Abstract
Purpose
The use of inter-body device in lumbar fusions has been difficult to validate, only few long-term RCT are available.
Methods
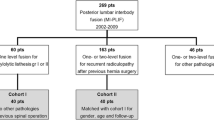
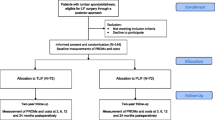
Between 2003 and 2005, 100 patients entered a RCT between transforaminal lumbar inter-body fusion (TLIF) or posterolateral instrumented lumbar fusion (PLF). The patients suffered from LBP due to segmental instability, disc degeneration, former disc herniation, spondylolisthesis Meyerding grade <2. Functional outcome parameters as Dallas pain questionnaire (DPQ), SF-36, low back pain questionnaire (LBRS), Oswestry disability index (ODI) were registered prospectively, and after 5–10 years.
Results
Follow-up reached 93 % of available, (94 %, 44 in the PLF’s and 92 %, 44 in the TLIF group p = 0.76). Mean follow-up was 8.6 years (5–10 years). Mean age at follow-up was 59 years (34–76 years p = 0.19). Reoperation rate in a long-term perspective was equal among groups 14 %, each p = 0.24. Back pain was 3.8 (mean) (Scale 0–10), TLIF (3.65) PLF (3.97) p = 0.62, leg pain 2.68 (mean) (Scale 0–10) 2.90 (TLIF) and 2.48 (PLF) p = 0.34. No difference in functional outcome between groups p = 0.93. Overall, global satisfaction with the primary intervention at 8.6 year was 76 % (75 % TLIF and 77 % PLF) p = 0.85.
Conclusion
In a long-term perspective, patients with TLIF’s did not experience better outcome scores.




Similar content being viewed by others
References
Brox JI, Sorensen R, Friis A et al (2003) Randomized clinical trial of lumbar instrumented fusion and cognitive intervention and exercises in patients with chronic low back pain and disc degeneration. Spine (Phila Pa 1976) 28:1913–1921
Brox JI, Reikeras O, Nygaard O et al (2006) Lumbar instrumented fusion compared with cognitive intervention and exercises in patients with chronic back pain after previous surgery for disc herniation: a prospective randomized controlled study. Pain 122:145–155
Moller H, Hedlund R (2000) Instrumented and noninstrumented posterolateral fusion in adult spondylolisthesis—a prospective randomized study: part 2. Spine (Phila Pa 1976) 25:1716–1721
Ekman P, Moller H, Hedlund R (2005) The long-term effect of posterolateral fusion in adult isthmic spondylolisthesis: a randomized controlled study. Spine J 5:36–44
Fritzell P, Hagg O, Wessberg P et al (2002) Chronic low back pain and fusion: a comparison of three surgical techniques: a prospective multicenter randomized study from the Swedish lumbar spine study group. Spine (Phila Pa 1976) 27:1131–1141
Brantigan JW, Neidre A, Toohey JS (2004) The lumbar I/F cage for posterior lumbar interbody fusion with the variable screw placement system: 10-year results of a food and drug administration clinical trial. Spine J 4:681–688
Harms JG, Jeszenszky D (1998) In process citation. Oper Orthop Traumatol 10:90–102
Gibson JN, Waddell G (2005) Surgery for degenerative lumbar spondylosis. Cochrane Database Syst Rev Cd001352
Thomsen K, Christensen FB, Eiskjaer SP et al (1997) 1997 Volvo Award winner in clinical studies. The effect of pedicle screw instrumentation on functional outcome and fusion rates in posterolateral lumbar spinal fusion: a prospective, randomized clinical study. Spine (Phila Pa 1976) 22:2813–2822
Barrick WT, Schofferman JA, Reynolds JB et al (2000) Anterior lumbar fusion improves discogenic pain at levels of prior posterolateral fusion. Spine (Phila Pa 1976) 25:853–857
Lee CK, Vessa P, Lee JK (1995) Chronic disabling low back pain syndrome caused by internal disc derangements. The results of disc excision and posterior lumbar interbody fusion. Spine (Phila Pa 1976) 20:356–361
Ekman P, Moller H, Tullberg T et al (2007) Posterior lumbar interbody fusion versus posterolateral fusion in adult isthmic spondylolisthesis. Spine (Phila Pa 1976) 32:2178–2183
Videbaek TS, Christensen FB, Soegaard R et al (2006) Circumferential fusion improves outcome in comparison with instrumented posterolateral fusion: long-term results of a randomized clinical trial. Spine (Phila Pa 1976) 31:2875–2880
