Abstract
Objectives
This investigation was designed to compare the effectiveness of enamel matrix derivative (EMD) proteins in combination with flapless or flap procedure in periodontal regeneration of deep intrabony defects.
Materials and methods
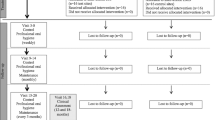
Thirty chronic periodontitis patients who had at least one residual periodontal defect with an intrabony component of ≥3 mm were consecutively enrolled. Defects were randomly assigned to test or control treatments which both consisted of the use of EMD to reach periodontal regeneration. Test sites (n = 15) were treated according to a novel flapless approach, whereas control sites (n = 15) by means of minimally invasive surgery (MIST). Clinical and radiographic parameters were recorded at baseline, 12 and 24 months post-operatively.
Results
Both therapeutic modalities yielded similar probing depth (PD) reduction and clinical attachment level (CAL) gain at 24 months. In flapless-treated sites, a mean PD reduction of 3.6 ± 1.0 mm and a CAL gain of 3.2 ± 1.1 mm were observed. In the MIST group, they were 3.7 ± 0.6 and 3.6 ± 0.9 mm. The operative chair time was twice as long in the MIST compared to the flapless group, whereas comparable patient-oriented outcomes were observed.
Conclusion
The flapless procedure may be successfully applied in the regenerative treatment of deep intrabony defects reaching clinical outcomes comparable with those of minimally invasive surgical approaches and may present important advantages in terms of reduction of operative chair time.
Clinical relevance
The use of EMD as an adjunct to non-surgical periodontal treatment may be considered a suitable option to treat defects mainly in the anterior sextants.



Similar content being viewed by others
References
Giannobile WV, Somerman MJ (2003) Growth and amelogenin-like factors in periodontal wound healing. A systematic review. Ann Periodontol 8:193–204
Bosshardt DD (2008) Biological mediators and periodontal regeneration: a review of enamel matrix proteins at the cellular and molecular levels. J Clin Periodontol 35(Suppl. 8):87–105
Venezia E, Goldstein M, Boyan BD, Schwartz Z (2004) The use of enamel matrix derivative in the treatment of periodontal defects: a literature review and meta-analysis. Crit Rev Oral Biol Med 15:382–402
Esposito M, Grusovin MG, Papanikolau N, Coulthard P, Worthington HV (2009) Enamel matrix derivative (Emdogain®) for periodontal tissue regeneration in intrabony defects. Cochrane Database Syst Rev 4:CD003875
Koop R, Merheb J, Quirynen M (2012) Periodontal regeneration with enamel matrix derivative in reconstructive periodontal therapy: a systematic review. J Periodontol 83:707–720
Hammarström L, Heijl L, Gestrelius S (1997) Periodontal regeneration in a buccal dehiscence model in monkeys after application of enamel matrix proteins. J Clin Periodontol 24:669–677
Heijl L (1997) Periodontal regeneration with enamel matrix derivative in one human experimental defect. A Case Report J Clin Periodontol 24:693–696
Mellonig JT (1999) Enamel matrix derivative for periodontal reconstructive surgery: technique and clinical and histologic case report. Int J Periodontics Restorative Dent 19:8–19
Yukna RA, Mellonig J (2000) Histologic evaluation of periodontal healing in humans following regenerative therapy with enamel matrix derivative. A 10-case series. J Periodontol 71:752–759
Sculean A, Chiantella GC, Windisch P, Donos N (2000) Clinical and histologic evaluation of treatment of intrabony defects with an enamel matrix protein derivative (Emdogain). Int J Periodontics Restorative Dent 20:374–381
Cortellini P, Tonetti MS (2009) Improved wound stability with a modified minimally invasive surgical technique in the regenerative treatment of isolated interdental intrabony defects. J Clin Periodontol 36:157–163
