Abstract
Purpose
The challenges of fertility loss owing to cancer treatment persist long after treatment. However, psychosocial care for fertility among cancer survivors who have completed cancer treatment is insufficient. This systematic review examined psychosocial experiences related to the potential loss of fertility and unsuccessful pregnancy after treatment in cancer survivors of reproductive age to identify psychosocial care needs.
Methods
A systematic review was conducted using the online databases PubMed, Cochrane Library, PsycINFO, CINAHL, and Ichushi-Web between August and December 2022 to identify studies that addressed psychosocial experiences after fertility loss or failure to conceive among young cancer survivors. Study quality was assessed using the Mixed Methods Appraisal Tool.
Results
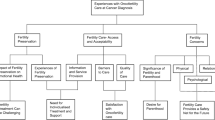
Forty studies were included, revealing psychosocial experiences across five categories: subjective fear of (potential) fertility loss, impact on romantic relationships, alternative methods for family building, reliance on social support, and specialized care. Only one study addressed the psychosocial aspects after complete loss of fertility in young cancer survivors.
Conclusions
The possibility and uncertainty of fertility loss led to stress and depression, loss of identity, decreased opportunities to meet a new partner, and damaged relationships established before diagnosis. The needs encompass fertility preservation, sexuality, approaches to building a family, partner communication, and other diverse needs.

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Smith KL, Gracia C, Sokalska A, Moore H (2018) Advances in fertility preservation for young women with cancer. Am Soc Clin Oncol Educ Book 38:27–37. https://doi.org/10.1200/EDBK_208301
Jeruss JS, Woodruff TK (2009) Preservation of fertility in patients with cancer. N Engl J Med 360(9):902–911. https://doi.org/10.1056/NEJMra0801454
McCarter K, Stewart J, Gordhandas S, Aluko A, Shah N, Schattman G, Rosenwaks Z (2022) The use of fertility preservation services for cancer patients: a single institution experience. F S Rep 3(4):349–354. https://doi.org/10.1016/j.xfre.2022.08.001
Rodriguez-Wallberg KA, Oktay K (2014) Fertility preservation during cancer treatment: clinical guidelines. Cancer Manag Res 6:105–117. https://doi.org/10.2147/CMAR.S32380
Lambertini M, Del Mastro L, Pescio MC et al (2016) Cancer and fertility preservation: international recommendations from an expert meeting. BMC Med 14:1. https://doi.org/10.1186/s12916-015-0545-7
Logan S, Perz J, Ussher JM, Peate M, Anazodo A (2019) Systematic review of fertility-related psychological distress in cancer patients: informing on an improved model of care. Psychooncology 28(1):22–30. https://doi.org/10.1002/pon.4927
Niemasik EE, Letourneau JM, Katz A, Belkora J, Cedars M, Rosen M (2012) Fertility preservation counseling at the time of cancer diagnosis reduces distress and anxiety. Fertil Steril 98(3):S46. https://doi.org/10.1016/j.fertnstert.2012.07.1067
Koizumi T, Sugishita Y, Suzuki-Takahashi Y, Nara K, Miyagawa T, Nakajima M, Sugimoto K, Futamura M, Furui T, Takai Y, Matsumoto H, Yamauchi H, Ohno S, Kataoka A, Kawai K, Fukuma E, Nogi H, Tsugawa K, Suzuki N (2023) Oncofertility-related psycho-educational therapy for young adult patients with breast cancer and their partners: randomized controlled trial. Cancer 129(16):2568–2580. https://doi.org/10.1002/cncr.34796
