Abstract
Purpose
The clinical significance of Modic changes in low back pain (LBP) is yet to be clarified. Thus, this study aimed to examine the association between Modic changes and LBP after adjustment for confounding factors.
Methods
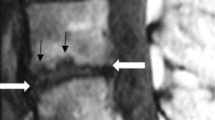
We evaluated participants in the second Wakayama Spine Study. The degree of endplate changes as measured using magnetic resonance imaging was classified based on the Modic classification system. The prevalence of the types of Modic change in the lumbar region and at each level was assessed. Multivariate logistic regression analysis was conducted to determine the association between the types of Modic changes and LBP with adjustment for age, sex, body mass index, disc degeneration score, and disc displacement score. The LBP intensity was also compared according to the Visual Analogue Scale (VAS) score among the three types of Modic change.
Results
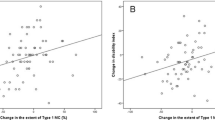
Overall, 814 subjects were evaluated. Type II Modic changes were the most prevalent (41.9%). Only type I Modic changes were significantly associated with LBP (odds ratio): 1.84, 95% confidence interval [CI]: 1.1–2.9). The LBP VAS score was significantly higher in subjects with type I Modic change than that in those with no Modic change (23.9 ± 26.3 vs. 9.9 ± 19.4, p < 0.05).
Conclusion
Type I Modic changes in the lumbar region are significantly associated with LBP. Profiling Modic changes may be helpful to improve targeted treatment of LBP.


Similar content being viewed by others
Code availability
Not applicable.
References
DALYs GBD, Collaborators H, Murray CJ et al (2015) Global, regional, and national disability-adjusted life years (DALYs) for 306 diseases and injuries and healthy life expectancy (HALE) for 188 countries, 1990–2013: quantifying the epidemiological transition. Lancet 386:2145–2191. https://doi.org/10.1016/S0140-6736(15)61340-XEpub 2015 Aug 28
Vos T, Flaxman AD, Naghavi M et al (2012) (2010) Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the global burden of disease study. Lancet 380:2163–2196. https://doi.org/10.1016/S0140-6736(12)61729-2
Karppinen J, Shen FH, Luk KD, Andersson GB, Cheung KM, Samartzis D (2011) Management of degenerative disk disease and chronic low back pain. Orthop Clin North Am 42:513–528. https://doi.org/10.1016/j.ocl.2011.07.009
Samartzis D, Borthakur A, Belfer I, Bow C, Lots CJ, Wang HQ, Cheung KMC, Carragee E, Karppinen J (2015) Novel diagnostic and therapeutic methods for intervertebral disc degeneration and low back pain. Spine J 15:1919–1932. https://doi.org/10.1016/j.spinee.2014.09.010
Boden SD, Davis DO, Dina TS, Patronas NJ, Wiesel SW (1990) Abnormal magnetic-resonance scans of the lumbar spine in asymptomatic subjects. A prospective investigation. J Bone Joint Surg Am 72:403–408
Brinjikji W, Diehn FE, Jarvik JG, Carr CM, Kallmes MH, Murad MH, Luetmer PH (2015) MRI findings of disc degeneration are more prevalent in adults with low back pain than in asymptomatic controls: a systematic review and meta-analysis. AJNR Am J Neuroradiol 36:2394–2399. https://doi.org/10.3174/ajnr.A4498
Teraguchi M, Cheung JPY, Karppinen J, Bow C, Hashizume H, Luk KDK, Cheung KMC, Samartzis D (2020) Lumbar high-intensity zones on MRI: imaging biomarkers for severe, prolonged low back pain and sciatica in a population-based cohort. Spine J 20:1025–1034. https://doi.org/10.1016/j.spinee.2020.02.015
Maatta J, Karppinen J, Paananen M, Bow C, Luk KDK, Chueng KMC, Samartzis D (2016) Refined phenotyping of Modic changes: potential imaging biomarkers of prolonged severe low back pain and disability. Medicine 95:e3495. https://doi.org/10.1097/MD.0000000000003495
Maatta JH, Karppinen JI, Luk KD, Cheung KM, Samartzis D (2015) Phenotype profiling of modic changes of the lumbar spine and its association with other MRI phenotypes: a large-scale population-based study. Spine J 15:1933–1942. https://doi.org/10.1016/j.spinee.2015.06.056
