Abstract
Purpose
This study was performed to assess the effectiveness of the combined intravenous and intra-articular tranexamic acid (TXA) regimen in total knee arthroplasty (TKA).
Methods
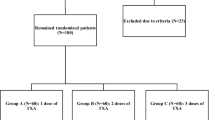
The perioperative blood loss in 75 consecutive patients undergoing unilateral TKA that received both 1000 mg of TXA intravenously and 1000 mg of intra-articular TXA (combined TXA group) was compared with a consecutive series of 77 patients that received 1000 mg of TXA intravenously (intravenous TXA group). An additional 1000 mg of intravenous TXA was administered 6 h after the initial administration in both groups. Neither a pneumatic tourniquet nor drain was used. The primary outcome was the perioperative blood loss at 3 days after TKA calculated using the blood volume and change in haemoglobin from the preoperative value.
Results
The perioperative blood loss was significantly lower in the combined TXA group at 3 days after TKA than the intravenous TXA group (686 ± 303 vs. 830 ± 317 mL; 95% CI 44–244 mL; p = 0.0049). The perioperative blood loss was also lower in the combined TXA group at 1 and 7 days after TKA (374 ± 265 vs. 459 ± 226 mL; 95% CI 7–165 mL; p = 0.034 and 751 ± 320 vs. 871 ± 327 mL; 95% CI 16–224 mL; p = 0.024, respectively). No thrombotic events were observed during the study periods.
Conclusions
Combined intra-articular and intravenous TXA regimen significantly reduced perioperative blood loss compared with only intravenous TXA until 7 days after TKA.

Similar content being viewed by others
References
Su EP, Su S (2016) Strategies for reducing peri-operative blood loss in total knee arthroplasty. Bone Joint J 98-B(1 Suppl A):98–100
Poeran J, Rasul R, Suzuki S, Danninger T, Mazumdar M, Opperer M, Boettner F, Memtsoudis SG (2014) Tranexamic acid use and postoperative outcomes in patients undergoing total hip or knee arthroplasty in the United States: retrospective analysis of effectiveness and safety. BMJ 349:g4829
Aggarwal AK, Singh N, Sudesh P (2016) Topical vs intravenous tranexamic acid in reducing blood loss after bilateral total knee arthroplasty: a prospective study. J Arthroplast 31:1442–1448
Goyal N, Chen DB, Harris IA, Rowden NJ, Kirsh G, MacDessi SJ (2017) Intravenous vs intra-articular tranexamic acid in total knee arthroplasty: a randomized, double-blind trial. J Arthroplast 32:28–32
Nielsen CS, Jans Ø, Ørsnes T, Foss NB, Troelsen A, Husted H (2016) Combined intra-articular and intravenous tranexamic acid reduces blood loss in total knee arthroplasty: a randomized, double-blind, placebo-controlled trial. J Bone Joint Surg Am 98:835–841
Good L, Peterson E, Lisander B (2003) Tranexamic acid decreases external blood loss but not hidden blood loss in total knee replacement. Br J Anaesth 90:596–599
Iwai T, Tsuji S, Tomita T, Sugamoto K, Hideki Y, Hamada M (2013) Repeat-dose intravenous tranexamic acid further decreases blood loss in total knee arthroplasty. Int Orthop 37:441–445
Tsukada S, Wakui M (2017) Combined intravenous and intra-articular tranexamic acid in simultaneous bilateral total knee arthroplasty without tourniquet use. JBJS Open Access 2:e0002
Tsukada S, Wakui M (2018) Continuing versus discontinuing antiplatelet drugs, vasodilators, and/or cerebral ameliorators on perioperative total blood loss in total knee arthroplasty without pneumatic tourniquet. Arthroplast Today 4:89–93
Nadler SB, Hidalgo JH, Bloch T (1962) Prediction of blood volume in normal human adults. Surgery 51:224–232
Mantz J, Samama CM, Tubach F et al (2011) Impact of preoperative maintenance or interruption of aspirin on thrombotic and bleeding events after elective non-cardiac surgery: the multicentre, randomized, blinded, placebo-controlled, STRATAGEM trial. Br J Anaesth 107:899–910
Wells PS, Anderson DR, Bormanis J, Guy F, Mitchell M, Gray L, Clement C, Robinson KS, Lewandowski B (1997) Value of assessment of pretest probability of deep-vein thrombosis in clinical management. Lancet 350:1795–1798
Adravanti P, Di Salvo E, Calafiore G, Vasta S, Ampollini A, Rosa MA (2018) A prospective, randomized, comparative study of intravenous alone and combined intravenous and intraarticular administration of tranexamic acid in primary total knee replacement. Arthroplast Today 4:85–88
Jansen JA, Lameijer JRC, Snoeker BAM (2017) Combined intravenous, topical and oral tranexamic acid administration in total knee replacement: evaluation of safety in patients with previous thromboembolism and effect on hemoglobin level and transfusion rate. Knee 24:1206–1212
Lin SY, Chen CH, Fu YC, Huang PJ, Chang JK, Huang HT (2015) The efficacy of combined use of intraarticular and intravenous tranexamic acid on reducing blood loss and transfusion rate in total knee arthroplasty. J Arthroplast 30:776–780
Horrow JC, Van Riper DF, Strong MD, Brodsky I, Parmet JL (1991) Hemostatic effects of tranexamic acid and desmopressin during cardiac surgery. Circulation 84:2063–2070
Mutsuzaki H, Ikeda K (2012) Intra-articular injection of tranexamic acid via a drain plus drain-clamping to reduce blood loss in cementless total knee arthroplasty. J Orthop Surg Res 7:32
Kelly J, Rudd A, Lewis RR, Hunt BJ (2002) Plasma D-dimers in the diagnosis of venous thromboembolism. Arch Intern Med 162:747–756
Morton V, Torgerson DJ (2003) Effect of regression to the mean on decision making in health care. BMJ 326:1083–1084
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they did not receive and will not receive any benefits or funding from any commercial party related directly or indirectly to the subject of this article.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Iseki, T., Tsukada, S., Wakui, M. et al. Intravenous tranexamic acid only versus combined intravenous and intra-articular tranexamic acid for perioperative blood loss in patients undergoing total knee arthroplasty. Eur J Orthop Surg Traumatol 28, 1397–1402 (2018). https://doi.org/10.1007/s00590-018-2210-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-018-2210-2