Abstract
Introduction
Osteoporosis is a major health issue in boys with Duchenne muscular dystrophy (DMD). Data on the specific bone deficits and microarchitectural alterations in children with DMD were limited. This study aimed to assess the bone microarchitectural alterations in boys with DMD on long-term glucocorticoid using high-resolution peripheral quantitative computed tomography (HR-pQCT).
Materials and methods
This was a cross-sectional, case–control study. Boys with DMD older than 5 years with no prior history of symptomatic fracture and had been on long-term glucocorticoid treatment were recruited from a single tertiary centre. For each participant, three gender- and age-matched controls were selected randomly from an existing HR-pQCT database of healthy individuals.
Results
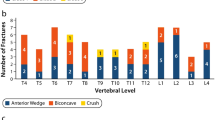
Nine boys with DMD at a median age of 9.3 years were included. Three were found to have asymptomatic vertebral compression fracture. The HR-pQCT findings of these nine boys were compared with 27 healthy controls. Trabecular microstructure indices at the distal radius were significantly lower but the cortical vBMD was significantly higher in the DMD boys when compared with healthy controls.
Conclusion
Lower microarchitectural measurement of trabecular bones, but higher cortical vBMD, was observed in DMD boys on long-term oral glucocorticoid. The results from this study provide preliminary, yet important insights into the bone microarchitecture of this group of patients.

Similar content being viewed by others
References
Bushby K, Finkel R, Birnkrant DJ et al (2010) Diagnosis and management of Duchenne muscular dystrophy, part 1: diagnosis, and pharmacological and psychosocial management. Lancet Neurol 9:77–93. https://doi.org/10.1016/S1474-4422(09)70271-6
Tian C, Wong BL, Hornung L et al (2016) Bone health measures in glucocorticoid-treated ambulatory boys with Duchenne muscular dystrophy. Neuromuscul Disord 26:760–767. https://doi.org/10.1016/j.nmd.2016.08.011
Buckner JL, Bowden SA, Mahan JD (2015) Optimizing bone health in Duchenne muscular dystrophy. Int J Endocrinol 2015:928385. https://doi.org/10.1155/2015/928385
Talim B, Malaguti C, Gnudi S et al (2002) Vertebral compression in Duchenne muscular dystrophy following deflazacort. Neuromuscul Disord 12:294–295
Houde S, Filiatrault M, Fournier A et al (2008) Deflazacort use in Duchenne muscular dystrophy: an 8-year follow-up. Pediatr Neurol 38:200–206. https://doi.org/10.1016/j.pediatrneurol.2007.11.001
McAdam LC, Rastogi A, Macleod K, Douglas Biggar W (2012) Fat embolism syndrome following minor trauma in Duchenne muscular dystrophy. Neuromuscul Disord 22:1035–1039. https://doi.org/10.1016/j.nmd.2012.07.010
Bell JM, Shields MD, Watters J et al (2017) Interventions to prevent and treat corticosteroid-induced osteoporosis and prevent osteoporotic fractures in Duchenne muscular dystrophy. Cochrane Database Syst Rev 1:CD010899. https://doi.org/10.1002/14651858.CD010899.pub2
Crabtree NJ, Arabi A, Bachrach LK et al (2014) Dual-energy X-ray absorptiometry interpretation and reporting in children and adolescents: the revised 2013 ISCD Pediatric Official Positions. J Clin Densitom 17:225–242. https://doi.org/10.1016/j.jocd.2014.01.003
Tung JY, Chan SH (2017) Bone health among boys with Duchenne muscular dystrophy after initiation of glucocorticoids. Doi: https://doi.org/10.1530/boneabs.6.LB17
Neu CM, Manz F, Rauch F et al (2001) Bone densities and bone size at the distal radius in healthy children and adolescents: a study using peripheral quantitative computed tomography. Bone 28:227–232
Digby MG, Bishop NJ, Paggiosi MA, Offiah AC (2016) HR-pQCT: a non-invasive “biopsy” to assess bone structure and strength. Arch Dis Child Educ Pract Ed 101:268–270. https://doi.org/10.1136/archdischild-2015-309455
Bala Y, Bui QM, Wang X-F et al (2015) Trabecular and cortical microstructure and fragility of the distal radius in women. J Bone Miner Res 30:621–629. https://doi.org/10.1002/jbmr.2388
Zemel BS, Kalkwarf HJ, Gilsanz V et al (2011) Revised reference curves for bone mineral content and areal bone mineral density according to age and sex for black and non-black children: results of the bone mineral density in childhood study. J Clin Endocrinol Metab 96:3160–3169. https://doi.org/10.1210/jc.2011-1111
Genant HK, Wu CY, van Kuijk C, Nevitt MC (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8:1137–1148. https://doi.org/10.1002/jbmr.5650080915
Wetzsteon RJ, Shults J, Zemel BS et al (2009) Divergent effects of glucocorticoids on cortical and trabecular compartment BMD in childhood nephrotic syndrome. J Bone Miner Res 24:503–513. https://doi.org/10.1359/jbmr.081101
Bm M, P R, Hj M, et al (2016) Histomorphometry and Bone Matrix Mineralization Before and After Bisphosphonate Treatment in Boys With Duchenne Muscular Dystrophy: A Paired Transiliac Biopsy Study. In: Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. https://pubmed.ncbi.nlm.nih.gov/26615086/. Accessed 31 May 2020
Tsampalieros A, Gupta P, Denburg MR et al (2013) Glucocorticoid effects on changes in bone mineral density and cortical structure in childhood nephrotic syndrome. J Bone Miner Res 28:480–488. https://doi.org/10.1002/jbmr.1785
Shen J, Griffith JF, Zhu TY et al (2018) Bone mass, microstructure, and strength can discriminate vertebral fracture in patients on long-term steroid treatment. J Clin Endocrinol Metab 103:3340–3349. https://doi.org/10.1210/jc.2018-00490
Acknowledgements
The authors would like to thank all the patients and families for participating in this study.
Author information
Authors and Affiliations
Contributions
JYT contributed in study design, recruitment of subjects, data analysis and manuscript preparation. SHC contributed to the study design, recruitment of subjects and interpretations of data. TPL contributed to the HR-pQCT scanning protocols and interpretations of DXA and HR-pQCT findings. All authors contributed to interpretation of findings and critically revised the manuscript and approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Tung, J.Yl., Lam, Tp. & Chan, S.Hs. Bone microarchitectural alterations in boys with Duchenne muscular dystrophy on long-term glucocorticoid treatment. J Bone Miner Metab 39, 606–611 (2021). https://doi.org/10.1007/s00774-020-01196-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-020-01196-w