Abstract
Objectives
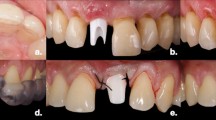
This paper aims to observe peri-implant time-related vertical bone level and soft tissue changes with immediate, non-detached glass-ceramic (lithium-disilicate) individualized abutments and dis-/reconnections.
Materials and methods
Sixteen split-mouth patients received provisionalized immediate definitive individualized abutments (test T) versus dis-/reconnected individualized abutments (control C). In group T, digital impressions were made by using titanium bases (Conelog, Camlog), and individualized abutments (E.maxCAD) and temporary crowns (TelioCAD) were designed and milled (CerecMCXL). Lithium-disilicate abutments were crystallized and luted (Multilink Hybrid Abutment) to titanium bases. Non-occluding temporary crowns were connected to abutments. After 16 weeks, definitive digital restorations were delivered. In group C, 8 weeks were allowed after healing cap mounting for conventional impressions. Lithium-disilicate individualized abutments were produced, try-ins were performed by dis-/reconnections. Crowns were luted. Cone beam computed tomography (CBCT) images were obtained at restoration delivery, 12 months and 24 months. Pink esthetic scoring was made, plaque-gingival index measurements were done and statistical analyses (Shapiro-Wilk, Mann-Whitney U, Wilcoxon’s, Spearman’s rank, α = 0.05) were completed.
Results
No implant failures occurred. At 12 months, T (−0.1 ± 0.14 mm) exhibited significantly reduced vertical bone loss only on the labial side than C (−0.24 ± 0.13 mm) (p < 0.05). In T, all sides except distal presented reduced vertical bone loss at 24 months (p < 0.05). Vertical bone loss for all measurement sides in both C (−0.12 ± 0.09 mm; −0.18 ± 0.11 mm) and T (−0.17 ± 0.11; −0.26 ± 0.10 mm) was higher for 24 months than 12 months, respectively (p < 0.05).
Conclusions
Reduced vertical bone loss was observed around implants with immediate definitive individualized abutments than abutments with repeated dis-/reconnections.
Clinical relevance
Non-detached immediate definitive lithium-disilicate individualized abutments and provisionalization through digital technology resulted in successful clinical outcomes and can be routinely applied.







Similar content being viewed by others
References
Hermann JS, Buser D, Schenk RK, Cochran DL (2000) Crestal bone changes around titanium implants. A histometric evaluation of unloaded non-submerged and submerged implants in the canine mandible J Periodontol 71:1412–1424
Maeda Y, Miura J, Taki I, Sogo M (2007) Biomechanical analysis on platform switching: is there any biomechanic rationale? Clin Oral Imp Res 18:581–584
Canullo L, Pellegrini G, Allievi C, Trombelli L, Annibali S, Dellavia C (2011) Soft tissues around long-term platform switching implant restorations: a histological human evaluation. Preliminary results J Clin Periodont 38:86–94
Becker J, Ferrari D, Mihatovic I, Sahm N, Schaer A, Schwarz F (2009) Stability of crestal bone level at platform-switched non-submerged titanium implants: a histomorphometrical study in dogs. J Clin Periodont 36:532–539
Baffone GM, Botticelli D, Pantani F, Cardoso LC, Schweikert MT, Lang NP (2011) Influence of various implant platform configurations on periimplant tissue dimensions. An experimental study in the dog Clin Oral Imp Res 22:438–444
Romanos GE, Toh CG, Siar CH, Swaminathan D (2002) Histologic and histomorphometric evaluation of peri-implant bone subjected to immediate loading: an experimental study with Macaca fascicularis. Int J Oral Maxillofac Implants 17:44–51
Cochran DL, Hermann JS, Schenk RK, Higginbottom FL, Buser D (1997) Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodont 68:186–198
