Abstract
Background
Spinal arachnoid cysts (SAC) are rare mostly idiopathic intradural lesions with compression of the spinal cord and clinical signs of radiculo- and/or myelopathy. We retrospectively analyzed radiological and clinical characteristics of patients with surgical treatment of SAC including a subgroup evaluation of long-term outcome and QoL.
Method
Patients with SAC treated between 1993 and 2017 were evaluated. Craniocaudal (c.c.) and anteroposterior (a.p) cyst diameters were measured pre- and post-OP. McCormick and Odom score for myelopathy, general outcome and QoL (SF-36, EORTC-QLQ30) were recorded.
Results
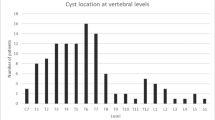
A total of 72 patients (female:male = 1.9:1) were analyzed with mean FU of 44.8 ± 60 months (long-term data from 25 patients with FU 78.2 ± 63.9 months). All had surgery due to solitary cysts: 10 cervical (13.9%), 45 thoracic (62.5%), and 17 lumbosacral (23.6%), the majority (79.2%) located dorsally. Main symptoms were gait disturbance (80%), dysesthesia (64%) and paresis (80%). Patients had (hemi-)laminectomy with cyst fenestration in 48 (66.7%) and complete resection in 18 cases (25.0%). Four cases (5.5%) were treated by cystoperitoneal shunt, 2 by marsupialization (2.8%). In total, 11 revisions were necessary in 9/72 (12.5%) patients (one patient underwent 3 revisions). Two patients were reoperated for wound revision/epidural hematoma (each n = 1). Seven patients needed additional cyst wall resection after 1.5–31.0 months due to insufficient cyst shrinking and persistent clinical symptoms after first surgery; most of the cysts were multiple septated and of post-hemorrhagic origin. The mean c.c. size decreased from 5.2 ± 3.7 cm pre-OP to 2.7 ± 3.9 cm (p < 0.05); the a.p. diameter decreased from 1.0 ± 0.5 cm to 0.3 ± 0.3 cm (p < 0.0001) without significant differences between fenestration and resection. McCormick and Odom scores revealed improved symptoms, particularly of gait disturbance, sensory deficits, and general performance. Long-term FU displayed satisfying QoL performance without differences of fenestration or resection.
Conclusion
SAC mostly affect women and are predominantly located in the thoracic spine, becoming apparent with clinical myelopathy. For cysts without intracystic septae and compartments, both fenestration and resection of the cyst wall provided significant reduction of cyst size and clinical improvement.








Similar content being viewed by others
References
Agnoli AL, Schonmayr R, Laun A (1982) Intraspinal arachnoid cysts. Acta Neurochir 61:291–302
Bellut D, Burkhardt JK, Mannion AF, Porchet F (2015) Assessment of outcome in patients undergoing surgery for intradural spinal tumor using the multidimensional patient-rated Core Outcome Measures Index and the modified McCormick Scale. Neurosurg Focus 39:E2. https://doi.org/10.3171/2015.5.FOCUS15163
Bitaraf MA, Zeinalizadeh M, Meybodi AT, Meybodi KT, Habibi Z (2009) Multiple extradural spinal arachnoid cysts: a case report and review of the literature. Cases J 2
Cloward RB (1968) Congenital spinal extradural cysts: case report with review of literature. Ann Sug 168(5):851–864
Ebner FH, Roser F, Falk M, Hermann S, Honegger J, Tatagiba M (2010) Management of intramedullary spinal cord lesions: interdependence of the longitudinal extension of the lesion and the functional outcome. Eur Spine J 19:665–669. https://doi.org/10.1007/s00586-009-1232-1
Endo T, Takahashi T, Jokura H, Tominaga T (2010) Surgical treatment of spinal intradural arachnoid cysts using endoscopy. J Neurosurg Spine 12
Ersahin Y, Ylldlzhan A, Seber N (1993) Spinal extradural arachnoidcyst. Childs Nerv Syst 9
Evangelou P, Meixensberger J, Bernhard M, Hirsch W, Kiess W, Merkenschlager A, Nestler U, Preuss M (2012) Operative management of idiopathic spinal intradural arachnoid cysts in children: a systematic review. Childs Nerv Syst 29
