Abstract
Introduction
The ventriculoperitoneal shunt is one of the most commonly performed neurosurgical procedures. One of the avoidable complications of shunt surgery is shunt infection. This PRISMA-compliant meta-analysis analysed the effectiveness of topical and/or intraventricular antibiotics in preventing shunt infections in patients undergoing shunt surgery.
Methods
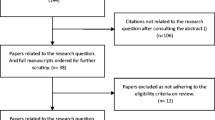
Four databases were searched from inception to 30th June 2021. Only original articles comparing the rate of shunt infection with and without antibiotics were included. Random-effects meta-analysis was used to compare the effect of the use of antibiotics in preventing infection and subgroup analysis for finding differences in various antibiotics.
Results
The rate of shunt infection was 2.24% (53 out of 2362) in the topical antibiotic group in comparison to 5.24% (145 out of 2764) in the control group (p = 0.008). Subgroup analysis revealed that there is no significant difference between the antibiotics used.
Conclusions
Our meta-analysis found that the risk of shunt infection is significantly reduced with the use of topical and intraventricular antibiotics without any serious adverse effect. No side effects of topical or intraventricular antibiotics were reported in the included studies. Further prospective studies are required to establish the safety and optimal dosage of topical antibiotics for them to be used routinely in neurosurgical practice. They can be used in patients at high risk of developing shunt infections till such studies are available.







Similar content being viewed by others
References
Kestle JRW, Holubkov R, Douglas Cochrane D et al (2016) A new Hydrocephalus Clinical Research Network protocol to reduce cerebrospinal fluid shunt infection. J Neurosurg Pediatr 17(4):391–396
Viechtbauer W (2010) Conducting meta-analyses in R with the metafor package. J Stat Softw 36(1):1–48
Govender ST, Nathoo N, van Dellen JR (2003) Evaluation of an antibiotic-impregnated shunt system for the treatment of hydrocephalus. J Neurosurg 99(5):831–839
Raygor KP, Oh T, Hwang JY, Phelps RRL, Ghoussaini K, Wong P, Silvers R, Ostling LR, Sun PP (2020) Ventriculoperitoneal shunt infection rates using a standard surgical technique, including topical and intraventricular vancomycin: the Children’s Hospital Oakland experience. J Neurosurg Pediatr 26:504–512. https://doi.org/10.3171/2020.4.PEDS209
Krause M, Mahr CV, Schob S, Nestler U, Wachowiak R (2019) Topical instillation of vancomycin lowers the rate of CSF shunt infections in children. Childs Nerv Syst 35(7):1155–1157
Attenello FJ, Garces-Ambrossi GL, Zaidi HA, Sciubba DM, Jallo GI (2010) Hospital costs associated with shunt infections in patients receiving antibiotic-impregnated shunt catheters versus standard shunt catheters. Neurosurgery 66(2):284–289; discussion 289
Lakomkin N, Hadjipanayis CG (2021) The role of prophylactic intraventricular antibiotics in reducing the incidence of infection and revision surgery in pediatric patients undergoing shunt placement. Neurosurgery 88(2):301–305
Isaacs AM, Riva-Cambrin J, Yavin D, Hockley A, Pringsheim TM, Jette N, Lethebe BC, Lowerison M, Dronyk J, Hamilton MG (2018) Age-specific global epidemiology of hydrocephalus: systematic review, metanalysis and global birth surveillance. PLoS ONE 13(10):e0204926
Konstantelias AA, Vardakas KZ, Polyzos KA, Tansarli GS, Falagas ME (2015) Antimicrobial-impregnated and -coated shunt catheters for prevention of infections in patients with hydrocephalus: a systematic review and meta-analysis. J Neurosurg 122(5):1096–1112
Yakut N, Soysal A, Kadayifci EK et al (2018) Ventriculoperitoneal shunt infections and re-infections in children: a multicentre retrospective study. Br J Neurosurg 32(2):196–200
Rozzelle CJ, Leonardo J, Li V (2008) Antimicrobial suture wound closure for cerebrospinal fluid shunt surgery: a prospective, double-blinded, randomized controlled trial. J Neurosurg Pediatr 2(2):111–117
Arts SH, Boogaarts HD, van Lindert EJ (2019) Route of antibiotic prophylaxis for prevention of cerebrospinal fluid-shunt infection. Cochrane Database Syst Rev 6:CD012902
Ragel BT, Schmidt RH (2006) Surgical shunt infection: significant reduction when using intraventricular and systemic antibiotic agents. J Neurosurg 105:6
Mallucci CL, Jenkinson MD, Conroy EJ et al (2019) Antibiotic or silver versus standard ventriculoperitoneal shunts (BASICS): a multicentre, single-blinded, randomised trial and economic evaluation. Lancet Lond Engl 394(10208):1530–1539
van Lindert EJ, van Bilsen M, van der Flier M, Kolwijck E, Delye H, ten Oever J (2018) Topical vancomycin reduces the cerebrospinal fluid shunt infection rate: a retrospective cohort study. PLoS ONE 13(1):e0190249
