Abstract
Purpose
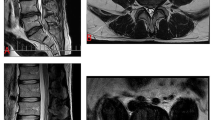
This study aims to report a new distribution pattern of Modic changes (MCs) in patients with lumbar disc herniation (LDH) and investigate the prevalence, correlative factors and clinical outcomes of asymmetric Modic changes (AMCs).
Methods
The study population consisted of 289 Chinese Han patients who were diagnosed with LDH and single-segment MCs from January 2017 to December 2019. Demographic, clinical and imagological information was collected. Lumbar MRI was performed to assess MCs and intervertebral discs. The visual analogue score (VAS) and Oswestry disability index (ODI) were evaluated in patients undergoing surgery preoperatively and at the final follow-up. Correlative factors contributing to AMCs were analysed by multivariate logistic regression.
Results
The study population included 197 patients with AMCs and 92 patients with symmetric Modic changes (SMCs). The incidence of leg pain (P < 0.001) and surgical treatment (P = 0.027) in the AMC group was higher than that in the SMC group. The VAS of low back pain was lower (P = 0.048), and the VAS of leg pain was higher (P = 0.036) in the AMC group than in the SMC group preoperatively. Multivariate logistic regression analysis revealed that leg pain (OR = 2.169, 95% CI = 1.218 ~ 3.864) and asymmetric LDH (OR = 7.342, 95% CI = 4.170 ~ 12.926) were independently associated with AMCs. The receiver operating characteristic curve showed an AUC of 0.765 (P < 0.001).
Conclusion
AMCs were a more common phenomenon than SMCs in this study. The asymmetric and symmetric distribution of MCs was closely related to LDH position. AMCs were related to leg pain and higher pain levels. Surgery can achieve satisfactory clinical improvement for asymmetric and symmetric MCs.





Similar content being viewed by others
Data availability
Data are available on request from the corresponding authors.
Abbreviations
- MCs:
-
Modic changes
- MRI:
-
Magnetic resonance imaging
- LDH:
-
Lumbar disc herniation
- LBP:
-
Low back pain
- BMI:
-
Body mass index
- T1WIs:
-
T1-weighted images
- T2WIs:
-
T2-weighted images
- AMCs:
-
Asymmetric Modic changes
- SMCs:
-
Symmetric Modic changes
- MSU:
-
Michigan State University
- VAS:
-
Visual analogue score
- ODI:
-
Oswestry Disability Index
- OR:
-
Odds ratio
- 95% CI:
-
95% confidence interval
- T2WI-FS:
-
T2-weighted fat suppression images
References
Modic MT, Steinberg PM, Ross JS, Masaryk TJ, Carter JR (1988) Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 166:193–199. https://doi.org/10.1148/radiology.166.1.3336678
Modic MT, Masaryk TJ, Ross JS, Carter JR (1988) Imaging of degenerative disk disease. Radiology 168:177–186. https://doi.org/10.1148/radiology.168.1.3289089
de Roos A, Kressel H, Spritzer C, Dalinka M (1987) MR imaging of marrow changes adjacent to end plates in degenerative lumbar disk disease. AJR Am J Roentgenol 149:531–534. https://doi.org/10.2214/ajr.149.3.531
Xu L, Chu B, Feng Y, Xu F, Zou YF (2016) Modic changes in lumbar spine: prevalence and distribution patterns of end plate oedema and end plate sclerosis. Br J Radiol 89:20150650. https://doi.org/10.1259/bjr.20150650
Mera Y, Teraguchi M (2021) Association between types of Modic changes in the lumbar region and low back pain in a large cohort: the Wakayama spine study. Eur Spine J 30:1011–1017. https://doi.org/10.1007/s00586-020-06618-x
Fayad F, Lefevre-Colau MM, Rannou F, Quintero N, Nys A, Macé Y, Poiraudeau S, Drapé JL, Revel M (2007) Relation of inflammatory modic changes to intradiscal steroid injection outcome in chronic low back pain. Eur Spine J 16:925–931. https://doi.org/10.1007/s00586-006-0301-y
el Barzouhi A, Vleggeert-Lankamp CL, van der Kallen BF, Lycklama à Nijeholt GJ, van den Hout WB, Koes BW, Peul WC (2014) Back pain’s association with vertebral end-plate signal changes in sciatica. Spine J 14:225–233. https://doi.org/10.1016/j.spinee.2013.08.058
Chen Y, Bao J, Yan Q, Wu C, Yang H, Zou J (2019) Distribution of Modic changes in patients with low back pain and its related factors. Eur J Med Res 24:34. https://doi.org/10.1186/s40001-019-0393-6
