Abstract
Purpose
Aging is a risk factor for several debilitating conditions including those related to chronic back pain and intervertebral disc degeneration, both of which have no cure. Mouse models are useful tools for studying disc degeneration and chronic back pain in a tightly controlled and clinically relevant aging environment. Moreover, mice offer the advantage of carrying out longitudinal studies to understand the etiology and progression of disc pathology induced by genetic or surgical strategies. Previously, age-related behavioral trends of discomfort and enhanced nociception in mice were reported; however, whether these measures are mediated by structural and pathological changes in the disc is unknown.
Methods
The goal of the present observational study was to identify behavioral correlates of age-related degenerative changes in the disc. Towards this, we collected radiographs from 150 mice (77 females) between three and 23 months of age and measured the disc height index for each level of lumbar disc. Behavioral measures were collected on several of these mice which included rearing and distance travelled in an open field test; time spent in rearing, reaching, immobile, and self-suspended in the tail suspension test; bilateral hind paw licking in response to cold allodynia using acetone; and unilateral hind paw licking in response to heat hyperalgesia using capsaicin.
Results
Results show that the lower lumbar discs lose height with age and these changes are independent of body composition measures including body weight, bone mineral density, fat mass, lean weight mass, percent fat mass, and percent lean mass. Disc height positively correlates with rearing and mobility in the open field test, immobility in the tail suspension test, and thermal hyperalgesia. Disc height negatively correlates with cold allodynia and rearing in the tail suspension test. Furthermore, mediation analysis shows that the lumbosacral disc significantly mediates the effect of age on rearing in the open field test, but not cold allodynia, suggesting this behavior is a useful measure of age-related axial discomfort due to disc degeneration.
Conclusion
In summary, the findings from the current study show that disc height are associated with measures of axial discomfort and nociception in mice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The increased prevalence and socio-economic burden of chronic low back pain (cLBP) is a growing concern, world-wide [1, 2]. This increase is attributed to the rising proportion of elderly who are disproportionately affected by musculoskeletal disorders [1, 3, 4], however, with no cure, as the source of the pain is often unknown [5, 6]. One established risk factor, however, is the presence of disc degeneration. Several reports have shown that individuals with disc degeneration are more likely to have cLBP than those without disc degeneration [7,8,9], especially in adults [10]. And older adults with LBP show a greater progression of disc degeneration years later than those without LBP [11]. Even with this strong association, one in three individuals with disc degeneration is asymptomatic [8], and the severity of disc degeneration based on MRI findings is not always predictive of degree of pain [12]. Overall, there is a need to better understand how structural and pathological changes in the degenerated discs promote the development of cLBP.
Several studies have correlated biomarkers of disc degeneration with cLBP severity and prognosis (reviewed in [13]. Many clinical studies use non-invasive metrics, like disc height and body morphometric measures, due to the relative ease of access and potential for longitudinal data collection. These metrics provide useful insights into the etiology and progression of cLBP mediated by structural or pathological changes in the disc. Moreover, cLBP in patients is positively associated with severity of disc degeneration [14]. In older adults (over 55 years) shorter disc height is associated with increased presence [9, 15], increased risk of recurrence [11], and increased intensity [16] of cLBP. Further, non-surgical decompression procedures, which increases disc height, result in decreased pain ratings in elderly individuals with cLBP [17]. However, how these structural changes of the disc cause pain are unclear. To establish a relationship between disc phenotype and pain pathology, the somatosensory nervous system must be actively responding to disc pathologies that may arise from structural or degenerative changes. These changes may occur at the level of the peripheral nerves and dorsal root ganglia, the spinal cord, the brain, or all the above. However, the unique contribution of pathological disc phenotype on the somatosensory nervous system and pain experience is difficult to assess in humans where control of environmental factors and tissue access are both limited.
Pre-clinical animal models of disc degeneration provide more control over environmental variables while at the same time have greater relevance to human physiology than ex vivo and in vitro models. However, it is critical to make the distinction between painful and innocuous disc degeneration in the pre-clinical animal models [18]. Lumbar disc height is reported to decline in aging mice, which was associated with increased disc pathologies, and pain and sensitivity in mice [19]. In this study, we have aggregated behavioral data, disc height measures using radiographic data, and body composition data on male and female mice of varying backgrounds and ages to explore the interaction of these variables within each experimental mouse. The goal is to identify the predictors and mediators of disc degeneration and behavioral correlates of pain in physiologically aging mice that can guide future studies as useful markers. By modeling level-dependent structural changes in the pathological disc including disc height and biometric characteristics with behavioral outcomes, we can begin to parse the pain-contributing features in spontaneous disc degeneration in naturally aging mice.
