Abstract
Aims
We aimed to estimate the prevalence of Diabetic peripheral neuropathy (DPN) and Cardiac autonomic neuropathy (CAN) in youth with type 1 diabetes; identify key risk factors; identify the most useful tests for the diagnostic evaluation of DPN and CAN; identify key treatment options for DPN and CAN.
Methods
A systematic search was performed including studies published in the last 15 years. PICO framework was used in the selection process and evidence was assessed using the GRADE system.
Results
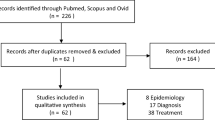
A total of 758 studies were identified and a final number of 49 studies were included in this systematic review. According to moderate-high level quality studies, the prevalence of probable DPN, ranged between 13.5 and 62%; subclinical DPN between 22 and 88%; confirmed DPN between 2.6 and 11%. The Michigan Neuropathy Screening Instrument was the tool with higher sensitivity and specificity for detecting DPN, which needs to be confirmed by nerve conduction velocity. The prevalence of CAN was 4–39%. Specific treatment options for DPN or CAN in patients younger than 25 years are not available. Key risk factors for DPN and CAN are hyperglycemia/HbA1c, age, diabetes duration, the presence of other microvascular complications, waist/height ratio, lipid profile and blood pressure. For CAN, additional risk factors were cigarette smoking, BMI and total daily insulin.
Conclusions
Prevalence of neuropathy in youth with type 1 diabetes varies depending on different screening methods and characteristics of the study populations. However, the assessed studies confirmed a relatively high prevalence of subclinical neuropathy, reiterating the importance of early identification of risk factors to prevent this complication.

Similar content being viewed by others
Data availability
All databases generated for this study are included in the article.
Abbreviations
- T1D:
-
Type 1 diabetes
- T2D:
-
Type 2 diabetes
- DKA:
-
Diabetic ketoacidosis
- DN:
-
Diabetic neuropathy
- DPN:
-
Diabetic peripheral neuropathy
- NDS:
-
Neuropathy disability score
- NSS:
-
Neuropathy symptom score
- QST:
-
Quantitative sensory testing
- VPT:
-
Vibration perception threshold
- TT:
-
Thermal threshold
- VT:
-
Vibration threshold
- MNSI:
-
Michigan neuropathy screening instrument examination
- NCS:
-
Nerve conduction studies
- NCV:
-
Nerve conduction velocity
- EMG:
-
Electromyography
- SD:
-
Standard deviation
- US:
-
Ultrasound
- HbA1c:
-
Hemoglobin A1c
- BMI SDS:
-
Body mass index standard deviation score
- CAN:
-
Cardiac autonomic neuropathy
- PAN GI:
-
Gastrointestinal
- GP:
-
Gastroparesis
- CARTs:
-
Cardiovascular tests
- BP:
-
Blood pressure
- BRS:
-
Baroreflex sensitivity
- HR:
-
Heart rate
- HRV:
-
Heart rate variability
- ECG:
-
Electrocardiography
- EDC:
-
Pittsburgh epidemiology of diabetes complications
References
Graves LE, Donaghue KC (2019) Management of diabetes complications in youth. Ther Adv Endocrinol Metab 10:2042018819863226. https://doi.org/10.1177/2042018819863226
Louraki M, Karayianni C, Kanaka-Gantenbein C, Katsalouli M, Karavanaki K (2012) Peripheral neuropathy in children with type 1 diabetes. Diabetes Metab 38(4):281–289. https://doi.org/10.1016/j.diabet.2012.02.006
Dabelea D, Stafford JM, Mayer-Davis EJ et al., (2017) Association of Type 1 Diabetes vs Type 2 Diabetes Diagnosed During Childhood and Adolescence With Complications During Teenage Years and Young Adulthood. JAMA 317(8):825–835. https://doi.org/10.1001/jama.2017.0686
Tesfaye S, Boulton AJM, Dyck PJ et al. (2010) Diabetic neuropathies: update on definitions, diagnostic criteria, estimation of severity, and treatments. Diabetes Care 33(10):2285–2293. https://doi.org/10.2337/dc10-1303
Jaiswal M, Divers J, Urbina EM et al. (2018) Cardiovascular autonomic neuropathy in adolescents and young adults with type 1 and type 2 diabetes: The SEARCH for Diabetes in Youth Cohort Study. Pediatr Diabetes 19(4):680–689. https://doi.org/10.1111/pedi.12633