Logan S, Perz J, Ussher JM, Peate M, Anazodo A (2018) A systematic review of patient oncofertility support needs in reproductive cancer patients aged 14 to 45 years of age. Psychooncology 27(2):401–409. https://doi.org/10.1002/pon.4502
Hong QN, Fàbregues S, Bartlett G, Boardman F, Cargo M, Dagenais P, Gagnon MP, Griffiths F, Nicolau B, O’Cathain A, Rousseau MC (2018) The mixed methods appraisal tool (MMAT) version 2018 for information professionals and researchers. Educ Inf 34(4):285–291
Ussher JM, Perz J (2019) Infertility-related distress following cancer for women and men: a mixed method study. Psychooncology 28(3):607–614. https://doi.org/10.1002/pon.4990
Bártolo A, Santos IM, Valério E, Monteiro S (2020) Depression and health-related quality of life among young adult breast cancer patients: the mediating role of reproductive concerns. J Adolesc Young Adult Oncol 9(3):431–435. https://doi.org/10.1089/jayao.2019.0144
Carter J, Rowland K, Chi D, Brown C, Abu-Rustum N, Castiel M, Barakat R (2005) Gynecologic cancer treatment and the impact of cancer-related infertility. Gynecol Oncol 97(1):90–95. https://doi.org/10.1016/j.ygyno.2004.12.019
Patterson P, Perz J, Tindle R, McDonald FEJ, Ussher JM (2021) Infertility after cancer: how the need to be a parent, fertility-related social concern, and acceptance of illness influence quality of life. Cancer Nurs 44(4):E244–E251. https://doi.org/10.1097/NCC.0000000000000811
Kirkman M, Winship I, Stern C, Neil S, Mann GB, Fisher JR (2014) Women’s reflections on fertility and motherhood after breast cancer and its treatment. Eur J Cancer Care (Engl) 23(4):502–513. https://doi.org/10.1111/ecc.12163
Benedict C, Shuk E, Ford JS (2016) Fertility issues in adolescent and young adult cancer survivors. J Adolesc Young Adult Oncol 5(1):48–57. https://doi.org/10.1089/jayao.2015.0024
Zebrack BJ, Casillas J, Nohr L, Adams H, Zeltzer LK (2004) Fertility issues for young adult survivors of childhood cancer. Psychooncology 13(10):689–699. https://doi.org/10.1002/pon.784
Lehmann V, Keim MC, Nahata L, Shultz EL, Klosky JL, Tuinman MA, Gerhardt CA (2017) Fertility-related knowledge and reproductive goals in childhood cancer survivors: short communication. Hum Reprod 32(11):2250–2253. https://doi.org/10.1093/humrep/dex297
Quinn GP, Murphy D, Knapp CA, Christie J, Phares V, Wells KJ (2013) Coping styles of female adolescent cancer patients with potential fertility loss. J Adolesc Young Adult Oncol 2(2):66–71. https://doi.org/10.1089/jayao.2012.0038
Newton K, Howard AF, Thorne S, Kelly MT, Goddard K (2021) Facing the unknown: uncertain fertility in young adult survivors of childhood cancer. J Cancer Surviv 15(1):54–65. https://doi.org/10.1007/s11764-020-00910-x
Gorman JR, Bailey S, Pierce JP, Su HI (2012) How do you feel about fertility and parenthood? The voices of young female cancer survivors. J Cancer Surviv 6(2):200–209. https://doi.org/10.1007/s11764-011-0211-9
Nilsson J, Jervaeus A, Lampic C, Eriksson LE, Widmark C, Armuand GM, Malmros J, Marshall Heyman M, Wettergren L (2014) ‘Will I be able to have a baby?’ Results from online focus group discussions with childhood cancer survivors in Sweden. Hum Reprod 29(12):2704–2711. https://doi.org/10.1093/humrep/deu280
Benedict C, Hahn AL, McCready A, Kelvin JF, Diefenbach M, Ford JS (2020) Toward a theoretical understanding of young female cancer survivors’ decision-making about family-building post-treatment. Support Care Cancer 28(10):4857–4867. https://doi.org/10.1007/s00520-020-05307-1
Dryden A, Ussher JM, Perz J (2014) Young women’s construction of their post-cancer fertility. Psychol Health 29(11):1341–1360. https://doi.org/10.1080/08870446.2014.932790