Saukkonen J, Määttä J, Oura P, Kyllönen E, Tervonen O, Niinimäki J, Auvinen J, Karppinen J (2020) Association between Modic changes and low back pain in middle age: a Northern Finland birth cohort study. Spine 45:1360–1367. https://doi.org/10.1097/brs.0000000000003529
Määttä JH, Wadge S, MacGregor A, Karppinen J, Williams FM (2015) ISSLS prize winner: vertebral endplate (Modic) change is an independent risk factor for episodes of severe and disabling low back pain. Spine 40:1187–1193. https://doi.org/10.1097/brs.0000000000000937
Wu HL, Ding WY, Shen Y, Zhang YZ, Guo JK, Sun YP, Cao LZ (2012) Prevalence of vertebral endplate Modic changes in degenerative lumbar scoliosis and its associated factors analysis. Spine 37:1958–1964. https://doi.org/10.1097/BRS.0b013e31825bfb85
Dudli S, Sing DC, Hu SS, Berven SH, Burch S, Deviren V, Cheng I, Tay BKB, Alamin TF, Ith MAM, Pietras EM, Lotz JC (2017) ISSLS PRIZE IN BASIC SCIENCE 2017: intervertebral disc/bone marrow cross-talk with Modic changes. Eur Spine J 26:1362–1373. https://doi.org/10.1007/s00586-017-4955-4
Jacobsen HE, Khan AN, Levine ME, Filippi CG, Chahine NO (2020) Severity of intervertebral disc herniation regulates cytokine and chemokine levels in patients with chronic radicular back pain. Osteoarthr Cartil 28:1341–1350. https://doi.org/10.1016/j.joca.2020.06.009
Ford JJ, Kaddour O, Gonzales M, Page P, Hahne AJ (2020) Clinical features as predictors of histologically confirmed inflammation in patients with lumbar disc herniation with associated radiculopathy. BMC Musculoskelet Disord 21:567. https://doi.org/10.1186/s12891-020-03590-x
Djuric N, Yang X, Ostelo R, van Duinen SG, Lycklama à Nijeholt GJ, van der Kallen BFW, Peul WC, Vleggeert-Lankamp CLA (2019) Disc inflammation and Modic changes show an interaction effect on recovery after surgery for lumbar disc herniation. Eur Spine J 28:2579–2587. https://doi.org/10.1007/s00586-019-06108-9
Gao X, Li J, Shi Y, Li S, Shen Y (2018) Asymmetrical degenerative marrow (Modic) changes in cervical spine: prevalence, correlative factors, and surgical outcomes. J Orthop Surg Res 13:85. https://doi.org/10.1186/s13018-018-0807-0
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 26:1873–1878. https://doi.org/10.1097/00007632-200109010-00011
Mysliwiec LW, Cholewicki J, Winkelpleck MD, Eis GP (2010) MSU classification for herniated lumbar discs on MRI: toward developing objective criteria for surgical selection. Eur Spine J 19:1087–1093. https://doi.org/10.1007/s00586-009-1274-4
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33(1):159–174
Feng Z, Liu Y, Wei W, Hu S, Wang Y (2016) Type II Modic changes may not always represent fat degeneration: a study using MR fat suppression sequence. Spine 41:E987-e994. https://doi.org/10.1097/brs.0000000000001526
Jensen TS, Bendix T, Sorensen JS, Manniche C, Korsholm L, Kjaer P (2009) Characteristics and natural course of vertebral endplate signal (Modic) changes in the Danish general population. BMC Musculoskelet Disord 10:81. https://doi.org/10.1186/1471-2474-10-81
Kuisma M, Karppinen J, Niinimäki J, Kurunlahti M, Haapea M, Vanharanta H, Tervonen O (2006) A three-year follow-up of lumbar spine endplate (Modic) changes. Spine 31:1714–1718. https://doi.org/10.1097/01.brs.0000224167.18483.14
Dudli S, Fields AJ, Samartzis D, Karppinen J, Lotz JC (2016) Pathobiology of Modic changes. Eur Spine J 25:3723–3734. https://doi.org/10.1007/s00586-016-4459-7
Albert HB, Kjaer P, Jensen TS, Sorensen JS, Bendix T, Manniche C (2008) Modic changes, possible causes and relation to low back pain. Med Hypotheses 70:361–368. https://doi.org/10.1016/j.mehy.2007.05.014
Mok FP, Samartzis D, Karppinen J, Fong DY, Luk KD, Cheung KM (2016) Modic changes of the lumbar spine: prevalence, risk factors, and association with disc degeneration and low back pain in a large-scale population-based cohort. Spine J 16:32–41. https://doi.org/10.1016/j.spinee.2015.09.060