Methods
Mice
Female and male mice used in these studies have a mixed FVB and C57BL/6J background and were bred in-house. Total 150 mice (77 females) between the ages of three and 23 months were analyzed. One to five mice were housed together in a Maxi-Miser® #9 cage (19.56 cm × 30.91 cm × 13.34 cm, 435.7 cm2 floor area) in a temperature-controlled facility with 12:12 light–dark cycle and food and water given ad libitum. Animals were maintained in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals, and all experiments were carried out in accordance with institutional guidelines under Institutional Animal Care and Use Committee (IACUC) approved at Weill Cornell Medical College (WCMC). IACUC and WCMC approved the study described in this manuscript with Animal Use Protocol number 2016-0026.
Radiography
Radiographs and dual energy X-ray absorptiometry (DEXA) scans were collected using the Ultra focus high resolution digital X-ray cabinet by Faxitron Bioptics, LLC (Arizona, USA). Radiographs were collected from 150 mice (77 females), of which 94 mice (42 females) had corresponding DEXA scans. Mice were anesthetized with isoflurane and placed in the chamber lying on their side in a natural position with tail extended to obtain sagittal radiographic images. Disc height index (DHI) was measured for L1-S1 intervertebral disc (discs) of 150 mice by taking the average of three measurements of the disc height from a sagittal plane and dividing it by the average of six measurements of the adjacent vertebral bones’ height [20]. Illustration of how DHI is computed is depicted in Fig. 1A. Measurements were made using the NIS-Elements Advanced Research microscopy imaging software. DEXA measurements recorded from 94 mice include weight, bone mineral density, muscle mass, and fat mass (all for the whole body).
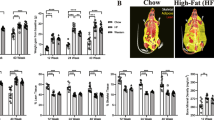
Lumbar disc height decreases linearly with age in mice. A Depiction of how disc height index (DHI) is assessed with equation below. B Representative radiographic images of the lumbar spine taken in the sagittal plane of mice at indicated ages. C–H Correlation of DHI at specified level with age. Red solid line is regression line with 95% confidence interval filled in with light red. I Comparison of slopes of linear regression lines in C–H with standard error of the mean indicated. *p < 0.05 in Dunnet’s post-hoc test compared to L6/S1 slope
Behavioral testing
Behavioral tests were performed on male and female mice from a range of ages during their life. All behavioral tests were performed by the same experimenter. Behavioral data was scored live and on video by multiple trained raters blind to the age and sex of the mice. Behavioral data presented here is based on an average of the scores. All behavioral data were collected from mice that had radiographic data collected to determine DHI within two weeks of behavioral test.
Open field test
The open field test was performed on 69 mice (27 females) as described previously [19]. In brief, the apparatus consisted of a rectangular arena (50 × 30 cm), with a transparent floor divided into 15 squares (10 × 10 cm). The test was initiated by placing a single mouse in the middle of the arena and letting it move freely for five minutes while being recorded from above. The behaviors were scored by the raters using a continuous sampling method. The number of squares crossed was measured as voluntary horizontal mobility and the duration of time spent rearing on hind legs was measured as voluntary standing.
Tail suspension test
The tail suspension assay [21] was performed on 49 mice (27 females) as described previously [22,23,24]. In brief, animals were suspended from the underside of a platform 30 cm above the tabletop using adhesive tape 0.5 cm from the base of the tail. Behaviors were recorded for three minutes while under supervision of the experimenter. The duration of time spent (1) reaching towards the ground, (2) immobile, (3) rearing towards their tail, and (4) self-suspended by holding onto the base of the tail, ankle or tape was analyzed over the testing period by the raters.
Cold allodynia
Cold allodynia was assessed on 51 mice (16 females) by measuring licking behaviors after 25 µl of acetone was applied using a pipette to the plantar surface of the hind paw as described previously [19]. Animals were placed in a 25 × 15 cm translucent plastic cage during the test. The time spent licking the affected hind paw and ankle during a two-minute period immediately following acetone application was measured.
Thermal hyperalgesia
Thermal hyperalgesia was assessed on 29 mice (6 females) by injecting capsaicin (2.5 µg in 5 µL of 0.25% ethanol, 0.125% Tween-20 in saline) into the dorsal surface of the left hind paw [22]. The duration spent licking or scratching the hind paw during a three-minute period was assessed by continuous sampling method by the raters.
Statistical analysis
All statistics were carried out using GraphPad Prism 9 and IBM SPSS statistics 24 software.
-
(1)
Normality of the data was assessed with the Shapiro–Wilk’s test, and homogeneity of variance between age groups and sex was examined with Levene’s test for each measure. A regression was constructed with sex as a factor; age, weight, and DHI as covariates; and behavioral measures as output variables.
