Abstract
Purpose
The objective of our study was to develop a clinical prediction model for prolonged air leak (PAL) after lobectomy for lung cancer using preoperative variables in a large patient dataset from the National Clinical Database (NCD) in Japan.
Methods
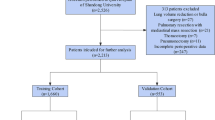
The preoperative characteristics of 57,532 and 30,967 patients who had undergone standard lobectomy for lung cancer were derived from the 2014 to 2015 and 2016 NCD datasets, respectively. PAL was defined as air leak persisting ≥ 7 days postoperatively or requiring postoperative interventional treatment, such as pleurodesis or reoperation. Risk models were developed from the 2014 to 2015 dataset and validated using the 2016 dataset. When performing model derivation, the least absolute shrinkage and selection operator (LASSO) method were applied for parameter selection.
Results
The rate of PAL was 4.5% in 2014–2015 and 5.3% in 2016. The age, sex, body mass index, comorbid interstitial pneumonia, smoking habits, forced expiratory volume in 1 s, tumor histology, multiple lung cancer, and tumor location were selected as important variables for PAL. Our risk model for predicting PAL was fair with a concordance index of 0.6895.
Conclusion
The LASSO-based risk model for PAL after lobectomy provided important preoperative variables for PAL and risk weighting for each variable.



Similar content being viewed by others
Abbreviations
- PAL:
-
Prolonged air leak
- NCD:
-
National Clinical Database
- BMI:
-
Body mass index
- FEV1:
-
Forced expiratory volume in 1 s
- FVC:
-
Forced vital capacity
- LASSO:
-
Least absolute shrinkage and selection operator
- BIC:
-
Bayesian information criterion
- VC:
-
Vital capacity
- ROC:
-
Receiver-operating characteristic
- AUC:
-
Area under the curve
References
Rice TW, Okereke IC, Blackstone EH. Persistent air-leak following pulmonary resection. Chest Surg Clin N Am. 2002;12(3):529–39.
Brunelli A, Cassivi SD, Halgren L. Risk factors for prolonged air leak after pulmonary resection. Thorac Cardiovasc Surg. 2010;20(3):359–64.
Rivera C, Bernard A, Falcoz PE, Thomas P, Schmidt A, Benard S, et al. Characterization and prediction of prolonged air leak after pulmonary resection: a nationwide study setting up the index of prolonged air leak. Ann Thoracic Surg 2011;92(3):1062–8; discussion 8.
Pompili C, Detterbeck F, Papagiannopoulos K, Sihoe A, Vachlas K, Maxfield MW, et al. Multicenter international randomized comparison of objective and subjective outcomes between electronic and traditional chest drainage systems. Ann Thoracic Surg 2014;98(2):490–6; discussion 6–7.
Murakami J, Ueda K, Tanaka T, Kobayashi T, Hamano K. Grading of emphysema is indispensable for predicting prolonged air leak after lung lobectomy. Ann Thorac Surg. 2018;105(4):1031–7.
Stephan F, Boucheseiche S, Hollande J, Flahault A, Cheffi A, Bazelly B, et al. Pulmonary complications following lung resection: a comprehensive analysis of incidence and possible risk factors. Chest. 2000;118(5):1263–70.
DeCamp MM, Blackstone EH, Naunheim KS, Krasna MJ, Wood DE, Meli YM, et al. Patient and surgical factors influencing air leak after lung volume reduction surgery: lessons learned from the National Emphysema Treatment Trial. Ann Thoracic Surg 2006;82(1):197–206; discussion -7.
Burt BM, Shrager JB. Prevention and management of postoperative air leaks. Ann Cardiothoracic Surg. 2014;3(2):216–8.
Attaar A, Winger DG, Luketich JD, Schuchert MJ, Sarkaria IS, Christie NA, et al. A clinical prediction model for prolonged air leak after pulmonary resection. J Thoracic Cardiovasc Surg. 2017;153(3):690–9 e2.
Cerfolio RJ, Bass CS, Pask AH, Katholi CR. Predictors and treatment of persistent air leaks. The Annals of thoracic surgery. 2002;73(6):1727–30; discussion 30–1.
Singhal S, Ferraris VA, Bridges CR, Clough ER, Mitchell JD, Fernando HC, et al. Management of alveolar air leaks after pulmonary resection. Ann Thorac Surg. 2010;89(4):1327–35.
Pompili C, Falcoz PE, Salati M, Szanto Z, Brunelli A. A risk score to predict the incidence of prolonged air leak after video-assisted thoracoscopic lobectomy: an analysis from the European Society of Thoracic Surgeons database. J Thorac Cardiovasc Surg. 2017;153(4):957–65.
Endo S, Ikeda N, Kondo T, Nakajima J, Kondo H, Yokoi K, et al. Development of an annually updated Japanese national clinical database for chest surgery in 2014. Gen Thorac Cardiovasc Surg. 2016;64(10):569–76.
Endo S, Ikeda N, Kondo T, Nakajima J, Kondo H, Yokoi K, et al. Model of lung cancer surgery risk derived from a Japanese nationwide web-based database of 78 594 patients during 2014–2015. Eur J Cardio-Thoracic Surg. 2017;52(6):1182–9.
Tibshirani R. Regression shrinkage and selection via the Lasso. J Roy Stat Soc B Met. 1996;58(1):267–88.
Petrella F, Rizzo S, Radice D, Borri A, Galetta D, Gasparri R, et al. Predicting prolonged air leak after standard pulmonary lobectomy: computed tomography assessment and risk factors stratification. Surgeon. 2011;9(2):72–7.
Elsayed H, McShane J, Shackcloth M. Air leaks following pulmonary resection for lung cancer: is it a patient or surgeon related problem? Ann R Coll Surg Engl. 2012;94(6):422–7.
Okereke I, Murthy SC, Alster JM, Blackstone EH, Rice TW. Characterization and importance of air leak after lobectomy. Ann Thorac Surg. 2005;79(4):1167–73.
Li SJ, Zhou K, Li YJ, Li PF, Wu YM, Liu LX, et al. Efficacy of the fissureless technique on decreasing the incidence of prolonged air leak after pulmonary lobectomy: a systematic review and meta-analysis. Int J Surg. 2017;42:1–10.
Pavlou M, Ambler G, Seaman SR, Guttmann O, Elliott P, King M, et al. How to develop a more accurate risk prediction model when there are few events. Bmj-Brit Med J. 2015;351:3868.
Zaraca F, Pipitone M, Feil B, Perkmann R, Bertolaccini L, Curcio C, et al. Predicting a Prolonged Air Leak After Video-Assisted Thoracic Surgery, Is It Really Possible? Semin Thorac Cardiovasc Surg. 2020.
Suzuki K, Saji H, Aokage K, Watanabe SI, Okada M, Mizusawa J, et al. Comparison of pulmonary segmentectomy and lobectomy: Safety results of a randomized trial. J Thorac Cardiovasc Surg. 2019;158(3):895–907.
Acknowledgements
The authors wish to thank all of the data managers and contributors at the participating institutions in this NCD project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yamamoto H, Fukuchi E, and Miyata H are affiliated with the Department of Healthcare Quality Assessment at the University of Tokyo. The department is a social collaboration department supported by grants from NCD, Johnson & Johnson K.K., and Nipro Co.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shintani, Y., Yamamoto, H., Sato, Y. et al. A risk model for prolonged air leak after lobectomy using the National Clinical Database in Japan. Surg Today 52, 69–74 (2022). https://doi.org/10.1007/s00595-021-02300-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-021-02300-x