Abstract
Background
Hemangioblastomas (HGBs) are highly vascular benign tumors, commonly located in the posterior fossa, and 80% of them are sporadic. Patients usually present with features of raised intracranial pressure and cerebellar symptoms. HGB can be classified as either mostly cystic or solids. Although the solid component is highly vascularized, aneurysm or hemorrhagic presentation is rarely described, having catastrophic results.
Methods
We identified 32 consecutive patients with posterior fossa HBG who underwent surgery from 2008 through 2020 at our medical center. Tumors were classified as predominantly cystic or solid according to radiological features. Resection was defined as gross total (GTR) or subtotal (STR).
Results
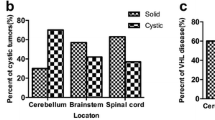
During the study period, 32 posterior fossa HGBs were resected. There were 26 cerebellar lesions and 4 medullar lesions, and in 2 patients, both structures were affected. Predominant cystic tumors were seen in 15 patients and solids in 17. Preoperative digital subtraction angiography (DSA) was performed in 8 patients with solid tumors, and 4 showed tumor-related aneurysms. Embolization of the tumors was performed in 6 patients, including the four tumor-related aneurysms. GTR was achieved in 29 tumors (91%), and subtotal resection in 3 (9%). Three patients had postoperative lower cranial nerve palsy. Functional status was stable in 5 patients (16%), improved in 24 (75%), and 3 patients (9%) deteriorated. One patient died 2 months after the surgery. Two tumors recurred and underwent a second surgery achieving GTR. The mean follow-up was 42.7 months (SD ± 51.0 months).
Conclusions
Predominant cystic HGB is usually easily treated as the surgery is straightforward. Those with a solid predominance present a more complex challenge sharing features similar to arteriovenous malformations. Given the important vascular association of solid predominance HGB with these added risk factors, the preoperative assessment should include DSA, as in arteriovenous malformations, and endovascular intervention should be considered before surgery.





Similar content being viewed by others
References
Ampie L, Choy W, Lamano JB, Kesavabhotla K, Kaur R, Parsa AT, Bloch O (2016) Safety and outcomes of preoperative embolization of intracranial hemangioblastomas: a systematic review. Clin Neurol Neurosurg 150:143–151. https://doi.org/10.1016/j.clineuro.2016.09.008
Cunha e Sa MJ, Stein BM, Solomon RA, McCormick PC (1992) The treatment of associated intracranial aneurysms and arteriovenous malformations. J Neurosurg 77:853–859. https://doi.org/10.3171/jns.1992.77.6.0853
Gao E, Young WL, Pile-Spellman J, Joshi S, Duong H, Stieg PE, Ma Q (1997) Cerebral arteriovenous malformation feeding artery aneurysms: a theoretical model of intravascular pressure changes after treatment. Neurosurgery 41:1345–1356; discussion 1356-1348. https://doi.org/10.1097/00006123-199712000-00020
Glasker S, Van Velthoven V (2005) Risk of hemorrhage in hemangioblastomas of the central nervous system. Neurosurgery 57:71–76; discussion 71-76. https://doi.org/10.1227/01.neu.0000163250.71951.18
Guzman R, Grady MS (1999) An intracranial aneurysm on the feeding artery of a cerebellar hemangioblastoma. Case report. J Neurosurg 91:136–138. https://doi.org/10.3171/jns.1999.91.1.0136
Hatva E, Bohling T, Jaaskelainen J, Persico MG, Haltia M, Alitalo K (1996) Vascular growth factors and receptors in capillary hemangioblastomas and hemangiopericytomas. Am J Pathol 148:763–775
Jagannathan J, Lonser RR, Smith R, DeVroom HL, Oldfield EH (2008) Surgical management of cerebellar hemangioblastomas in patients with von Hippel-Lindau disease. J Neurosurg 108:210–222. https://doi.org/10.3171/JNS/2008/108/2/0210
Ju C, Wright CH, Wright J, Duan Y, Bambakidis NC (2017) Subarachnoid hemorrhage associated with intratumoral aneurysm rupture within a posterior fossa hemangioblastoma: the importance of continued surveillance for cerebral vasospasm. Cureus 9:e1606. https://doi.org/10.7759/cureus.1606
Kuharic M, Jankovic D, Splavski B, Boop FA, Arnautovic KI (2018) Hemangioblastomas of the posterior cranial fossa in adults: demographics, clinical, morphologic, pathologic, surgical features, and outcomes. A systematic review. World Neurosurg 110:e1049–e1062. https://doi.org/10.1016/j.wneu.2017.11.173
Lee JY, Dong SM, Park WS, Yoo NJ, Kim CS, Jang JJ, Chi JG, Zbar B, Lubensky IA, Linehan WM, Vortmeyer AO, Zhuang Z (1998) Loss of heterozygosity and somatic mutations of the VHL tumor suppressor gene in sporadic cerebellar hemangioblastomas. Cancer Res 58:504–508
Liu X, Zhang Y, Hui X, You C, Yuan F, Chen W, Zhang S (2015) Surgical management of medulla oblongata hemangioblastomas in one institution: an analysis of 62 cases. Int J Clin Exp Med 8:5576–5590