-
(2)
Mediation was only considered for the analysis if three conditions were met: (1) when age predicted the behavioral assay, (2) when age predicted the level-specific DHI and (3) DHI level predicted the behavioral assay. Mediation analysis was performed using the PROCESS macro for SPSS [25], employing model 4 with bootstrapping [25].
Results
Mouse demographics
A total of 150 mice (77 females) between the ages of three months to 23 months were used to generate our model (see Table 1). Previous study reported that weight, bone mineral density (BMD), and muscle mass are correlated with age in mice [19], and we found the same associations in the current study (Supp. Fig. 1A–C). Also, consistent with previous reports [19], total fat mass, percent body fat and percent muscle mass were uncorrelated with age in male and female mice (Supp. Fig. 1D–F).
Disc height index decreases with age in mice
To confirm that lumbar DHI is an appropriate age-related disc phenotype, we measured DHI in 150 male and female mice between three and 23 months of age. The measurements are depicted in Fig. 1A. Representative radiographs are depicted in Fig. 1B. DHI at each lumbar level is significantly negatively associated with age in mice (Fig. 1C–H p < 0.0001 for each level). No sex-based differences were observed as male and female mice show comparable rates of DHI narrowing with age (Supp. Fig. 2A–F). Next to assess whether each disc level loses height at the same rate we compared the regression slopes. A one-way ANOVA revealed that rate of DHI narrowing with age is significantly different between each level [F(5852) = 2.566, p = 0.0257]. As the disc at the last lumbar level (L6/S1) is the most frequently affected by age in humans and mice, we performed a Dunnett’s post-hoc test comparing it to the other levels. Post-hoc comparison revealed that the L6/S1 DHI decreases significantly faster than the L5/L6 [t(852) = 2.904, p = 0.0167], L4/L5 [t(852) = 2.559, p = 0.0447], L3/L4 [t(852) = 2.968, p = 0.0138], and the L2/L3 [t(852) = 2.689, p = 0.0314] (Fig. 1I). In the 94 mice with DEXA data, no correlation was observed between DHI of the lumbosacral discs (L4-S1 levels), which are pathologically most affected with age [19, 26] nor with any body composition measures, including weight, BMD, muscle mass, fat mass, percent lean mass and percent fat mass in mice with age (Supp. Fig. 3A–F). Although, positive correlations between DHI and weight for L2/3 level (Supp. Fig. 3A), between DHI and fat for L1/2 level (Supp. Fig. 3D), and between DHI and percent fat mass for L1/2 (Supp. Fig. 3E) were observed. Moreover, a negative correlation between DHI and percent lean mass (% muscle) for L1/2 level (Supp. Fig. 3E) was observed. Thus, as mice get older, the lumbosacral (L4-S1) DHI decreases independent of body composition, with the L6/S1 level decreasing the most rapidly.
Reduced lumbar DHI is predictive of axial discomfort in the open field test
Previous studies reported that measures of axial strain are adversely affected with age in mice [19]. As DHI is a useful metric of LBP in older humans, we assessed how it relates to behavioral correlates of axial discomfort in mice. We found that rearing time in the open field test was positively associated with DHI at multiple lumbar levels (Fig. 2A). The strongest association was observed in the L6/S1 level (r2 = 0.1949, p = 0.0003), which is also the level most affected by age. Thus, mice with shorter discs are less likely to voluntarily take bipedal positions during exploration and this association is the strongest in the lumbosacral level. Interestingly, the L2/L3 level was the only level that did not positively associate with rearing times and squares crossed on all four limbs (Fig. 2A, B). DHI at all other levels were significantly associated with rearing time and the number of squares crossed on all fours in the open field test, a proxy for mobility (Fig. 2A, B). Previously it was reported that while both rearing and squares crossed negatively correlated with aging in mice, the number of squares crossed was not independently correlated with aging after controlling for rearing time [19]. In the present study we also observed that the relationship between DHI and open field test behaviors are independent of BMD, weight, and muscle mass in mice (Fig. 2C–E). Overall, DHI is strongly associated with behaviors of axial discomfort in the open field test, and this is not attributable to body composition.
