Abstract
Purpose
Secondary displacement of traumatic ankle fractures with subsequent soft-tissue breakdown is a troublesome issue after inappropriate conservative treatment among non-compliant diabetic patients with severe peripheral neuropathy. This study was conducted to evaluate the results of a less-invasive arthrodesis procedure as an alternative to osteosynthesis in these complex scenarios.
Methods
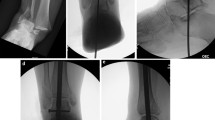
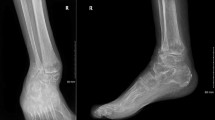
A total of 46 diabetics, who underwent fluoroscopy-assisted trans-calcaneal retrograde nailing-based ankle arthrodesis between 2012 and 2018 for salvaging secondary-displaced diabetic ankle fractures in their insensate feet, were evaluated in this retrospective study. All fractures were associated with uninfected mechanical ulcers overlying malleoli, without Charcot changes, after failed conservative cast immobilization. The patients (mean age: 52.52 ± 3.70 years; 18 males; 46 feet) were evaluated radiologically for union and clinically for limb salvage, modified American Orthopedic Ankle and Foot Scale (AOAFS), and the overall subjective patients' satisfaction.
Results
The mean follow-up was 29.5 ± 3.1 months. All ulcers have healed with local care only with 100% limb salvage. Four patients experienced minor wound healing problems at posterior heel, and another one developed acute Charcot changes that was successfully managed by offloading and repeat surgery. Forty patients (86.96%) had fully consolidated fusions with a mean time to fusion 15.78 ± 2.58 weeks, while the other six cases had stable fibrous-union. At the final follow-up, the mean modified-AOFAS was 76.85 ± 6.0 from 86 total points. All, but four patients (91.30%) were completely satisfied while the other four patients were partially satisfied.
Conclusions
The presented less-invasive arthrodesis technique is reproducible and effective alternative for salvaging unstable diabetic ankle fractures in the insensate feet when standard surgical procedures would be more risky.
Level of evidence: IV, retrospective case series




Similar content being viewed by others
Data availability
The datasets used and analyzed during this study are available from the corresponding author on reasonable request.
References
Chaudhary SB, Liporace FA, Gandhi A et al (2008) Complications of ankle fracture in patients with diabetes. J Am Acad Orthop Surg 16(3):159–170. https://doi.org/10.5435/00124635-200803000-00007
Ayoub MA (2008) Ankle fractures in diabetic neuropathic arthropathy: can tibiotalar arthrodesis salvage the limb? J Bone Joint Surg Br 90(7):906–914. https://doi.org/10.1302/0301-620X.90B7.20090
Mehta SS, Rees K, Cutler L, Mangwani J (2014) Understanding risks and complications in the management of ankle fractures. Indian J Orthop 48(5):445–452. https://doi.org/10.4103/0019-5413.139829
Yee J, Pillai A, Ferris L. (2014) Diabetic ankle fractures: a review of the literature and an introduction to the adelaide fracture in the diabetic ankle algorithm and score. Bio Med Res Int. doi:https://doi.org/10.1155/2014/153146.
Jani MM, Ricci WM, Borrelli JJr, et al. (2003) A protocol for treatment of unstable ankle fractures using trans-articular fixation in patients with diabetes mellitus and loss of protective sensibility. Foot Ankle Int 24(11): 838–44. doi: https://doi.org/10.1177/107110070302401106.
Perry MD, Taranow WS, Manoli A 2nd et al (2005) Salvage of failed neuropathic ankle fractures: use of large-fragment fibular plating and multiple syndesmotic screws. J Surg Orthop Adv 14(2):85–91
Facaros Z, Ramanujam CL, Stapleton JJ (2010) Combined circular external fixation and open reduction internal fixation with pro-syndesmotic screws for repair of a diabetic ankle fracture. Diabet Foot Ankle. https://doi.org/10.3402/dfa.v1i0.5554.
