Abstract
Purpose
As narrative medicine interventions are integrated increasingly into medical practice, growing evidence indicates benefits for healthcare professionals. Presently, the prevalence and impact of narrative medicine interventions in the field of oncology remain unknown. This systematic review synthesizes published data on narrative medicine interventions in oncology and reports current knowledge on feasibility, acceptability, and impact on cancer care professionals.
Methods
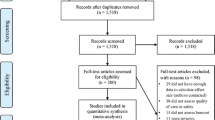
Following PRISMA guidelines, we searched Ovid Medline, Embase, Scopus, Web of Science, Cochrane, and ClinicalTrials.gov databases from inception through February 2024. Eligible articles were published in English and contained original data on feasibility, acceptability, and/or impact of a narrative medicine intervention for oncology professionals. Database searches identified 2614 deduplicated articles, from which 50 articles were identified for full-text assessment and 11 articles met inclusion criteria. Two additional articles were identified through manual review of references.
Results
Thirteen articles described 12 unique narrative medicine interventions targeting cancer care professionals. All studies described their respective interventions as feasible, acceptable, and impactful for participants. Interventions involved writing, reading, reflection, and other narrative-based strategies. Standardized validated tools evaluated outcomes including burnout, empathy expression, secondary trauma, quality of humanistic care, and well-being. Participants reported appreciation of opportunities for reflection, perspective sharing, and bearing witness, which they perceived to strengthen wellness and community.
Conclusion
Narrative medicine interventions are feasible and acceptable and may bolster oncology clinicians’ functioning across domains. Multi-site, prospective, randomized studies are needed to investigate the broader impact of narrative medicine interventions and advance the science of narrative medicine in oncology.
Trial registration
ClinicalTrials.gov Identifier: CRD42022369432


Similar content being viewed by others
Data availability
The review protocol can be accessed on the Prospero registry. No amendments were made to information provided in the protocol. Template data collection forms, data extracted from included studies, data used for all analyses, and analytic code are all provided in this manuscript.
Abbreviations
- MeSH :
-
Medical Subject Headings
- MMAT :
-
McGill Mixed Methods Appraisal Tool
- PICOTS :
-
Patient population, Intervention, Comparator, Outcome, Timing, Setting
- PRISMA :
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
References
Charon R (2001). The patient-physician relationship. Narrative medicine: a model for empathy, reflection, profession, and trust. JAMA, 286(15), 1897–1902. https://doi.org/10.1001/JAMA.286.15.1897
Remein CDF, Childs E, Pasco JC, Trinquart L, Flynn DB, Wingerter SL, Bhasin RM, Demers LB, Benjamin EJ (2020). Content and outcomes of narrative medicine programmes: a systematic review of the literature through 2019. BMJ Open, 10(1). https://doi.org/10.1136/BMJOPEN-2019-031568
Charon R, Hermann N, Devlin MJ (2016) Close reading and creative writing in clinical education: teaching attention, representation, and affiliation. Acad Med : J Assoc Ame Med Colleges 91(3):345–350. https://doi.org/10.1097/ACM.0000000000000827
Hlubocky FJ, Back AL, Shanafelt TD (2016) Addressing burnout in oncology: why cancer care clinicians are at risk, what individuals can do, and how organizations can respond. American Society of Clinical Oncology Educational Book. American Society of Clinical Oncology. Annual Meeting, 35(36), 271–279. https://doi.org/10.1200/EDBK_156120
Medisauskaite A, Kamau C (2017) Prevalence of oncologists in distress: systematic review and meta-analysis. Psycho-Oncology 26(11):1732–1740. https://doi.org/10.1002/PON.4382
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, Moher D (2021). The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ, 372. https://doi.org/10.1136/BMJ.N71
Pluye P, Gagnon MP, Griffiths F, Johnson-Lafleur J (2009) A scoring system for appraising mixed methods research, and concomitantly appraising qualitative, quantitative and mixed methods primary studies in mixed studies reviews. Int J Nursing Stud 46(4):529–546. https://doi.org/10.1016/J.IJNURSTU.2009.01.009
Phillips CS, Volker DL, Davidson KL, Becker H (2020) Storytelling through music: a multidimensional expressive arts intervention to improve emotional well-being of oncology nurses. JCO Oncol Prac 16(4):E405–E414. https://doi.org/10.1200/JOP.19.00748
Laing CM, Moules NJ, Sinclair S, Estefan A (2020). Understanding the impact on healthcare professionals of viewing digital stories of adults with cancer: a hermeneutic study. J Appl Hermeneutics.
