Abstract
Purpose
The dynamic cervical implant (DCI) is a novel motion-preserving concept for the treatment of degenerative cervical disorders. The aim of this prospective clinical study was to validate the concept and analyse clinical and radiological performance of the implant.
Materials/methods
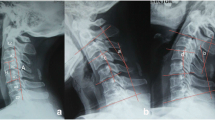
One hundred seventy-five consecutive patients with degenerative cervical disorders, median age, 47 years, were treated with discectomy and DCI, and followed for 2 years. Clinical outcome was evaluated with the Neck Disability Index (NDI), the SF-12, and visual analogue scale (VAS) assessment of arm and neck pain. Range of motion (ROM) and cervical alignment were analysed using radiographic imaging.
Results
All clinical outcome measures—VAS neck and arm pain, NDI, and SF-12 mental and physical component summaries—improved significantly after surgery (each p < 0.001) and remained stable over the whole observation period. The ROM (flexion/extension) at the level treated with DCI was slightly reduced, but no significant changes could be verified at the adjacent levels. Six surgery or device-related adverse events were documented during the study.
Conclusions
Good clinical and excellent radiological outcomes demonstrate that DCI is a safe and efficient treatment option in patients with degenerative cervical disorders.




Similar content being viewed by others
References
Denaro V, Di Martino A (2011) Cervical spine surgery: an historical perspective. Clin Orthop Relat Res 469:639–648
Vanek P, Bradac O, DeLacy P, Saur K, Belsan T, Benes V (2012) Comparison of 3 fusion techniques in the treatment of the degenerative cervical spine disease. Is stand-alone autograft really the “gold standard?”: prospective study with 2-years follow-up. Spine (Phila Pa 1976) 37:1645–1651
Ryu WH, Kowalczyk I, Duggal N (2013) Long-term kinematic analysis of cervical spine after single-level implantation of Bryan cervical disc prosthesis. Spine J 13:628–634
Dean CL, Gabriel JP, Cassinelli EH, Bolesta MJ, Bohlman HH (2009) Degenerative spondylolisthesis of the cervical spine: analysis of 58 patients treated with anterior cervical decompression and fusion. Spine J 9:439–446
Nunley PD, Jawahar A, Kerr EJ 3rd, Gordon CJ, Cavanaugh DA, Birdsong EM, Stocks M, Danielson G (2012) Factors affecting the incidence of symptomatic adjacent-level disease in cervical spine after total disc arthroplasty: 2- to 4-years follow-up of 3 prospective randomized trials. Spine (Phila Pa 1976) 37:445–451
McAfee PC, Reah C, Gilder K, Eisermann L, Cunningham B (2012) A meta-analysis of comparative outcomes following cervical arthroplasty or anterior cervical fusion: results from 4 prospective multicenter randomized clinical trials and up to 1226 patients. Spine (Phila Pa 1976) 37:943–952
Bydon M, Xu R, Macki M, De la Garza-Ramos R, Sciubba DM, Wolinsky JP, Witham TF, Gokaslan ZL, Bydon A (2014) Adjacent segment disease after anterior cervical discectomy and fusion in a large series. Neurosurgery 74:139–146 (discussion 146)
Jawahar A, Cavanaugh DA, Kerr EJ 3rd, Birdsong EM, Nunley PD (2010) Total disc arthroplasty does not affect the incidence of adjacent segment degeneration in cervical spine: results of 93 patients in three prospective randomized clinical trials. Spine J 10:1043–1048
Anderson PA, Sasso RC, Hipp J, Norvell DC, Raich A, Hashimoto R (2012) Kinematics of the cervical adjacent segments after disc arthroplasty compared with anterior discectomy and fusion: a systematic review and meta-analysis. Spine (Phila Pa 1976) 37:S85–S95
Boselie TF, Willems PC, van Mameren H, de Bie RA, Benzel EC, van Santbrink H (2013) Arthroplasty versus fusion in single-level cervical degenerative disc disease: a cochrane review. Spine (Phila Pa 1976) 38:E1096–E1107
