Abstract
Aims
To determine the importance of blood sugar control, blood pressure, and other key systemic factors on the risk of progression from no retinopathy to various stages of diabetic retinopathy.
Methods
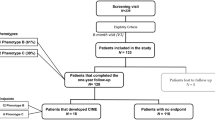
Restrospective cohort analysis of patients (N = 99, 280) in the Kaiser Permanente Northern California healthcare system with a baseline retina photographic screening showing no evidence of retinopathy and a minimum follow-up surveillance period of 3 years from 2008 to 2019. We gathered longitudinal data on diabetic retinopathy progression provided by subsequent screening fundus photographs and data captured in the electronic medical record over a mean surveillance of 7.3 ± 2.2 (mean ± SD) years. Progression from an initial state of no diabetic retinopathy to any of four outcomes was determined: (1) any incident retinopathy, (2) referable (moderate or worse) retinopathy, (3) diabetic macular edema, and (4) proliferative diabetic retinopathy. Multiple predictors, including age, race, gender, glycosylated hemoglobin (HbA1c), systolic blood pressure (SBP), cholesterol, chronic renal disease, and type of diabetes were investigated.
Results
Among modifiable risk factors, the average HbA1c had the strongest impact on the progression of diabetic retinopathy, followed by average SBP control and total cholesterol. Patients with an average HbA1c of 10.0% or greater (≥ 97 mmol/mol) had a risk ratio of 5.72 (95% CI 5.44–6.02) for progression to any retinopathy, 18.84 (95% CI 17.25–20.57) for referable retinopathy, 22.85 (95% CI 18.87–27.68) for diabetic macular edema, and 25.96 (95% CI 18.75–36.93) for proliferative diabetic retinopathy compared to those with an average HbA1c of 7.0% (53 mmol/mol) or less. Non-white patients generally had a higher risk of progression to all forms of diabetic retinopathy, while Asian patients were less likely to develop diabetic macular edema (HR 0.76, 95% CI 0.66–0.87).
Conclusions
We confirm the critical importance of glucose control as measured by HbA1c on the risk of development of diabetic retinopathy.


Similar content being viewed by others
References
Saeedi P, Petersohn I, Salpea P et al (2019) Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2015: results from the International Diabetes Federation Diabetes Atlas, 9(th) edition. Diabetes Res Clin Pract 157:107843. https://doi.org/10.1016/j.diabres.2019.107843
Yau JW, Rogers SL, Kawasaki R et al (2012) Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care 35:556–564. https://doi.org/10.2337/dc11-1909
Teo ZL, Tham Y, Yu M et al (2021) Global prevalence of diabetic retinopathy and projection of burden through 2045. Ophthalmology 128:1580–1591. https://doi.org/10.1016/j.ophtha.2021.04.027
The Early Treatment Diabetic Retinopathy Study Research Group (1991) Early photocoagulation for diabetic retinopathy: ETDRS report number 9. Ophthalmology 98:766–785
Wong TY, Sabanyagam C (2020) Strategies to tackle the global burden of diabetic retinopathy: from epidemiology to artificial intelligence. Ophthalmologica 243:9–20. https://doi.org/10.1159/000502387
Klein R, Klein BE, Moss SE et al (1984) The Wisconsin Epidemiologic Study of Diabetic Retinopathy. II Prevalence and risk of diabetic retinopathy when age at diagnosis is 30 or Less Years. Arch Ophthalmol 102:520–526. https://doi.org/10.1001/archopht.1984.01040030405011
Klein R, Knudtson MD, Lee KE et al (2008) The Wisconsin Epidemiologic Study of Diabetic Retinopathy XXII. The twenty-five year progression of retinopathy in persons with Type 1 diabetes. Ophthalmol 115:1859–1868. https://doi.org/10.1016/j.ophtha.2008.08.023
Varma R (2008) From a population to patients: The Wisconsin Epidemiologic Study of Diabetic Retinopathy. Ophthalmol 115:1857–1858. https://doi.org/10.1016/j.ophtha.2008.09.023
The Diabetes Control and Complications Trial Research Group, Nathan DM, Genuth S et al (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329:977–986. https://doi.org/10.1056/NEJM199309303291401
UK Prospective Diabetes Study Group (1998) Intensive blood-glucose control with sulphonylureas or insulin compared to conventional treatment and risk of complications in patients with type 2 diabetes. Lancet 352:837–853
Klein R, Klein BE, Moss SE et al (1989) Is blood pressure a predictor of the incidence or progression of diabetic retinopathy? Arch Int Med 149:2427–2432