Disc height index is associated with performance on the open field test. A Multiple regression of each lumbar disc height index (DHI) compared to the amount of time the mouse spent rearing up on hind legs in the open field test (OFT). B Multiple regression of each lumbar DHI compared to the total number of squares crossed on all fours in the open field test. Individual points represent a measure from one animal and color specifies lumbar level measured. Regression lines with 95% confidence intervals are given for each level, indicated by color. C Regression of rearing and squares crossed in the open field test compared to bone mineral density (BMD). D Regression of rearing and squares crossed in the open field test compared to mouse weight. E Regression of rearing and squares crossed in the open field test compared to muscle mass. Asterisks indicate a significant correlation with age. *p < 0.05, **p < 0.01, ***p < 0.001, n.s. = not significant
L6/S1 DHI impacts rearing and immobility in the tail suspension test
The tail suspension test has been adapted as a measure of axial strain tolerance and disc degeneration. Previous study reported that after controlling for weight, older mice reduce the time reaching and increase the time rearing during the tail suspension test [19]. Here we show that only L6/S1 DHI was associated with any behavior in the tail suspension test (Fig. 3A–D). Mice with shorter L6/S1 discs spent less time immobile (r2 = 0.1081, p = 0.0358) and more time rearing (r2 = 0.1165, p = 0.0290). DHI had no impact on the time spent reaching or self-suspended. Interestingly, no other disc level showed any relationship with tail suspension test behavior. This is interesting as both rearing in the open field test and reaching and rearing in the tail suspension test have been considered measures of axial strain. Our results show that rearing in open field test as well as in tail suspension test is impacted by DHI. Analysis of body composition data revealed that BMD, muscle mass, and weight have no impact on tail suspension test behaviors (Fig. 3E–G).
L6/S1 disc height index is associated with performance on the tail suspension test. A–D Multiple regression of each lumbar DHI compared to the proportion of time the mouse spent in each of the four positions during the tail suspension test (TST). E Regression of each tail suspension test position compared to bone mineral density (BMD). F Regression of each tail suspension test position compared to mouse weight. G Regression of each tail suspension test position compared to muscle mass. Asterisks indicate a significant correlation with age. *p < 0.05, n.s. = not significant
Shorter DHI predicts greater cold allodynia, larger DHI predicts greater thermal hyperalgesia
Previous reports show that hind paw cold allodynia in mice, but not thermal hyperalgesia is influenced by age in mice [19]. Previous reports also show that cold allodynia on both the hind paw [27] and back [23] in older mice, but not tail [23], suggesting cold allodynia is both age and location dependent. We found that changes in DHI at L2-5 and L6/S1 levels show a significant negative association with cold allodynia (Fig. 4A). Thus, having shorter discs at these levels is associated with an enhanced cold sensitivity to acetone in the hind paws. Interestingly, L5/L6 DHI was significantly associated with hind paw thermal hyperalgesia, with a larger disc being correlated with greater thermal hyperalgesia (Fig. 4B). Neither cold allodynia nor thermal hyperalgesia was associated with BMD, weight, or muscle mass in mice (Fig. 4C–E).
Shorter disc height index is negatively associated with cold allodynia and positively associated with heat hyperalgesia. A Multiple regression of each lumbar disc height index (DHI) compared to the time spent licking the hind paws following acetone application. B Multiple regression of each lumbar DHI compared to the time spent licking the hind paw following capsaicin injection. C Regression of acetone and capsaicin responses with bone mineral density (BMD). D Regression of acetone and capsaicin responses with mouse weight. E Regression of acetone and capsaicin responses with muscle mass. Asterisks indicate a significant correlation with age. *p < 0.05, **p < 0.01, n.s. = not significant
DHI mediates age-related axial strain, but not cold allodynia
As both open field test rearing and cold allodynia are correlated with age and DHI, which are in turn associated with each other, we assessed how interdependent these correlations were by employing mediation modeling. Specifically, we tested whether the relationship between aging and axial discomfort and cold allodynia is driven by the loss of disc height. Mediation analysis revealed that L6/S1 DHI partially mediates age-related open field test rearing behaviors (Fig. 5). The model identified that the inclusion of L6/S1 DHI has a mediator, the direct effect of age on rearing remains significant [c’ = − 3.2059, 95% CI (− 1.6200, − 4.7918), p = 0.0013], but the indirect effect of L6/S1 DHI accounts for over 22% of the total variance [indirect effect = − 0.9255, 95% CI (− 0.1247, − 1.6900)]. No other lumbar disc showed a significant mediation effect on rearing. Importantly, as the direct effect of age on rearing remained significant, DHI is not the only factor contributing to age-related rearing behaviors. In contrast, age-related cold allodynia is not mediated by the loss of DHI. Rather, the relationship between DHI and cold allodynia was lost entirely after accounting for age [b2 = − 0.6060, 95% CI (− 35.2952, 34.0833), p = 0.9767], indicating both variables are driven independently by age. These data give stronger support for the role of the lumbar disc in driving axial discomfort but not cold allodynia.