Mok FP, Samartzis D, Karppinen J, Fong DY, Luk KD, Cheung KM (2016) Modic changes of the lumbar spine: prevalence, risk factors, and association with disc degeneration and low back pain in a large-scale population-based cohort. Spine J 16:32–41. https://doi.org/10.1016/j.spinee.2015.09.060
Samartzis D, Mok FP, Karppinen J, Fong DY, Luk KD, Cheung KM (2016) Classification of Schmorl's nodes of the lumbar spine and association with disc degeneration: a large-scale population-based MRI study. Osteoarthr Cartil 24:1753–1760. https://doi.org/10.1016/j.joca.2016.04.020
Modic MT, Steinberg PM, Ross JS, Carter JR (1988) Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 166:193–199. https://doi.org/10.1148/radiology.166.1.3336678
Toyone T, Takahashi K, Kitahara H, Yamagata M, Murakami M, Moriya H (1994) Vertebral bone-marrow changes in degenerative lumbar disc disease. An MRI study of 74 patients with low back pain. J Bone Joint Surg Br 76:757–764
Wang Y, Videman T, Battie MC (2012) Modic changes: prevalence, distribution patterns, and association with age in white men. Spine J 12:411–416. https://doi.org/10.1016/j.spinee.2012.03.026
Kjaer P, Korsholm L, Bendix T, Sørensen JS, Leboeuf-Yde C (2006) Modic changes and their associations with clinical findings. Eur Spine J 15:1312–1319. https://doi.org/10.1007/s00586-006-0185-x
Maatta JH, Kraatari M, Wolber L, Niinimaki J, wadge S, Karppinen J, Williams FMK. (2014) Vertebral endplate change as a feature of intervertebral disc degeneration: a heritability study. Eur Spine J 23:1856–1862. https://doi.org/10.1007/s00586-014-3333-8
el Barzouhi A, Vleggeert-Lankamp CL, van der Kallen BF et al (2014) Back pain’s association with vertebral end-plate signal changes in sciatica. Spine J 14:225–233. https://doi.org/10.1016/j.spinee.2013.08.058
Kovacs FM, Arana E, Royuela A et al (2012) Vertebral endplate changes are not associated with chronic low back pain among Southern European subjects: a case control study. AJNR Am J Neuroradiol 33:1519–1524. https://doi.org/10.3174/ajnr.A3087
Ohtori S, Inoue G, Ito T, Koshi T, Ozawa T, Doya ST, Kazuhisa M, Takahashi K (2006) Tumor necrosis factor-immunoreactive cells and PGP 9.5- immunoreactive nerve fibers in vertebral endplates of patients with discogenic low back pain and Modic Type 1 or Type 2 changes on MRI. Spine(Phila Pa 1976) 31:1026–1031. https://doi.org/10.1097/01.brs.0000215027.87102.7c
Luoma K, Vehmas T, Grönblad M, Kerttula L, Kääpä E (2009) Relationship of modic type 1 change with disc degeneration: a prospective MRI study. Skeletal Radiol 38:237–244. https://doi.org/10.1007/s00256-008-0611-8
Kjaer P, Leboeuf-Yde C, Korsholm L, Sorense JS, Bendix T (2005) Magnetic resonance imaging and low back pain in adults: a diagnostic imaging study of 40-year-old men and women. Spine (Phila Pa 1976) 30:1173–1180. https://doi.org/10.1097/01.brs.0000162396.97739.76
Kuisma M, Karppinen J, Niinimaki J et al (2007) Modic changes in endplates of lumbar vertebral bodies: prevalence and association with low back and sciatic pain among middle-aged male workers. Spine(Phila Pa 1976) 32:1116–1122. https://doi.org/10.1097/01.brs.0000261561.12944.ff
Teraguchi M, Yoshimura N, Hashizume H, Muraki S, Yamada H, Minamide A et al (2014) Prevalence and distribution of intervertebral disc degeneration over the entire spine in a population-based cohort: the Wakayama spine study. Osteoarthr Cartil 22:104–110. https://doi.org/10.1016/j.joca.2013.10.019
Teraguchi M, Yoshimura N, Hashizume H, Muraki S, Yamada H, Oka H et al (2015) The association of combination of disc degeneration, end plate signal change, and schmorl node with low back pain in a large population study: the Wakayama spine study. Spine J 15:622–628. https://doi.org/10.1016/j.spinee.2014.11.012