Sculean A, Alessandri R, Miron RJ, Salvi G, Bosshard DD (2011) Enamel matrix proteins and periodontal wound healing and regeneration. Clin Adv Periodontics 1:101–117
Wikesjö UM, Nilvéus RE (1990) Periodontal repair in dogs: effect of wound stabilization on healing. J Periodontol 61:719–724
Tonetti MS, Prato GP, Cortellini P (1996) Factors affecting the healing response of intrabony defects following guided tissue regeneration and access flap surgery. J Clin Periodontol 23:548–556
Ramseier CA, Rasperini G, Batia S, Giannobile WV (2012) advanced reconstructive technologies for periodontal tissue repair. Periodontol2000 59:185–202
Wikesjö UM, Nilvéus RE, Selvig KA (1992) Significance of early wound healing on periodontal repair: a review. J Periodontol 63:158–165
Haney JM, Nilvéus RE, McMillan PJ, Wikesjö UM (1993) Periodontal repair in dogs: expanded polytetrafluoroethylene barrier membranes support wound stabilization and enhance bone regeneration. J Periodontol 64:883–890
Francetti L, Del Fabbro M, Basso M, Testori T, Wienstein R (2004) Enamel matrix proteins in the treatment of intrabony defects. A prospective 24-month clinical trial. J Clin Periodontol 31:52–59
Harrel SK, Wilson TG Jr, Nunn ME (2005) Prospective assessment of the use of enamel matrix proteins with minimally invasive surgery. J Periodontol 76:380–384
Cortellini P, Tonetti MS (2007) Minimally invasive surgical technique (MIST) and enamel matrix derivative (EMD) in intrabony defects. (I) Clinical outcomes and morbidity. J Clin Periodontol 34:1082–1088
Cortellini P, Pini-Prato G, Nieri M, Tonetti MS (2009) Minimally invasive surgical technique and enamel matrix derivative (EMD) in intrabony defects: 2. Factors associated with healing outcomes. Int J Periodontics Restorative Dent 29:257–265
Farina R, Simonelli A, Minenna L, Rasperini G, Trombelli L (2014) Single-flap approach in combination with enamel matrix derivative in the treatment of periodontal intraosseus defects. Int J Periodontics Restorative Dent 34:497–506
Rethman MP, Harrel SK (2010) Minimally invasive periodontal therapy: will periodontal therapy remain a technologic laggard? J Periodontol 81:1390–1395
Ribeiro FV, Casarin RCV, Palma MAG, Júnior FHN, Sallum EA, Casati MZ (2011) Clinical and patient-centered outcomes after minimally invasive non-surgical or surgical approaches for the treatment of intrabony defects: a randomized clinical trial. J Periodontol 82:1256–1266
Mellonig JT, Valderrama P, Gregory HJ, Cochran DL (2009) Clinical and histologic evaluation of non-surgical periodontal therapy with enamel matrix derivative: a report of four cases. J Periodontol 80:1534–1540
Armitage GC (1999) Development of a classification system for periodontal diseases and conditions. Ann Periodontol 4:1–6
Trombelli L, Farina R, Franceschetti G, Calura G (2009) Single-flap approach with buccal access in periodontal reconstructive procedures. J Periodontol 80:353–360
Aimetti M, Mariani GM, Ferrarotti F, Ercoli E, Audagna M, Bignardi C, Romano F (2015) Osseous resective surgery with and without fibre retention technique in the treatment of shallow intrabony defects: a split-mouth randomized clinical trial. J Clin Periodontol 42:182–189
Schei O, Waerhaug J, Lovdal A, Arro A (1959) Alveolar bone loss as related to oral hygiene and age. J Periodontol 30:7–16
Tonetti MS, Fourmousis I, Suvan J, Cortellini P, Bragger U, Lang NP, European Research Group on Periodontology (ERGOPERIO) (2004) Healing, post-operative morbidity and patient perception of outcomes following regenerative therapy of deep intrabony defects. J Clin Periodontol 31:1092–1098
Harrel SK, Wilson TG Jr, Nunn ME (2010) Prospective assessment of the use of enamel matrix derivative with minimally invasive surgery: 6-year results. J Periodontol 81:435–441
Heitz-Mayfield LJ, Trombelli L, Heitz F, Needleman I, Moles D (2002) A systematic review of the effect of surgical debridement vs non-surgical debridement for the treatment of chronic periodontitis. J Clin Periodontol 29(Suppl. 3):92–102