The lumbosacral disc height index mediates age-related rearing open field test behaviors, but not cold allodynia. a = partial effect of age on L6/S1 DHI, b1 = partial effect of L6/S1 DHI on rearing behavior in the open field test (OFT), b2 = partial effect of L6/S1 DHI on cold allodynia, c1’ = partial effect of age on rearing in the open field test, c2’ = partial effect of age on cold allodynia. Bold lines and numbers indicate significant effects. Hashed lines and non-bolded numbers indicate non-significant effects
Discussion
Animal models are useful paradigms for understanding the etiology and progression of disc degeneration but are often underutilized for their potential to probe for clinically relevant symptom of disc degeneration and cLBP. As mice show age-related disc degenerative phenotypes [19, 26], and age-associated changes in their behavioral repertoire [19], the present study probed these relationships further by exploiting linear modeling and mediation analysis. We found that the mouse lumbar disc loses height with age at each level, with the lumbosacral disc (L6/S1) having the most rapid decline. Mediation analysis shows that the declining lumbosacral DHI with age contributes to a reduction in rearing behaviors observed in older mice, but it does not contribute to age-related cold allodynia.
In this study, we used DHI as a proxy for disc degeneration. While this measure does not capture the robust and heterogeneous nature of disc degeneration, it has been shown to correlate strongly with both total disc histological score and the histological scores of the individual components in the disc [20]. Further, the ease of implementation for large number of animals in vivo, and collection of longitudinal data, it is a practical tool for the kind of analyses we wished to perform [20]. The steady reduction in DHI with age in mice diverges from the human data, where DHI increases until middle age and declines thereafter [9, 28]. One possible reason for this discrepancy is that laboratory mice have a sedentary lifestyle which may accelerate the rate of disc degeneration. Physical inactivity in humans contributes not only to cLBP but also narrower lumbar discs [29]. This may be due to declining musculature supporting the spine. A different trajectory for behavioral correlates of pain as well as DHI may be observed in more active mice.
Consistent with human data is the vulnerability of the lumbosacral disc (L6/S1) in mice, which we show has the most rapid loss in height with aging. In one study, more than 40% of older adults with LBP showed disc height narrowing in the lumbosacral disc, the level most affected in this age group [9]. However, why the lumbosacral disc is the most vulnerable remains poorly understood. Interestingly in bipeds, the lumbosacral level bears more weight owing to its position in the spinal column, and, therefore, subject to more compressive forces over our lifetime. Hence, one limitation of the study is that the results are from quadruped mice, but the human is biped: therefore, it is difficult to say from the current study whether similar results for the human. Although, previous studies using larger animal models reported that the spine in quadruped’s is loaded by axial compression at its long axis [30]. And the axial loading of quadruped’s spine is like that of human spine [30, 31]. Moreover, the lumbosacral disc is unique as it adjoins the sacral vertebrae, a region fused and immobile in both adult humans and mice. Due to the adjacent sacral inflexibility, the L6/S1 in mice, or L5/S1 in humans, may be subjected to more torsion. Indeed, following lumbar fusion surgery a common complication is adjacent segment disease, wherein the discs next to the fused levels develop degenerative phenotypes. Interestingly, these discs have also been reported to lose height following fusion surgery [32]. While there are undoubtedly a multitude of factors that predispose the most caudal lumbar disc to degeneration, the finding that the same pattern emerges in both murine and human data lends further support for the use of rodent models.
An important finding in this study was the observation that the loss of DHI in the lumbosacral disc mediates age-related reduction in open field test rearing. In humans, degree of recurrent lumbar disc degeneration is significantly correlated with reduced sagittal range of motion, measured as the maximum flexion and extension angles during a radiographic exam [33]. The loss of the lumbosacral disc height may similarly impair the range of motion required to take bipedal movements in mice. Whether the limited motion is due to inflexibility or avoided because the position is painful cannot be concluded in this study. However, given that the loss of L6/S1 disc height was also associated with a greater time spent in a rearing position in the tail suspension test—a position that requires flexibility to mitigate axial stretching-inflexibility seems unlikely. Further, muscle mass was not associated with changes in the open field test, indicating muscle loss does not account for a reduction in open field test rearing. This leaves the distinct possibility that rearing in the open field, an innocuous position in mice with healthy discs, becomes more uncomfortable with age in part due to age-related lumbosacral degeneration, resulting in fewer voluntary rearing behaviors.