Arana E, Kovacs FM, Royuela A, Estremera A, Asenjo B, Sarasíbar H, Amengual G, Galarraga I, Alonso A, Casillas C, Muriel A, Montoya J, Ordóñez C, Martínez C, Zamora J, Campillo C, Abraira V (2011) Modic changes and associated features in Southern European chronic low back pain patients. Spine J 11:402–411. https://doi.org/10.1016/j.spinee.2011.03.019
Jensen TS, Sorensen JS, Kjaer P (2007) Intra- and interobserver reproducibility of vertebral endplate signal (modic) changes in the lumbar spine: the Nordic Modic Consensus Group classification. Acta Radiol 48:748–754. https://doi.org/10.1080/02841850701422112
Han C, Kuang MJ, Ma JX, Ma XL (2017) Prevalence of Modic changes in the lumbar vertebrae and their associations with workload, smoking and weight in northern China. Sci Rep 7:46341. https://doi.org/10.1038/srep46341
Fayad F, Lefevre-Colau MM, Drapé JL, Feydy A, Chemla N, Quintéro N, Rannou F, Poiraudeau S, Fermanian J, Revel M (2009) Reliability of a modified Modic classification of bone marrow changes in lumbar spine MRI. Joint Bone Spine 76:286–289. https://doi.org/10.1016/j.jbspin.2008.09.012
Albert HB, Briggs AM, Kent P, Byrhagen A, Hansen C, Kjaergaard K (2011) The prevalence of MRI-defined spinal pathoanatomies and their association with modic changes in individuals seeking care for low back pain. Eur Spine J 20:1355–1362. https://doi.org/10.1007/s00586-011-1794-6
Latif R, Imran S, Ahmad I, Ilyas MS, Aziz A, Zehra U (2021) Vertebral endplate changes correlate with presence of cartilaginous endplate in the herniated disc tissue: factor predicting failure of conservative treatment. Asian Spine J 16(2):212–220. https://doi.org/10.31616/asj.2021.0106
Jensen TS, Karppinen J, Sorensen JS, Niinimäki J, Leboeuf-Yde C (2008) Vertebral endplate signal changes (Modic change): a systematic literature review of prevalence and association with non-specific low back pain. Eur Spine J 17:1407–1422. https://doi.org/10.1007/s00586-008-0770-2
Thompson KJ, Dagher AP, Eckel TS, Clark M, Reinig JW (2009) Modic changes on MR images as studied with provocative diskography: clinical relevance–a retrospective study of 2457 disks. Radiology 250:849–855. https://doi.org/10.1148/radiol.2503080474
Kumarasamy D, Rajasekaran S, Anand KSSV, Soundararajan DCR, Shetty TAP, Kanna PRM, Pushpa BT (2021) Lumbar disc herniation and preoperative modic changes: a prospective analysis of the clinical outcomes after microdiscectomy. Global Spine J 12(5):940–951. https://doi.org/10.1177/2192568220976089
Buttermann GR, Heithoff KB, Ogilvie JW, Transfeldt EE, Cohen M (1997) Vertebral body MRI related to lumbar fusion results. Eur Spine J 6:115–120. https://doi.org/10.1007/bf01358743
Wang T, Yang SD, Liu S, Wang H, Liu H, Ding WY (2016) 17β-Estradiol inhibites tumor necrosis factor-α induced apoptosis of human nucleus pulposus cells via the PI3K/Akt pathway. Med Sci Monit 22:4312–4322
Liu S, Yang SD, Huo XW, Yang DL, Ma L, Ding WY (2018) 17β-Estradiol inhibits intervertebral disc degeneration by down-regulating MMP-3 and MMP-13 and up-regulating type II collagen in a rat model. Artif Cells Nanomed Biotechnol 46(sup2):182–191. https://doi.org/10.1080/21691401.2018.1453826
Funding
No funding was used in this study.
Author information
Authors and Affiliations
Contributions
WD designed the study. ZL and XG collected data. RL, XG and ZL analysed lumbar MR images. ZL performed data analysis and drafted the manuscript. SY reviewed and revised the manuscript.
Corresponding authors
Ethics declarations
Conflicts of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This retrospective study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Ethics Committee of the Third Hospital of Hebei Medical University approved this study (Approval Number: No. 2021-015-1).
Consent to participate
Verbal informed consent was obtained prior to the interview.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, Z., Gao, X., Ding, W. et al. Asymmetric distribution of Modic changes in patients with lumbar disc herniation. Eur Spine J 32, 1741–1750 (2023). https://doi.org/10.1007/s00586-023-07664-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07664-x