Abstract
Purpose
We aimed to evaluate the effect of cervical disc herniation (CDH) and lumbar disc herniation (LDH) on female sexual functioning before and after surgical intervention.
Methods
The current study was conducted from February 2022 to February 2023. A total of 100 sexually active female patients in their reproductive phase who were diagnosed with CDH and LDH based on physical examination and previous magnetic resonance imaging (MRI) results, as well as 50 healthy females, were enrolled. The female subjects were evaluated using the validated Arabic version of the female sexual function index (ArFSFI), a 0 to 10 visual analogue scale (VAS), the Oswestry disability index (ODI) and Beck’s depression index (BDI).
Results
The baseline ArFSFI domains and total scores were greatest in the controls, followed by the CDH group. The ArFSFI domains and total scores were greatest in the control group, followed by the postoperative ArFSFI domains and total scores in the cervical group. The variations in satisfaction, pain, and overall ArFSFI ratings were significant across research groups. The difference in desire, arousal, lubrication, and orgasm was substantial in the lumbosacral group, but there were no significant changes between the cervical and control groups. Postoperatively, ArFSFI domains and overall scores improved in both of the cervical and lumbar groups. Both research groups’ ODI score and grade improved after surgery. Finally, both groups’ BDI score and grade improved after surgery.
Conclusion
Female sexual dysfunctions caused by CDH and LDH improved considerably after surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pain is caused by degenerative spine disease, which affects around 80% of the population over their entire lifespan [1]. The sexual function is extremely important for people’s lives. It is not merely a reproductive function, but also a crucial component in maintaining interpersonal connections and self-confidence. The cessation of sexual activity for whatever reason, might lead to major concerns among partners [2]. Body movements with developing chronic pain disorders can greatly limit sexual activity. Other contributing factors leading to sexual dysfunction include sadness produced by chronic pain and the medications utilized. All of these negative variables combine to form a vicious circle between the person in pain and their husband or wife [3]. Pain and function improve significantly following spine surgery, based on many patient-reported outcome measures [4, 5]. Sexual function is a crucial factor to consider when evaluating functional results following spine surgery. Despite the fact that sexual dysfunction is common among people with spinal cord injury, sexual health counseling is not commonly provided as a part of medical care [6]. Furthermore, sexual function is not often discussed during adult spinal deformity (ASD) repair surgery patient visits [7, 8]. One explanation might be that the issue of “sexual life” has been postponed [9]. Furthermore, there is a paucity of reliable data since studies rarely evaluate sexual function efficiently as an essential endpoint. As a result, healthcare providers are unable to establish expectations for postoperative sexual function or the known surgical risks [10]. Back pain was found to have a high correlation with decreased sexual activity among both sexes [11]. Besides that, 55% of men and 84% of women reported sexual dysfunctions associated with the onset of low back pain. In contrast, patients’ sexual function improved significantly after surgery for single-level lumbar disc herniation (LDH) [12, 13]. Nonetheless, a recent research found that 39% of individuals experienced worsened sexual function after cervical spine surgery, with only 5% reporting improved performance [14]. Along with that, Hamilton et al. found a 42% incidence of significant sexual dysfunction postoperatively in their study [15]. The greatest cause of impaired sexual function, however, was a lack of a sexual partner. In addition, despite a mean age of 70 years and substantial spinopelvic instrumentation, around 40% of patients reported no or just minor sexual problems. Importantly, there was no preoperative assessment of sexual function for comparison. As a result, the effect of ASD surgery on patient sexual function was inconclusive [2]. Jordon stated that the prevalence of LDH in Finland and Italy was 1–3%, which was a two times higher incidence for men aged 30–59 years compared to women [16]. Deyo et al. [17] suggested that the incidence of LDH in America would project to 1–2%. Radhakrishnan et al. [18] mentioned that the annual incidence of cervical disc herniation (CDH) in Rochester and Minnesota was around 18.6 of 100,000 individuals between 1976 and 1990 reaching its peak in their 60s.