Fam MD, Woodroffe RW, Helland L, Noeller J, Dahdaleh NS, Menezes AH, Hitchon PW (2018) Spinal arachnoid cysts in adults: diagnosis and management. A single-center experience. J Neurosurg Spine 29:711–719. https://doi.org/10.3171/2018.5.SPINE1820
Fortuna A, La Torre E, Ciappetta P (1977) Arachnoid diverticula: a unitary approach to spinal cysts communicating with the subarachnoid space. Acta Neurochir 39
Funao H, Nakamura M, Hosogane N, Watanabe K, Tsuji T, Ishii K, Kamata M, Toyama Y, Chiba K, Matsumoto M (2012) Surgical treatment of spinal extradural arachnoid cysts in the thoracolumbar spine. J Neurol Surg 71
Gao Y, Zhang H, Yang J, Fu Q, Zheng J, Shuai M, Hu Z, Tan W, Cao W, Yang X, Jin A, Zhou R, Lu H (2015) Thoracolumbar arachnoid cyst with Horner syndrome: a case report and review of the literature. Cell Biochem Biophys 71
Griessenauer CJ, Bauer DF, Moore TA 2nd, Pritchard PR, Hadley MN (2014) Surgical manifestations of thoracic arachnoid pathology: series of 28 cases. J Neurosurg Spine 20:30–40. https://doi.org/10.3171/2013.9.SPINE1323
Hamamcioglu MK, Kilincer C, Hicdonmez T, Simsek O, Birgili B, Cobanoglu S (2006) Giant cervicothoracic extradural arachnoid cyst: case report. Eur Spine J 15
Hamburger C, Lanksch W, Oeckler R, Bachmann C (1994) The treatment of spondylotic cervical myelopathy by ventral discectomy. Long term results on 121 patients. Neurosurg Rev 17:247–252. https://doi.org/10.1007/bf00306811
Hingwala D, Chatterjee S, Kesavadas C, Thomas B, Kapilamoorthy TR (2011) Applications of 3D CISS sequence for problem solving in neuroimaging. Indian J Radiol Imaging 21:90–97. https://doi.org/10.4103/0971-3026.82283
Hironori F, Kazuhiro S, Toshiro K, Koichi M, Kenji F, Tooru I (2015) Extensive multilocular spinal extradural meningeal cyst developed 16 years after traumatic brachial plexus injury: a case report. World Neurosurgery
Kadono Y, Yuguchi T, Ohnishi Y, Iwatsuki K, Yoshimine T (2015) A symptomatic spinal extradural arachnoid cyst with lumbar disc herniation. Case Rep Orthop 2015
Kazan S, Ozdemir O, Akyüz M, Tuncer R (1999) Spinal intradural arachnoid cysts located anterior to the cervical spinal cord. Report of two cases and review of the literature. J Neurosurg 91
Kikuta K-I, Hojo M, Gomi M, Hashimoto N, Nozaki K (2006) Expansive duraplasty for the treatment of spinal extradural arachnoid cysts. J Neurosurg Spine 4
Klekamp J (2017) A new classification for pathologies of spinal meninges-part 2: primary and secondary intradural arachnoid cysts. Neurosurgery 81:217–229. https://doi.org/10.1093/neuros/nyx050
Klekamp J (2017) A new classification for pathologies of spinal meninges, part 1: dural cysts, dissections, and ectasias. Neurosurgery 81:29–44. https://doi.org/10.1093/neuros/nyx049
Kong W, Cho K, Hong S (2013) Spinal extradural arachnoid cyst: a case report. Korean J Spine 10
Kumar S, Desai A, Bhatia L, Garg A (2015) Multiple spinal arachnoid cysts in a child. Pediatr Neurol 1
Kusin DJ, Ahn UM, Ahn NU (2015) The effect of smoking on spinal cord healing following surgical treatment of cervical myelopathy. Spine 40:1391–1396. https://doi.org/10.1097/brs.0000000000001014
Lee SH, Shim HK, Eun SS (2014) Twist technique for removal of spinal extradural arachnoid cyst: technical note. Eur Spine J 23
Li AE, Wilkinson MD, McGrillen KM, Stoodley MA, Magnussen JS (2015) Clinical applications of cine balanced steady-state free precession MRI for the evaluation of the subarachnoid spaces. Clin Neuroradiol
Liu Y, Ban D, Kan S, Cao T, Feng S (2017) The impact of diabetes mellitus on patients undergoing cervical spondylotic myelopathy: a meta-analysis. Eur Neurol 77:105–112. https://doi.org/10.1159/000453547
