol 80(4):609–617. https://doi.org/10.1902/jop.2009.080323
Weng D, Nagata MJ, Bell M, Bosco AF, de Melo LG, Richter EJ (2008) Influence of microgap location and configuration on the periimplant bone morphology in submerged implants. An experimental study in dogs. Clin Oral Implants Res 19(11):1141–1147. https://doi.org/10.1111/j.1600-0501.2008.01564.x
Koutouzis T, Fetner M, Fetner A, Lundgren T (2011) Retrospective evaluation of crestal bone changes around implants with reduced abutment diameter placed non-submerged and at subcrestal positions: the effect of bone grafting at implant placement. J Periodontol 82(2):234–242. https://doi.org/10.1902/jop.2010.100340
Donovan R, Fetner A, Koutouzis T, Lundgren T (2010) Crestal bone changes around implants with reduced abutment diameter placed non-submerged and at subcrestal positions: a 1-year radiographic evaluation. J Periodontol 81(3):428–434. https://doi.org/10.1902/jop.2009.090317
Welander M, Abrahamsson I, Berglundh T (2009) Subcrestal placement of two-part implants. Clin Oral Implants Res 20(3):226–231. https://doi.org/10.1111/j.1600-0501.2008.01637.x
Degidi M, Perrotti V, Shibli JA, Novaes AB, Piattelli A, Iezzi G (2011) Equicrestal and subcrestal dental implants: a histologic and histomorphometric evaluation of nine retrieved human implants. J Periodontol 82(5):708–715. https://doi.org/10.1902/jop.2010.100450
Weng D, Nagata MJ, Bosco AF, de Melo LG (2011) Influence of microgap location and configuration on radiographic bone loss around submerged implants: an experimental study in dogs. Int J Oral Maxillofac Implants 26(5):941–946
Novaes AB Jr, Barros RR, Muglia VA, Borges GJ (2009) Influence of interimplant distances and placement depth on papilla formation and crestal resorption: a clinical and radiographic study in dogs. J Oral Implantol 35:18–27
Becker J, Ferrari D, Herten M, Kirsch A, Schaer A, Schwarz F (2007) Influence of platform switching on crestal bone changes at non-submerged titanium implants: a histomorphometrical study in dogs. J Clin Periodontol 34(12):1089–1096. https://doi.org/10.1111/j.1600-051X.2007.01155.x
Becker J, Ferrari D, Mihatovic I, Sahm N, Schaer A, Schwarz F (2009) Stability of crestal bone level at platform-switched non-submerged titanium implants: a histomorphometrical study in dogs. J Clin Periodontol 36(6):532–539. https://doi.org/10.1111/j.1600-051X.2009.01413.x
Schwarz F, Mihatovic I, Golubovich V, Schar A, Sager M, Becker J (2015) Impact of abutment microstructure and insertion depth on crestal bone changes at nonsubmerged titanium implants with platform switch. Clin Oral Implants Res 26(3):287–292. https://doi.org/10.1111/clr.12478
Rodriguez X, Navajas A, Vela X, Fortuno A, Jimenez J, Nevins M (2016) Arrangement of Peri-implant connective tissue fibers around platform-switching implants with conical abutments and its relationship to the underlying bone: a human histologic study. Int J Periodontics Restorative Dent 36(4):533–540. https://doi.org/10.11607/prd.2580
Huang B, Meng H, Zhu W, Witek L, Tovar N, Coelho PG (2015) Influence of placement depth on bone remodeling around tapered internal connection implants: a histologic study in dogs. Clin Oral Implants Res 26(8):942–949. https://doi.org/10.1111/clr.12384
Schwarz F, Hegewald A, Becker J (2014) Impact of implant-abutment connection and positioning of the machined collar/microgap on crestal bone level changes: a systematic review. Clin Oral Implants Res 25(4):417–425. https://doi.org/10.1111/clr.12215
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339(jul21 1):b2700. https://doi.org/10.1136/bmj.b2700
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62(10):1006–1012. https://doi.org/10.1016/j.jclinepi.2009.06.005
