Abstract
Purpose
The objective of this study was to determine the underlying factors that drive the decision for surgeons to pursue operative versus nonoperative management for proximal humerus fractures (PHF) and if fellowship training had an impact on these decisions.
Methods
An electronic survey was distributed to members of the Orthopaedic Trauma Association and the American Shoulder and Elbow Surgeons Society to assess differences in patient selection for operative versus nonoperative management of PHF. Descriptive statistics were reported for all respondents.
Results
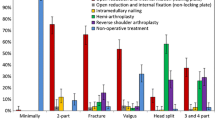
A total of 250 fellowship trained Orthopaedic Surgeons responded to the online survey. A greater proportion of trauma surgeons preferred nonoperative management for displaced PHF fractures in patients over the age of 70. Operative management was preferred for older patients with fracture dislocations (98%), limited humeral head bone subchondral bone (78%), and intraarticular head split (79%). Similar proportions of trauma surgeons and shoulder surgeons cited that acquiring a CT was crucial to distinguish between operative and nonoperative management.
Conclusion
We found that surgeons base their decisions on when to operate primarily on patient’s comorbidities, age, and the amount of fracture displacement when treating younger patients. Further, we found a greater proportion of trauma surgeons elected to proceed with nonoperative management in patients older than the age of 70 years old as compared to shoulder surgeons.

Similar content being viewed by others
References
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 8:691–697
Horak J, Nilsson BE (1975) Epidemiology of fracture of the upper end of the humerus. Clin Orthop Relat Res 112:250–253
Vachtsevanos L, Hayden L, Desai AS et al (2014) Management of proximal humerus fractures in adults. World J Orthop 5:685–693
Yahuaca BI, Simon P, Christmas KN et al (2020) Acute surgical management of proximal humerus fractures: ORIF vs. hemiarthroplasty vs. reverse shoulder arthroplasty. J Shoulder Elb Surg 7S:S32–S40
Chalmers PN, Slikker W 3rd, Mall NA et al (2014) Reverse total shoulder arthroplasty for acute proximal humeral fracture: comparison to open reduction-internal fixation and hemiarthroplasty. J Shoulder Elb Surg 2:197–204
Chivot M, Lami D, Bizzozero P et al (2019) Three- and four-part displaced proximal humeral fractures in patients older than 70 years: reverse shoulder arthroplasty or nonsurgical treatment? J Shoulder Elb Surg 2:252–259
Ferrel JR, Trinh TQ, Fischer RA (2015) Reverse total shoulder arthroplasty versus hemiarthroplasty for proximal humeral fractures: a systematic review. J Orthop Trauma 1:60–68
Gupta AK, Harris JD, Erickson BJ et al (2015) Surgical management of complex proximal humerus fractures-a systematic review of 92 studies including 4500 patients. J Orthop Trauma 1:54–59
Solberg BD, Moon CN, Franco DP et al (2009) Surgical treatment of three and four-part proximal humeral fractures. J Bone Jt Surg Am 7:1689–1697
Handoll H H G, Brorson S (2015) Interventions for treating proximal humeral fractures in adults. Cochrane Database Syst Rev CD000434
Helmy N, Hintermann B (2006) New trends in the treatment of proximal humerus fractures. Clin Orthop Relat Res 442:100–108
Rangan A, Handoll H, Brealey S et al (2015) Surgical vs nonsurgical treatment of adults with displaced fractures of the proximal humerus: the PROFHER randomized clinical trial. JAMA 313(10):1037–1047
Huttunen TT, Launonen AP, Pihlajamäki H et al (2012) Trends in the surgical treatment of proximal humeral fractures—a nationwide 23-year study in Finland. BMC Musculoskelet Disord 13:261
Fjalestad T, Hole MØ, Jørgensen JJ et al (2010) Health and cost consequences of surgical versus conservative treatment for a comminuted proximal humeral fracture in elderly patients. Injury 1(6):599–605
Launonen AP, Sumrein BO, Reito A et al (2016) Operative versus non-operative treatment for 2-part proximal humerus fracture: a multicenter randomized controlled trial. PLoS Med 7:e1002855
Brorson S, Olsen BS, Frich LH et al (2009) Effect of osteosynthesis, primary hemiarthroplasty, and non-surgical management for displaced four-part fractures of the proximal humerus in elderly: a multi-centre, randomised clinical trial. Trials 10(1):1–5
Beks RB, Ochen Y, Frima H et al (2018) Operative versus nonoperative treatment of proximal humeral fractures: a systematic review, meta-analysis, and comparison of observational studies and randomized controlled trials. J Shoulder Elb Surg 8:1526–1534
Harris PA, Taylor R, Thielke R et al (2009) Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 2:377–381