Lehmann V, Nahata L, Ferrante AC, Hansen-Moore JA, Yeager ND, Klosky JL, Gerhardt CA (2018) Fertility-related perceptions and impact on romantic relationships among adult survivors of childhood cancer. J Adolesc Young Adult Oncol 7(4):409–414. https://doi.org/10.1089/jayao.2017.0121
Partridge AH, Gelber S, Peppercorn J, Sampson E, Knudsen K, Laufer M, Rosenberg R, Przypyszny M, Rein A, Winer EP (2004) Web-based survey of fertility issues in young women with breast cancer. J Clin Oncol 22(20):4174–4183. https://doi.org/10.1200/JCO.2004.01.159
Brånvall E, Derolf AR, Johansson E, Hultcrantz M, Bergmark K, Björkholm M (2014) Self-reported fertility in long-term survivors of acute myeloid leukemia. Ann Hematol 93(9):1491–1498. https://doi.org/10.1007/s00277-014-2088-y
Geue K, Richter D, Schmidt R, Sender A, Siedentopf F, Brähler E, Stöbel-Richter Y (2014) The desire for children and fertility issues among young German cancer survivors. J Adolesc Health 54(5):527–535. https://doi.org/10.1016/j.jadohealth.2013.10.005
Kim C, McGlynn KA, McCorkle R et al (2010) Fertility among testicular cancer survivors: a case-control study in the U.S. J Cancer Surviv. 4(3):266–273. https://doi.org/10.1007/s11764-010-0134-x
Guzik P, McKinney JA, Ulack C, Suarez J, Davis V, Teisberg E, Wallace S, Eckhardt SG, Capasso A (2021) Outcomes that matter most to young adults diagnosed with cancer: a qualitative study. J Adolesc Young Adult Oncol 10(5):534–539. https://doi.org/10.1089/jayao.2020.0150
Armuand G, Wettergren L, Nilsson J, Rodriguez-Wallberg K, Lampic C (2018) Threatened fertility: a longitudinal study exploring experiences of fertility and having children after cancer treatment. Eur J Cancer Care 27(2):e12798. https://doi.org/10.1111/ecc.12798
Goossens J, Delbaere I, Beeckman D, Verhaeghe S, Van Hecke A (2015) Communication difficulties and the experience of loneliness in patients with cancer dealing with fertility issues: a qualitative study. Oncol Nurs Forum 42(1):34–43. https://doi.org/10.1188/15.ONF.34-43
Wenzel L, Dogan-Ates A, Habbal R, Berkowitz R, Goldstein DP, Bernstein M, Kluhsman BC, Osann K, Newlands E, Seckl MJ, Hancock B, Cella D (2005) Defining and measuring reproductive concerns of female cancer survivors. J Natl Cancer Inst Monogr 34:94–98. https://doi.org/10.1093/jncimonographs/lgi017
Cherven B, Meacham L, Williamson Lewis R, Klosky JL, Marchak JG (2021) Evaluation of the modified reproductive concerns scale among emerging adult cancer survivors. J Adolesc Young Adult Oncol 10(6):661–667. https://doi.org/10.1089/jayao.2020.0219
Gorman JR, Su HI, Pierce JP, Roberts SC, Dominick SA, Malcarne VL (2014) A multidimensional scale to measure the reproductive concerns of young adult female cancer survivors. J Cancer Surviv 8(2):218–228. https://doi.org/10.1007/s11764-013-0333-3
Ota Y, Shimada K, Aoki G, Ohata K, Takamatsu H, Kondo Y, Yamazaki H (2018) Gaining a deepener understanding the thoughts of female hematopoietic tumor survivors regarding having a child through their life stories. J Wellness Health Care 41(2):129–137
Hawkey A, Ussher JM, Perz J, Parton C (2021) Talking but not always understanding: couple communication about infertility concerns after cancer. BMC Public Health 21(1):161. https://doi.org/10.1186/s12889-021-10188-y
Dobinson KA, Hoyt MA, Seidler ZE, Beaumont AL, Hullmann SE, Lawsin CR (2016) A grounded theory investigation into the psychosexual unmet needs of adolescent and young adult cancer survivors. J Adolesc Young Adult Oncol 5(2):135–145. https://doi.org/10.1089/jayao.2015.0022