A second important finding is that age-related cold allodynia is driven by age-related factors outside of disc height. Previous reports show an increases in hind paw sensitivity to cold stimuli with age [19, 27] and the cold-sensing ion channel, TRPA1, is increased in aged dorsal root ganglia [19]. However, what drives this change is unknown. Cold allodynia is a feature of several pain disorders, including several models of disc degeneration [22, 23, 27, 34, 35]. While one possibility is the presence of nerve impingement leading to radiating pain, there is no radiating thermal hyperalgesia in aging mice [19, 23] nor mouse models of disc degeneration [23, 36,37,38]. However, a similar phenomenon—cold allodynia in the absence of thermal hyperalgesia—can be reliably induced in humans via a nerve compression block which inhibits the conduction by myelinated Aδ but not unmyelinated fibers [39]. This results in increased cold sensitivity and produces a burning pain sensation, referred to as paradoxical heat sensation, with no change in thermal sensitivity [39]. Mechanistically this process is thought to be mediated by the loss of inhibitory input from the myelinated Aδ fibers on pain fibers, allowing the nociceptive afferents to respond to normally innocuous cold stimuli [40]. Paradoxical heat sensation [41] is a common feature of sciatica, a condition also driven by impinged nerve fibers. Both lateral disc bulging and facet joint compression on nerves can lead to nerve impingement. Unfortunately, radiographs used in this study do not show the disc outline, and therefore disc width and disc bulging could not be assessed in this study. Using histomorphometric analysis a previous study reported that in addition to reduced disc height, older mice have increased disc width [19]. Changes in lumbar disc width may therefore be a degenerative phenotype more closely associated with radiating cold sensitivity. Imaging techniques that reveal the disc shape and permit quantification of disc width in live mice would be better suited to address this possibility.
Here, we also found that while both weight and muscle mass increase with age and BMD declines with age, body composition measures did not predict any behavioral outcomes. This is an interesting observation as a high body mass index (BMI) in patients is associated with an increased risk for disc degeneration [42]. However, it is difficult to make a direct comparison in rodents which lack an analogous measure to BMI. Additionally, the mice in this study were fed a standard chow diet. Hence, mice with greater bodyweight received the same diet and nutritional profile as mice with lower weight. The same is not true in humans. Individuals with a greater caloric intake also tend to have a different macronutrient profile compared to those with lesser caloric intake, actor that likely contributes to the patterns observed with BMI. Murine models that include features of Western diet may be more appropriate to investigate body compositional impacts of aging and cLBP rather than the chow-fed models used here.
There are many ways in which the aging disc can cause cLBP, and many forms that this pain is manifested. The difficulty in reproducing these features in the preclinical setting is finding analogous phenotypes to human symptoms. Mouse models are being widely used to investigate the initiation, development, and progression of disc degeneration to prevent and develop treatments for the growing problem of cLBP; however, until we better understand the association between disc phenotype and pain outcome, the clinical relevance will remain tenuous. Here we see how a degenerative disc phenotype—loss of height—mediates a progressive behavioral change which occurs during the mouse aging process. Importantly, we observe that disc height cannot be used as a ubiquitous measure for painful disc degeneration, as it does not contribute to radiating pain. Additionally, researchers should be conscientious of factors that covary with disc height or other metrics of disc degeneration but are not a direct consequence of these measures. However, several physiological changes are associated with aging, and aging is often associated with various pathologies which could drive the behavior responses noted here. Hence, further studies using conditional and specific models of accelerated disc degeneration are required to test whether reduction in DHI and disc pathologies are causative of behaviors changes indicative of pain and sensitivity in mice. Overall, these data support the continued use of mice as clinically relevant models of disc degeneration and cLBP and recommends specific behavioral assays as markers of phenotype-specific disc degeneration.
References
