Abstract
Purpose
It remains unclear whether laparoscopic gastrectomy (LG) for gastric cancer is a suitable treatment for very elderly (VE) patients. We aimed to assess the safety and feasibility of LG for gastric cancer in VE patients.
Methods
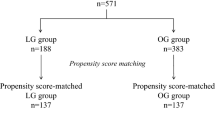
We reviewed 226 consecutive patients who underwent LG between January 2010 and December 2016. We compared VE patients (age ≥ 80, n = 38) with non-elderly patients (age ≤ 79, n = 188).
Results
An ASA-PS score ≥ 2 was more common in VE group (86.8 vs. 48.9%; P < 0.01). There were no significant differences in the operating time, blood loss, postoperative hospital stay, or postoperative morbidity between the groups. The 3-year survival rate and 3-year disease-specific survival rate were lower in the VE group (53.7 vs. 85.6%; P < 0.0001, 78.5 vs. 92.4%; P = 0.0116). A univariate analysis showed that PS scores ≥ 2, Charlson comorbidity index ≥ 4, and pN stage were independent predictors of decreased overall survival rates in the VE group. A multivariate analysis showed total gastrectomy, a Charlson comorbidity index ≥ 4, and the pN stage to be independent predictors in the VE group.
Conclusion
LG for gastric cancer is, thus, considered to be safe for patients aged 80 years or older. Total gastrectomy, a Charlson comorbidity index ≥ 4, and the pN stage were independent risk factors for a poor prognosis in these patients.


Similar content being viewed by others
References
Health_Labor_and_Welfare”M.Vital Statistics in Japan–The latest trend(Japanese). 2018.https://ganjoho.jp/reg_stat/statistics/dl/index.html. Accessed 12 Dec 2018.
Kitano S, Iso Y, Moriyama M, Sugimachi K. Laproscopy-assisted Billroth I gastrectomy. Surg Laparosc Endosc. 1994;4:146–8.
Kim HH, Hyung WJ, Cho GS, Kim MC, Han SU, Kim W, et al. Morbidity and mortality of laparoscopic gastrectomy versus open gastrectomy for gastric cancer: an interim report-a phase III multicenter, prospective, randomized Trial(KLASS Trial). Ann Surg. 2010;251:417–20.
Vinuela EF, Gonen M, Brennan MF, Coit DG, Strong VE. Laparscopic versus open gastrectomy for gastric cancer, a meta-analysis of randomized controlled trials and high-quality nonrandomized studies. Ann Surg. 2012;255:446–56.
Haverkamp L, Brenkman HJ, Seesing MF, Gisbertz SS, van Berge Henegouwen MI, Luyer MD, LOGICA study group. Laparoscopic versus open gastrectomy for gastric cancer, multicenter prospectively randomized controlled trial (LOGICA-trial). BMC Cancer. 2015. https://doi.org/10.1186/S12885-015-1551-Z:556.
Hu Y, Huang C, Sun Y, Su X, Cao H, Hu J, et al. Morbidity and mortality of laparoscopic versus open D2 distal gastrectomy for advanced gastric cancer: a randomized controlled trial. J Clin Oncol. 2016;34:1350–7.
Mohri Y, Yasuda H, Ohi M, Tanaka K, Saigusa S, Okigami M, et al. Short-and long-term outcomes of laparoscopic gastrectomy in elderly patients with gastric cancer. Surg Endosc. 2015;29:1627–35.
Shimoda S, Sawada N, Oae S, Seki J, Takano Y, Ishiyama Y, et al. Safety and curability of laparoscopic gastrectomy in elderly patients with gastric cancer. Surg Endosc. 2018;32:4277–83.
Aratani K, Sakuramoto S, Chuman M, Kasuya M, Wakata M, Miyawaki Y, et al. Laparoscopy-assisted distal gastrectomy for gastric cancer in elderly patients: surgical outcomes and prognosis. Antica Res. 2018;38:1721–5.
Yang XY, Zhu SH, Li PZ, Li WZ, Sun XL. Outcomes of laparoscopic gastrectomy for gastric cancer in elderly patients. JBUON. 2018;23:85–91.
Japanese Gastric Cancer Association. Japanese classification of gastric carcinoma. Gastric Cancer. 2011;14:101–12 (3rd English edition).
Dindo D, Demartines N, Clavien P. Classification of surgical complications. A new proposal with evaluation in a cohort of 6336 patients and results of survey. Ann Surg. 2004;240:205–13.
Kitano S, Shiraishi N, Fujiki K, Yasuda K, Inomata M, Adachi Y. A randomized controlled trial comparing open versus laparoscopy-assisted distal gastrectomy for the treatment of early gastric cancer:an interim report. Surgery. 2002;131(1 Suppl):306–11.
Mochiki E, Nakabayashi T, Kamimura H, Haga N, Asao T, Kuwano H. Gastrointestinal recovery and outcome after laparoscopy-assisted versus conventional open distal gastrectomy for early gastric cancer. World J Surg. 2002;26:1145–9.
Huscher CG, Mingoli A, Sgarzini G, Sansonetti A, Di Paola M, Recher A, et al. Laparoscopic versus open subtotal gastrectomy for distal gastric cancer: five-year results of a randomized prospective trial. Ann Surg. 2005;241:232–7.
Kitano S, Shiraishi N, Uyama I, Sugihara K, Tanigawa N, Japanese Laparoscopic Surgery Study Group. A multicenter study on oncologic outcome of laparoscopic gastrectomy for early cancer in Japan. Ann Surg. 2007;245:68–72.