On the other hand, Kim et al. [19] stated that the diagnosis of symptomatic CDH and LDH among individuals increased with age together with incidence of these diseases being higher in women compared to men. Notably, there are different therapeutic approaches for CDH including, McKenzie approach [20], minimally invasive spinal surgery [21] as well as the anterior approach for removing ruptured cervical discs [22]. While there are different approaches for LDH starting from transdural resection to the conventional approach [23, 24] followed by microsurgery and endoscopic and percutaneous surgery especially among men in their forties [25, 26]. The current study is one of the first to evaluate the impact of CDH and LDH on female sexual function as well as the effect of surgical correction of both conditions on female sexual function.
Patients and methods
Study design and settings and participants
From February 2022 to February 2023, the study was conducted at the outpatient clinic of Beni-Suef university hospital. Notably, it complies with the Helsinki Declaration 2013, and it was approved by the institutional review board [27]. The approval number of the institutional review board was FMBSUREC/09012022. A total of 100 sexually active female patients in their reproductive period, who were diagnosed with CDH or LDH based on physical examination and prior MRI results, as well as 50 age-matched healthy females, were enrolled. Furthermore, all patients were evaluated two months following the procedure.
Determination of sample size
T tests—means and analysis: A priori were used to compute the required sample size using the following inputs: tail(s) = two, effect size d = 0.73, α err prob = 0.05, power (1-β err prob) = 0.95, and allocation ratio N2/N1 = 1. The outputs were non-centrality parameter δ = 3.6500000, critical t = 1.9844675Df = 98. Thus, sample size groups 1 and 2 were set to be 50 each and a total sample size was 100 at actual power = 0.9509402.
Inclusion criteria
Female patients in their reproductive years with severe CDH or LDH for at least 6 months, as diagnosed clinically and by MRI and who were scheduled to have the herniation corrected surgically were enrolled.
Exclusion criteria
Subjects with a history of uncontrolled chronic illness, a previous pelvic surgery, a history of antidepressant, anxiolytic, or anticonvulsant medications use, a history of a major psychiatric disorder, urinary and fecal incontinence, or a limited range of motion in the hand, knee, or hip joints were all excluded. In addition, chronic alcohol consumption, oral or vaginal estrogen medication, and loss of motor strength owing to a disc herniation or any other neurological condition, as well as cauda equina syndrome, were all ruled out of the study.
All the participants were exposed to the following:
All participants were subjected to proper history taking, and underwent a full physical examination. Besides that, the socioeconomic characteristics of included subjects were collected. All questionnaires were given to each patient in a room where she was alone with a female physician. As such, an appropriate setting for patients to complete the questionnaire has been established. Patients were told that their personal information would be kept confidential. Only the questions that the patient did not understand were clarified. The validated Arabic version of the female sexual function Index (ArFSFI) was used to assess the participants’ sexual function [28]. Furthermore, the degree of pain was assessed using a 0 to 10 Visual analogue scale (VAS) [29]. Moreover, the Oswestry disability index (ODI) was used to assess the significance of sexuality and disability in individuals with CDH as well as LDH [30]. It should be noted that the ODI is the most extensively used functional status questionnaire in the literature, with proven reliability and validity. In addition, Beck’s depression index (BDI) is a dependable and accurate method for assessing depression symptoms in a society. BDI is a 21- item index including items about pessimism, sense of failure, dissatisfaction, a sense of guilt, restlessness, fatigue, decreased appetite, indecisiveness, sleep disorders and social withdrawal [31]. The questionnaires were given to each patient before and after surgery.
Statistical methods
All collected data were coded, tabulated, and statistically analyzed using IBM SPSS statistics software version 28.0, IBM Corp., Chicago, USA, 2021. Quantitative data were evaluated for normality using the Shapiro–Wilk test, then represented as mean SD (standard deviation), minimum and maximum of the range, and compared using the ANOVA test (three independent groups) and the paired t-test (paired data). Qualitative data are expressed as a number and a percentage, and it is then compared using the Chi-square test, Fisher’s exact test, and the marginal homogeneity test (two dependent multinomial variables). For post hoc comparisons, the Bonferroni test is utilized. The threshold of significance was set at p-value 0.050, which was considered significant; otherwise, it was considered non-significant.