Sun Y, Zhao YB, Pan SF, Zhou FF, Chen ZQ, Liu ZJ (2012) Comparison of adjacent segment degeneration 5 years after single level cervical fusion and cervical arthroplasty: a retrospective controlled study. Chin Med J (Engl) 125:3939–3941
Zigler JE, Delamarter R, Murrey D, Spivak J, Janssen M (2013) ProDisc-C and anterior cervical discectomy and fusion as surgical treatment for single-level cervical symptomatic degenerative disc disease: five-year results of a Food and Drug Administration study. Spine (Phila Pa 1976) 38:203–209
Lee JY, Hohl JB, Fedorka CJ, Devin C, Brodke DS, Branch CL Jr, Vaccaro AR (2011) Surgeons agree to disagree on surgical options for degenerative conditions of the cervical and lumbar spine. Spine (Phila Pa 1976) 36:E203–E212
Mo ZJ, Zhao YB, Wang LZ, Sun Y, Zhang M, Fan YB (2014) Biomechanical effects of cervical arthroplasty with U-shaped disc implant on segmental range of motion and loading of surrounding soft tissue. Eur Spine J 23:613–621
Welke B, Hurschler C, Schwarze M, Packheiser A, Tak S, Richter B, Daentzer D (2011) Biomechanical comparison between fusion, TDR and dynamic stabilization. In: 6th German Spine Conference, Hamburg, Germany, 8th–11th December 2011. Eur Spine J 20:2017–2018
Zhu R, Yang H, Wang Z, Wang G, Shen M, Yuan Q (2014) Comparisons of three anterior cervical surgeries in treating cervical spondylotic myelopathy. BMC Musculoskelet Disord 15:233
Matgé G, Berthold C, Gunness VR, Hana A, Hertel F (2015) Stabilization with the dynamic cervical implant: a novel treatment approach following cervical discectomy and decompression. J Neurosurg Spine 22:237–245
Wang L, Song YM, Liu LM, Liu H, Li T (2014) Clinical and radiographic outcomes of dynamic cervical implant replacement for treatment of single-level degenerative cervical disc disease: a 24-months follow-up. Eur Spine J 23:1680–1687
Cho SK, Riew KD (2013) Adjacent segment disease following cervical spine surgery. J Am Acad Orthop Surg 21:3–11
Park JY, Kim KH, Kuh SU, Chin DK, Kim KS, Cho YE (2013) What are the associative factors of adjacent segment degeneration after anterior cervical spine surgery? Comparative study between anterior cervical fusion and arthroplasty with 5-years follow-up MRI and CT. Eur Spine J 22:1078–1089
Herdmann J, Buddenberg P, Trautwein F, Rhee S, Piltz A, Floeth F (2012) Does maintenance of physiologic kinematics in the adjacent segment prevent adjacent segment degeneration following cervical dynamic stabilization? In: 7th German Spine Conference, Stuttgart, Germany, 6th–8th December 2012. Eur Spine J 21:2329
Auerbach JD, Jones KJ, Fras CI, Balderston JR, Rushton SA, Chin KR (2008) The prevalence of indications and contraindications to cervical total disc replacement. Spine J 8:711–716
Anakwenze OA, Auerbach JD, Milby AH, Lonner BS, Balderston RA (2009) Sagittal cervical alignment after cervical disc arthroplasty and anterior cervical discectomy and fusion: results of a prospective, randomized, controlled trial. Spine (Phila Pa 1976) 34:2001–2007
Guérin P, Obeid I, Gille O, Bourghli A, Luc S, Pointillart V, Vital JM (2012) Sagittal alignment after single cervical disc arthroplasty. J Spinal Disord Tech 25:10–16
Tu TH, Wu JC, Huang WC, Wu CL, Ko CC, Cheng H (2012) The effects of carpentry on heterotopic ossification and mobility in cervical arthroplasty: determination by computed tomography with a minimum 2-year follow-up: clinical article. J Neurosurg Spine 16:601–609
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Matgé, G., Buddenberg, P., Eif, M. et al. Dynamic cervical stabilization: a multicenter study. Eur Spine J 24, 2841–2847 (2015). https://doi.org/10.1007/s00586-015-4218-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4218-1