Martin CL, Albers JW, Pop-Busui R, DCCT/EDIC Research Group (2014) Neuropathy and related findings in the diabetes control and complications trial/epidemiology of diabetes interventions and complications study. Diabetes Care 37(1):31–38. https://doi.org/10.2337/dc13-2114
Boysen A, Lewin MA, Hecker W, Leichter HE, Uhlemann F (2007) Autonomic function testing in children and adolescents with diabetes mellitus. Pediatr Diabetes 8(5):261–264. https://doi.org/10.1111/j.1399-5448.2007.00254.x
Donaghue KC, Marcovecchio ML, Wadwa RP, et al. (2018) ISPAD Clinical Practice Consensus Guidelines 2018: Microvascular and macrovascular complications in children and adolescents. Pediatr Diabetes 27:262–274. https://doi.org/10.1111/pedi.12742
American Diabetes Association (2020) Microvascular Complications and Foot Care: Standards of Medical Care in Diabetes-2020. Diabetes Care 43(Suppl 1):S135–S151. https://doi.org/10.2337/dc20-S011
Malik FS, Stafford JM, Reboussin BA et al. (2020) Receipt of recommended complications and comorbidities screening in youth and young adults with type 1 diabetes: Associations with metabolic status and satisfaction with care. Pediatr Diabetes 21(2):349–357. https://doi.org/10.1111/pedi.12948
Cho YH, Craig ME, Hing S, et al. (2011) Microvascular complications assessment in adolescents with 2- to 5-yr duration of type 1 diabetes from 1990 to 2006. Pediatr Diabetes 12(8):682–689. https://doi.org/10.1111/j.1399-5448.2011.00762.x
Elbarbary NS, Ismail EAR, El-Hilaly RA, Ahmed FS (2018) Role of neopterin as a biochemical marker for peripheral neuropathy in pediatric patients with type 1 diabetes: Relation to nerve conduction studies. Int Immunopharmacol 59:68–75. https://doi.org/10.1016/j.intimp.2018.03.026
Schünemann HJ, Cuello C, Akl EA etal. (2019) GRADE guidelines: 18. How ROBINS-I and other tools to assess risk of bias in nonrandomized studies should be used to rate the certainty of a body of evidence. J Clin Epidemiol 111:105–114. https://doi.org/10.1016/j.jclinepi.2018.01.012
Türkyilmaz H, Güzel O, Edizer S, Ünalp A (2017) Evaluation of polyneuropathy and associated risk factors in children with type 1 diabetes mellitus. Turk J Med Sci 47(3):942–946. https://doi.org/10.3906/sag-1601-183
AboElAsrar MA, Elbarbary NS, Elshennawy DE et al. (2012) Insulin-like growth factor-1 cytokines cross-talk in type 1 diabetes mellitus: relationship to microvascular complications and bone mineral density. Cytokine 59(1):86–93. https://doi.org/10.1016/j.cyto.2012.03.019
Amutha A, Datta M, Unnikrishnan IR, et al. (2011) Clinical profile of diabetes in the young seen between 1992 and 2009 at a specialist diabetes centre in south India. Prim Care Diabetes 5(4):223–229. https://doi.org/10.1016/j.pcd.2011.04.003
Blankenburg M, Kraemer N, Hirschfeld G, et al. (2012) Childhood diabetic neuropathy: functional impairment and non-invasive screening assessment. Diabet Med 29(11):1425–1432. https://doi.org/10.1111/j.1464-5491.2012.03685.x
Ghaemi N, Hasanabadi H, Ashrafzadeh F, et al. (2018) Peripheral Neuropathy in Children and Adolescents with Insulin-dependent Diabetes Mellitus. Iran J Child Neurol 12(2):83–90
Hajas G, Kissova V, Tirpakova A (2016) A 10-yr follow-up study for the detection of peripheral neuropathy in young patients with type 1 diabetes. Pediatr Diabetes 17(8):632–641. https://doi.org/10.1111/pedi.12382
Hasani N, Khosrawi S, Hashemipour M, et al. (2013) Prevalence and related risk-factors of peripheral neuropathy in children with insulin-dependent diabetes mellitus. J Res Med Sci 18(2):132–136
Elsamahy MH, Elbarbary NS, Elmorsi HM (2015) Current status of diabetes management, glycemic control and complications in children and adolescents with diabetes in Egypt Where do we stand now And where do we go from here. Diabetes Res Clin Pract 107(3):370–376