Results
There were no statistically significant differences between the analyzed groups in terms of age, BMI, or parity as shown in (Table 1). The controls had the highest baseline ArFSFI domains and total scores, followed by the CDH group, and the lowest in the lumbosacral group. Furthermore, the variations in desire, arousal, pleasure, pain, and overall ArFSFI ratings across research groups were statistically significant. The lumbosacral group had substantially lower baseline lubrication and orgasm ratings than the cervical group and controls. In addition, the cervical group had substantially higher postoperative ArFSFI domains and overall scores than the lumbosacral group. The differences in satisfaction, pain and total ArFSFI scores were statistically significant between the study groups. Finally, desire, arousal, lubrication and orgasm significantly improved postoperatively in the lumbosacral group (Table 2). On the other hand, the controls had considerably lower baseline ODI than the other groups. Moreover, the ODI grade improved considerably postoperatively in both groups with disc herniation (Table 3). Similarly, the controls had considerably lower baseline BDI than the other groups as shown in (Table 4). Concerning the postoperative BDI grading, it was found to be improved significantly among both groups with disc herniation (Table 4). Finally, in both groups, the ArFSFI domains and total scores, ODI score and grade, and BDI score and grade improved significantly postoperatively (Tables 5, 6, 7).
Discussion
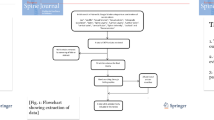
The present study evaluated 125 subjects for eligibility and enrolled 100 patients (50 in each group). Based on the inclusion criteria, sixteen individuals were excluded from the study; while, nine patients refused to take part. Finally, the study was based on data from 100 sexually active female patients in their reproductive years that were divided equally into two groups with CDH and LDH as well as 50 healthy age-matched females. The current study found that the controls had the highest baseline ArFSFI domains and total scores, followed by the CDH group, and the lowest in the lumbosacral group. Furthermore, the cervical group’s postoperative ArFSFI domains and overall scores were considerably greater than the lumbosacral group’s. Notably, desire, arousal, lubrication and orgasm improved dramatically after surgery in the lumbosacral group. Postoperative ODI and BDI grading improved significantly in both groups. In the same context, Akbas et al. [12] found a large rise in the frequency of intercourse as well as a significant decrease in the description of any form of sexual difficulty following LDH surgery. However, they reported no difference in levels of sexual desire. Similarly, Elsharkawy et al. [13] found that LDH surgery improved sexual function. However, it should be noted that the majority of participants in the previously mentioned study did not observe a significant change in their sexual life, rating it the same as before surgery.
Similarly, Daniels et al. (2020) demonstrated that the greatest importance of surgical correction for ASD was evidenced by significant improvement in the ODI, scoliosis research society-22r total score, and sagittal vertical axis at 2-year postoperative follow-up [2]. LDH is a prevalent disorder that can result in social and economic losses as well as a decrease in people’s quality of life. One of the most well-known causes of low back pain is LDH [32]. Neurological deficits, acute pain and restrictions in physical activity are common consequences of disc degeneration, which can lead to a reduced quality of life or apathy or depression. All of these factors may impact not just an individual’s social life, but also their sexual life and interactions with their partners [33]. The correlation between chronic low back pain, quality of life and sexual function is equally crucial to both sexes. Furthermore, the presence of musculoskeletal problems leads to sexual act limitations owing to discomfort, immobility, and diminished muscular strength, resulting in lower sexual excitement and difficulties in positioning for the intercourse. Low back pain, in particular, has a negative influence on sexual activity because it causes discomfort during sexual intercourse, which reduces the frequency of sexual intercourse and disturbs feelings in the relationship with the partner resulting in a lack of desire or sexual activity [2]. On the other hand, Moscicki et al. [34] reported that surgery did not alleviate perianal hypoesthesia and diminished sensation in the sacral region associated with L5-S1 disc pathology. In the same context, Keefe et al. [14] found significant difficulty in the postoperative period after cervical spine surgery, with 39% of patients reporting impaired sexual function. Notable limitations of the study include a lower sample size compared to previously mentioned studies and a lack of multicentric research. Larger, multicenter studies with both males and females are needed for greater significance. The new study’s prospective design, on the other hand, enhances the findings. Moreover, non-validated Arabic indices of Beck’s depression and Oswestry disability were utilized to assess the patients.
