Abstract
Purpose
To provide a systematic review with meta-analysis providing evidence of the current diagnostic test accuracy (DTA) of pedicle screw electrical stimulation.
Methods
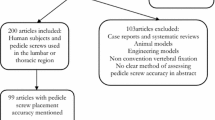
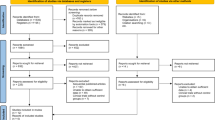
A systematic database search on PubMed, Scopus and Web of Science was performed according to the PRISMA-DTA guidelines, and eligibility criteria applied to reduce the results to: (1) only journal articles reporting electrical stimulation of the pedicle screw head, (2) screw position confirmation by imaging techniques, and (3) enough information allowing the calculation of a 2 × 2 contingency table. Sample characteristics, image confirmation method, electrical current threshold and stimulation results were retrieved and analyzed using according to appropriate DTA analysis methods, and allowing the calculation of specificity, sensitivity for pedicle screws insertion at the lumbar and thoracic levels.
Results
Lumbar screw stimulation presents a higher sensitivity (0.586 [0.336, 0.798] and specificity (0.984 [0.958, 0.994]) than thoracic screws (sensitivity: 0.270 [0.096; 0.562]; specificity: 0.958 [0.931, 0.975]). The same is observed in terms of the diagnostic odds ratio for lumbar (88.32 [32.136, 242.962]) and thoracic (8.460 [2.139, 33.469]) levels. When performing a sub-group analysis, it is possible to divide the lumbar stimulation threshold as 8 and 10–12 mA, and the thoracic threshold as 6 and 9–12 mA. A threshold of 8 mA at the lumbar level provides higher sensitivity and specificity. Increasing the threshold results in higher specificity but not sensitivity. In fact, at the range of 10–12 mA, the diagnostic validity is too low to confer this technique any robust diagnostic validity. Similarly, at the thoracic level, lower threshold currents are associated with increased sensitivity, but their diagnostic validity is very low.
Conclusion
Electrical stimulation of the pedicle screw can be used as an adequate diagnostic capability at the lumbar level with a threshold of 8 mA. However, thoracic stimulation is currently not reliable, with very low sensitivity and diagnostic validity at 6 mA or higher.




Similar content being viewed by others
Data Availability
This review study used data available from the searched databases.
References
Calancie B et al (1992) Intraoperative evoked EMG monitoring in an animal model. A new technique for evaluating pedicle screw placement. Spine (Phila Pa 1976) 17(10):1229–1235
Ravindra VM, Kalra RR, Dailey AT (2019) Electromyography stimulation compared with intraoperative O-arm imaging for evaluating pedicle screw breaches in lumbar spine surgery: a prospective analysis of 1006 screws in 164 patients. Spine J 19(2):206–211
Ajiboye RM et al (2017) Utility of intraoperative neuromonitoring for lumbar pedicle screw placement is questionable: a review of 9957 cases. Spine (Phila Pa 1976) 42(13):1006–1010
Raynor BL et al (2002) Can triggered electromyograph thresholds predict safe thoracic pedicle screw placement? Spine (Phila Pa 1976) 27(18):2030–2035
Samdani AF et al (2011) Triggered electromyography for placement of thoracic pedicle screws: is it reliable? Eur Spine J 20(6):869–874
Parker SL et al (2011) Ability of electromyographic monitoring to determine the presence of malpositioned pedicle screws in the lumbosacral spine: analysis of 2450 consecutively placed screws. J Neurosurg Spine 15(2):130–135
Kulik G et al (2013) A CT-based study investigating the relationship between pedicle screw placement and stimulation threshold of compound muscle action potentials measured by intraoperative neurophysiological monitoring. Eur Spine J 22(9):2062–2068
Raynor BL et al (2007) Correlation between low triggered electromyographic thresholds and lumbar pedicle screw malposition: analysis of 4857 screws. Spine (Phila Pa 1976) 32(24):2673–2678
Kaliya-Perumal A-K et al (2017) Intraoperative electromyographic monitoring to optimize safe lumbar pedicle screw placement—a retrospective analysis. BMC Musculoskelet Disord 18(1):229–229
Shi YB et al (2003) Electrical stimulation for intraoperative evaluation of thoracic pedicle screw placement. Spine (Phila Pa 1976) 28(6):595–601
Calancie B, Madsen P, Lebwohl N (1994) Stimulus-evoked EMG monitoring during transpedicular lumbosacral spine instrumentation. Initial clinical results. Spine (Phila Pa 1976) 19(24):2780–2786
Glassman SD et al (1995) A prospective analysis of intraoperative electromyographic monitoring of pedicle screw placement with computed tomographic scan confirmation. Spine (Phila Pa 1976) 20(12):1375–1379
Lenke LG et al (1995) Triggered electromyographic threshold for accuracy of pedicle screw placement. An animal model and clinical correlation. Spine (Phila Pa 1976) 20(14):1585–1591
