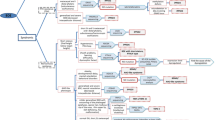
Abstract
Aims
The precision medicine approach of tailoring treatment to the individual characteristics of each patient has been a great success in monogenic diabetes subtypes, highlighting the importance of accurate clinical and genetic diagnoses of the type of diabetes. We sought to describe three unique cases of childhood-onset diabetes in whom skeletal manifestations led to the revelation of a rare type of diabetes.
Methods
Case-scenarios and review of the literature.
Results
Case 1: A homozygous mutation in TRMT10A, a tRNA methyltransferase, was identified in a 15-year-old boy with new-onset diabetes, developmental delay, microcephaly, dysmorphism, short stature and central obesity. The progressive apoptosis of pancreatic beta cells required insulin replacement therapy, with increased demand due to an unfavorable body composition. Case 2: Congenital generalized lipodystrophy type 1 was suspected in an adolescent male with an acromegaloid facial appearance, muscular habitus, and diabetes who presented with a pathological fracture in a cystic bone lesion. A homozygous mutation in AGPAT2, an acyl transferase which mediates the formation of phospholipid precursors, was identified. Leptin replacement therapy initiation resulted in a remarkable improvement in clinical parameters. Case 3: A 12-year-old boy with progressive lower limb weakness and pain was diagnosed with diabetic ketoacidosis. Diffuse diaphyseal osteosclerosis compatible with the diagnosis of Camurati-Engelmann disease and a heterozygous mutation in TGFβ1 were identified. Preservation of euglycemia by insulin replacement relieved pain, suggesting that the diabetic milieu may have augmented TGFβ1 overexpression.
Conclusion
Unraveling the precise genetic cause for the clinical manifestations led to the prediction of phenotypic manifestations, and enhanced the clinical outcomes.

Similar content being viewed by others
Data availability
All data are provided in the manuscript.
References
Mayer-Davis EJ, Lawrence JM, Dabelea D et al (2017) Incidence trends of Type 1 and Type 2 diabetes among youths, 2002–2012. N Engl J Med 376:1419–1429. https://doi.org/10.1056/NEJMoa1610187
Leete P, Oram RA, McDonald TJ et al (2020) Studies of insulin and proinsulin in pancreas and serum support the existence of aetiopathological endotypes of type 1 diabetes associated with age at diagnosis. Diabetologia 63:1258–1267. https://doi.org/10.1007/s00125-020-05115-6
Battaglia M, Ahmed S, Anderson MS et al (2020) Introducing the endotype concept to address the challenge of disease heterogeneity in Type 1 diabetes. Diabetes Care 43:5–12. https://doi.org/10.2337/dc19-0880
Delvecchio M, Pastore C, Giordano P (2020) Treatment options for MODY patients: a systematic review of literature. Diabetes Ther 11:1667–1685. https://doi.org/10.1007/s13300-020-00864-4
Shepherd M, Shields B, Hammersley S et al (2016) Systematic population screening, using biomarkers and genetic testing, identifies 2.5% of the UK pediatric diabetes population with monogenic diabetes. Diabetes Care 39:1879–1888. https://doi.org/10.2337/dc16-0645
Ellard S, Lango Allen H, De Franco E et al (2013) Improved genetic testing for monogenic diabetes using targeted next-generation sequencing. Diabetologia 56:1958–1963. https://doi.org/10.1007/s00125-013-2962-5
McCarthy MI (2017) Painting a new picture of personalised medicine for diabetes. Diabetologia 60:793–799. https://doi.org/10.1007/s00125-017-4210-x
Igoillo-Esteve M, Genin A, Lambert N et al (2013) tRNA methyltransferase homolog gene TRMT10A mutation in young onset diabetes and primary microcephaly in humans. PLoS Genet 2013(9):e1003888. https://doi.org/10.1371/journal.pgen.1003888
Gillis D, Krishnamohan A, Yaacov B, Shaag A, Jackman JE, Elpeleg O (2014) TRMT10A dysfunction is associated with abnormalities in glucose homeostasis, short stature and microcephaly. J Med Genet 51:581–586. https://doi.org/10.1136/jmedgenet-2014-102282
Machnicka MA (2013) MODOMICS: a database of RNA modification pathways: 2012 update. Nucleic Acids Res 41:D262–D267. https://doi.org/10.1093/nar/gks1007
Swinehart WE, Henderson JC, Jackman JE (2013) Unexpected expansion of tRNA substrate recognition by the yeast m1G9 methyltransferase Trm10. RNA 19:1137–1146. https://doi.org/10.1261/rna.039651.113