Mahoney FI, Barthel DW (1965) Functional evaluation: the Barthel Index: a simple index of independence useful in scoring improvement in the rehabilitation of the chronically ill. Maryland State Med J 14:61–65
Mao H-Q, Yang H-L, Geng D-C, Bao Z-H, Tang T-S (2011) Spinal extradural arachnoid cyst following percutaneous vertebroplasty. Eur Spine J 20
Mohindra S, Gupta R, Bal A (2010) Intra-dural spinal arachnoid cysts: a short series of 10 patients. Br J Neurosurg 24:679–683. https://doi.org/10.3109/02688697.2010.504052
Nabors MW, Pait TG, Byrd EB, Karim NO, Davis DO, Kobrine AI, Rizolli HV (1988) Updated assessment and current classification of spinal meningeal cysts. J Neurosurg 68
Nakashima H, Imagama S, Yagi H, Kato F, Kanemura T, Sato K, Kawakami N, Kamiya M, Yoshihara H, Ito K, Matsuyama Y, Nishida Y, Ishiguro N (2017) Clinical and radiographical differences between thoracic idiopathic spinal cord herniation and spinal arachnoid cyst. Spine 42:E963–E968. https://doi.org/10.1097/brs.0000000000002013
Nath PC, Mishra SS, Deo RC, Satapathy MC (2015) Intra-dural spinal arachnoid cyst; a long term post laminectomy complication: a case report and review of literatures. World Neurosurgery
Nepomuceno E, Pacola LM, Dessotte CAM, Furuya RK, Defino HLA, Herrero CFPDS, RAS D (2016) Health-related quality of life and expectations of spinal stenosis patients towards the surgical treatment. Texto Contexto Enfermagem:25. https://doi.org/10.1590/0104-07072016001080015
Odom GL, Finney W, Woodhall B (1958) Cervical disk lesions. J Am Med Assoc 166:23–28. https://doi.org/10.1001/jama.1958.02990010025006
Osenbach RK, Godersky JC, Traynelis VC, Schelper RD (1992) Intradural extramedullary cysts of the spinal canal: clinical presentation, radiographic diagnosis, and surgical management. Neurosurgery 30:35–42
Ospina Moreno C, Vela Marin AC, Castan Senar A, Montejo Ganan I, Cozar Bartos M, Marin Cardenas MA (2016) Radiological diagnosis of spinal arachnoid cysts: a pictorial essay. J Med Imaging Radiat Oncol 60:632–638. https://doi.org/10.1111/1754-9485.12470
Papavlasopoulos F, Stranjalis G, Kouyialis AT, Korfias S, Sakas D (2007) Arachnoiditis ossificans with progressive syringomyelia and spinal arachnoid cyst. J Clin Neurosci 14:572–576. https://doi.org/10.1016/j.jocn.2006.02.024
Parmar H, Park P, Brahma B, Gandhi D (2008) Imaging of idiopathic spinal cord herniation. Radiographics 28:511–518. https://doi.org/10.1148/rg.282075030
Perret G, Green D, Keller J (1962) Diagnosis and treatment of intradural arachnoid cysts of the thoracic spine. Radiology 79:425–429. https://doi.org/10.1148/79.3.425
Peruzzotti-Jametti L, Ferrari S, Politi LS, Snider S, Mammi S, Comi G, Comola M (2010) Giant anterior arachnoid cyst associated with syringomyelia: implications for treatment and follow-up. Spine (Phila Pa 1976) 35:E322–E324. https://doi.org/10.1097/BRS.0b013e3181c8a40a
Petridis AK, Doukas A, Barth H, Mehdorn HM (2010) Spinal cord compression caused by idiopathic intradural arachnoid cysts of the spine: review of the literature and illustrated case. Eur Spine J 19(Suppl 2):S124–S129. https://doi.org/10.1007/s00586-009-1156-9
Qi J, Yang J, Wang G (2014) A novel five-category multimodal T1-weighted and T2-weighted magnetic resonance imaging-based stratification system for the selection of spinal arachnoid cyst treatment: a 15-year experience of 81 cases. Neuropsychiatr Dis Treat 10:499–506. https://doi.org/10.2147/NDT.S52517
Qi W, Zhao L, Fang J, Chang X, Xu Y (2015) Clinical characteristics and treatment strategies for idiopathic spinal extradural arachnoid cysts: a single-center experience. Acta Neurochir 157
Rexed BA, Wennstrom KG (1957) Arachnoidal proliferation and cystic formation in the spinal nerve-root pouches of man
Skoog A (1915) Spinal cord compression from leptomeningeal cysts. With a report of two cases. JAMA 65
