Abstract
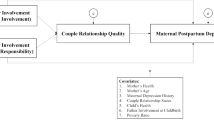
This mixed-methods research study aimed to assess the contribution of interparental relationship quality and paternal support for mothers to maternal mental health among Black parents in a metro area characterized by severe racial disparities. We also explored Black parents’ understanding of meaningful paternal support for mothers. Using survey data collected from Black mothers (N = 75), we examined correlations among the study variables, then conducted mediation and moderation analyses to examine whether relationship quality would mediate the association between paternal support and maternal mental health and to test whether relationship quality would moderate the association between paternal support and maternal self-reported overall health. We used inductive thematic analysis to analyze data from focus groups with Black parents (N = 15). We found that mothers’ mental health was positively correlated with relationship quality, mothers’ subjective health was positively correlated with paternal support, and relationship quality significantly mediates the relationship between paternal support and maternal mental health while controlling for relationship status. Our thematic analysis yielded four themes to characterize meaningful paternal support for mothers and a high quality interparental relationship: (1) Teammates; (2) Multidimensional, everyday support; (3) Communication is key; and (4) Challenge racism and disrupt intergenerational trauma. Findings suggest that paternal support and interparental relationship quality can play a protective role, promoting maternal mental health and wellbeing. Providers of perinatal services should support Black parents to support one another, including as advocates in confronting racism.

Similar content being viewed by others
Data Availability
Due to privacy and ethical concerns, supporting data cannot be made openly available. Further information about the data is available from the authors upon request.
Change history
05 May 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00737-023-01323-2
References
Alio AP, Lewis CA, Scarborough K et al (2013) A community perspective on the role of fathers during pregnancy: a qualitative study. BMC Pregnancy Childbirth 13:60. https://doi.org/10.1186/1471-2393-13-60
Artiga S, Pham O, Ranji U (2020) Racial disparities in Maternal and infant health: an overview. Kaiser Family Foundation. Kaiser Family Foundation https://www.kff.org/report-section/racial-disparities-in-maternal-and-infant-health-an-overview-issue-brief/. Accessed 26 January 2022
Cabrera NJ, Fagan J, Farrie D (2008) Explaining the long reach of fathers’ prenatal involvement on later paternal engagement. J Marriage Fam 70(5):1094. https://doi.org/10.1111/j.1741-3737.2008.00551.x
Caldwell CH, Misra DP, Rogers WB et al (2018) Interpersonal relationships among Black couples and depressive symptoms during pregnancy. MCN Am J Matern Child Nurs 43(5):265–270. https://doi.org/10.1097/NMC.0000000000000460
Coles RL, Green C (Eds.) (2010) The myth of the Missing Black father. Columbia University Press, NYC. http://www.jstor.org/stable/https://doi.org/10.7312/cole14370
Corbin J, Strauss A (2008) Basics of qualitative research: techniques and procedures for developing grounded theory, 3rd edn. Sage, Thousand Oaks, CA
Crear-Perry J, Correa-de-Araujo R, Johnson TL et al (2021) J Women’s Health 2:230–235
Declerq ER, Sakala C, Corry MP et al (2013). Listening to mother III: new mothers speak out-report of the national survey of women’s childbearing experiences conducted October -December 2012 and January-April 2013.
Downs, K. (2015, Mar. 5). Why is Milwaukee so bad for Black people? [Radio broadcast]. National Public Radio. https://www.npr.org/sections/codeswitch/2015/03/05/390723644/why-is-milwaukee-so-bad-for-black-people
Eboh RN, Giurgescu C, Misra DP (2018) Relationship with the father of the baby and perceived stress among Black women. MCN Am J Matern Child Nurs 43(5):259–264. https://doi.org/10.1097/NMC.0000000000000459
Elliott R, Fischer CT, Rennie DL (1999) Evolving guidelines for publication of qualitative research studies in psychology and related fields. Br J Clin Psychol 38(3):215–229
Garfield CF (2015) Supporting fatherhood before and after it happens. Pediatrics 135(2):e528–e530. https://doi.org/10.1542/peds.2014-3747
Garfield CF, Isacco A (2009) Urban fathers’ role in maternal postpartum mental health. Fathering: A J Theory Res Practice about Men as Fathers 7:286–302. https://doi.org/10.3149/fth.0703.286
Ghosh JKC, Wilhelm MH, Dunkel-Schetter C et al (2010) Paternal support and preterm birth, and the moderation of effects of chronic stress: a study in Los Angeles County mothers. Archive of Women’s Mental Health 13:327–338. https://doi.org/10.1007/s00737-009-0135-9
Giurgescu C, Templin TN (2015) Father involvement and psychological well-being of pregnant women. MCN Am J Matern Child Nurs 40(6):381–387. https://doi.org/10.1097/NMC.0000000000000183
Giurgescu C, Zenk SN, Engeland CG et al (2017) Racial discrimination and psychological wellbeing of pregnant women. MCN Am J Matern Child Nurs 42(1):8–13. https://doi.org/10.1097/NMC.0000000000000297
Glazer KB, Howell EA (2021) A way forward in the maternal mortality crisis: addressing maternal health disparities and mental health. Archives of Women’s Mental Health 24:823–830. https://doi.org/10.1007/s00737-021-01161-0
Gondwe KW, White-Traut R, Brandon D et al (2017) The role of sociodemographic factors in maternal psychological distress and mother-preterm infant interactions. Res Nurs Health 40(6):528–540. https://doi.org/10.1002/nur.21816
