Abstract
Purpose
Lumbar spinal canal stenosis (LSCS) is associated with fibrosis, decreased elastin-to-collagen ratio, and hypertrophy of the ligamentum flavum (LF). Diabetes mellitus (DM) is known to cause metabolic disturbances within the extracellular matrix in multiple tissues. These alterations may play a major role in the severity of clinical symptoms of LSCS affecting diabetic patients. We aimed to examine the hypothesis that DM may contribute to the LF changes seen in patients with LSCS.
Methods
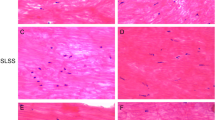
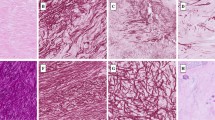
The study cohort included 29 patients: 23 with LSCS (10 with DM vs. 13 without DM) as well as six patients with lumbar disc herniation (LDH). Surgical LF specimens were retrieved for histological assessment. Morphologic quantification of confocal microscopy images using fast Fourier transform analysis allowed us to compare anisotropy and elastin fiber orientation between groups.
Results
There was a significant positive correlation between fasting plasma glucose values and degree of elastin degradation (r = 0.36, p = 0.043). The diabetic patients with LSCS showed a significantly greater loss of elastic fibers (2.3 ± 0.9 vs. 1.5 ± 0.55, p = 0.009), although fibrosis was shown to be similar (1.44 ± 0.7 vs. 1.43 ± 0.88, p = 0.98). There was no significant difference in the degree of calcification in the LSCS group between patients with and without diabetes (1.71 vs. 2.05%, p = 0.653). Fiber orientation was found to be less homogenous in the LSCS compared with the LDH group, although not significantly affected by DM.
Conclusions
The present study points to a significant contribution of DM to the loss of elastin fibers that occurs in the LF of patients with LSCS.



Similar content being viewed by others
References
Park JO, Lee BH, Kang YM, Kim TH, Yoon JY, Kim H, Kwon UH, Lee KI, Lee HM, Moon SH (2013) Inflammatory cytokines induce fibrosis and ossification of human ligamentum flavum cells. J Spinal Disord Tech 26:E6–12. doi:10.1097/BSD.0b013e3182698501
Park J-B, Kong C-G, Suhl K-H, Chang E-D, Riew KD (2009) The increased expression of matrix metalloproteinases associated with elastin degradation and fibrosis of the ligamentum flavum in patients with lumbar spinal stenosis. Clin Orthop Surg 1:81–89
Park JB, Lee JK, Park SJ, Riew KD (2005) Hypertrophy of ligamentum flavum in lumbar spinal stenosis associated with increased proteinase inhibitor concentration. J Bone Jt Surg 87:2750–2757
Abbas J, Hamoud K, Masharawi YM, May H, Hay O, Medlej B, Peled N, Hershkovitz I (2010) Ligamentum flavum thickness in normal and stenotic lumbar spines. Spine 35:1225
Altinkaya N, Yildirim T, Demir S, Alkan O, Sarica FB (2011) Factors associated with the thickness of the ligamentum flavum: is ligamentum flavum thickening due to hypertrophy or buckling? Spine (Phila Pa 1976) 36:E1093–E1097. doi:10.1097/BRS.0b013e318203e2b5
Anekstein Y, Smorgick Y, Lotan R, Agar G, Shalmon E, Floman Y, Mirovsky Y (2010) Diabetes mellitus as a risk factor for the development of lumbar spinal stenosis. Isr Med Assoc J 12:16–20
Asadian L, Haddadi K, Aarabi M, Zare A (2016) Diabetes mellitus, a new risk factor for lumbar spinal stenosis: a case–control study. Clin Med Insights Endocrinol Diabetes 9:1–5. doi:10.4137/CMED.S39035