Conclusion
Female Sexual dysfunctions caused by CDH and LDH resolved considerably after surgery. Furthermore, physical activity constraints substantially improved following surgery resulting in an improvement in quality of life. The current study emphasizes the relevance of surgical repair of disc herniation to the patients’ sexual health outcomes.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Rubin DI (2007) Epidemiology and risk factors for spine pain. Neurol Clin 25(2):353–371
Daniels AH, Reid D, Durand W, Disilvestro K, Hamilton DK, Passias P et al (2020) Sexual dysfunction secondary to lumbar stiffness in adult spinal deformity patients before and after long-segment spinal fusion. World Neurosurgery 139:e474–e479. https://doi.org/10.1016/j.wneu.2020.04.033. (Epub 2020 Apr 18 PMID: 32311559)
Chan AK, Bisson EF, Fu K-M, Park P, Robinson LC, Bydon M et al (2020) Sexual dysfunction: Prevalence and prognosis in patients operated for degenerative lumbar spondylolisthesis. Neurosurgery 87(2):200–210
Zanoli G, Strömqvist B, Jönsson B (2001) Visual analog scales for interpretation of back and leg pain intensity in patients operated for degenerative lumbar spine disorders. Spine (Phila Pa 1976) 26(21):2375–2380
Carreon LY, Glassman SD, Campbell MJ, Anderson PA (2010) neck disability index, short form-36 physical component summary, and pain scales for neck and arm pain: the minimum clinically important difference and substantial clinical benefit after cervical spine fusion. Spine J 10(6):469–474
Korse NS, Nicolai MP, Both S, Vleggeert-Lankamp CL, Elzevier HW (2016) Discussing sexual health in spinal care. Eur Spine J 25(3):766–773
Wimberly YH, Hogben M, Moore-Ruffin J, Moore SE, Fry-Johnson Y (2006) Sexual history-taking among primary care physicians. J Natl Med Assoc 98(12):1924–1929
Marwick C (1999) Survey says patients expect little physician help on sex. JAMA 281(23):2173–2174
Temple-Smith M, Hammond J, Pyett P, Presswell N (1996) Barriers to sexual history taking in general practice. AustFam Physician 25(9 Suppl 2):S71–S74
Malik AT, Jain N, Kim J, Khan SN, Yu E (2018) Sexual activity after spine surgery: a systematic review. Eur Spine J 27(10):2395–2426
Maigne JY, Chatellier G (2001) Assessment of sexual activity in patients with back pain compared with patients with neck pain. ClinOrthopRelat Res 385:82–87
Akbaş NB, Dalbayrak S, Külcü DG, Yilmaz M, Yilmaz T, Naderi S (2010) Assessment of sexual dysfunction before and after surgery for lumbar disc herniation. J Neurosurg Spine 13(5):581–586
Elsharkawy AE, Lange B, Caldas F, Alabbasi AH, Klassen PD (2018) Predictors and long-term outcome of sexual function after surgical treatment for single-level lumbar disk herniation among patients in a german spine center. Clin Spine Surg 31(8):356–362
Keefe MK, Zygourakis CC, Theologis AA et al (2017) Sexual function after cervical spine surgery: independent predictors of functional impairment. J ClinNeurosci 36:94–101
Hamilton DK, Smith JS, Nguyen T, Arlet V, Kasliwal MK, Shaffrey CI (2013) Sexual function in older adults following thoracolumbar to pelvic instrumentation for spinal deformity. J Neurosurg Spine 19(1):95–100
Jordon J, Konstantinou K, O’Dowd J (2009) Herniated lumbar disc. BMJ. Clin Evid 209:1118
Deyo RA, Tsui-Wu YJ (1987) Descriptive epidemiology of low-back pain and its related medical care in the United States. Spine 12:264–268 ([CrossRef] [PubMed])
Radhakrishnan K, Kitchy WJ, O’Fallon M, Kurland LT (1994) Epidemiology of cervical radiculopathy: A population-based study from Rochester, Minnesota, 1976 through 1990. Brain 117:325–335 ([CrossRef] [PubMed])
Kim YK, Kang D, Lee I, Kim SY (2018) Differences in the incidence of symptomatic cervical and lumbar disc herniation according to age, sex and national health insurance eligibility: a pilot study on the disease’s association with work. Int J Environ Res Public Health 15(10):2094. https://doi.org/10.3390/ijerph15102094
Edmond SL, Werneke MW, Young M, Grigsby D, McClenahan B, Harris G, McGill T (2020) Cognitive behavioural interventions, and function and pain outcomes among patients with chronic neck pain managed with the McKenzie approach. Musculoskeletal Care 18(1):46–52
Yang B, Xie J, Yin B, Wang L, Fang S, Wan S (2014) Treatment of cervical disc herniation through percutaneous minimally invasive techniques. Eur Spine J 23(2):382–388. https://doi.org/10.1007/s00586-013-3063-3.