Hohmann-Marriott B (2011) Coparenting and father involvement in married and unmarried coresident couples. J Marriage Fam 73(1):296–309. https://doi.org/10.1111/j.1741-3737.2010.00805.x
Hoyert LD (2021) Maternal mortality rates in the United States, 2019. National Center for Health Statistics. https://www.cdc.gov/nchs/data/hestat/maternal-mortality-2021/E-Stat-Maternal-Mortality-Rates-H.pdf. Accessed 26 January 2022
Jones J & Mosher WD (2013). Fathers’ involvement with their children: United States, 2006-2010 (National Health Statistics Reports No. 71). National Center for Health Statistics. https://www.cdc.gov/nchs/data/nhsr/nhsr071.pdf
Jonsdottir SS, Thome M, Steingrimsdottir T, Lydsdottir LB et al (2017) Partner relationship, social support and perinatal distress among pregnant Icelandic women. Women and Birth 30(1):e46–e55. https://doi.org/10.1016/j.wombi.2016.08.005
Julion WA, Sumo J, Bounds DT (2018) A tripartite model for recruiting African-Americans into fatherhood intervention research. Public Health Nurs 35(5):420–426. https://doi.org/10.1111/phn.12411
Kozhimannil KB, Trinacty CM, Busch AB et al (2011) Racial and ethnic disparities in postpartum depression care among low-income women. Psychiatric Service 62(6):619–625. https://doi.org/10.1176/ps.62.6.pss6206_0619
Kroenke K, Spitzer RL, Williams JB et al (2009) An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics 50(6):613–621
Lee SJ, Sanchez DT, Grogan-Kaylor A (2018) Father early engagement behaviors and infant low birth weight. Matern Child Health J 22(10):1407–1417. https://doi.org/10.1007/s10995-018-2521-2
Leech NL, Onwuegbuzie AJ (2008) Qualitative data analysis: a compendium of techniques and a framework for selection for school psychological research and beyond. Sch Psychol Q 23:587–604
Levine, MV (2020) The state of Black Milwaukee in national perspective: racial inequality in the Nation’s 50 largest metropolitan areas. Center for Economic Development Publications, 56. https://dc.uwm.edu/ced_pubs/56
Nelson JA, O’Brien M, Blankson AN, Calkins SD, Keane SP (2009) Family stress and parental responses to children’s negative emotions tests of the spillover, crossover, and compensatory hypotheses. J Fam Psych JFP J Division Fam Psych Am Psych Assoc (Division 43) 23(5):671–679
Nowak AL, Giurgescu C (2017) The built environment and birth outcomes: a systematic review. MCN Am J Matern Child Nurs 42(1):14–20. https://doi.org/10.1097/NMC.0000000000000299
Nowak AL, Giurgescu C, Templin TN et al (2020) How depressive symptoms among African American women relate to measures of social disorder in her childhood and pregnancy neighborhood. J Urban Health 97(1):26–36. https://doi.org/10.1007/s11524-019-00409-6
Rini C, Schetter CD, Hobel CJ et al (2006) Effective social support: antecedents and consequences of partner support during pregnancy. Pers Relat 13:207–229
Rosenthal L, Lobel M (2011) Explaining racial disparities in adverse birth outcomes: Unique sources of stress for Black American women. Soc Sci Med 72(6):977–983. https://doi.org/10.1016/j.socscimed.2011.01.013
Sealy-Jefferson S, Giurgescu C, Slaughter-Acey J et al (2016) Neighborhood context and preterm delivery among African American women: the mediating role of psychosocial factors. J Urban Health 93(6):984–996. https://doi.org/10.1007/s11524-016-0083-4
Sidebotton A, Vacquier M, LaRusso E et al (2021) Perinatal depression screening practices in a large health system: identifying current state and assessing opportunities to provide more equitable care. Arch Women’s Mental Health 24:133–144
Sobel ME (1982) Asymptotic confidence intervals for indirect effects in structural equation models. Sociol Methodol 13:290–312
Stapleton LR, Schetter CD, Westling E et al (2012) Perceived partner support in pregnancy predicts lower maternal and infant distress. J Fam Psychol 26(3):453–463. https://doi.org/10.1037/a0028332
Thomas DA (2006) A general inductive approach for analyzing qualitative evaluation data. Am J Eval 27(2):237–246. https://doi.org/10.1177/1098214005283748
Walsh TB, Tolman RM, Palladino CL et al (2014) Moving up the ‘magic moment’: Fathers’ experience of prenatal ultrasound. Fathering 12(1):18–37
Walsh TB, Carpenter E, Costanzo MA et al (2021) Present as a partner and a parent: mothers’ and fathers’ perspectives on father participation in prenatal care. Infant Ment Health J42(3):386–399. https://doi.org/10.1002/imhj.21920
Acknowledgements
The authors thank all of the participants in this research for their contribution, and thank research assistant Hassnaa Mohammed and the team at the African American Breastfeeding Network, in particular Brooks Griffin and Terron Edwards, for their support of the study.
Funding
Funding for this project was provided by the UW School of Medicine and Public Health from the Wisconsin Partnership Program through a grant to the UW Institute for Clinical and Translational Research. Research reported in this publication was supported in part by the Eunice Kennedy Shriver National Institute of Child Health & Human Development, the Office of Research on Women’s Health, Building Interdisciplinary Research Careers in Women’s Health (BIRCWH) program, the Office of The Director, National Institutes of Health and the National Cancer Institute, under Award Number K12HD055894. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised due to instance of blinded content.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Walsh, T.B., Thomas, A., Quince, H. et al. Black fathers’ contributions to maternal mental health. Arch Womens Ment Health 26, 117–126 (2023). https://doi.org/10.1007/s00737-022-01284-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-022-01284-y