UK Prospective Diabetes Study Group (1998) Tight blood pressure control and risk of macrovascular and microvascular complications in Type 2 diabetes (UKPDS 38). BMJ 317:703–713
Vujosevic S, Aldington SJ, Silva P et al (2020) Screening for diabetic retinopathy: new perspectives and challenges. Lancet Diabetes-Endocrinol 8:337–347. https://doi.org/10.1016/S2213-8587(19)30411-5
Wilkinson CP, Ferris FL, Klein RE et al (2003) Global Diabetic Retinopathy Study Group (2003) Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology 110:1677–1682. https://doi.org/10.1016/S0161-6420(03)00475-5
Strandberg-Larsen M, Schiotz ML, Silver JD et al (2010) Is the Kaiser Permanente model superior in terms of clinical integration? a comparative study of Kaiser Permanente, Northern California and the Danish healthcare system. BMC Health Serv Res 10:1–13. https://doi.org/10.1186/1472-6963-10-91
Melles RB, Conell C, Siegner SW, Tarasewicz D (2020) Diabetic retinopathy screening using a virtual reading center. Acta Diabetol 57:183–188. https://doi.org/10.1007/s00592-019-01392-9
Moffet HH, Adler N, Schillinger D et al (2009) The Diabetes Study of Northern California (DISTANCE)-objectives and design of a survey follow-up of social health disparities in a managed care population. Int J Epidemiol 38:38–47. https://doi.org/10.1093/ije/dyn040
Kuntz J, Young D, Saelens B et al (2021) Validity of the exercise vital sign tool to assess physical activity. Am J Prev Med 60:866–872. https://doi.org/10.1016/j.amepre.2021.01.012
Gong Q, Fang L (2013) Comparison of different parametric proportional hazards models for interval-censored data: a simulation study. Contemp Clin Trials 36:276–283. https://doi.org/10.1016/j.cct.2013.07.012
Jaffe MG, Young JD (2016) The Kaiser Permanente Northern California Story: Improving hypertension control from 44% to 90% in 13 years (2000 to 2013). J Clin Hypertens 18:260–261. https://doi.org/10.1111/jch.12803
Man R, Sasongko M, Wang J et al (2015) The association of estimated glomerular filtration rate with diabetic retinopathy and macular edema. Invest Ophthalmol Vis Sci 56:4810–4816. https://doi.org/10.1167/iovs.15-16987
Rajalakshmi R, Rani C, Venkatesan U et al (2020) Correlation between markers of renal function and sight threatening diabetic retinopathy in type 2 diabetes: a longitudinal study in an Indian clinic population. BMJ Open Diabetes Res Care 8:1–9. https://doi.org/10.1136/bmjdrc-2020-001325
Wang Z, do Carmo J, Aberdein N et al (2017) Synergistic interaction of hypertension and diabetes in promoting kidney injury and the role of endoplasmic reticulum stress. Hypertension 69:879–891. https://doi.org/10.1161/HYPERTENSIONAHA.116.08560
He F, Xia X, Wu XF et al (2013) Diabetic retinopathy in predicting diabetic nephropathy in patients with type 2 diabetes and renal disease: a meta-analysis. Diabetologia 56:457–466. https://doi.org/10.1007/s00125-012-2796-6
Aspelund T, Thornorisdottir O, Olafsdottir E et al (2011) Individual risk assessment and information technology to optimize screening frequency for diabetic retinopathy. Diabetologia 54:2525–2532. https://doi.org/10.1007/s00125-011-2257-7
Eleuteri A, Fisher AC, Broadbent DM et al (2017) Individualised variable-interval risk-based screening for sight-threatening diabetic retinopathy: the Liverpool Risk Calculation Engine. Diabetologia 60:2174–2182. https://doi.org/10.1007/s00125-017-4386-0
Agardh E, Tababat-Khani P (2011) Adopting 3-year screening intervals for sight-threatening retinal vascular lesions in type 2 diabetic subjects without retinopathy. Diabetes Care 34:1318–1319. https://doi.org/10.2337/dc10-2308
Funding
This work was funded by Kaiser Permanente Community Health Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicting relationship exists for any author.
Ethics Approval
This study was performed under Kaiser Permanente Institutional Review Board approval and adhered to the tenets of the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article belongs to the topical collection Eye Complications of Diabetes, managed by Giuseppe Querques.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tarasewicz, D., Conell, C., Gilliam, L.K. et al. Quantification of risk factors for diabetic retinopathy progression. Acta Diabetol 60, 363–369 (2023). https://doi.org/10.1007/s00592-022-02007-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-022-02007-6