Cloward RB (2007) The anterior approach for removal of ruptured cervical disks. J Neurosurg 6:496–511
Love JG (1939) Removal of intervertebral disc without laminectomy. Proc Staff Meet Mayo Clinic 14:800
Sammes RE (1939) Diagnosis of ruptured intervertebral disc without contrast myelography and comment upon recent experience with modified hemilaminectomy for their removal. Yale J Biol Med 11(5):433–435
Vialle LR, Vialle EN, Suárez Henao JE, Giraldo G (2015) LUMBAR DISC HERNIATION Rev Bras Ortop 45(1):17–22. https://doi.org/10.1016/S2255-4971(15)30211-1
Spangfort EV (1972) The lumbar disc herniation. A computer-aided analysis of 2504 operations. Acta Orthop Scand Suppl 142:1–95
World Medical Association (2013) World medical association declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA 310(20):2191–2194
Anis TH, Gheit SA, Saied HS, Al Kherbash SA (2011) Arabic translation of female sexual function Index and validation in an Egyptian population. J Sex Med 8(12):3370–3378
Gould D, Kelly D, Goldstone L, Gammon J (2001) Examining the validity of pressure ulcer risk assessment scales: developing and using illustrated patient simulations to collect the data. J ClinNurs 10(5):697–706
Vianin M (2008) Psychometric properties and clinical usefulness of the oswestry disability index. J Chiropr Med 7(4):161–163. https://doi.org/10.1016/j.jcm.2008.07.001.PMID:19646379;PMCID:PMC2697602
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1961) An inventory for measuring depression. Arch Gen Psychiatry 4:561–571
Akkurt HE, Yilmaz H, YilmazSD, Ordahan B, Şen Z, Gürbüz C, Göksu H (2017) Sexual dysfunction in women with lumbosacral disc disease. J Phys Med Rehabilit Sci 20(1)
Łabuz-Roszak B, Babińska A, Skupiński J, Czech E, Szczygieł J, Wawrzynek W (2018) Sexual quality of life in patients with low back pain and the radiological changes evaluated in magnetic resonance. WiadLek 71(5):1039–1045
Moscicki P, Bachmann GA (2022) Characterization of Female Sexual Dysfunction Associated with Spinal Pathology and Surgery. Sex Med Rev 10(4):493–498
Acknowledgements
The authors would like to thank the neurosurgeons who performed the disc removal operations for the patients. Also, we would like to thank the participants for their cooperation to continue the study.
Funding
Open access funding provided by The Science, Technology & Innovation Funding Authority (STDF) in cooperation with The Egyptian Knowledge Bank (EKB). The current work did not receive any fund.
Author information
Authors and Affiliations
Contributions
SF & NN developed conception and study design as well as drafting the manuscript and critical revision of the data. AAS & MAS & AR & RB recruitment of the cases and performed the statistics. MA evaluation of the cases as well as performed the surgeries for the cases.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the local ethical committee.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
GamalEl Din, S.F., Nabil, N., Alaa, M. et al. Evaluation of the effect of cervical and lumbar disc herniations on female sexual function: a comparative prospective study. Eur Spine J 33, 1391–1397 (2024). https://doi.org/10.1007/s00586-024-08191-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-024-08191-z