Daly., G., H.G. DALYs , H. Collaborators (2015) Global, regional, and national disability-adjusted life-years (DALYs) for 315 diseases and injuries and healthy life expectancy (HALE), 1990–2015: a systematic analysis for the Global Burden of Disease Study. Lancet. 388 (10053): 1603–1658. https://doi.org/10.1016/s0140-6736(16)31460-x
Dieleman JL, Baral R, Birger M et al (2016) US spending on personal health care and public health, 1996–2013. JAMA 316(24):2627–2646. https://doi.org/10.1001/jama.2016.16885
Hartvigsen J, Christensen K, Frederiksen H (2003) Back pain remains a common symptom in old age. A population-based study of 4486 Danish twins aged 70–102. Eur Spine J 12(5):528–34. https://doi.org/10.1007/s00586-003-0542-y
Hurwitz EL, Randhawa K, Yu H et al (2018) The global spine care initiative: a summary of the global burden of low back and neck pain studies. Eur Spine J 27(Suppl 6):796–801. https://doi.org/10.1007/s00586-017-5432-9
Hartvigsen J, Hancock MJ, Kongsted A et al (2018) What low back pain is and why we need to pay attention. Lancet 391(10137):2356–2367. https://doi.org/10.1016/s0140-6736(18)30480-x
Maher C, Underwood M, Buchbinder R (2017) Non-specific low back pain. Lancet 389(10070):736–747. https://doi.org/10.1016/s0140-6736(16)30970-9
Luoma K, Riihimäki H, Luukkonen R et al (2000) Low back pain in relation to lumbar disc degeneration. Spine (Phila Pa 1976) 25(4):487–92. https://doi.org/10.1097/00007632-200002150-00016
Brinjikji W, Diehn FE, Jarvik JG et al (2015) MRI findings of disc degeneration are more prevalent in adults with low back pain than in asymptomatic controls: a systematic review and meta-analysis. AJNR Am J Neuroradiol 36(12):2394–2399. https://doi.org/10.3174/ajnr.A4498
de Schepper EI, Damen J, van Meurs JB et al (2010) The association between lumbar disc degeneration and low back pain: the influence of age, gender, and individual radiographic features. Spine (Phila Pa 1976) 35(5):531–6. https://doi.org/10.1097/BRS.0b013e3181aa5b33
DePalma MJ, Ketchum JM, Saullo T (2011) What is the source of chronic low back pain and does age play a role? Pain Med 12(2):224–233. https://doi.org/10.1111/j.1526-4637.2010.01045.x
Symmons DP, van Hemert AM, Vandenbroucke JP et al (1991) A longitudinal study of back pain and radiological changes in the lumbar spines of middle aged women II radiographic findings. Ann Rheum Dis 50(3):162–166. https://doi.org/10.1136/ard.50.3.162
Vagaska E, Litavcova A, Srotova I et al (2019) Do lumbar magnetic resonance imaging changes predict neuropathic pain in patients with chronic non-specific low back pain? Medicine (Baltimore) 98(17):e15377. https://doi.org/10.1097/md.0000000000015377
Khan AN, Jacobsen HE, Khan J et al (2017) Inflammatory biomarkers of low back pain and disc degeneration: a review. Ann N Y Acad Sci 1410(1):68–84. https://doi.org/10.1111/nyas.13551
Foizer GA, Paiva VC, Nascimento RDD et al (2022) Is there any association between the severity of disc degeneration and low back pain? Rev Bras Ortop (Sao Paulo) 57(2):334–340. https://doi.org/10.1055/s-0041-1735831
Pye SR, Reid DM, Smith R et al (2004) Radiographic features of lumbar disc degeneration and self-reported back pain. J Rheumatol 31(4):753–758
Luoma K, Vehmas T, Kerttula L et al (2016) Chronic low back pain in relation to modic changes, bony endplate lesions, and disc degeneration in a prospective MRI study. Eur Spine J 25(9):2873–2881. https://doi.org/10.1007/s00586-016-4715-x
Apfel CC, Cakmakkaya OS, Martin W et al (2010) Restoration of disk height through non-surgical spinal decompression is associated with decreased discogenic low back pain: a retrospective cohort study. BMC Musculoskelet Disord 11:155. https://doi.org/10.1186/1471-2474-11-155
Mosley GE, Evashwick-Rogler TW, Lai A et al (2017) Looking beyond the intervertebral disc: the need for behavioral assays in models of discogenic pain. Ann N Y Acad Sci 1409(1):51–66. https://doi.org/10.1111/nyas.13429
Vincent K, Mohanty S, Pinelli R et al (2019) Aging of mouse intervertebral disc and association with back pain. Bone 123:246–259. https://doi.org/10.1016/j.bone.2019.03.037
Masuda K, Aota Y, Muehleman C et al (2005) A novel rabbit model of mild, reproducible disc degeneration by an anulus needle puncture: correlation between the degree of disc injury and radiological and histological appearances of disc degeneration. Spine (Phila Pa 1976) 30(1):5–14. https://doi.org/10.1097/01.brs.0000148152.04401.20
Steru L, Chermat R, Thierry B et al (1985) The tail suspension test: a new method for screening antidepressants in mice. Psychopharmacology 85(3):367–370. https://doi.org/10.1007/bf00428203
Millecamps M, Tajerian M, Naso L et al (2012) Lumbar intervertebral disc degeneration associated with axial and radiating low back pain in ageing SPARC-null mice. Pain 153(6):1167–1179. https://doi.org/10.1016/j.pain.2012.01.027
Millecamps M, Tajerian M, Sage EH et al (2011) Behavioral signs of chronic back pain in the SPARC-null mouse. Spine (Phila Pa 1976) 36(2):95–102. https://doi.org/10.1097/BRS.0b013e3181cd9d75