Cui G, Watanabe K, Miyauchi Y, Hosogane N, Tsuji T, Ishii K, Nakamura M, Toyama Y, Chiba K, Miyamoto T, Matsumoto M (2011) Matrix metalloproteinase 13 in the ligamentum flavum from lumbar spinal canal stenosis patients with and without diabetes mellitus. J Orthop Sci 16:785–790. doi:10.1007/s00776-011-0135-2
Cavero-Redondo I, Peleteiro B, Alvarez-Bueno C, Rodriguez-Artalejo F, Martinez-Vizcaino V (2017) Glycated haemoglobin A1c as a risk factor of cardiovascular outcomes and all-cause mortality in diabetic and non-diabetic populations: a systematic review and meta-analysis. BMJ Open 7:e015949. doi:10.1136/bmjopen-2017-015949
American Diabetes A (2015) (2) Classification and diagnosis of diabetes. Diabetes Care 38(Suppl):S8–S16. doi:10.2337/dc15-S005
Fairbank JC, Pynsent PB (2000) The Oswestry disability index. Spine 25:2940–2953
Pratt RK, Fairbank JC, Virr A (2002) The reliability of the Shuttle Walking Test, the Swiss Spinal Stenosis Questionnaire, the Oxford Spinal Stenosis Score, and the Oswestry Disability Index in the assessment of patients with lumbar spinal stenosis. Spine 27:84–91
Sairyo K, Biyani A, Goel VK, Leaman DW, BoothJr R, Thomas J, Ebraheim NA, Cowgill IA, Mohan SE (2007) Lumbar ligamentum flavum hypertrophy is due to accumulation of inflammation-related scar tissue. Spine (Phila Pa 1976) 32:E340–E347. doi:10.1097/01.brs.0000263407.25009.6e
de Carvalho HF, Taboga SR (1996) The applicability of hematoxylin–eosin staining plus fluorescence or confocal laser scanning microscopy to the study of elastic fibers in cartilages. C R Acad Sci III 319:991–996
de Carvalho HF, Taboga SR (1996) Fluorescence and confocal laser scanning microscopy imaging of elastic fibers in hematoxylin–eosin stained sections. Histochem Cell Biol 106:587–592
Ayres CE, Jha BS, Meredith H, Bowman JR, Bowlin GL, Henderson SC, Simpson DG (2008) Measuring fiber alignment in electrospun scaffolds: a user’s guide to the 2D fast Fourier transform approach. J Biomater Sci Polym Ed 19:603–621. doi:10.1163/156856208784089643
Schneider CA, Rasband WS, Eliceiri KW (2012) NIH Image to ImageJ: 25 years of image analysis. Nat Methods 9:671–675
Nihei A, Hagiwara K, Kikuchi M, Yashiro T, Hoshino Y (2003) Histological investigation of rabbit ligamentum flavum with special reference to differences in spinal levels. Anat Sci Int 78:162–167. doi:10.1046/j.0022-7722.2003.00050.x
Hijioka A, Suzuki K, Nakamura T, Yokoyama M, Kanazawa Y (1994) Light and electron microscopy of hydroxyapatite depositions in the ligamentum flavum. Spine (Hagerstown) 19:2626–2631
Okuda T, Baba I, Fujimoto Y, Tanaka N, Sumida T, Manabe H, Hayashi Y, Ochi M (2004) The pathology of ligamentum flavum in degenerative lumbar disease. Spine 29:1689–1697
Schräder P, Grob D, Rahn BA, Cordey J, Dvorak J (1999) Histology of the ligamentum flavum in patients with degenerative lumbar spinal stenosis. Eur Spine J 8:323–328
Chen J, Liu Z, Zhong G, Qian L, Li Z, Qiao Z, Chen B, Wang H (2014) Hypertrophy of ligamentum flavum in lumbar spine stenosis is associated with increased miR-155 level. Dis Markers 2014:786543. doi:10.1155/2014/786543
Kosaka H, Sairyo K, Biyani A, Leaman D, Yeasting R, Higashino K, Sakai T, Katoh S, Sano T, Goel VK, Yasui N (2007) Pathomechanism of loss of elasticity and hypertrophy of lumbar ligamentum flavum in elderly patients with lumbar spinal canal stenosis. Spine (Phila Pa 1976) 32:2805–2811. doi:10.1097/BRS.0b013e31815b650f