Saint-Louis NM, Bourjolly JN (2018) Narrative intervention: stories from the front lines of oncology health care. Social Work Health Care 57(8):637–655. https://doi.org/10.1080/00981389.2018.1474836
Pediatric narrative oncology: interprofessional training to promote empathy, build teams, and prevent burnout - PubMed. (n.d.). Retrieved March 25, 2023, from https://pubmed.ncbi.nlm.nih.gov/18847073/
Sands SA, Stanley P, Charon R (2008) Pediatric narrative oncology: interprofessional training to promote empathy, build teams, and prevent burnout. J Support Oncol, 6(7), 307–312. https://pubmed.ncbi.nlm.nih.gov/18847073/
Saint-Louis NM, Senreich E (2018) Thse evaluation of a narrative intervention for health-care professionals in an urban oncology inpatient unit. Urban Social Work 2(2):176–190. https://doi.org/10.1891/2474-8684.2.2.176
Wall LM (2021) Ethics education: using storytelling to teach ethics to novice oncology nurses. Clin J Oncol Nursing 25(6):E63–E68. https://doi.org/10.1188/21.CJON.E63-E68
Phillips CS, Volker DL, Becker H, Davidson KL (2021) Storytelling through music to improve well-being in oncology nurses: a feasibility study. Cancer Nursing 44(6):473–481. https://doi.org/10.1097/NCC.0000000000000836
Using second life to facilitate peer storytelling for grieving oncology nurses - PubMed. (n.d.). Retrieved March 25, 2023, from https://pubmed.ncbi.nlm.nih.gov/25598720/
Shaw AC, McQuade JL, Reilley MJ, Nixon B, Baile WF, Epner DE (2019) Integrating storytelling into a communication skills teaching program for medical oncology fellows. J Cancer Education : official J Ame Assoc Cancer Educ 34(6):1198–1203. https://doi.org/10.1007/S13187-018-1428-3
Richardson DR, Tan X, Winzelberg G, Rosenstein DL, Collichio FA (2020) Development of an art of oncology curriculum to mitigate burnout and foster solidarity among hematology/oncology fellows. JCO Oncol Prac 16(4):E384–E394. https://doi.org/10.1200/JOP.19.00529
Rice KL, Bennett MJ, Billingsley L (2014) Using second life to facilitate peer storytelling for grieving oncology nurses. Ochsner J, 14(4), 551. /pmc/articles/PMC4295732/
Klein J (2003) Narrative oncology. Oncology. Times 25(4):10. https://doi.org/10.1097/01.COT.0000289617.51284.63
Mohanti BK (2021) Lessons from narrative medicine: cancer care will improve with narrative oncology. Indian J Cancer 58(4):615–618. https://doi.org/10.4103/IJC.IJC_809_20
Schapira L, Meisel JL, Srivastava R (2017). For our patients, for ourselves: the value of personal reflection in oncology. American Society of Clinical Oncology Educational Book. American Society of Clinical Oncology. Annual Meeting, 37(37), 765–770. https://doi.org/10.1200/EDBK_175520
A conversation with Lidia Schapira, MD, the new JCO art of oncology editor - the ASCO post. (n.d.). Retrieved April 3, 2023, from https://ascopost.com/issues/september-1-2014/a-conversation-with-lidia-schapira-md-the-new-jco-art-of-oncology-editor/
Steensma DP (2013) Stories we tell one another: narrative reflection and the art of oncology. American society of clinical oncology educational book. American society of clinical oncology. Annual Meeting, 33, e331–e335. https://doi.org/10.14694/EDBOOK_AM.2013.33.E331
Winkel AF (2016). Narrative medicine: a writing workshop curriculum for residents. MedEdPORTAL : The Journal of Teaching and Learning Resources, 12. https://doi.org/10.15766/MEP_2374-8265.10493
Columbia University: Narrative Medicine. (n.d.). https://Sps.Columbia.Edu/Academics/Masters/Narrative-Medicine
University of Toronto: narrative-based medicine program. (n.d.). https://Temertymedicine.Utoronto.ca/Event/Narrative-Based-Medicine-Digital-Certificate-Program
The good listening project: certified listener poet course. (n.d.). https://www.Goodlistening.Org/Certified-Listener-Poet-Course
West CP, Dyrbye LN, Sloan JA, Shanafelt TD (2009) Single item measures of emotional exhaustion and depersonalization are useful for assessing burnout in medical professionals. J Gen Inter Med 24(12):1318–1321. https://doi.org/10.1007/S11606-009-1129-Z
West CP, Dyrbye LN, Satele DV, Sloan JA, Shanafelt TD (2012) Concurrent validity of single-item measures of emotional exhaustion and depersonalization in burnout assessment. J Gen Inter Med 27(11):1445–1452. https://doi.org/10.1007/S11606-012-2015-7
Lorenz FJ, Darok MC, Ho L, Holstrom-Mercader MS, Freiberg AS, Dellasega CA (2022) The impact of an unconventional elective in narrative medicine and pediatric psycho-oncology on humanism in medical students. J Cancer Educ 37(6):1798–1805. https://doi.org/10.1007/s13187-021-02029-8
Lu N, Ma Z, Shi Y, Yao S, Zhang L, Shan J, Zhai L, Li C, Cheng F (2023) A narrative medicine-based training program increases the humanistic care quality of new nurses in cancer hospital. Prec Med Sci 12(1):23–28. https://doi.org/10.1002/prm2.12091
Funding
This work is supported in part by ALSAC. Additionally, Dr. Kaye receives salary support from the National Cancer Institute (K08CA266935).
Author information
Authors and Affiliations
Contributions
TP, YR, AG, RE, AS, and DM performed systematic review. JW and ER created systematic review search with TP. EK and MW reviewed PRISMA protocol and systematic review findings, and assisted with drafting manuscript. TP created all tables and RE created Fig. 2. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Précis
Narrative medicine interventions are feasible, acceptable, and may bolster oncology clinicians’ functioning. Multi-site, prospective, randomized studies are needed to advance the science of narrative medicine in oncology.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Paul, T.K., Reddy, Y., Gnanakumar, A. et al. Narrative medicine interventions for oncology clinicians: a systematic review. Support Care Cancer 32, 241 (2024). https://doi.org/10.1007/s00520-024-08434-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08434-1