Harris PA, Taylor R, Minor BL et al (2019) The RED Cap consortium: building an international community of software platform partners. J Biomed Inform 95:103208
Karl JW, Olson PR, Rosenwasser MP (2015) The Epidemiology of Upper Extremity Fractures in the United States, 2009. J Orthop Trauma 8:e242–e244
Baudi P, Campochiaro G, Serafini F et al (2014) Hemiarthroplasty versus reverse shoulder arthroplasty: comparative study of functional and radiological outcomes in the treatment of acute proximal humerus fracture. Musculoskelet Surg Suppl 1:19–25
Gradl G, Knobe M, Pape H-C et al (2015) Decision making in displaced fractures of the proximal humerus: fracture or surgeon based? Int Orthop 2:329–334
Ansari U, Adie S, Harris IA et al (2011) Practice variation in common fracture presentations: a survey of orthopaedic surgeons. Injury 4:403–407
Okike K, Lee OC, Makanji H et al (2013) Factors associated with the decision for operative versus non-operative treatment of displaced proximal humerus fractures in the elderly. Injury 4:448–455
Walters JM, Ahmadi S (2020) High-energy proximal humerus fractures in geriatric patients: a review. Geriatr Orthop Surg Rehabil 11:2151459320971568
Dillon MT, Inacio MCS, Burke MF et al (2013) Shoulder arthroplasty in patients 59 years of age and younger. J Shoulder Elb Surg 10:1338–1344
Slobogean GP, Johal H, Lefaivre KA et al (2016) A scoping review of the proximal humerus fracture literature. BMC Musculoskelet Disord 112:1–10
Hodgson SA, Mawson SJ, Saxton JM et al (2007) Rehabilitation of two-part fractures of the neck of the humerus (two-year follow-up). J Shoulder Elb Surg 2:143–145
Lefevre-Colau MM, Babinet A, Fayad F et al (2018) Immediate mobilization compared with conventional immobilization for the impacted nonoperatively treated proximal humeral fracture: a randomized controlled trial. J Bone Jt Surg Am 12:2582–2590
Court-Brown CM, Cattermole H, McQueen MM (2004) Impacted valgus fractures(B1.1) of the proximal humerus: the results of non-operative treatment. J Bone Jt Surg 84(4):504–508
Martínez R, Santana F, Pardo A et al (2021) One versus 3-week immobilization period for nonoperatively treated proximal humeral fractures: a prospective randomized trial. J Bone Jt Surg Am 103(16):1491–1498
Leyshon RL (1984) Closed treatment of fractures of the proximal humerus. Acta Orthop Scand 55(1):48–51
Murray IR, Amin AK, White TO et al (2011) Proximal humeral fractures: current concepts in classification, treatment and outcomes. J Bone Jt Surg Br 93(1):1–11
Brorson S, Alispahic N, Bahrs C et al (2019) Complications after non-surgical management of proximal humeral fractures: a systematic review of terms and definitions. BMC Musculoskelet Disord 20(1):91
Neer CS (1974) Displaced proximal humeral fractures: part II treatment of three-part and four-part displacement. J Bone Jt Surg Am 52(6):1090–1103
Teunis T, Janssen SJ, Guitton TG et al (2010) Surgeon personality is associated with recommendation for operative treatment. Hand 10(4):779–784
Acknowledgements
The authors acknowledge the help of Julie Agel, ATC. The authors would like to acknowledge and thank all of the members of the OTA Evidence Based Quality, Value & Safety Committee: Alex Benedick, MD; Ryan K. Harrison, MD; Michael Leslie, DO; Anna N. Miller, MD; Gudrun E. Mirick, MD; William M. Reisman, MD. The authors would also like to acknowledge and thank all of the members of the ASES Multicenter Taskforce on Proximal Humerus Fractures: Joseph A. Abboud, M.D.; Luke S. Austin, M.D.; Jonathan D. Barlow, M.D.; N. Douglas Boardman III, M.D.; Kamal I. Bohsali, M.D.; Shannon R. Carpenter, M.D.; Patrick J. Denard, M.D.; Brody A. Flanagin, M.D.; Grant E. Garrigues, M.D.; Andrew Green, M.D.; Heinz R. Hoenecke Jr, M.D.; J. Gabriel Horneff III, M.D.; Joseph P. Iannotti, M.D.; Scott G. Kaar, M.D.; David Kovacevic, M.D.; John E. Kuhn, M.D.; Mark D. Lazarus, M.D.; Donald H. Lee, M.D.; David Kovavecik M.D.; Surena Namdari, M.D.; Gregory P. Nicholson, M.D.; E. Scott Paxton, M.D.; Brent A. Ponce, M.D.; Matthew L. Ramsey, M.D.; Gerald R. Williams, M.D
Funding
This study received no outside funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Joseph J. King is a consultant for Exactech, Inc. Catherine Fedorka is a consultant for Stryker. The other authors, their immediate families, and any research foundations with which they are affiliated have not received any financial payments or other benefits from any commercial entity related to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Reed, L.A., Hao, K.A., Patch, D.A. et al. How do surgeons decide when to treat proximal humerus fractures with operative versus nonoperative management?. Eur J Orthop Surg Traumatol 33, 3683–3691 (2023). https://doi.org/10.1007/s00590-023-03610-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-023-03610-1