Miyagi M, Millecamps M, Danco AT et al (2014) ISSLS prize winner: increased innervation and sensory nervous system plasticity in a mouse model of low back pain due to intervertebral disc degeneration. Spine (Phila Pa 1976) 39(17):1345–54. https://doi.org/10.1097/brs.0000000000000334
Hayes AF (2017) Introduction to mediation, moderation, and conditional process analysis: a regression-based approach, 2nd edn. Guilford Press, New York
Mohanty S, Pinelli R, Pricop P et al (2019) Chondrocyte-like nested cells in the aged intervertebral disc are late-stage nucleus pulposus cells. Aging Cell 18(5):e13006. https://doi.org/10.1111/acel.13006
Tajerian M, Alvarado S, Millecamps M et al (2011) DNA methylation of SPARC and chronic low back pain. Mol Pain 7:65. https://doi.org/10.1186/1744-8069-7-65
Roberts N, Gratin C, Whitehouse GH (1997) MRI analysis of lumbar intervertebral disc height in young and older populations. J Magn Reson Imaging 7(5):880–886. https://doi.org/10.1002/jmri.1880070517
Teichtahl AJ, Urquhart DM, Wang Y et al (2015) Physical inactivity is associated with narrower lumbar intervertebral discs, high fat content of paraspinal muscles and low back pain and disability. Arthritis Res Ther 17(1):114. https://doi.org/10.1186/s13075-015-0629-y
Smit TH (2002) The use of a quadruped as an in vivo model for the study of the spine—biomechanical considerations. Eur Spine J 11(2):137–144. https://doi.org/10.1007/s005860100346
Wilke HJ, Krischak S, Claes L (1996) Biomechanical comparison of calf and human spines. J Orthop Res 14(3):500–503. https://doi.org/10.1002/jor.1100140321
Miyakoshi N, Abe E, Shimada Y et al (2000) Outcome of one-level posterior lumbar interbody fusion for spondylolisthesis and postoperative intervertebral disc degeneration adjacent to the fusion. Spine (Phila Pa 1976) 25(14):1837–42. https://doi.org/10.1097/00007632-200007150-00016
Kim KT, Park SW, Kim YB (2009) Disc height and segmental motion as risk factors for recurrent lumbar disc herniation. Spine (Phila Pa 1976) 34(24):2674–8. https://doi.org/10.1097/BRS.0b013e3181b4aaac
Krock E, Millecamps M, Currie JB et al (2018) Low back pain and disc degeneration are decreased following chronic toll-like receptor 4 inhibition in a mouse model. Osteoarthr Cartil 26(9):1236–1246. https://doi.org/10.1016/j.joca.2018.06.002
Millecamps M, Czerminski JT, Mathieu AP et al (2015) Behavioral signs of axial low back pain and motor impairment correlate with the severity of intervertebral disc degeneration in a mouse model. Spine J 15(12):2524–2537. https://doi.org/10.1016/j.spinee.2015.08.055
Allen KD, Griffin TM, Rodriguiz RM et al (2009) Decreased physical function and increased pain sensitivity in mice deficient for type IX collagen. Arthritis Rheum 60(9):2684–2693. https://doi.org/10.1002/art.24783
Lai A, Moon A, Purmessur D et al (2015) Assessment of functional and behavioral changes sensitive to painful disc degeneration. J Orthop Res 33(5):755–764. https://doi.org/10.1002/jor.22833
Li Z, Liu H, Yang H et al (2014) Both expression of cytokines and posterior annulus fibrosus rupture are essential for pain behavior changes induced by degenerative intervertebral disc: an experimental study in rats. J Orthop Res 32(2):262–272. https://doi.org/10.1002/jor.22494
Wahren LK, Torebjörk E, Jörum E (1989) Central suppression of cold-induced C fibre pain by myelinated fibre input. Pain 38(3):313–319. https://doi.org/10.1016/0304-3959(89)90218-2
Wasner G, Schattschneider J, Binder A et al (2004) Topical menthol—a human model for cold pain by activation and sensitization of C nociceptors. Brain 127(Pt 5):1159–1171. https://doi.org/10.1093/brain/awh134
Freynhagen R, Rolke R, Baron R et al (2008) Pseudoradicular and radicular low-back pain—a disease continuum rather than different entities? answers from quantitative sensory testing. Pain 135(1–2):65–74. https://doi.org/10.1016/j.pain.2007.05.004
Samartzis D, Karppinen J, Chan D et al (2012) The association of lumbar intervertebral disc degeneration on magnetic resonance imaging with body mass index in overweight and obese adults: a population-based study. Arthritis Rheum 64(5):1488–1496. https://doi.org/10.1002/art.33462
Acknowledgements
Research reported in this publication was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health under Award Number R01AR065530, R01AR077145, R01AG070079, and S10OD026763 awarded to CLD. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The research was also supported by the research award from S and L Marx Foundation made to CLD.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Vincent, K.F., Bundock, J., Dona, C.P.G. et al. Loss of lumbar disc height with age and its impact on pain and sensitivity associated behaviors in mice. Eur Spine J 32, 848–858 (2023). https://doi.org/10.1007/s00586-023-07545-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07545-3