Yoshida K, Matsui Y (2022) The impact of cancer on romantic relationships and marriage postdiagnosis among young adult cancer survivors in Japan: a qualitative study. J Adolesc Young Adult Oncol 11(2):146–155. https://doi.org/10.1089/jayao.2020.0199
Ussher JM, Perz J (2018) Australian Cancer and Fertility Study Team (ACFST). Threat of biographical disruption: the gendered construction and experience of infertility following cancer for women and men. BMC Cancer 18(1):250. https://doi.org/10.1186/s12885-018-4172-5
Stinson JN, Jibb LA, Greenberg M, Barrera M, Luca S, White ME, Gupta A (2015) A qualitative study of the impact of cancer on romantic relationships, sexual relationships, and fertility: perspectives of Canadian adolescents and parents during and after treatment. J Adolesc Young Adult Oncol 4(2):84–90. https://doi.org/10.1089/jayao.2014.0036
Jardim FA, Lopes-Júnior LC, Nascimento LC, Neves ET, de Lima RAG (2021) Fertility-related concerns and uncertainties in adolescent and young adult childhood cancer survivors. J Adolesc Young Adult Oncol 10(1):85–91. https://doi.org/10.1089/jayao.2020.0058
Carter J, Raviv L, Applegarth L, Ford JS, Josephs L, Grill E, Sklar C, Sonoda Y, Baser RE, Barakat RR (2010) A cross-sectional study of the psychosexual impact of cancer-related infertility in women: third-party reproductive assistance. J Cancer Surviv 4(3):236–246. https://doi.org/10.1007/s11764-010-0121-2
Gorman JR, Whitcomb BW, Standridge D, Malcarne VL, Romero SA, Roberts SA, Su HI (2017) Adoption consideration and concerns among young adult female cancer survivors. J Cancer Surviv 11(1):149–157. https://doi.org/10.1007/s11764-016-0572-1
Russell AM, Galvin KM, Harper MM, Clayman ML (2016) A comparison of heterosexual and LGBTQ cancer survivors’ outlooks on relationships, family building, possible infertility, and patient-doctor fertility risk communication. J Cancer Surviv 10(5):935–942. https://doi.org/10.1007/s11764-016-0524-9
Tschudin S, Bunting L, Abraham J, Gallop-Evans E, Fiander A, Boivin J (2010) Correlates of fertility issues in an internet survey of cancer survivors. J Psychosom Obstet Gynaecol 31(3):150–157. https://doi.org/10.3109/0167482X.2010.503910
Mobley EM, Foster KJ, Terry WW (2018) Identifying and understanding the gaps in care experienced by adolescent and young adult cancer patients at the University of Iowa hospitals and clinics. J Adolesc Young Adult Oncol 7(5):592–603. https://doi.org/10.1089/jayao.2018.0023
Gilles EE, Qian Y (2017) Online social support among women with post-cancer infertility and reproductive difficulty. Women Reprod Health 4(1):14–28
Sparidaens EM, Beerendonk C, Fleischer K et al (2022) Exploration of fertility and early menopause related information needs and development of online information for young breast cancer survivors. BMC Women’s Health 22(1):1–10
Irene SuH, Stark S, Kwan B, Boles S, Chingos D, Ehren J, Gorman JR, Krychman M, Romero SAD, Mao JJ, Pierce JP, Natarajan L (2019) Efficacy of a web-based women’s health survivorship care plan for young breast cancer survivors: a randomized controlled trial. Breast Cancer Res Treat 176(3):579–589. https://doi.org/10.1007/s10549-019-05260-6
Takekawa Y, Sugimoto K, Masaki K, Koizumi T, Mori H, Shiraishi E, Maezawa T, Tanigaki S, Shirai C, Suzuki N (2024) Differences between cancer survivors and healthy subjects in factors that facilitate and obstruct the use of the foster parent system and special adoption system: a nationwide cross-sectional study in Japan. J Adolesc Young Adult Oncol. https://doi.org/10.1089/jayao.2023.0088