Nakamura T, Okada T, Endo M, Kadomatsu T, Taniwaki T, Sei A, Odagiri H, Masuda T, Fujimoto T, Nakamura T, Oike Y, Mizuta H (2014) Angiopoietin-like protein 2 induced by mechanical stress accelerates degeneration and hypertrophy of the ligamentum flavum in lumbar spinal canal stenosis. PLoS ONE 9:e85542. doi:10.1371/journal.pone.0085542
Oh IS, Suh DW, Ha KY (2013) Hypertrophy of the ligament flavum in degenerative lumbar stenosis associated with the increased expression of fractalkine (CX3CL1)/CX3CR1 chemokine. Connect Tissue Res 54:380–385. doi:10.3109/03008207.2013.848199
Park JB, Chang H, Lee JK (2001) Quantitative analysis of transforming growth factor-beta 1 in ligamentum flavum of lumbar spinal stenosis and disc herniation. Spine 26:E492–E495
Zhong ZM, Zha DS, Xiao WD, Wu SH, Wu Q, Zhang Y, Liu FQ, Chen JT (2011) Hypertrophy of ligamentum flavum in lumbar spine stenosis associated with the increased expression of connective tissue growth factor. J Orthop Res 29:1592–1597. doi:10.1002/jor.21431
Anekstein Y, Smorgick Y, Lotan R, Agar G, Shalmon E, Floman Y, Mirovsky Y (2010) Diabetes mellitus as a risk factor for the development of lumbar spinal stenosis. Isr Med Assoc J 12:16–20
Lotan R, Oron A, Anekstein Y, Shalmon E, Mirovsky Y (2008) Lumbar stenosis and systemic diseases: is there any relevance? J Spinal Disord Tech 21:247–251. doi:10.1097/BSD.0b013e31813707af
Kim HJ, Lee KW, Cho HG, Kang KT, Chang BS, Lee CK, Yeom JS (2015) Indirect effects of decompression surgery on glycemic homeostasis in patients with type 2 diabetes mellitus and lumbar spinal stenosis. Spine J 15:25–33. doi:10.1016/j.spinee.2014.06.016
Kim KT, Cho DC, Sung JK, Kim CH, Kang H, Kim DH (2017) Changes in HbA1c levels and body mass index after successful decompression surgery in patients with type 2 diabetes mellitus and lumbar spinal stenosis: results of a 2-year follow-up study. Spine J 17:203–210. doi:10.1016/j.spinee.2016.08.029
Nicoloff G, Baydanoff S, Stanimirova N, Petrova C, Christova P (2000) An association of anti-elastin IgA antibodies with development of retinopathy in diabetic children. Gen Pharmacol 35:83–87
Thongboonkerd V, Barati MT, McLeish KR, Benarafa C, Remold-O’Donnell E, Zheng S, Rovin BH, Pierce WM, Epstein PN, Klein JB (2004) Alterations in the renal elastin-elastase system in type 1 diabetic nephropathy identified by proteomic analysis. J Am Soc Nephrol 15:650–662
Orasanu G, Plutzky J (2009) The pathologic continuum of diabetic vascular disease. J Am Coll Cardiol 53:S35–S42. doi:10.1016/j.jacc.2008.09.055
Knutsson B, Sanden B, Sjoden G, Jarvholm B, Michaelsson K (2015) Body mass index and risk for clinical lumbar spinal stenosis: a cohort study. Spine 40:1451–1456. doi:10.1097/BRS.0000000000001038
Acknowledgements
The study was supported by a research grant obtained from the research authority at the Rabin Medical Center.
Author information
Authors and Affiliations
Contributions
All authors have demonstrated (1) substantial contributions to research design, or the acquisition, analysis or interpretation of data; (2) drafting the paper or revising it critically; (3) approval of the submitted and final versions.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Shemesh, S., Sidon, E., Kaisler, E. et al. Diabetes mellitus is associated with increased elastin fiber loss in ligamentum flavum of patients with lumbar spinal canal stenosis: results of a pilot histological study. Eur Spine J 27, 1614–1622 (2018). https://doi.org/10.1007/s00586-017-5315-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5315-0