Jung BA, Harzer W, Wehrbein H, Gedrange T, Hopfenmuller W, Ludicke G, Moergel M, Diedrich P, Kunkel M (2011) Immediate versus conventional loading of palatal implants in humans: a first report of a multicenter RCT. Clin Oral Investig 15(4):495–502. https://doi.org/10.1007/s00784-010-0407-9
Esposito M, Grusovin MG, Maghaireh H and Worthington HV (2013) Interventions for replacing missing teeth: different times for loading dental implants. Cochrane Database Syst Rev CD003878
Chen ST, Buser D (2009) Clinical and esthetic outcomes of implants placed in postextraction sites. Int J Oral Maxillofac Implants 24(Suppl):186–217
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, Cochrane Bias Methods Group, Cochrane Statistical Methods Group (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343(oct18 2):d5928. https://doi.org/10.1136/bmj.d5928
Ten Heggeler JM, Slot DE, Van der Weijden GA (2011) Effect of socket preservation therapies following tooth extraction in non-molar regions in humans: a systematic review. Clin Oral Implants Res 22(8):779–788. https://doi.org/10.1111/j.1600-0501.2010.02064.x
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605. https://doi.org/10.1007/s10654-010-9491-z
Kilkenny C, Browne W, Cuthill IC, Emerson M, Altman DG, Group NCRRGW (2010) Animal research: reporting in vivo experiments: the ARRIVE guidelines. Br J Pharmacol 160(7):1577–1579. https://doi.org/10.1111/j.1476-5381.2010.00872.x
Schwarz F, Iglhaut G, Becker J (2012) Quality assessment of reporting of animal studies on pathogenesis and treatment of peri-implant mucositis and peri-implantitis. A systematic review using the ARRIVE guidelines. J Clin Periodontol 39(Suppl 12):63–72. https://doi.org/10.1111/j.1600-051X.2011.01838.x
Romanos GE, Aydin E, Gaertner K, Nentwig GH (2015) Long-term results after subcrestal or crestal placement of delayed loaded implants. Clin Implant Dent Relat Res 17(1):133–141. https://doi.org/10.1111/cid.12084
Koutouzis T, Neiva R, Nonhoff J, Lundgren T (2013) Placement of implants with platform-switched Morse taper connections with the implant-abutment interface at different levels in relation to the alveolar crest: a short-term (1-year) randomized prospective controlled clinical trial. Int J Oral Maxillofac Implants 28(6):1553–1563. https://doi.org/10.11607/jomi.3184
Kutan E, Bolukbasi N, Yildirim-Ondur E, Ozdemir T (2015) Clinical and radiographic evaluation of marginal bone changes around platform-switching implants placed in crestal or subcrestal positions: a randomized controlled clinical trial. Clin Implant Dent Relat Res 17(Suppl 2):e364–e375. https://doi.org/10.1111/cid.12248
Pellicer-Chover H, Penarrocha-Diago M, Penarrocha-Oltra D, Gomar-Vercher S, Agustin-Panadero R, Penarrocha-Diago M (2016) Impact of crestal and subcrestal implant placement in peri-implant bone: a prospective comparative study. Med Oral Patol Oral Cir Bucal 21(1):e103–e110
Al Amri MD, Al-Johany SS, Al Baker AM, Al Rifaiy MQ, Abduljabbar TS, Al-Kheraif AA (2016) Soft tissue changes and crestal bone loss around platform-switched implants placed at crestal and subcrestal levels: 36-month results from a prospective split-mouth clinical trial. Clin Oral Implants Res 28(11):1342–1347. https://doi.org/10.1111/clr.12990
de Siqueira RA, Fontao FN, Sartori IA, Santos PG, Bernardes SR, Tiossi R (2016) Effect of different implant placement depths on crestal bone levels and soft tissue behavior: a randomized clinical trial. Clin Oral Implants Res 28(10):1227–1233. https://doi.org/10.1111/clr.12946
Veis A, Parissis N, Tsirlis A, Papadeli C, Marinis G, Zogakis A (2010) Evaluation of peri-implant marginal bone loss using modified abutment connections at various crestal level placements. Int J Periodontics Restorative Dent 30(6):609–617
Weng D, Nagata MJ, Bell M, de Melo LG, Bosco AF (2010) Influence of microgap location and configuration on peri-implant bone morphology in nonsubmerged implants: an experimental study in dogs. Int J Oral Maxillofac Implants 25(3):540–547