Christensen MMB, Hommel EE, Jørgensen ME, et al. (2018) Prevalence of Diabetic Neuropathy in Young Adults with Type 1 Diabetes and the Association with Insulin Pump Therapy. Diabetes Technol Ther. https://doi.org/10.1089/dia.2018.0249
Jaiswal M, Divers J, Dabelea D, et al. (2017) Prevalence of and Risk Factors for Diabetic Peripheral Neuropathy in Youth With Type 1 and Type 2 Diabetes: SEARCH for Diabetes in Youth Study. Diabetes Care 40(9):1226–1232. https://doi.org/10.2337/dc17-0179
Albers JW, Herman WH, Pop-Busui R et al. (2010) Effect of prior intensive insulin treatment during the Diabetes Control and Complications Trial (DCCT) on peripheral neuropathy in type 1 diabetes during the Epidemiology of Diabetes Interventions and Complications (EDIC) Study. Diabetes Care 33(5):1090–1096. https://doi.org/10.2337/dc09-1941
Chistiakov DA, Spitsina EV, Nikitin AG, Strokov IA, Nosikov VV (2009) A splice variant of GNB3 and peripheral polyneuropathy in type 1 diabetes. Dis Markers 26(3):111–117. https://doi.org/10.3233/DMA-2009-0620
Braffett BH, Gubitosi-Klug RA, Albers JW et al. (2020) Risk Factors for Diabetic Peripheral Neuropathy and Cardiovascular Autonomic Neuropathy in the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Study. Diabetes 69(5):1000–1010. https://doi.org/10.2337/db19-1046
Williams KW, Becker DJ, Orchard TJ, Costacou T (2019) Persistent C-peptide levels and microvascular complications in childhood onset type 1 diabetes of long duration. J Diabetes Complications 33(9):657–661. https://doi.org/10.1016/j.jdiacomp.2019.05.019
Marshall SL, Edidin D, Sharma V, et al. (2013) Current clinical status, glucose control, and complication rates of children and youth with type 1 diabetes in Rwanda. Pediatr Diabetes 14(3):217–226. https://doi.org/10.1111/pedi.12007
Verkauskiene R, Danyte E, Dobrovolskiene R, et al. (2016) The course of diabetes in children, adolescents and young adults: does the autoimmunity status matter? BMC Endocr Disord 16(1):61. https://doi.org/10.1186/s12902-016-0145-3
Hirschfeld G, von Glischinski M, Knop C, et al. (2015) Difficulties in screening for peripheral neuropathies in children with diabetes. Diabet Med 32(6):786–789. https://doi.org/10.1111/dme.12684
Louraki M, Tsentidis C, Kallinikou D, et al. (2014) Reproducibility of vibration perception threshold values in children and adolescents with type 1 diabetes mellitus and associated factors. Prim Care Diabetes 8(2):147–157. https://doi.org/10.1016/j.pcd.2013.11.002
Sauder KA, Stafford JM, Mayer-Davis EJ et al. (2019) Co-occurrence of early diabetes-related complications in adolescents and young adults with type 1 diabetes: an observational cohort study. Lancet Child Adolesc Health 3(1):35–43. https://doi.org/10.1016/S2352-4642(18)30309-2
Walter-Höliner I, Seick Barbarini D, Lütschg J, et al. (2018) High Prevalence and Incidence of Diabetic Peripheral Neuropathy in Children and Adolescents With Type 1 Diabetes Mellitus: Results From a Five-Year Prospective Cohort Study. Pediatr Neurol 80:51–60. https://doi.org/10.1016/j.pediatrneurol.2017.11.017
Abuelwafaa N, Ahmed H, Omer I, et al. (2019) Electrophysiological Characterization of Neuropathy Complicating Type 1 Diabetes Mellitus. J Diabetes Res 2019:2435261. https://doi.org/10.1155/2019/2435261
Ising E, Dahlin LB, Elding Larsson H (2018) Impaired vibrotactile sense in children and adolescents with type 1 diabetes - Signs of peripheral neuropathy. PLoS ONE 13(4):e0196243. https://doi.org/10.1371/journal.pone.0196243
Aulich J, Cho YH, Januszewski AS, et al. (2019) Associations between circulating inflammatory markers, diabetes type and complications in youth. Pediatr Diabetes 20(8):1118–1127. https://doi.org/10.1111/pedi.12913
Weintrob N, Amitay I, Lilos P, et al. (2007) Bedside neuropathy disability score compared to quantitative sensory testing for measurement of diabetic neuropathy in children, adolescents, and young adults with type 1 diabetes. J Diabetes Complications 21(1):13–19. https://doi.org/10.1016/j.jdiacomp.2005.11.002