Yoshimura N, Muraki S, Oka H, Kawaguchi H, Nakamura K, Akune T (2010) Cohort profile: research on oste-oarthritis/osteoporosis against disability (ROAD) study. Int J Epidemiol 39(4):988–995. https://doi.org/10.1093/ije/dyp276
Vavken P, Ganal-Antonio AKB, Shen FH, Chapman J, Samartzis D (2015) Fundamentals of clinical outcomes assessment for spinal disorders: study designs, methodologies, and analyses. Glob Spine J5:156–164. https://doi.org/10.1055/s-0035-1547525
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine(Phila Pa 1976) 26:1873–1878. https://doi.org/10.1097/00007632-200109010-00011
Cheung KMC, Karppinen J, Chan D, Ho DWH, Song YQ, Sham P et al (2009) Prevalence and pattern of lumbar magnetic resonance imaging changes in a population study of one thousand forty-three individuals. Spine(Phila Pa 1976) 20 34(9):934–940. https://doi.org/10.1097/BRS.0b013e3181a01b3f
Kerttula L, Luoma K, Vehmas T, Grönblad M, Kääpä E (2012) Modic type I change may predict rapid progressive, deforming disc degeneration: a prospective 1-year follow-up study. Eur Spine J 21:1135–1142. https://doi.org/10.1007/s00586-012-2147-9
Acknowledgements
The authors wish to thank Mrs. Tamako Tsutsumi, Mrs. Kanami Maeda, and other members of the Public Office in Taiji Town for their assistance in locating and scheduling the participants for examinations. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Funding
This work was supported by H-25-Choujyu-007 (Director, NY), H25-Nanchitou (Men)-005 (Director, ST), and 201417014A (Director, NY) from the Ministry of Health, Labour and Welfare, a Grant-in-Aid for Scientific Research (C 26861206) of JSPS KAKENHI grant. And Collaborating Research with NSF 08033011–00262 (Director, NY) from the Ministry of Education, Culture, Sports, Science and Technology in Japan. This study also was supported by grants from the Japan Osteoporosis Society (NY, HO, and TA), a grant from JA Kyosai Research Institute (HO), Japan Society for the Promotion of Science, Grants-in-Aid for Scientific Research (KAKENHI) Research C (1 7 K 1 0 9 3 7) (MT), a Grant from the Japanese Orthopaedics and Traumatology Foundation, Inc (No. 287) (MT). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Yoshimasa Mera Initial drafted the paper; Masatoshi Teraguchi was involved in critical editing of the paper, interpreted the findings, provided administrative support, obtained the funding, and contributed to the supervision of the study and conception of study design; Hiroshi Hashizume contributed to critical editing of the paper and interpreted the findings; Hiroyuki Oka collected the data, contributed to critical editing of the paper, and interpreted the findings; Shigeyuki Muraki, Toru Akune, Hiroshi Kawaguchi, Kozo Nakamura, and Sakae Tanaka were involved in critical editing of the paper; Hidenobu Tamai collected the data and contributed to critical editing of the paper; Munehito Yoshida, Noriko Yoshimura, and Hiroshi Yamada were involved in critical editing of the paper, supervision of the study, and conception of study design.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare there is no conflict of interests.
Ethics approval
The study was conducted with the approval of the ethics committee of our university and in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments.
Consent to participate
All patients were required to provide written informed consent prior to participation.
Consent for publication
All author had consent for publication.
Availability of data and material
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mera, Y., Teraguchi, M., Hashizume, H. et al. Association between types of Modic changes in the lumbar region and low back pain in a large cohort: the Wakayama spine study. Eur Spine J 30, 1011–1017 (2021). https://doi.org/10.1007/s00586-020-06618-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06618-x