Abstract
Purpose
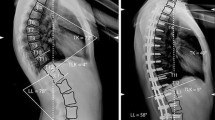
To analyze changes in spino-pelvic parameters (SPPs) after surgery of high-grade lumbar isthmic spondylolisthesis (HDIS).
Methods
We analyzed 41 patients affected by HDIS operated upon by attempt of reduction and posterior spinal fusion with pedicle screw systems with or without interbody fusion. Pelvic tilt (PT), lumbar lordosis (LL), pelvic incidence (PI), and sacral slope (SS) were measured, and patients were further divided into balanced and unbalanced pelvis subgroups.
Results
SS passed from 46.8° ± 9.8° preoperatively to 50.1° ± 10.1° (p = 0.02). PT passed from 26.7° ± 6.7° preoperatively to 22.9° ± 7.5° (p = 0.003). Unbalanced patients showed significantly higher PT and lower SS compared to the balanced patients preoperatively, and these corrected after surgery. Patients with instrumentation failure (n = 5) had significant increase in PT values postoperatively (p = 0.018).
Conclusions
We confirmed the positive effect of surgery on the SPPs in patients affected by HDIS, which showed different patterns of corrections with surgery for balanced and unbalanced pelvis patients.

Similar content being viewed by others
References
DeWald RL (1997) Spondylolisthesis. In: Bridwell KH, DeWald R (eds) Texbook of spinal surgery, 2nd edn. Lippincott Williams & Wilkins, Philadelphia, pp 1201–1209
Agabegi SS, Fischgrund JS (2010) Contemporary management of isthmic spondylolisthesis: pediatric and adult. Spine J 10:530–543
Ganju A (2002) Isthmic spondylolisthesis. Neurosurg focus 13:1–6
Beutler WJ, Fredrickson BE, Murtland A, Sweeney CA, Grant WD, Baker D (2003) The natural history of spondylolysis and spondylolisthesis: 45-year follow-up evaluation. Spine (Phila Pa 1976) 28:1027–1035
Bourghli A, Aunoble S, Reebye O, Le Huec JC (2011) Correlation of clinical outcome and spinopelvic sagittal alignment after surgical treatment of low-grade isthmic spondylolisthesis. Eur Spine J 20:663–668
Hensinger RN, Lang JR, MacEwen GD (1976) Surgical management of spondylolisthesis in children and adolescents. Spine (Phila Pa 1976) 1:207–216
Faldini C, Di Martino A, De Fine M, Miscione MT, Calamelli C, Mazzotti A, Perna F (2013) Current classification systems for adult degenerative scoliosis. Musculoskel Surg 97:1–8
Hresko MT, Labelle H, Roussouly P, Berthonnaud E (2007) Classification of high-grade spondylolistheses based on pelvic version and spine balance: possible rationale for reduction. Spine (Phila Pa 1976) 32:2208–2213
Mac-Thiong JM, Wang Z, de Guise JA, Labelle H (2008) Postural model of sagittal spino-pelvic alignment and its relevance for lumbosacral developmental spondylolisthesis. Spine (Phila Pa 1976) 33:2316–2325
Dubousset J (1997) Treatment of spondylolysis and spondylolisthesis in children and adolescents. Clin Orthop Relat Res 337:77–85
Mac-Thiong JM, Roussouly P, Berthonnaud É, Guigui P (2010) Sagittal parameters of global spinal balance: normative values from a prospective cohort of seven hundred nine Caucasian asymptomatic adults. Spine (Phila Pa 1976) 35:E1193–E1198
Martiniani M, Lamartina C, Specchia N (2012) “In situ” fusion or reduction in high-grade high dysplastic developmental spondylolisthesis (HDSS). Eur Spine J 21:134–140
Lazennec JY, Ramare S, Arafati N et al (2000) Sagittal alignment in lumbosacral fusion: relations between radiological parameters and pain. Eur Spine J 9:47–55
Hresko MT, Hirschfeld R, Buerk AA, Zurakowski D (2009) The effect of reduction and instrumentation of spondylolisthesis on spinopelvic sagittal alignment. J Pediatr Orthop 29:157–162
DeWald CJ, Vartabedian JE, Rodts MF, Hammerberg KW (2005) Evaluation and management of high-grade spondylolisthesis in adults. Spine (Phila Pa 1976) 30(6):S49–S59
Lamartina C (2001) A square to indicate the unstable zone in severe spondylolisthesis. Eur Spine J 10:444–448
Lonstein JE (1999) Spondylolisthesis in children: cause, natural history, and management. Spine(Phila Pa 1976) 24:2640–2648
Erfani MA, Pourabbas B, Nouraie H, Vadiee I, Vosoughi AR (2014) Results of fusion and instrumentation of thoracic and lumbar vertebral fractures in children: a prospective ten-year study. Musculoskelet Surg 98(2):107–114 (Epub ahead of print)
Bradford DS (1979) Treatment of severe spondylolisthesis: a combined approach for reduction and stabilization. Spine (Phila Pa 1976) 4:423–429
Poussa M, Schlenzka D, Seitsalo S, Ylikoski M, Hurri H, Österman K (1993) Surgical treatment of severe isthmic spondylolisthesis in adolescents: reduction or fusion in situ. Spine (Phila Pa 1976) 18:894–901
Molinari RW, Bridwell KH, Lenke LG, Ungacta FF, Riew KD (1999) Complications in the surgical treatment of pediatric high-grade, isthmic dysplastic spondylolisthesis: a comparison of three surgical approaches. Spine (Phila Pa 1976) 24:1701–1711
Longo UG, Loppini M, Romeo G, Maffulli N, Denaro V (2014) Evidence-based surgical management of spondylolisthesis: reduction or arthrodesis in situ. J Bone Joint Surg 96:53–58
Labelle H, Mac-Thiong JM, Roussouly P (2011) Spino-pelvic sagittal balance of spondylolisthesis: a review and classification. Eur Spine J 20:641–646
Labelle H, Roussouly P, Chopin D, Berthonnaud E, Hresko T, O’Brien M (2008) Spino-pelvic alignment after surgical correction for developmental spondylolisthesis. Eur Spine J 17:1170–1176
Wang Z, Wang B, Yin B, Liu W, Yang F, Lv G (2014) The relationship between spinopelvic parameters and clinical symptoms of severe isthmic spondylolisthesis: a prospective study of 64 patients. Eur Spine J 23:560–568
Acknowledgements
We wish to thank Prof. Roberta Aronica for English revision of the current manuscript.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Faldini, C., Di Martino, A., Perna, F. et al. Changes in spino-pelvic alignment after surgical treatment of high-grade isthmic spondylolisthesis by a posterior approach: a report of 41 cases. Eur Spine J 23 (Suppl 6), 714–719 (2014). https://doi.org/10.1007/s00586-014-3552-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3552-z