Barros RR, Novaes AB Jr, Muglia VA, Iezzi G, Piattelli A (2010) Influence of interimplant distances and placement depth on peri-implant bone remodeling of adjacent and immediately loaded Morse cone connection implants: a histomorphometric study in dogs. Clin Oral Implants Res 21(4):371–378. https://doi.org/10.1111/j.1600-0501.2009.01860.x
Cochran DL, Mau LP, Higginbottom FL, Wilson TG, Bosshardt DD, Schoolfield J, Jones AA (2013) Soft and hard tissue histologic dimensions around dental implants in the canine restored with smaller-diameter abutments: a paradigm shift in peri-implant biology. Int J Oral Maxillofac Implants 28(2):494–502. https://doi.org/10.11607/jomi.3081
Lee J, Fiorini T, Gamborena I, Wenzel BA, Schupbach P, Wikesjo UM, Susin C (2016) Effect of platform shift/switch on crestal bone levels and mucosal profile following flapless surgery and crestal/subcrestal implant placement. Clin Implant Dent Relat Res 18(1):73–81. https://doi.org/10.1111/cid.12243
Huang B, Meng H, Piao M, Xu L, Zhang L, Zhu W (2012) Influence of placement depth on bone remodeling around tapered internal connection implant: a clinical and radiographic study in dogs. J Periodontol 83(9):1164–1171. https://doi.org/10.1902/jop.2012.110617
Pontes AE, Ribeiro FS, Iezzi G, Piattelli A, Cirelli JA, Marcantonio E Jr (2008) Biologic width changes around loaded implants inserted in different levels in relation to crestal bone: histometric evaluation in canine mandible. Clin Oral Implants Res 19(5):483–490. https://doi.org/10.1111/j.1600-0501.2007.01506.x
Fickl S, Zuhr O, Stein JM, Hurzeler MB (2010) Peri-implant bone level around implants with platform-switched abutments. Int J Oral Maxillofac Implants 25(3):577–581
Berglundh T, Lindhe J, Ericsson I, Marinello CP, Liljenberg B, Thomsen P (1991) The soft tissue barrier at implants and teeth. Clin Oral Implants Res 2(2):81–90. https://doi.org/10.1034/j.1600-0501.1991.020206.x
Buser D, Weber HP, Donath K, Fiorellini JP, Paquette DW, Williams RC (1992) Soft tissue reactions to non-submerged unloaded titanium implants in beagle dogs. J Periodontol 63(3):225–235. https://doi.org/10.1902/jop.1992.63.3.225
Cochran DL, Hermann JS, Schenk RK, Higginbottom FL, Buser D (1997) Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodontol 68(2):186–198. https://doi.org/10.1902/jop.1997.68.2.186
Tomasi C, Tessarolo F, Caola I, Wennstrom J, Nollo G, Berglundh T (2014) Morphogenesis of peri-implant mucosa revisited: an experimental study in humans. Clin Oral Implants Res 25(9):997–1003. https://doi.org/10.1111/clr.12223
Lang NP, Wetzel AC, Stich H, Caffesse RG (1994) Histologic probe penetration in healthy and inflamed peri-implant tissues. Clin Oral Implants Res 5(4):191–201. https://doi.org/10.1034/j.1600-0501.1994.050401.x
Lindhe J, Meyle J, Group DoEWoP (2008) Peri-implant diseases: consensus report of the sixth European Workshop on Periodontology. J Clin Periodontol 35:282–285
Buser D, Belser UC, Lang NP (1998) The original one-stage dental implant system and its clinical application. Periossdontol 17(1):106–118. https://doi.org/10.1111/j.1600-0757.1998.tb00128.x
Acknowledgements
The authors would like to thank Dr. Cristina Esquinas, Universitat Internacional de Catalunya, for the statistical analysis. We also thank to Alberto Monje for his support in conducting this systematic review.
Funding
The work was self-funded.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Valles, C., Rodríguez-Ciurana, X., Clementini, M. et al. Influence of subcrestal implant placement compared with equicrestal position on the peri-implant hard and soft tissues around platform-switched implants: a systematic review and meta-analysis. Clin Oral Invest 22, 555–570 (2018). https://doi.org/10.1007/s00784-017-2301-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2301-1