Snahnicanova Z, Mendelova A, Grendar M, et al. (2018) Association of Polymorphisms in CYBA, SOD1, and CAT Genes with Type 1 Diabetes and Diabetic Peripheral Neuropathy in Children and Adolescents. Genet Test Mol Biomarkers 22(7):413–419. https://doi.org/10.1089/gtmb.2018.0018
Al-Taweela YA, Fahmia RM, Shehtaa N, et al. (2016) Frequency and determinants of subclinical neuropathy in type 1 diabetes mellitus. Egyptian J Neurol Psychiatry Neurosurg 53(4):232. https://doi.org/10.4103/1110-1083.202383
Craig ME, Duffin AC, Gallego PH, et al. (2008) Plantar fascia thickness, a measure of tissue glycation, predicts the development of complications in adolescents with type 1 diabetes. Diabetes Care 31(6):1201–1206. https://doi.org/10.2337/dc07-2168
Wever A, Schickenberg-Werrij BG, Willems J, Schaper NC, Schott DA (2016) Prevalence and awareness of functional and structural foot abnormalities in children and adolescents with type 1 diabetes. J Pediatr Endocrinol Metab 29(9):1019–1024. https://doi.org/10.1515/jpem-2015-0455
Billow A, Anjana RM, Ngai M, et al. (2015) Prevalence and clinical profile of metabolic syndrome among type 1 diabetes mellitus patients in southern India. J Diabetes Complications 29(5):659–664. https://doi.org/10.1016/j.jdiacomp.2015.03.014
Toopchizadeh V, Shiva S, Khiabani NY, Ghergherechi R (2016) Electrophysiologic pattern and prevalence of subclinical peripheral neuropathy in children and adolescents with type I diabetes mellitus in Iran. Saudi Med J 37(3):299–303. https://doi.org/10.15537/smj.2016.3.13625
Jaiswal M, Urbina EM, Wadwa RP, et al. (2013) Reduced heart rate variability among youth with type 1 diabetes: the SEARCH CVD study. Diabetes Care 36(1):157–162. https://doi.org/10.2337/dc12-0463
Louraki M, Katsalouli M, Kanaka-Gantenbein C, et al. (2016) The prevalence of early subclinical somatic neuropathy in children and adolescents with Type 1 diabetes mellitus and its association with the persistence of autoantibodies to glutamic acid decarboxylase (GAD) and islet antigen-2 (IA-2). Diabetes Res Clin Pract 117:82–90. https://doi.org/10.1016/j.diabres.2016.04.044
Moser JT, Langdon DR, Finkel RS, et al. (2013) The evaluation of peripheral neuropathy in youth with type 1 diabetes. Diabetes Res Clin Pract 100(1):e3-6. https://doi.org/10.1016/j.diabres.2013.01.015
Metwalley KA, Hamed SA, Farghaly HS (2018) Cardiac autonomic function in children with type 1 diabetes. Eur J Pediatr 177(6):805–813. https://doi.org/10.1007/s00431-018-3122-1
Cho YH, Craig ME, Jopling T, Chan A, Donaghue KC (2018) Higher body mass index predicts cardiac autonomic dysfunction: A longitudinal study in adolescent type 1 diabetes. Pediatr Diabetes 19(4):794–800. https://doi.org/10.1111/pedi.12642
Cho YH, Craig ME, Srinivasan S, et al. (2014) Heart rate variability in pubertal girls with type 1 diabetes: its relationship with glycaemic control, insulin resistance and hyperandrogenism. Clin Endocrinol (Oxf) 80(6):818–824. https://doi.org/10.1111/cen.12238
Dyck PJ, Bushek W, Spring EM et al. (1987) Vibratory and cooling detection thresholds compared with other tests in diagnosing and staging diabetic neuropathy. Diabetes Care 10(4):432–440. https://doi.org/10.2337/diacare.10.4.432
Gentile S, Turco S, Corigliano G, Marmo R (1995) Simplified diagnostic criteria for diabetic distal polyneuropathy Preliminary data of a multicentre study in the Campania region. Acta Diabetol 32(1):7–12. https://doi.org/10.1007/BF00581037
Herman WH, Pop-Busui R, Braffett BH et al. (2012) Use of the Michigan Neuropathy Screening Instrument as a measure of distal symmetrical peripheral neuropathy in Type 1 diabetes: results from the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications. Diabet Med 29(7):937–944. https://doi.org/10.1111/j.1464-5491.2012.03644.x