Hermann JS, Buser D, Schenk RK, Higginbottom FL, Cochran DL (2000) Biologic width around titanium implants. A physiologically formed and stable dimension over time. Clin Oral Impl Res 11:1–11
Linkevicius T, Apse P (2008) Biologic width around implants. An evidence-based review. Stomatologija, Baltic Dental and Maxillofacial J 10:27–35
Linkevicius T, Apse P (2008) Influence of abutment material on stability of peri-implant tissues: a systematic review. Int J Oral Maxillofac Implants 23:449–456
Becker K, Mihatovic I, Golubovic V, Schwarz F (2012) Impact of abutment material and dis/re-connection on soft and hard tissue changes at implants with platform-switching. J Clin Periodontol 39:774–780
Alves CC, Munoz F, Ramos I, Neves M, Blanco J (2015) Marginal bone and soft tissue behavior following platform switching abutment connection/disconnection a dog model study. Clin Oral Impl Res 26:983–999
Romanos GE (2015) Tissue preservation strategies for fostering long-term soft and hard tissue stability. Int J Periodont Restor Dent 35:363–371
Abrahasomsson I, Berglundh T, Lindhe J (1997) The mucosal barrier following abutment dis/re-connection. An experimental study in dogs. J Clin Periodontol 24:568–572
Romanos GE, Malmstrom H, Feng C, Ercoli C, Caton J (2014) Immediately loaded platform switched implants in the anterior mandible with fixed prostheses: a randomized, split-mouth, masked prospective trial. Clin Implant Dent Relat Res 16:884–892
Mombelli A, van Oosten MA, Schurch E Jr, Land NP (1987) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 2:145–151
Loe H, Silness J (1963) Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand 21:533–551
Furhauser R, Florescu D, Benesch T, Haas R, Mailath G, Watzek G (2005) Evaluation of soft tissue around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res 16:639–644
Chiu YW, Lee SY, Lin YC, Lai YL (2015) Significance of the width of keratinized mucosa on peri-implant health. J Chinese Med Assoc 78:389–394
Schwarz F, Mihatovic I, Becker J, Bormann KH, Keeve PL, Friedmann A (2013) Histological evaluation of different abutments in the posterior maxilla and mandible: an experimental study in humans. J Clin Periodontol 40:807–815
Cochran DL, Mau LP, Higginbottom FL, Wilson TG, Bosshardt DD, Schoolfield J, Jones AA (2013) Soft and hard tissue histologic dimensions around dental implants in the canine restored with smaller-diameter abutments: a paradigm shift in peri-implant biology. Int J Oral Maxillofac Implants 28:494–502
Romanos GE, Toh CG, Siar CH, Swaminathan D (2002) Histologic and histomorphometric evaluation of peri-implant bone subjected to immediate loading: an experimental study in Macaca fascicularis. Int J Oral Maxillofac Implants 17:44–51
Sculean A, Gruber R, Bosshardt DD (2014) Soft tissue wound healing around teeth and dental implants. J Clin Periodontol 41:6–22
Kumar M, Shanavas M, Sidappa A, Kiran M (2015) Cone beam computed tomography—know its secrets. J Int Oral Health 7:64–68
de Faria VK, Evangelista KM, Rodrigues CD, Estrela C, de Sousa TO, Silva MA (2012) Detection of periodontal bone loss using cone beam CT and intraoral radiography. Dentomaxillofac Radiol 41:64–69
Veltri M, Ekestubbe A, Abrahamasson I, Wennström JL (2015) Three-dimensional buccal bone anatomy and aesthetic outcome of single dental implants replacing maxillary incisors. Clin Oral Impl Res doi: 10.1111/clr.12664. [Epub ahead of print,1–9]
Hashimoto M, Akagawa Y, Nikai H, Tsuru H (1989) Ultrastructure of the peri-implant junctional epithelium on single-crystal sapphire endosseous dental implant loaded with functional stress. J Oral Rehabil 16:261–270
Tomasi C, Tessarolo F, Caola I, Wennstrom J, Nollo G, Berglundh T (2014) Morphogenesis of peri-implant mucosa revisited: an experimental study in humans. Clin Oral Imp Res 25:997–1003