Kim MC, Jung GJ, Kim HH. Morbidity and mortality of laparoscopy-assisted gastrectomy with extraperigastric lymph node dissection for gastric cancer. Dig Dis Sci. 2007;52:543–8.
Kim MC, Kim W, Kim HH, Ryu SW, Ryu SW, Song KY, Korean Laparoscopic Gastrointestinal Surgery Study (KLASS) Group. Risk factors associated with complication following laparoscopy-assisted gastrectomy for gastric cancer: a large-scale korean multicenter study. Ann Surg Oncol. 2008;15:2692–700.
Lee JH, Yom CK, Han HS. Comparison of long-term outcomes of laparoscopy-assisted and open distal gastrectomy for early gastric cancer. Surg Endosc. 2009;23:1759–63.
Katai H, Mizusawa J, Katayama H, Takagi M, Yoshikawa T, Fukagawa T, et al. Short-term surgical outcomes from a phase III study of laparoscopy-assisted versus open distal gastrectomy with nodal dissection for clinical stage IA/IB gastric cancer: Japan Clinical Oncology Group Study JCOG0912. Gastric Cancer. 2017;20:699–708.
Hiki N, Katai H, Mizusawa J, Nakamura K, Nakamori M, Yoshikawa T, Stomach Cancer Study Group of Japan Clinical Oncology Group. Long-term outcomes of laparoscopic -assisted distal gastrectomy with suprapancreatic nodal dissection for clinical stage I gastric cancer: multicenter phase II trial (JCOG0703). Gastric Cancer. 2018;21:155–61.
Li Z, Li B, Bai B, Yu P, Lian B, Zhao Q. Long-term outcomes of laparoscopic versus open D2 gastrectomy for advanced gastric cancer. Surg Oncol. 2018;27:441–8.
Inaki N, Etoh T, Ohyama T, Uchiyama K, Katada N, Koeda K, et al. A multi-institutional, prospective phase II feasibility study of laparoscopy-assisted distal gastrectomy with D2 lymph node dissection for locally advanced gastric cancer(JLSSG0901). World J Surg. 2015;39:2734–41.
Evers EM, Townsend CM Jr, Thompson JC. Organ physiology of aging. Surg Clin North Am. 1994;74:23–39.
Jeon SH, Ahn HS, Yoo MW, Cho JJ, Lee HJ, Kim HH, et al. Increased morbidity rates in patients with heart disease or chronic liver disease following radical gastric surgery. Ann Surg Oncol. 2010;101:200–4.
Tsuchiya N, Kunisaki C, Makino H, Kimura J, Takagawa R, Sato S, et al. Feasibility of laparoscopy-assisited gastrectomy for gastric cancer in elderly patients: a case-control study. Surg Laparosc Endosc Percutan Tech. 2018;28:102–7.
Yoshida M, Koga S, Ishimaru K, Yamamoto Y, Matsuo Y, Akita S, et al. Laparoscopy-assisted distal gastrectomy is feasible also for elderly patients aged 80 years and over: effectiveness and long-term prognosis. Surg Endosc. 2017;31:4431–7.
Inokuchi M, Tanioka T, Nagakawa M, Okuno K, Gokita K, Kojima K. Laparoscopic distal gastrectomy is feasible in very elderly patients as compared with open distal gastrectomy. J Invest Surg. 2017;22:1–7.
Kim SM, Youn HG, An JY, Choi YY, Noh SH, Oh SJ, et al. Comparison of open and laparoscopic gastrectomy in elderly patients. J Gastrointest Surg. 2018;22:785–91.
Matsushita I, Hanai H, Kajimura M, Tamakoshi K, Nakajima T, Matsubayashi Y, et al. Should gastric cancer patients more than 80 years of age undergo surgery? Comparison with patients not treated surgically concerning prognosis and quality of life. J Clin Gastroenterol. 2002;35:29–34.
Choo JW, Ju Y, Lim H, Youn SH, Soh JS, Park JW, et al. Is it beneficial to perform surgical resection in elderly patients more than 80 years old with advanced gastric cancer. Scand J Gastroenterol. 2017;52:1057–64.
Okabe H, Obama K, Tsunoda S, Tanaka E, Sakai Y. Advantage of completely laparoscopic gastrectomy with linear stapled reconstruction. A long-term follow-up study. Ann Surg. 2014;259:109–16.
Zhuang CL, Huang DD, Pang WY, Zhou CJ, Wang SL, Lou N, et al. Sarcopenia is an independent predictor of severe postoperative complications and long-term survival after radical gastrectomy for gastric cancer: analysis from a large-scale cohort. Medicine. 2016;95:e3164.
Nishigori T, Tsunoda S, Obama K, Hisamori K, Hashimoto K, Itatani Y, et al. Optimal cutoff values of skeletal muscle index to define sarcopenia for prediction of survival in patients with advanced gastric cancer. Ann Surg Oncol. 2018;25:3596–603.
Liu P, Hao Q, Hai S, Wang H, Cao Li, Dong B. Sarcopenia as a predictor of all-cause mortality among community-dwelling older people: a systematic review and meta-analysis. Maturitas. 2017;103:16–22.
Beaudart C, Zaaria M, Pasleau F, Reginster JY, Bruyere O. Health outcomes of sarcopenia: a systematic review and meta-analysis. PLoS ONE. 2017;12:e0169548.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest in association with this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mikami, R., Tanaka, E., Murakami, T. et al. The safety and feasibility of laparoscopic gastrectomy for gastric cancer in very elderly patients: short-and long-term outcomes. Surg Today 51, 219–225 (2021). https://doi.org/10.1007/s00595-020-02078-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-020-02078-4