Heitz-Mayfield LJ (2005) How effective is surgical therapy compared with nonsurgical debridement? Periodontol 2000(37):72–87
Heijl L, Heden G, Svärdström G, Ostgren A (1997) Enamel matrix derivative (Emdogain) in the treatment of intrabony periodontal defects. J Clin Periodontol 24:705–714
Gutierrez MA, Mellonig JT, Cochran DL (2003) Evaluation of enamel matrix derivative as an adjunct to non-surgical periodontal therapy. J Clin Periodontol 30:739–745
Sculean A, Windisch P, Keglevich T, Gera I (2003) Histologic evaluation of human intrabony defects following non-surgical periodontal therapy with and without application of an enamel matrix protein derivative. J Periodontol 74:153–160
Mombelli A, Brochut P, Plagnat D, Casagni F, Giannopoulou C (2005) Enamel matrix proteins and systemic antibiotics as adjuncts to non-surgical periodontal treatment: clinical effects. J Clin Periodontol 32:225–230
Rabbani GM, Ash MM, Caffesse RG (1981) The effectiveness of sub-gingival scaling and root planing in calculus removal. J Periodontol 52:119–123
Adriaens PA, LM A (2004) Effects of nonsurgical periodontal therapy on hard and soft tissues. Periodontol 2000 36:121–145
Wylam JM, Mealey BL, Mills MP, Waldrop TC, Moskowicz DC (1993) The clinical effectiveness of open versus closed scaling and root planing on multirooted teeth. J Periodontol 64:1023–1028
Sherman PR, Hutchens LH Jr, Jewson LG, Moriarty JM, Greco GW, McFall WT Jr (1990) The effectiveness of subgingival scaling and root planing. I Clinical Detection of Residual Calculus J Periodontol 61:3–8
Brayer WK, Mellonig JT, Dunlap RM, Marinak KW, Carson RE (1989) Scaling and root planing effectiveness: the effect of root surface access and operator experience. J Periodontol 60:67–72
Fleischer HC, Mellonig JT, Brayer WK, Gray JL, Barnett JD (1989) Scaling and root planing efficiency in multirooted teeth. J Periodontol 60:402–409
Nibali L, Pometti D, Chen T-T, Tu Y-K (2015) Minimally invasive non surgical approach for the treatment of periodontal intrabony defects: a retrospective analysis. J Clin Periodontol 42:853–859
Cortellini P (2012) Minimally invasive surgical techniques in periodontal regeneration. J Evid Based Dent Pract 12(Suppl. 3):89–100
Jepsen S, Topoll H, Rengers H, Heinz B, Teich M, Hoffmann T, Al-Machot E, Meyle J, Jervoe-Storm PM (2008) Clinical outcomes after treatment of intrabony defects with an EMD/synthetic bone graft or EMD alone: a multicentre randomized-controlled clinical trial. J Clin Periodontol 35:420–428
Harrell SK, Wilson TG Jr, Nunn ME (2010) Prospective assessment of the use of enamel matrix derivative with minimally invasive surgery: a 6-year results. J Periodontol 81:435–441
Ribeiro FV, Casarin RCV, Jùnior FHN, Sallum EA, Casati MZ (2011) The role of enamel matrix derivative protein in minimally invasive surgery in treating intrabony defects in single-rooted: a randomized clinical trial. J Periodontol 82:522–532
Cortellini P, Tonetti MS (2011) Clinical and radiographic outcomes of the modified minimally invasive surgical technique with and without regenerative materials: a randomized-controlled trial in intrabony defects. J Clin Periodontol 38:365–373
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures involving humans were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
The authors declare that there were no financial supports from any external source regarding the current study.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Aimetti, M., Ferrarotti, F., Mariani, G.M. et al. A novel flapless approach versus minimally invasive surgery in periodontal regeneration with enamel matrix derivative proteins: a 24-month randomized controlled clinical trial. Clin Oral Invest 21, 327–337 (2017). https://doi.org/10.1007/s00784-016-1795-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-016-1795-2