Crawshaw M (2013) Male coping with cancer-fertility issues: putting the ‘social’ into biopsychosocial approaches. Reprod Biomed Online 27(3):261–270. https://doi.org/10.1016/j.rbmo.2013.04.017
City of Hope. Relationships after cancer treatment. https://www.cityofhope.org/patients/survivorship/relationships-after-cancer-treatment. Accessed 12 Mar 2023
Leukemia and Lymphoma Society®. New relationship. https://www.lls.org/managing-your-cancer/sexuality-and-intimacy/new-relationships. Accessed 12 Mar 2023
Benedict C, Nieh JL, Hahn AL, McCready A, Diefenbach M, Ford JS (2021) “Looking at future cancer survivors, give them a roadmap”: addressing fertility and family-building topics in post-treatment cancer survivorship care. Support Care Cancer 29(4):2203–2213. https://doi.org/10.1007/s00520-020-05731-3
Peate M, Meiser B, Cheah BC, Saunders C, Butow P, Thewes B, Hart R, Phillips KA, Hickey M, Friedlander M (2012) Making hard choices easier: a prospective, multicentre study to assess the efficacy of a fertility-related decision aid in young women with early-stage breast cancer. Br J Cancer 106(6):1053–1061. https://doi.org/10.1038/bjc.2012.61
Benedict C, Dauber-Decker KL, King D, Hahn A, Ford JS, Diefenbach M (2021) A decision aid intervention for family building after cancer: developmental study on the initial steps to consider when designing a web-based prototype. JMIR Form Res 5(1):e20841. https://doi.org/10.2196/20841
Yoshida K, Matsui Y (2023) An examination of the association between psychosocial aspects of fertility issues and demographic characteristics of unmarried adolescent and young adult cancer survivors. J Adolesc Young Adult Oncol. https://doi.org/10.1089/jayao.2023.0097
Shiraishi E, Sugimoto K, Shapiro JS, Ito Y, Kamoshita K, Kusuhara A, Haino T, Koizumi T, Okamoto A, Suzuki N (2020) Study of the awareness of adoption as a family-building option among oncofertility stakeholders in Japan. JCO Glob Oncol 6:350–355. https://doi.org/10.1200/JGO.18.00043
Quinn GP, Zebrack BJ, Sehovic I, Bowman ML, Vadaparampil ST (2015) Adoption and cancer survivors: findings from a learning activity for oncology nurses. Cancer 121(17):2993–3000. https://doi.org/10.1002/cncr.29322
Dong Y, Yue Z, Zhuang H, Zhang C, Fang Y, Jiang G (2023) The experiences of reproductive concerns in cancer survivors: a systematic review and meta-synthesis of qualitative studies. Cancer Med 12(24):22224–22251
Funding
This study was supported by a Health Labour Sciences Research Grant from the Ministry of Health, Labour and Welfare (grant number 20EA1004).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception. Literature search and data analysis were performed by KY, TH, and TK. The first draft of the manuscript was written by KY, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Implications for cancer survivors
It is natural to experience stress after the loss of fertility owing to cancer. No established care has yet been developed, and future research should clarify this issue. Cancer survivors may need to express themselves based on their diverse needs.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yoshida, K., Hashimoto, T., Koizumi, T. et al. Psychosocial experiences regarding potential fertility loss and pregnancy failure after treatment in cancer survivors of reproductive age to identify psychosocial care needs: a systematic review. Support Care Cancer 32, 337 (2024). https://doi.org/10.1007/s00520-024-08544-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08544-w