Abstract
Objective
To develop a classification and regression tree (CART) model to predict the need of tracheostomy in patients with traumatic cervical spinal cord injury (TCSCI) and to quantify scores of risk factors to make individualized clinical assessments.
Methods
The clinical characteristics of patients with TCSCI admitted to our hospital from January 2014 to December 2020 were retrospectively analyzed. The demographic characteristics (gender, age, smoking history), mechanism of injury, injury characteristics (ASIA impairment grades, neurological level of impairment, injury severity score), preexisting lung disease and preexisting medical conditions were statistically analyzed. The risk factors of tracheostomy were analyzed by univariate logistic regression analysis (ULRA) and multiple logistic regression analysis (MLRA). The CART model was established to predict tracheostomy.
Results
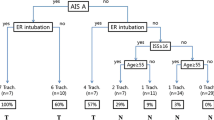
Three hundred and forty patients with TCSCI met the inclusion criteria, in which 41 patients underwent the tracheostomy. ULRA and MLRA showed that age > 50, ISS > 16, NLI > C5 and AIS A were significantly associated with tracheostomy. The CART model showed that AIS A and NLI > C5 were at the first and second decision node, which had a significant influence on the decision of tracheostomy. The final scores for tracheostomy from CART algorithm, composed of age, ISS, NLI and AIS A with a sensitivity of 0.78 and a specificity of 0.96, could also predict tracheostomy.
Conclusion
The establishment of CART model provided a certain clinical guidance for the prediction of tracheostomy in TCSCI. Quantifications of risk factors enable accurate prediction of individual patient risk of need for tracheostomy.



Similar content being viewed by others
References
Wang Y, Lu H, Teng H, Cui G, Fan D, Li M (2020) Efficacy and safety of early tracheotomy in acute cervical spinal cord injury. J Coll Physicians Surg Pak 30:956–960
Mu Z, Zhang Z (2019) Risk factors for tracheostomy after traumatic cervical spinal cord injury. J Orthop Surg (Hong Kong) 27:2309499019861809
Yugue I, Okada S, Ueta T, Maeda T, Mori E, Kawano O, Takao T, Sakai H, Masuda M, Hayashi T, Morishita Y, Shiba K (2012) Analysis of the risk factors for tracheostomy in traumatic cervical spinal cord injury. Spine Phila Pa 1976 37:E1633-1638
Hayashi T, Fujiwara Y, Sakai H, Maeda T, Ueta T, Shiba K (2017) Risk factors for severe dysphagia in acute cervical spinal cord injury. Spinal Cord 55:940–943
Lee D, Park C, Carriere K, Ahn J (2017) Classification and regression tree model for predicting tracheostomy in patients with traumatic cervical spinal cord injury. Eur Spine J 26:2333–2339
Childs BR, Moore TA, Como JJ, Vallier HA (2015) American Spinal Injury Association Impairment Scale predicts the need for tracheostomy after cervical spinal cord injury. Spine Phila Pa 1976 40:1407–1413
Hou YF, Lv Y, Zhou F, Tian Y, Ji HQ, Zhang ZS, Guo Y (2015) Development and validation of a risk prediction model for tracheostomy in acute traumatic cervical spinal cord injury patients. Eur Spine J 24:975–984
Scantling D, Granche J, Williamson J, Gracely E, Thosani D, McCracken B (2019) Development of clinical tracheostomy score to identify cervical spinal cord injury patients requiring prolonged ventilator support. J Trauma Acute Care Surg 87:195–199
Flanagan CD, Childs BR, Moore TA, Vallier HA (2018) Early tracheostomy in patients with traumatic cervical spinal cord injury appears safe and may improve outcomes. Spine Phila Pa 1976 43:1110–1116
Seidl RO, Wolf D, Nusser-Muller-Busch R, Niedeggen A (2010) Airway management in acute tetraplegics: a retrospective study. Eur Spine J 19:1073–1078
Beom JY, Seo HY (2018) The need for early tracheostomy in patients with traumatic cervical cord injury. Clin Orthop Surg 10:191–196
Nakashima H, Yukawa Y, Imagama S, Ito K, Hida T, Machino M, Kanbara S, Morita D, Hamajima N, Ishiguro N, Kato F (2013) Characterizing the need for tracheostomy placement and decannulation after cervical spinal cord injury. Eur Spine J 22:1526–1532