Ontiveros RJ, Shen H, Stoute J et al (2020) Coordination of mRNA and tRNA methylations by TRMT10A. Proc Natl Acad Sci U S A 117:7782–7791. https://doi.org/10.1073/pnas.1913448117
Shao Z, Yan W, Peng J et al (2014) Crystal structure of tRNA m1G9 methyltransferase Trm10: insight into the catalytic mechanism and recognition of tRNA substrate. Nucleic Acids Res 42:509–525. https://doi.org/10.1073/pnas.1913448117
Cosentino C, Toivonen S, Diaz Villamil E et al (2018) Pancreatic β-cell tRNA hypomethylation and fragmentation link TRMT10A deficiency with diabetes. Nucleic Acids Res 46:10302–10318. https://doi.org/10.1093/nar/gky839
Lin H, Zhou X, Chen X et al (2020) tRNA methyltransferase 10 homologue A (TRMT10A) mutation in a Chinese patient with diabetes, insulin resistance, intellectual deficiency and microcephaly. BMJ Open Diabetes Res Care 8:e001601. https://doi.org/10.1136/bmjdrc-2020-001601
Gorin K, Golomb M, Spitzen S et al (2020) A rare frameshift mutation in the AGPAT2 gene in a family from gaza with congenital generalized lipodystrophy. Clin Endocrinol (Oxf) 93:212–214. https://doi.org/10.1111/cen.14223
Leung DW (2001) The structure and functions of human lysophosphatidic acid acyltransferases. Front Biosci 6:D944–D953. https://doi.org/10.2741/leung
Simha V, Garg A (2003) Phenotypic heterogeneity in body fat distribution in patients with congenital generalized lipodystrophy caused by mutations in the AGPAT2 or seipin genes. J Clin Endocrinol Metab 88:5433–5437. https://doi.org/10.1210/jc.2003-030835
Subauste AR, Das AK, Li X et al (2012) Alterations in lipid signaling underlie lipodystrophy secondary to AGPAT2 mutations. Diabetes 61:2922–2931. https://doi.org/10.2337/db12-0004
Imai T, Takakuwa R, Marchand S et al (2004) Peroxisome proliferator-activated receptor gamma is required in mature white and brown adipocytes for their survival in the mouse. Proc Natl Acad Sci USA 101:4543–4547. https://doi.org/10.1073/pnas.0400356101
Yao-Borengasser A, Rassouli N, Varma V et al (2008) Stearoyl-coenzyme A desaturase 1 gene expression increases after pioglitazone treatment and is associated with peroxisomal proliferator-activated receptor-gamma responsiveness. J Clin Endocrinol Metab 93:4431–4439. https://doi.org/10.1210/jc.2008-0782
Agarwal AK, Sukumaran S, Cortés VA et al (2011) Human 1-acylglycerol-3-phosphate O-acyltransferase isoforms 1 and 2: biochemical characterization and inability to rescue hepatic steatosis in Agpat2(-/-) gene lipodystrophic mice. J Biol Chem 286:37676–37691. https://doi.org/10.1074/jbc.M111.250449
Teboul-Coré S, Rey-Jouvin C, Miquel A et al (2016) Bone imaging findings in genetic and acquired lipodystrophic syndromes: an imaging study of 24 cases. Skeletal Radiol 45:1495–1506. https://doi.org/10.1007/s00256-016-2457-9
Brown RJ, Araujo-Vilar D, Cheung PT et al (2016) The Diagnosis and Management of Lipodystrophy Syndromes: A Multi-Society Practice Guideline. J Clin Endocrinol Metab 101:4500–4511. https://doi.org/10.1210/jc.2016-2466
Chakarova N, Balabanski L, Dimova R, Shinkov A, Tankova T (2021) A novel AGPAT2 mutation associated with a case of late-diagnosed congenital generalized lipodystrophy type 1. Acta Diabetol 58:505–511. https://doi.org/10.1007/s00592-020-01639-w
Lightbourne M, Brown RJ (2017) Genetics of lipodystrophy. Endocrinol Metab Clin North Am 46:539–554. https://doi.org/10.1016/j.ecl.2017.01.012
Stephen TL, Rutkowski MR, Allegrezza MJ et al (2014) Transforming growth factor β-mediated suppression of antitumor T cells requires FoxP1 transcription factor expression. Immunity 41:427–439. https://doi.org/10.1016/j.immuni.2014.08.012
Han A, Zhao H, Li J, Pelikan R, Chai Y (2014) ALK5-mediated transforming growth factor β signaling in neural crest cells controls craniofacial muscle development via tissue-tissue interactions. Mol Cell Biol 34:3120–3131. https://doi.org/10.1128/MCB.00623-14
Feng YF, Yuan F, Guo H, Wu WZ (2014) TGF-β1 enhances SDF-1-induced migration and tube formation of choroid-retinal endothelial cells by up-regulating CXCR4 and CXCR7 expression. Mol Cell Biochem 397:131–138. https://doi.org/10.1007/s11010-014-2180-6
Park JG, Lee DH, Moon YS, Kim KH (2014) Reversine increases the plasticity of lineage-committed preadipocytes to osteogenesis by inhibiting adipogenesis through induction of TGF-β pathway in vitro. Biochem Biophys Res Commun 446:30–36. https://doi.org/10.1016/j.bbrc.2014.02.036
Janssens K, ten Dijke P, Janssens S, Van Hul W (2005) Transforming growth factor-beta1 to the bone. Endocr Rev 26:743–774. https://doi.org/10.1210/er.2004-0001