Ng K, Mabasa VH, Chow I, Ensom MHH (2014) Systematic review of efficacy, pharmacokinetics, and administration of intraventricular vancomycin in adults. Neurocrit Care 20(1):158–171
Simon TD, Hall M, Riva-Cambrin J, Albert JE, Jeffries HE, Lafleur B, Dean JM, Kestle JRW, Hydrocephalus Clinical Research Network (2009) Infection rates following initial cerebrospinal fluid shunt placement across pediatric hospitals in the United States. Clinical article J Neurosurg Pediatr 4(2):156–165
Higgins JPT, Savovic J, Page M, Elbers R, Sterne J. Chapter 8: Assessing risk of bias in a randomized trial. In: Cochrane Handbook for Systematic Reviews of Interventions version 62 (updated February 2021) [Internet]. Cochrane, 2021; [cited 2021 Dec 8]. Available from: https://training.cochrane.org/handbook/current/chapter-08
Theophilius CS, Siregar J (2011) A randomised control trial on the use of topical methicillin in reducing post- operative ventriculoperitoneal shunt infection. Malays J Med Sci 18(1):30–37
Harrer M, Cuijpers P, FT A, Ebert DD (2021) Doing meta-analysis with R: a hands-on guide, 1st edn. Chapman & Hall/CRC Press, Boca Raton, FL and London
Bullock R, van Dellen JR, Ketelbey W, Reinach SG (1988) A double-blind placebo-controlled trial of perioperative prophylactic antibiotics for elective neurosurgery. J Neurosurg 69(5):687–691
Casey ATH, Kimmings EJ, Kleinlugtebeld AD, Taylor WaS, Harkness WF, Hayward RD (1997) The long-term outlook for hydrocephalus in childhood. Pediatr Neurosurg 27(2):63–70
Goda R, Ganesh kumar A, Katiyar V, Sharma R, Gurjar HK, Chaturvedi A, Sahu R, Rai HIS, Vora Z (2021) Efficacy of antimicrobial medicated ventricular catheters: a network meta-analysis with trial sequential analysis. Neurosurg Rev. https://doi.org/10.1007/s10143-021-01532-2
Beckman JM, Amankwah EK, Tetreault LL, Tuite GF (2015) Reduction in CSF shunt infection over a 10-year period associated with the application of concentrated topical antibiotic powder directly to surgical wounds prior to closure. J Neurosurg Pediatr 16(6):648–661
Moussa WMM, Mohamed MAA (2016) Efficacy of postoperative antibiotic injection in and around ventriculoperitoneal shunt in reduction of shunt infection: a randomized controlled trial. Clin Neurol Neurosurg 143:144–149
Kalangu KKN, Esene IN, Dzowa M, Musara A, Ntalaja J, Badra AK (2020) Towards zero infection for ventriculoperitoneal shunt insertion in resource-limited settings: a multicenter prospective cohort study. Childs Nerv Syst 36(2):401–409
Piatt JH, Garton HJL (2008) Clinical diagnosis of ventriculoperitoneal shunt failure among children with hydrocephalus. Pediatr Emerg Care 24(4):201–210
Drake JM, Kestle JR, Milner R et al (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43(2):294–303; discussion 303–305
Stoodley P, Braxton EE, Nistico L, Hall-Stoodley L, Johnson S, Quigley M, Post JC, Ehrlich GD, Kathju S (2010) Direct demonstration of staphylococcus biofilm in an external ventricular drain in a patient with a history of recurrent ventriculoperitoneal shunt failure. Pediatr Neurosurg 46(2):127–132
Zhang Q, Chen H, Zhu C, Chen F, Sun S, Liang N, Zheng W (2019) Efficacy and safety of intrathecal meropenem and vancomycin in the treatment of postoperative intracranial infection in patients with severe traumatic brain injury. Exp Ther Med 17(6):4605–4609
Author information
Authors and Affiliations
Contributions
Dr Ganesh VL—data collection, writing manuscript, approved final draft. Dr Kanwaljeet Garg—conceptualization, data collection, analysis, writing manuscript, approved final draft. Dr Vivek Tandon—approved final draft, supervision. Dr Sachin A Borkar—approved final draft, supervision. Prof GD Satyarthi—approved final draft, supervision. Prof Manmohan Singh—approved final draft, supervision. Prof P S Chandra—approved final draft, supervision. Prof S S Kale—approved final draft, supervision.
Corresponding author
Ethics declarations
Ethics approval
Not required as patient data was not used.
Consent to participate
Patient consent was taken.
Consent for publication
Patient consent for publication was taken.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
No portion of the contents of this paper has not been presented or published previously.
This article is part of the Topical Collection on Infection
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
VL, G., Garg, K., Tandon, V. et al. Effect of topical and intraventricular antibiotics used during ventriculoperitoneal shunt insertion on the rate of shunt infection—a meta-analysis. Acta Neurochir 164, 1793–1803 (2022). https://doi.org/10.1007/s00701-022-05248-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05248-0