Romero J, Vari A, Gambarrutta C, Oliviero A (2009) Tracheostomy timing in traumatic spinal cord injury. Eur Spine J 18:1452–1457
Speybroeck N (2011) Classification and regression trees. Int J Public Health 57:243–246
Henrard S, Speybroeck N, Hermans C (2015) Classification and regression tree analysis vs. multivariable linear and logistic regression methods as statistical tools for studying haemophilia. Haemophilia 21:715–722
Committee. AaIIS (2019) The 2019 revision of the international standards for neurological classification of spinal cord Injury (ISNCSCI)-What’s new? Spinal Cord 57:815–817
Baker S (1974) The injury severity score, a method for describing patients with multiple injuries and evaluating emergency care. J Trauma 14:187–196
Kirshblum SC, Waring W, Biering-Sorensen F, Burns SP, Johansen M, Schmidt-Read M, Donovan W, Graves D, Jha A, Jones L, Mulcahey MJ, Krassioukov A (2011) Reference for the 2011 revision of the international standards for neurological classification of spinal cord injury. J Spinal Cord Med 34:547–554
Durga P, Sahu BP, Mantha S, Ramachandran G (2010) Development and validation of predictors of respiratory insufficiency and mortality scores: simple bedside additive scores for prediction of ventilation and in-hospital mortality in acute cervical spine injury. Anesth Analg 110:134–140
Jones TS, Burlew CC, Johnson JL, Jones E, Kornblith LZ, Biffl WL, Stovall RT, Pieracci FM, Stahel PF, Moore EE (2015) Predictors of the necessity for early tracheostomy in patients with acute cervical spinal cord injury: a 15-year experience. Am J Surg 209:363–368
Berney S, Gordon I, Opdam H, Denehy L (2011) A classification and regression tree to assist clinical decision making in airway management for patients with cervical spinal cord injury. Spinal Cord 49:244–250
Higashi T, Eguchi H, Wakayama Y, Sumi M, Saito T, Inaba Y (2019) Analysis of the risk factors for tracheostomy and decannulation after traumatic cervical spinal cord injury in an aging population. Spinal Cord 57:843–849
Tanaka J, Yugue I, Shiba K, Maeyama A, Naito M (2016) A study of risk factors for tracheostomy in patients with a cervical spinal cord injury. Spine Phila Pa 1976 41:764–771
Wang Y, Guo Z, Fan D, Lu H, Xie D, Zhang D, Jiang Y, Li P, Teng H (2018) A Meta-analysis of the influencing factors for tracheostomy after cervical spinal cord injury. Biomed Res Int 2018:5895830
McCully BH, Fabricant L, Geraci T, Greenbaum A, Schreiber MA, Gordy SD (2014) Complete cervical spinal cord injury above C6 predicts the need for tracheostomy. Am J Surg 207:664–668 (discussion 668-669)
Branco BC, Plurad D, Green DJ, Inaba K, Lam L, Cestero R, Bukur M, Demetriades D (2011) Incidence and clinical predictors for tracheostomy after cervical spinal cord injury: a National Trauma Databank review. J Trauma 70:111–115
Harrop J, Sharan A, Scheid E, Vaccaro A, Przybylski G (2004) Tracheostomy placement in patients with complete cervical spinal cord injuries: American spinal injury association grade A. J Neurosurg 100:20–23
Funding
None.
Author information
Authors and Affiliations
Contributions
DS: Investigation, Data statistics, Writing. HZ: Data collection, Data statistics. ZZ: Conceptualization; Writing-review & editing.
Corresponding authors
Ethics declarations
Data availability
The datasets generated during and analyzed during the current study are available from the corresponding author on reasonable request.
Ethics approval and consent to participate
All procedures used in this research were approved by the Ethics Committee of Army Medical University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sun, D., Zhao, H. & Zhang, Z. Classification and regression tree (CART) model to assist clinical prediction for tracheostomy in patients with traumatic cervical spinal cord injury: a 7-year study of 340 patients. Eur Spine J 31, 1283–1290 (2022). https://doi.org/10.1007/s00586-022-07154-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-022-07154-6