Lonser RR, Butman JA, Huntoon K, Asthagiri AR, Wu T, Bakhtian KD, Chew EY, Zhuang Z, Linehan WM, Oldfield EH (2014) Prospective natural history study of central nervous system hemangioblastomas in von Hippel-Lindau disease. J Neurosurg 120:1055–1062. https://doi.org/10.3171/2014.1.JNS131431
Lv X, Wu Z, Li Y, Jiang C, Yang X, Zhang J (2011) Cerebral arteriovenous malformations associated with flow-related and circle of Willis aneurysms. World Neurosurg 76:455–458. https://doi.org/10.1016/j.wneu.2011.04.015
McKissock W, Paterson JH (1956) A clinical survey of intracranial angiomas with special reference to their mode of progression and surgical treatment: a report of 110 cases. Brain 79:233–266. https://doi.org/10.1093/brain/79.2.233
Meisel HJ, Mansmann U, Alvarez H, Rodesch G, Brock M, Lasjaunias P (2000) Cerebral arteriovenous malformations and associated aneurysms: analysis of 305 cases from a series of 662 patients. Neurosurgery 46:793–800; discussion 800-792. https://doi.org/10.1097/00006123-200004000-00004
Menovsky T, Andre Grotenhuis J, Bartels RH (2002) Aneurysm of the anterior inferior cerebellar artery (AICA) associated with high-flow lesion: report of two cases and review of literature. J Clin Neurosci 9:207–211. https://doi.org/10.1054/jocn.2001.0945
Murai Y, Kobayashi S, Tateyama K, Teramoto A (2006) Persistent primitive trigeminal artery aneurysm associated with cerebellar hemangioblastoma. Case report. Neurol Med Chir (Tokyo) 46:143–146. https://doi.org/10.2176/nmc.46.143
Redekop G, TerBrugge K, Montanera W, Willinsky R (1998) Arterial aneurysms associated with cerebral arteriovenous malformations: classification, incidence, and risk of hemorrhage. J Neurosurg 89:539–546. https://doi.org/10.3171/jns.1998.89.4.0539
Rothbart D, Awad IA, Lee J, Kim J, Harbaugh R, Criscuolo GR (1996) Expression of angiogenic factors and structural proteins in central nervous system vascular malformations. Neurosurgery 38:915–924; discussion 924-915. https://doi.org/10.1097/00006123-199605000-00011
Schmidt NO, Reitz M, Raimund F, Treszl A, Grzyska U, Westphal M, Regelsberger J (2011) Clinical relevance of associated aneurysms with arteriovenous malformations of the posterior fossa. Acta Neurochir Suppl 112:131–135. https://doi.org/10.1007/978-3-7091-0661-7_23
Seong Eom K, Won Kim D, Sung Choi S, Ha Choi K, Young Kim T (2011) Preoperative embolization of a cerebellar haemangioblastoma using Onyx: case report and literature review. Neurol Neurochir Pol 45:292–296. https://doi.org/10.1016/s0028-3843(14)60082-7
Skirgaudas M, Awad IA, Kim J, Rothbart D, Criscuolo G (1996) Expression of angiogenesis factors and selected vascular wall matrix proteins in intracranial saccular aneurysms. Neurosurgery 39:537–545; discussion 545-537. https://doi.org/10.1097/00006123-199609000-00021
Slater A, Moore NR, Huson SM (2003) The natural history of cerebellar hemangioblastomas in von Hippel-Lindau disease. AJNR Am J Neuroradiol 24:1570–1574
Sreenivasan SA, Madhugiri VS, Sasidharan GM, Kumar RV (2016) Measuring glioma volumes: a comparison of linear measurement based formulae with the manual image segmentation technique. J Cancer Res Ther 12:161–168. https://doi.org/10.4103/0973-1482.153999
Suzuki M, Umeoka K, Kominami S, Morita A (2014) Successful treatment of a ruptured flow-related aneurysm in a patient with hemangioblastoma: case report and review of literature. Surg Neurol Int 5:S430–S433. https://doi.org/10.4103/2152-7806.141887
Ueno K, Mabuchi S, Echizenya K, Isu T, Goto S (1977) Incidentally-discovered aneurysm--a report of eight cases (author's transl). No Shinkei Geka 5:183–188
Westphal M, Grzyska U (2000) Clinical significance of pedicle aneurysms on feeding vessels, especially those located in infratentorial arteriovenous malformations. J Neurosurg 92:995–1001. https://doi.org/10.3171/jns.2000.92.6.0995
Wizigmann-Voos S, Breier G, Risau W, Plate KH (1995) Up-regulation of vascular endothelial growth factor and its receptors in von Hippel-Lindau disease-associated and sporadic hemangioblastomas. Cancer Res 55:1358–1364
Yoshii Y, Maki Y, Tomono Y, Nakamura T (1976) Cerebellar hemangioblastoma with multiple aneurysms. No To Shinkei 28:703–708
Zager EL, Shaver EG, Hurst RW, Flamm ES (2002) Distal anterior inferior cerebellar artery aneurysms. Report of four cases. J Neurosurg 97:692–696. https://doi.org/10.3171/jns.2002.97.3.0692
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Tumor — Other
Rights and permissions
About this article
Cite this article
Moscovici, S., Candanedo, C., Spektor, S. et al. Solid vs. cystic predominance in posterior fossa hemangioblastomas: implications for cerebrovascular risks and patient outcome. Acta Neurochir 164, 1357–1364 (2022). https://doi.org/10.1007/s00701-021-04828-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-021-04828-w