Cruz-Almeida Y, Fillingim RB (2014) Can quantitative sensory testing move us closer to mechanism-based pain management? Pain Med 15(1):61–72. https://doi.org/10.1111/pme.12230
Baba M, Matsui N, Kuroha M, Wasaki Y, Ohwada S (2019) Mirogabalin for the treatment of diabetic peripheral neuropathic pain: A randomized, double-blind, placebo-controlled phase III study in Asian patients. J Diabetes Investig 10(5):1299–1306. https://doi.org/10.1111/jdi.13013
Wahren J, Foyt H, Daniels M, Arezzo JC (2016) Long-Acting C-Peptide and Neuropathy in Type 1 Diabetes: A 12-Month Clinical Trial. Diabetes Care 39(4):596–602. https://doi.org/10.2337/dc15-2068
Mu Y, Liu X, Li Q, et al. (2018) Efficacy and safety of pregabalin for painful diabetic peripheral neuropathy in a population of Chinese patients: A randomized placebo-controlled trial. J Diabetes 10(3):256–265. https://doi.org/10.1111/1753-0407.12585
Fensom B, Harris C, Thompson SE, Al Mehthel M, Thompson DM (2016) Islet cell transplantation improves nerve conduction velocity in type 1 diabetes compared with intensive medical therapy over six years. Diabetes Res Clin Pract 122:101–105. https://doi.org/10.1016/j.diabres.2016.10.011
Brown S, Johnston B, Amaria K, et al. (2016) A randomized controlled trial of amitriptyline versus gabapentin for complex regional pain syndrome type I and neuropathic pain in children. Scand J Pain 13:156–163. https://doi.org/10.1016/j.sjpain.2016.05.039
Fraser DA, Diep LM, Hovden IA, et al. (2012) The effects of long-term oral benfotiamine supplementation on peripheral nerve function and inflammatory markers in patients with type 1 diabetes: a 24-month, double-blind, randomized, placebo-controlled trial. Diabetes Care 35(5):1095–1097. https://doi.org/10.2337/dc11-1895
Sun J, Wang Y, Zhang X, Zhu S, He H (2020) Prevalence of peripheral neuropathy in patients with diabetes: A systematic review and meta-analysis. Prim Care Diabetes 14(5):435–444. https://doi.org/10.1016/j.pcd.2019.12.005
Akinci G, Savelieff MG, Gallagher G, Callaghan BC, Feldman EL (2021) Diabetic neuropathy in children and youth: New and emerging risk factors. Pediatr Diabetes 22(2):132–147. https://doi.org/10.1111/pedi.13153
Hirschfeld G, von Glischinski M, Blankenburg M, Zernikow B (2014) Screening for peripheral neuropathies in children with diabetes: a systematic review. Pediatrics 133(5):e1324–e1330. https://doi.org/10.1542/peds.2013-3645
Tang M, Donaghue KC, Cho YH, Craig ME (2013) Autonomic neuropathy in young people with type 1 diabetes: a systematic review. Pediatr Diabetes 14(4):239–248. https://doi.org/10.1111/pedi.12039
Vasigh A, Abdi A, Borji M, Tarjoman A (2019) The prevalence of neuropathy among type 1 diabetic adolescents in Iran: a systematic review and meta-analysis. Int J Adolesc Med Health. https://doi.org/10.1515/ijamh-2018-0223
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
RF, EM, MLM conceived the study. RF and EM made a substantial contribution to the design of this literature review and screened abstracts. FDC, FR, LL, AL, FM, CAP conducted the full paper analysis. EM and RF independently assessed the certainty of the evidence for each of the outcomes. MLM resolved discrepancies. VC, AF, MLM wrote the manuscript. All the authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial or non-financial conflicts of interest to declare.
Human and animal rights
This article does not contain any studies with human participants performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Managed by Massimo Federici.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Franceschi, R., Mozzillo, E., Di Candia, F. et al. A systematic review of the prevalence, risk factors and screening tools for autonomic and diabetic peripheral neuropathy in children, adolescents and young adults with type 1 diabetes. Acta Diabetol 59, 293–308 (2022). https://doi.org/10.1007/s00592-022-01850-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-022-01850-x