Schwarz F, Ferrari D, Herten M, Mihatovic I, Wieland M, Sager M, Becker J (2007) Effects of surface hydrophilicity and microtopography on early stages of soft and hard tissue integration at non-submerged titanium implants: an immunohistochemical study in dogs. J Periodontol 78:2171–2184
Hermann JS, Buser D, Schenk RK, Higginbottom FL, Cochran DL (2000) Biologic width around titanium implants. A physiologically formed and stable dimension over time. Clin Oral Imp Res 11:1–11
Grunder U, Gracis S, Capelli M (2005) Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodont Restor Dent 25:113–119
Rodriguez X, Vela X, Mendez V, Segala M, Calvo-Guirado JL, Tarnow DP (2013) The effect of abutment dis/reconnections on periimplant bone resorption: a radiologic study of platform-switched and non-platform-switched implants placed in animals. Clin Oral Imp Res 24:305–311
Abrahamsson I, Berglundh T, Lindhe J (1997) The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 24:568–572
Albrektsson T, Zarb G, Worthington P, Eriksson AR (1986) The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral & Maxillofac Implants 1:11–25
Forster A, Ungvari K, Györgyey A, Kukovecz A, Turzo K, Nagy K (2014) Human epithelial tissue culture study on restorative materials. J Dent 42:7–14
Busscher HJ, Rinastiti M, Siswomihardjo W, van der Mei HC (2010) Biofilm formation on dental restorative and implant materials. J Dent Res 89:657–665
Ertürk BK, Çömlekoğlu ME, Çömlekoğlu MD, Aladağ A, Güngör MA (2015) A customized zirconia abutment design combined with a CAD/CAM laminate veneer: a clinical report. Int J Periodont Rest Dent 35:201–209
Belser UC, Grütter L, Vailati F, Bornstein MM, Weber HP, Buser D (2009) Outcome evaluation of early placed maxillary anterior single-tooth implants using objective esthetic criteria: a cross-sectional, retrospective study in 45 patients with a 2- to 4-year follow-up using pink and white esthetic scores. J Periodontol 80:140–151
Cabello G, Rioboo M, Fábrega JG (2013) Immediate placement and restoration of implants in the aesthetic zone with a tri-modal approach: soft tissue alterations and its relation to gingival biotype. Clin Oral Implants Res 24:1094–1100
Patil R, den Hartog L, Dilbaghi A, de Jong B, Kerdijk W, Cune MS (2015) Papillary fill response in single-tooth implants using abutments of different geometry. Clin Oral Implants Res doi. doi:10.1111/clr.12594 [Epub ahead of print]
Acknowledgments
This clinical study has been supported by the Camlog Foundation (Project no: CF41104) and the authors would like to thank the scientific board of Camlog Foundation, Prof. Jürgen Becker, Dr. Alex Schar and Francoise Peters, for generous material supply and financial support as well as IvoclarVivadent for supplying ceramic abutment blocks and luting materials for the study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This research involved human participants whose informed consents were also taken.
Conflict of interest
Author M. Erhan Çömlekoğlu has received a research grant from Camlog Foundation. Authors M. Erhan Çömlekoğlu, Mine Dündar Çömlekoğlu and Nejat Nizam declare that they have no conflict of interest.
Funding
This study was funded by the Camlog Foundation (Funding no: CF41104).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (Ethical Committee of Ege University (Number: 12-3.1/16; date 20 April 2012)) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Erhan Çömlekoğlu, M..., Nizam, N. & Çömlekoğlu, M.D. Immediate definitive individualized abutments reduce peri-implant bone loss: a randomized controlled split-mouth study on 16 patients. Clin Oral Invest 22, 475–486 (2018). https://doi.org/10.1007/s00784-017-2136-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-017-2136-9