Kong C, Kolla L, Wing K et al (2014) Arthroscopy-assisted closed reduction and percutaneous nail fixation of unstable ankle fractures: description of a minimally invasive procedure. Arthrosc Tech 3(1):e181–e184. https://doi.org/10.1016/j.eats.2013.09.018
Noonan T, Paxinos O, Pinzur MS et al (2005) Tibio-talo-calcaneal arthrodesis with a retrograde intramedullary nail: a biomechanical analysis of the effect of nail length. Foot Ankle Int 26(4):304–308. https://doi.org/10.1177/107110070502600406
Pinzur MS, Noonan T (2005) Ankle arthrodesis with a retrograde femoral nail for Charcot ankle arthropathy. Foot Ankle Int 26(7):545–549. https://doi.org/10.1177/107110070502600709
Caravaggi C, Cimmino M, Caruso S et al (2006) Intramedullary compressive nail fixation for the treatment of severe Charcot deformity of the ankle and rear foot. J Foot Ankle Surg 45(1):20–24. https://doi.org/10.1053/j.jfas.2005.10.003
Goebel M, Gerdesmeyer L et al (2006) Retrograde intramedullary nailing in tibio-talo-calcaneal arthrodesis: a short-term. Prospective Study J Foot Ankle Surg 45(2):89–96. https://doi.org/10.1053/j.jfas.2005.12.001
Dalla Paola L, Volpe A, Varotto D et al (2007) Use of a retrograde nail for ankle arthrodesis in Charcot neuroarthropathy: a limb salvage procedure. Foot Ankle Int 28(9):967–970. https://doi.org/10.3113/FAI.2007.0967
Fetter NL, DeOrio JK (2012) Posterior approach with fibular preservation for tibio-talo-calcaneal arthrodesis with an intramedullary nail. Foot Ankle Int 33(9):746–749. https://doi.org/10.3113/FAI.2012.0746
ElAlfy B, Ali AM, Fawzy SI (2017) Ilizarov external fixator versus retrograde intramedullary nailing for ankle joint arthrodesis in diabetic charcot neuroarthropathy. J Foot Ankle Surg 54(2):309–313. https://doi.org/10.1053/j.jfas.2016.10.014
Mulligan RP, Adams S, Easley ME et al (2017) Comparison of posterior approach with intramedullary nailing versus lateral transfibular approach with fixed-angle plating for tibio-talo-calcaneal arthrodesis. Foot Ankle Int 38(12):1343–1348. https://doi.org/10.1177/1071100717731728
DeVries JG, Berlet GC, Hyer CF (2013) Predictive risk assessment for major amputation after tibio-talo-calcaneal arthrodesis. Foot Ankle Int 34(6):846–850. https://doi.org/10.1177/1071100712472488
Mader K, Verheyen CC, Gausepohl T et al (2007) Minimally invasive ankle arthrodesis with a retrograde locking nail after failed fusion. Strategies Trauma Limb Reconstr 2(1):39–47. https://doi.org/10.1007/s11751-007-0018-4
Bevernage BD, Deleu PA, Maldague P et al (2010) Technique and early experience with posterior arthroscopic tibio-talo-calcaneal arthrodesis. Orthop Traumatol Surg Res 96(4):469–475. https://doi.org/10.1016/j.otsr.2010.03.012
Hammit MD, Hobgood ER, Tarquinio TA (2006) Midline posterior approach to the ankle and hind-foot. Foot Ankle Int 27(9):711–715. https://doi.org/10.1177/107110070602700910
Kitaoka HB, Alexander IJ, Adelaar RS et al (1994) Clinical rating systems for the ankle-hind-foot, hallux, and lesser toes. Foot Ankle Int 15(7):349–355. https://doi.org/10.1177/107110079401500701
Guyton GP (2005) An analysis of iatrogenic complications from the total contact cast. Foot Ankle Int 26(11):903–907. https://doi.org/10.1177/107110070502601101
Wukich DK, Belczyk RJ, Burns PR et al (2008) Complications encountered with circular ring fixation in persons with diabetes mellitus. Foot Ankle Int 29(10):994–1000. https://doi.org/10.3113/FAI.2008.0994
Duan X, Yang L, Yin L (2016) Arthroscopic arthrodesis for ankle arthritis without bone graft. J Orthop Surg Res 11(1):154. https://doi.org/10.1186/s13018-016-0490-y
Means KR, Parks BG, Nguyen A et al (2006) Intramedullary nail fixation with posterior-to-anterior compared to transverse distal screw placement for tibio-talo-calcaneal arthrodesis: a biomechanical investigation. Foot Ankle Int 27(12):1137–1142. https://doi.org/10.1177/107110070602701221
Bazarov I, Peace RA, Lagaay PM et al (2017) Early protected weight-bearing after ankle fractures in patients with diabetes mellitus. J Foot Ankle Surg 56(1):30–33. https://doi.org/10.1053/j.jfas.2016.09.010
Acknowledgements
Not applicable.
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Ethical approval
All procedures performed were in accordance with the ethical standards of our institutional ethical committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consents were obtained from all patient before interventions. The study was approved by the ethical research committee of the Faculty of Medicine—Tanta University under the code: 32423.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
El-Tantawy, A., Atef, A. & Samy, A. Trans-calcaneal retrograde nailing for secondary-displaced traumatic ankle fractures in diabetics with insensate feet: a less-invasive salvage-arthrodesis technique. Eur J Orthop Surg Traumatol 32, 37–46 (2022). https://doi.org/10.1007/s00590-021-02898-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-02898-1