Filvaroff E, Erlebacher A, Ye J et al (1999) Inhibition of TGF-beta receptor signaling in osteoblasts leads to decreased bone remodeling and increased trabecular bone mass. Development 126:4267–4279
Ota K, Quint P, Weivoda MM et al (2013) Transforming growth factor beta 1 induces CXCL16 and leukemia inhibitory factor expression in osteoclasts to modulate migration of osteoblast progenitors. Bone 57:68–75. https://doi.org/10.1016/j.bone.2013.07.023
Matt P, Schoenhoff F, Habashi J et al (2009) GenTAC Consortium. Circulating transforming growth factor-beta in Marfan syndrome. Circulation 120:526–532. https://doi.org/10.1161/CIRCULATIONAHA.108.841981
Janssens K, Gershoni-Baruch R, Guañabens N et al (2000) Mutations in the gene encoding the latency-associated peptide of TGF-beta 1 cause Camurati-Engelmann disease. Nat Genet 26:273–275. https://doi.org/10.1038/81563
Chang AS, Hathaway CK, Smithies O, Kakoki M (2016) Transforming growth factor-β1 and diabetic nephropathy. Am J Physiol Renal Physiol 310:F689–F696. https://doi.org/10.1152/ajprenal.00502.2015
Flores L, Näf S, Hernáez R, Conget I, Gomis R, Esmatjes E (2004) Transforming growth factor beta at clinical onset of Type 1 diabetes mellitus. A pilot study. Diabet Med 21:818–822. https://doi.org/10.1111/j.1464-5491.2004.01242.x
Cooper MS, Hewison M, Stewart PM (1999) Glucocorticoid activity, inactivity and the osteoblast. J Endocrinol 163:159–164. https://doi.org/10.1677/joe.0.1630159
Elena C, Chiara M, Angelica B et al (2018) Hyperglycemia and diabetes induced by glucocorticoids in nondiabetic and diabetic patients: revision of literature and personal considerations. Curr Pharm Biotechnol 19:1210–1220. https://doi.org/10.2174/1389201020666190102145305
Ayyavoo A, Derraik JG, Cutfield WS, Hofman PL (2014) Elimination of pain and improvement of exercise capacity in Camurati-Engelmann disease with losartan. J Clin Endocrinol Metab 99:3978–3982. https://doi.org/10.1210/jc.2014-2025
Pilemann-Lyberg S, Lindhardt M, Persson F, Andersen S, Rossing P (2018) Serum uric acid and progression of diabetic nephropathy in type 1 diabetes. J Diabetes Complications 32:470–473. https://doi.org/10.1016/j.jdiacomp.2018.02.002
Brener A, Peleg I, Rosenfeld T et al (2021) Beyond body mass index—body composition assessment by bioimpedance in routine endocrine practice. Endocr Pract 27:419–425. https://doi.org/10.1016/j.eprac.2020.10.013
McCarthy HD (2006) Body fat measurements in children as predictors for the metabolic syndrome: focus on waist circumference. Proc Nutr Soc 65:385–392. https://doi.org/10.1017/s0029665106005143
Kahn CR, Wang G, Lee KY (2019) Altered adipose tissue and adipocyte function in the pathogenesis of metabolic syndrome. J Clin Invest 129:3990–4000. https://doi.org/10.1172/JCI129187
Oral EA, Chan JL (2010) Rationale for leptin-replacement therapy for severe lipodystrophy. Endocr Pract 16:324–333. https://doi.org/10.4158/EP09155.RA
Acknowledgements
The authors wish to thank the subjects and their parents who participated in this study. The study was supported in part by the Morris Kahn family foundation, ISF Grant 2034/18 (to OSB) and the National Knowledge Center for Rare/Orphan Diseases of the Israel Ministry of Science, Technology and Space. The authors thank Esther Eshkol for editorial assistance.
Funding
None. The study was supported in part by the Morris Kahn family foundation, ISF Grant 2034/18 (to OSB) and the National Knowledge Center for Rare/Orphan Diseases of the Israel Ministry of Science, Technology and Space.
Author information
Authors and Affiliations
Contributions
AB and YL Conceptualization, AB, LZ, YW, OSB, TR, EC and YL Data curation, LZ, YW and OSB Investigation, AB Writing—original draft, AB, LZ, YW, OSB, TR, EC and YL Writing—review & editing, All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki.
Informed consent
The patients and their parents gave their informed consent to publish their case.
Additional information
Managed by Antonio Secchi.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Brener, A., Zeitlin, L., Wilnai, Y. et al. Looking for the skeleton in the closet—rare genetic diagnoses in patients with diabetes and skeletal manifestations. Acta Diabetol 59, 711–719 (2022). https://doi.org/10.1007/s00592-022-01854-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-022-01854-7