Fritzell P, Hagg O, Nordwall A (2003) Complications in lumbar fusion surgery for chronic low back pain: comparison of three surgical techniques used in a prospective randomized study. A report from the Swedish Lumbar Spine Study Group. Eur Spine J 12:178–189
Hoy K, Bunger C, Niederman B et al (2013) Transforaminal lumbar interbody fusion (TLIF) versus posterolateral instrumented fusion (PLF) in degenerative lumbar disorders: a randomized clinical trial with 2-year follow-up. Eur Spine J 22:2022–2029
Christensen FB, Hansen ES, Eiskjaer SP et al (2002) Circumferential lumbar spinal fusion with Brantigan cage versus posterolateral fusion with titanium Cotrel–Dubousset instrumentation: a prospective, randomized clinical study of 146 patients. Spine (Phila Pa 1976) 27:2674–2683
Lawlis GF, Cuencas R, Selby D et al (1989) The development of the Dallas Pain Questionnaire. An assessment of the impact of spinal pain on behavior. Spine (Phila Pa 1976) 14:511–516
Manniche C, Asmussen K, Lauritsen B et al (1994) Low back pain rating scale: validation of a tool for assessment of low back pain. Pain 57:317–326
Fairbank JC, Pynsent PB (2000) The Oswestry disability index. Spine (Phila Pa 1976) 25:2940–2952 (discussion 2952)
Ware JE, Jr (2000) SF-36 health survey update. Spine (Phila Pa 1976) 25:3130–3139
Soegaard R, Bunger CE, Christiansen T et al (2007) Circumferential fusion is dominant over posterolateral fusion in a long-term perspective: cost-utility evaluation of a randomized controlled trial in severe, chronic low back pain. Spine (Phila Pa 1976) 32:2405–2414
Mannion AF, Leivseth G, Brox JI et al (2014) ISSLS Prize winner: Long-term follow-up suggests spinal fusion is associated with increased adjacent segment disc degeneration but without influence on clinical outcome: results of a combined follow-up from 4 randomized controlled trials. Spine (Phila Pa 1976) 39:1373–1383
Andersen T, Videbaek TS, Hansen ES et al (2008) The positive effect of posterolateral lumbar spinal fusion is preserved at long-term follow-up: a RCT with 11–13 year follow-up. Eur Spine J 17:272–280
Levin DA, Hale JJ, Bendo JA (2007) Adjacent segment degeneration following spinal fusion for degenerative disc disease. Bull NYU Hosp Jt Dis 65:29–36
Park P, Garton HJ, Gala VC et al (2004) Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine (Phila Pa 1976) 29:1938-1944
Videbaek TS, Egund N, Christensen FB et al (2010) Adjacent segment degeneration after lumbar spinal fusion: the impact of anterior column support: a randomized clinical trial with an eight- to thirteen-year magnetic resonance imaging follow-up. Spine (Phila Pa 1976) 35:1955–64
Videbaek TS, Bunger CE, Henriksen M et al (2011) Sagittal spinal balance after lumbar spinal fusion: the impact of anterior column support results from a randomized clinical trial with an eight- to thirteen-year radiographic follow-up. Spine (Phila Pa 1976) 36:183–191
Jiang SD, Chen JW, Jiang LS (2012) Which procedure is better for lumbar interbody fusion: anterior lumbar interbody fusion or transforaminal lumbar interbody fusion? Arch Orthop Trauma Surg 132:1259–1266
Audat Z, Moutasem O, Yousef K et al (2012) Comparison of clinical and radiological results of posterolateral fusion, posterior lumbar interbody fusion and transforaminal lumbar interbody fusion techniques in the treatment of degenerative lumbar spine. Singapore Med J 53:183–187
Rodriguez-Vela J, Lobo-Escolar A, Joven E et al (2013) Clinical outcomes of minimally invasive versus open approach for one-level transforaminal lumbar interbody fusion at the 3- to 4-year follow-up. Eur Spine J 22:2857–2863
Christensen A, Hoy K, Bunger C et al (2014) Transforaminal lumbar interbody fusion vs. posterolateral instrumented fusion: cost-utility evaluation alongside an RCT with a 2-year follow-up. Eur Spine J 23:1137–1143
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Høy, K., Truong, K., Andersen, T. et al. Addition of TLIF does not improve outcome over standard posterior instrumented fusion. 5–10 years long-term Follow-up: results from a RCT. Eur Spine J 26, 658–665 (2017). https://doi.org/10.1007/s00586-016-4592-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4592-3