Spiegelmann R, Rappaport ZH, Sahar A (1984) Spinal arachnoid cyst with unusual presentation. J Neurosurg 60
Spiller WG (1903) A case of intradural arachnoid cyst with operation and recovery. Trans Coll Physicians Philadelphia 25:1–18
Srinivasan VM, Fridley JS, Thomas JG, Omeis I (2016) Nuances in localization and surgical treatment of syringomyelia associated with fenestrated and webbed Intradural spinal arachnoid cyst: a retrospective analysis. World Neurosurg 87:176–186. https://doi.org/10.1016/j.wneu.2015.11.004
Stern Y, Spiegelmann R, Sadeh M (1991) Spinal intradural arachnoid cysts. Neurochirurgia (Stuttg) 34
Sun C, Meng X, Xie S, Yu Y, Yang H, Wu B (2011) Unilateral hemilaminectomy for patients with intradural extramedullary tumors. Biomed Biotechnol 12
T KM (1996) The interpretation of scores from the EORTC quality of life questionnaire QLQ-C30. Qual Life Res 5
Tarlov IM (1970) Spinal perineurial and meningeal cysts. J Neurol Neurosurg Psychiatry 33
Tauro A, Jovanovik J, Driver CJ, Rusbridge C (2018) Clinical application of 3D-CISS MRI sequences for diagnosis and surgical planning of spinal arachnoid diverticula and adhesions in dogs. Vet Comp Orthop Traumatol 31:83–94. https://doi.org/10.3415/VCOT-16-12-0169
Tucer B, Yılmaz MB, Ekıcı MA, Menku A, Koc K (2014) Spinal arachnoid cysts associated with syringomyelia: a review of the literature and report of a case. Turk Neurosurg 24
Viswanathan VK, Manoharan SR, Do H, Minnema A, Shaddy SM, Elder JB, Farhadi HF (2017) Clinical and radiologic outcomes after fenestration and partial wall excision of idiopathic intradural spinal arachnoid cysts presenting with myelopathy. World Neurosurg 105:213–222. https://doi.org/10.1016/j.wneu.2017.05.136
Zhang D, Papavassiliou E (2017) Spinal Intradural arachnoid webs causing spinal cord compression with inconclusive preoperative imaging: a report of 3 cases and a review of the literature. World Neurosurg 99:251–258. https://doi.org/10.1016/j.wneu.2016.12.015
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Comments
Schmutzer et al. present a large series of spinal intradural extramedullary arachnoid cysts. A few aspects are interesting and should be pointed out. First, CISS-3D MRI sequences are valuable in defining a cyst as monocompartimental and, if so, fenestration seems to be as good as cyst wall resection. Second, among the various myelopathic symptoms, only gait ataxia appears to benefit substantially from the surgical treatment. For other symptoms surgery is less beneficial and patients should also be informed on the possibility of relapse over time. Third, post-hemorrhagic cysts are rare but more prone to require revision surgery.
Francesco Sala
Verona, Italy
The authors report on 72 patients who had spinal intradural extramedullary arachnoid cysts. These cysts were treated with either fenestration or resection of the cyst. In a few cases, a cystoperitoneal shunt was utilized, and two patients had marsupialization. Good follow-up was provided with good neurological recovery. A good review of the literature is also provided. The authors found that comparing the two surgical techniques, the results were similar. It is still unclear to this reviewer when fenestration should be done vs. complete resection of the cyst wall. I congratulate the authors on an excellent follow-up when reporting on this relatively rare entity.
Volker K. H. Sonntag
Phoenix, Arizona
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Spine - Other
Rights and permissions
About this article
Cite this article
Schmutzer, M., Tonn, JC. & Zausinger, S. Spinal intradural extramedullary arachnoid cysts in adults—operative therapy and clinical outcome. Acta Neurochir 162, 691–702 (2020). https://doi.org/10.1007/s00701-019-04156-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-019-04156-0