Lee CH et al (2015) Can triggered electromyography thresholds assure accurate pedicle screw placements. A systematic review and meta-analysis of diagnostic test accuracy. Clin Neurophysiol 126(10):2019–2025
Mikula AL, Williams SK, Anderson PA (2016) The use of intraoperative triggered electromyography to detect misplaced pedicle screws: a systematic review and meta-analysis. J Neurosurg Spine 24(4):624–638
Fonseca P et al (2021) A bibliometric analysis of intraoperative neuromonitoring in spine surgery. World Neurosurgery 154:3–12
Page MJ et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Salameh J-P et al (2020) Preferred reporting items for systematic review and meta-analysis of diagnostic test accuracy studies (PRISMA-DTA): explanation, elaboration, and checklist. BMJ 370:m2632
Freeman SC et al (2019) Development of an interactive web-based tool to conduct and interrogate meta-analysis of diagnostic test accuracy studies: MetaDTA. BMC Med Res Methodol 19(1):81
Patel A et al (2021) Graphical enhancements to summary receiver operating characteristic plots to facilitate the analysis and reporting of meta-analysis of diagnostic test accuracy data. Res Synth Methods 12(1):34–44
Whiting PF et al (2011) QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155(8):529–536
Rubinstein ML, Kraft CS, Parrott JS (2018) Determining qualitative effect size ratings using a likelihood ratio scatter matrix in diagnostic test accuracy systematic reviews. Diagnosis 5(4):205–214
Alemo S, Sayadipour A (2010) Role of intraoperative neurophysiologic monitoring in lumbosacral spine fusion and instrumentation: a retrospective study. World Neurosurgery 73(1):72–76
Rodriguez-Olaverri JC et al (2008) Using triggered electromyographic threshold in the intercostal muscles to evaluate the accuracy of upper thoracic pedicle screw placement (T3–T6). Spine (Phila Pa 1976) 33(7):E194–E197
Plana MN, Pérez T, Zamora J (2021) New measures improved the reporting of heterogeneity in diagnostic test accuracy reviews: a metaepidemiological study. J Clin Epidemiol 131:101–112
Leeflang MMG (2014) Systematic reviews and meta-analyses of diagnostic test accuracy. Clin Microbiol Infect 20(2):105–113
Limthongkul W et al (2009) Evaluation of the intrinsic properties of pedicle screws: do diameter, manufacturing and screw design affect resistance and/or resistivity. Bosn J Basic Med Sci 9(Suppl 1):77–82
Davis TT et al (2014) Can triggered electromyography be used to evaluate pedicle screw placement in hydroxyapatite-coated screws: an electrical examination. J Clin Neurophysiol 31(2):138–142
Zyss J et al (2017) Limitations and pitfalls of the pedicle screw testing monitoring technique: an in vivo and in vitro study. Neurophysiol Clin 47(5–6):393–403
Fonseca P et al (2021) A new coupling method for accurate measurement of pedicle screw electrical properties for surgical procedures. Appl Sci 11(21):9861
Regidor I, de Blas G, Barrios C et al. (2011) Recording triggered EMG thresholds from axillary chest wall electrodes: a new refined technique for accurate upper thoracic (T2–T6) pedicle screw placement. Eur Spine J 20:1620–1625. https://doi.org/10.1007/s00586-011-1800-z
Acknowledgements
The authors would like to acknowledge the advisory contribution of Renato Andrade regarding the procedures required to perform a systematic review with meta-analysis.
Funding
The author Pedro Fonseca received financial support by Spine Implantes Brasil as tuition for the persecution of a PhD degree. Márcio Goethel is a partner of Scripibomer, a branch company of the aforementioned company. The remaining authors do not have any other financial interests.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design and conceptualization of the review. P.F. performed the database search, application of PRISMA protocol, analysis of results and drafting of initial manuscript. M.G. performed analysis of results and drafting of the original manuscript. J.P.V.B, M.G. and M.V.C. provided a review of results, cooperated in the discussion and the conclusion, and participated in the writing of the article.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethics approval
This is a systematic review with meta-analysis, reflecting a bibliographic analysis of published work, and therefore does not require the approval of an Ethics Committee.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fonseca, P., Goethel, M., Vilas-Boas, J. et al. A systematic review with meta-analysis of the diagnostic test accuracy of pedicle screw electrical stimulation. Eur Spine J 31, 1599–1610 (2022). https://doi.org/10.1007/s00586-022-07218-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-022-07218-7